The immune system comprises a complex network of immune cells that work in synergy with proteins such as cytokines in order to combat pathogenic invaders such as bacteria, viruses, fungi, parasitic worms, abnormal cells, etc. They have a unique ability to distinguish self-molecules from non-self-molecules except in some diseased conditions such as autoimmune diseases. The ability to distinguish self from non-self is based on the unique Major Histocompatibility Complex (MHC) protein that an individual’s all body cells possess on their surface, except for identical twins. There are two types of MHC proteins: MHC I and MHC II in which MHC I differentiate the body’s own cells from foreign cells or pathogens and displays antigen on the surface of the cell however, MHC II is present in immune cells called antigen-presenting cells (APC) along with MHC I and these display phagocytosed microbe on the cell surface. MHC proteins are absent in red blood cells.
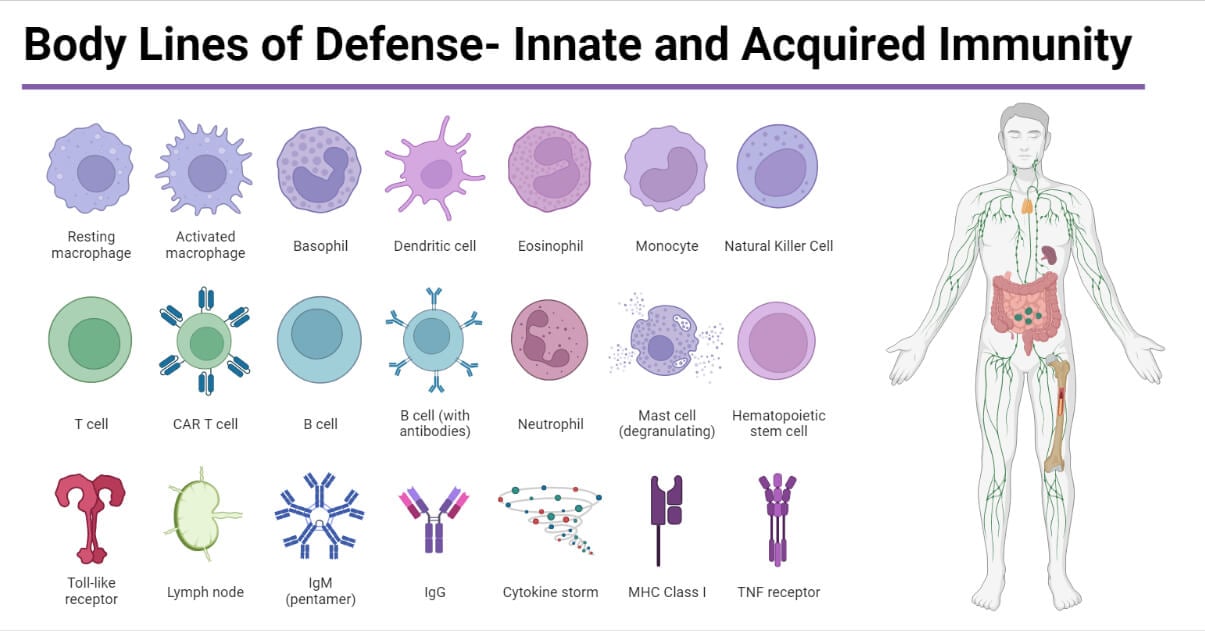
Innate and Acquired Defense Systems
There are two types of body responses against invaders:
Innate (Natural/Non-specific response) and Acquired (Adaptive/Specific) responses.
- Innate responses occur to same extent no matter how many times the pathogen is exposed while acquired responses are improved with the repeated subsequent exposure to foreign particles.
- Innate responses employ phagocytic cells such as neutrophils, monocytes and macrophages, and Natural Killer (NK) cells. However, adaptive responses involve antigen-specific B and T cells or antigen-presenting cells (APCs).
- Innate responses respond immediately to the foreign attack while adaptive take a longer time to react.
- Innate responses fight against all invaders, hence termed as non-specific and acquired responses fight against specific types of invaders, specific.
- Innate response comprises of the first and second line of defense and acquired response includes the third line of defense.
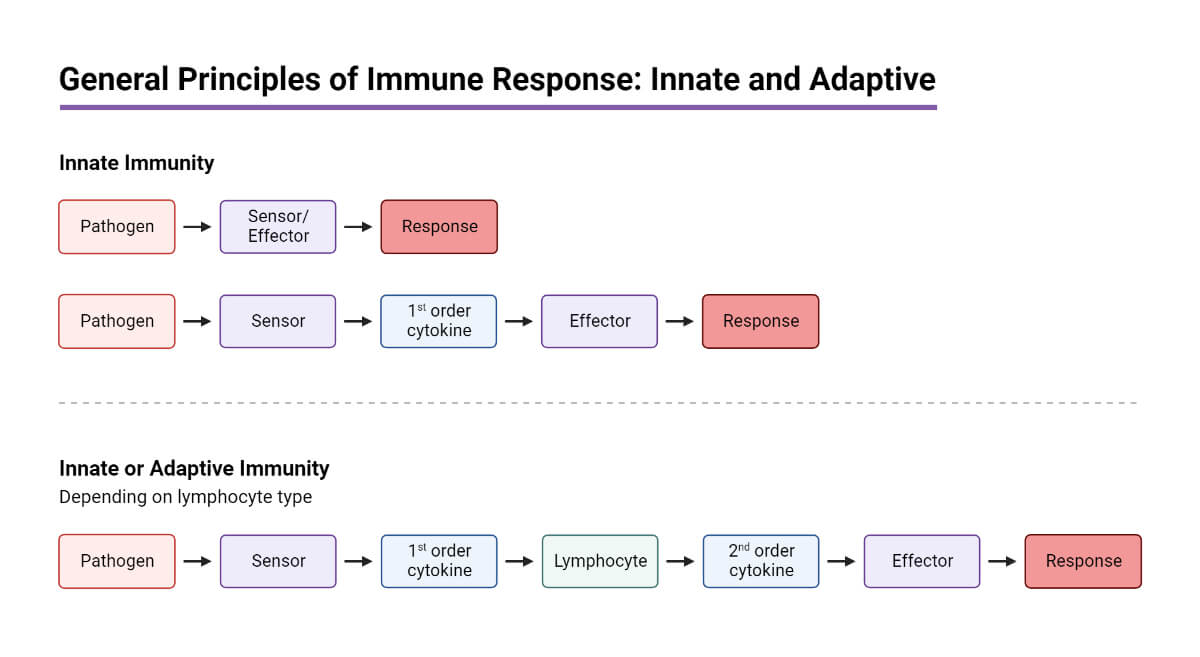
Basically, there are three types of lines of defense:
1. First line of defense
2. Second line of defense
3. Third line of defense
1. First Line of Defense
- It is also known as an outside defense system.
- Physical, chemical, and biological defenses form the first line of defense against the invasion of pathogens and these do not function independently and can overlap based on their functions.
i) Physical defenses: These include physical barriers and mechanical defenses which block the entry point of pathogens such as intact skin and mucus.
- Skin has three layers: the epidermis, the dermis, and the hypodermis. The topmost layer, the epidermis is packed with keratin along with dead skin cells. These dead cells are frequently being shed and replaced. The keratin is highly water-resistant and mechanically tough hence, resists microbial growth.
- Nasal hairs filter air contaminated with microbes, dust, and dirt while microscopic cilia lining the respiratory tract, sweep mucus and trap particles inhaled towards body openings where they can be removed from the body.
- Mucous membranes lining respiratory, urinary, and reproductive tracts, produce mucus, a slimy substance that traps foreign particles and directs them out of the body by mechanical actions such as shedding, coughing, peristalsis, and flushing of bodily fluids (e.g. urination, tears)
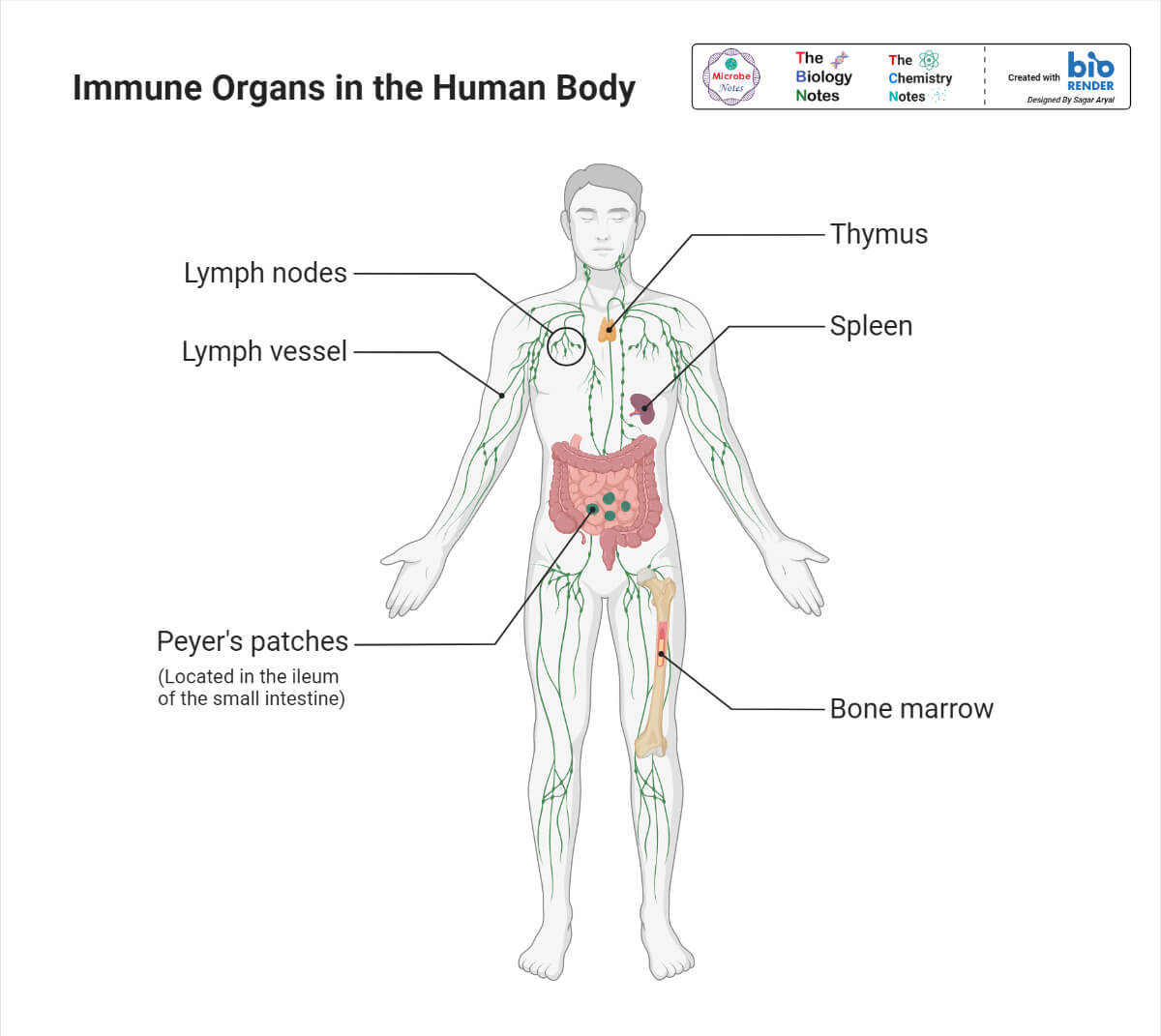
ii) Chemical defenses comprise chemicals and enzymes in body fluids, a variety of plasma protein mediators, cytokines, antimicrobial peptides, inflammation- eliciting mediators that destroys pathogens on the outer body surface, at body opening, and on inner body linings.
- Sweat, tears, mucus, and saliva contain enzymes that kill pathogens. Lysozyme, an enzyme found in tears, perspiration, and saliva can break down the cell walls of bacteria and kill them. Likewise, secretory IgA function in a similar manner by attacking peptidoglycans in the cell wall of bacteria. Antimicrobial peptides (AMPs) include dermcidin, cathelicidin, defensins, histatins, and bacteriocins. AMPs are produced in response to pathogens on the skin
- Cerumen or ear wax contains fatty acids thereby lowering the pH between 3 and 5, it protects the auditory canal from foreign particles like microbes.
- Gastric juice (pH 2-3) is highly acidic in nature and those pathogens that enter the stomach through the oral cavity or nasal tract are destroyed by it.
- Urine flow, acidic in pH, kill microbes and direct out of the urethra.
- Serum (unsaturated fatty acids) reduce water loss as well as inhibit microbial growth however, it is found to have certain compounds that facilitate to provide nutrition for certain microbes.
iii) Biological defenses are provided by living microorganisms that are friendly and beneficial. These are resident natural flora that resides on our skin, in our bowel, and in other places such as the mouth, gut, reproductive part, etc. These prevent pathogen adherence and their colonization by creating an acidic environment with the help of fermentation of sugars to acids, occupying available cellular binding sites and competing with them for available nutrients. Thus, resident normal microbiota also contributes to chemical defenses as they produce bacteriocins that perform the antibacterial activity.
2. Second Line of Defense
It is also known as the immune system.
When the first line of defense is broken, the second line of defense within our body ‘kicks’ in and gets activated i.e. when the pathogens successfully win the battle against barriers from the first line of defense, they are next encountered by the second line. This mechanism involves the participation of mainly immune cells mainly white blood cells (leucocytes) such as phagocytes, NK cells, dendritic cells, mast cells, and complement proteins to recognize and eliminate any non-specific pathogen entered into the body. There is no immunological memory.
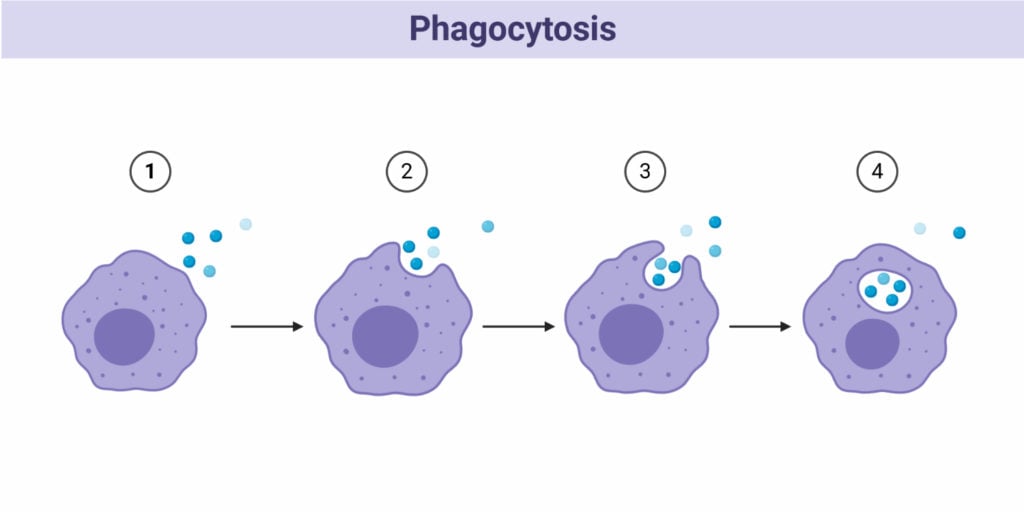
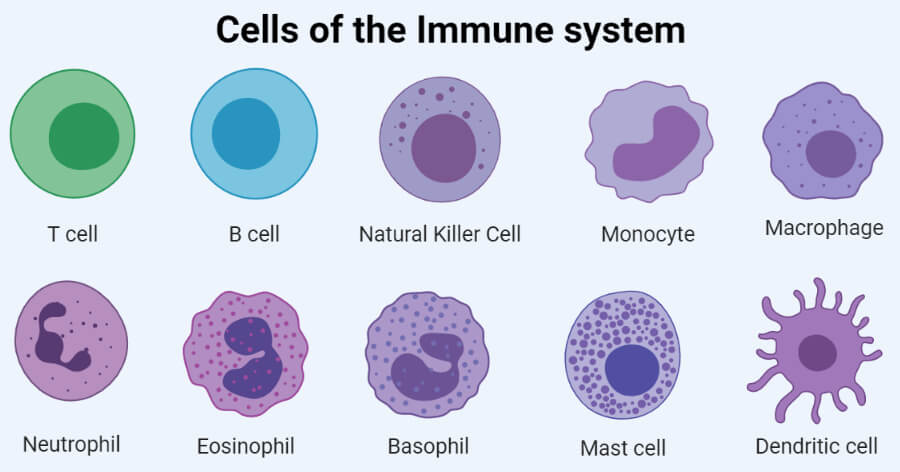
Phagocytes (eating cells) and their relatives
- Basophils: These account for merely 1% of WBCs. These are known for their inflammatory response associated with asthma and allergies as when they are stimulated, they release heparin and histamine.
- Mast cells: These exhibit functional similarities with basophils although these reside within tissues. They show inflammatory response as a result of activation with different inflammatory mediators, and antigens. It releases granules that include inflammatory histamine once it recognizes pathogens.
- Monocytes: These are related to scavenging and are known as “garbage trucks” or “vacuum cleaners” of the immune system. These comprise around 2-6% of WBCs in the blood. These cells form the largest among WBCs. They differentiate into macrophages and dendritic cells after leaving the circulation into tissues in response to inflammation.
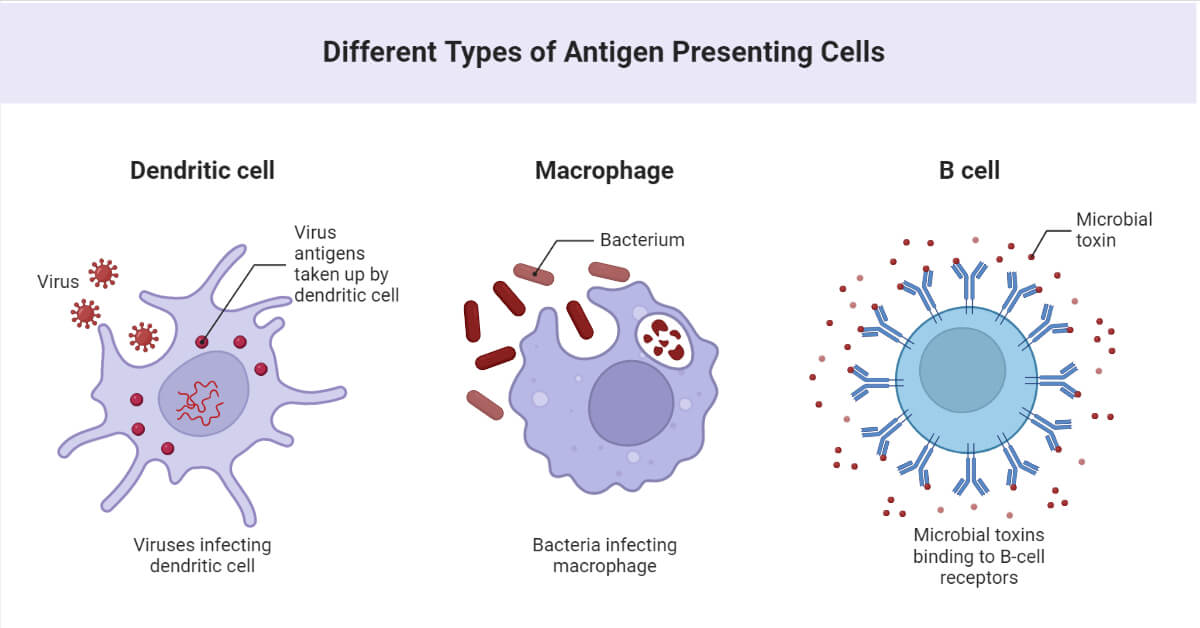
- Macrophages: These engulf and digest pathogens lacking specific surface proteins to healthy body cells, such as cancerous cells, microbes, cellular debris, etc., and are found in the tissues and organs. They release regulatory factors such as interferons, interleukins, etc, and a wide array of chemicals including enzymes, and complement proteins. These active T cells and hence, the adaptive immune system by acting as “antigen-presenting cells” as these processes engulfed antigens and present them to T cells.
- Dendritic cells: These are differentiated from monocytes present in the tissues located in contact with the external environment such as skin, nose, lungs, etc. These cells link innate immunity and adaptive immunity. Once they find foreign particles, they migrate to lymph nodes where they present the antigen and interact with T cells and B cells that initiate an adaptive immune response. These are named dendritic in the sense that they have their cellular morphology in the form of a “tree-like” structure.
- Neutrophils: These are the first immune cells to respond to intruders and form approximately 65% of WBCs. They squeeze out through capillaries into the site of infection as well as send out signals to alert other immune cells. Thus, these are also known as ‘patrol tissue’. Once they are released from bone marrow, they have a short life span of about only eight hours.
- Natural Killer (NK) cells: These are the only cytotoxic lymphocytes belonging to the innate immune system and respond rapidly to virus-infected cells or tumor cells without any priming or prior activation. Thus, these are best known for their “natural” killing ability subsequently, help to detect and control early signs of cancer.
Mechanism of the second line of defense
With the invasion of the pathogen at the entry site, neutrophils come into action to engulf and destroy them. If they evade the action of neutrophils, then macrophages and dendritic cells go into battle which helps to phagocytose and present antigens to T cells. Different internal defense includes phagocytosis, NK cells, inflammatory response, fever, and the complement system in the second line of defense. Different cytokines are released by immune cells as well as infected cells which amplify the quantity of cytokine secretion. This triggers an inflammatory response, capillary dilation, and increased permeability of the capillary wall. Macrophages are involved in the resolution of the inflamed site and clearing up cellular debris. Cytokines also increase the core body temperature resulting in fever. This increased temperature inhibits microbial growth and speeds up recovery and repair processes. NK cells detect viral infested cells or cancerous cells thereby inducing apoptosis. Similarly, different complement proteins found in the blood serum, are attracted to pathogens tagged with the adaptive immune system. A cascade of binding of complement proteins to pathogens coats the pathogen which serves as a marker to detect the presence of a pathogen in phagocytes and their digestion by the phagocytosis process.
3. Third Line of Defense
It is also known as the adaptive immune system which is not acquired by birth but during the lifetime. These target only specific pathogens and build long-lasting immunity, strong immune response, and immunological memory. It takes a long time to develop innate immunity as lag time occurs between exposure and maximal response. However, on repeated exposure to the same antigen, these respond quickly to eliminate. It works to identify, destroy and remember principles. It gets activated only when pathogens pass the first and second line of defense. Different cells involved in the third line of defense are antigen-presenting cells (APC), B lymphocytes, and T lymphocytes.
Lymphocytes comprise T cells, B cells, and NK cells which make up 20-30% of WBCs and are found in the lymph hence named lymphocytes. Among them, T and B cells are components of adaptive immune response while NK cells are of the innate immune response as aforementioned. Humoral and cell-mediated immune responses are part of this defense.
Humoral or antibody-mediated immune response
B cells participate in antibody-mediated response where B cells in contact with a pathogen, are activated and produce antibodies that are released into the bloodstream. Notation ‘B’ cell was derived after the experiment conducted by Max Cooper in the 1960s to study the function of B cells where he demonstrated that antibody production was completely abrogated in irradiated chicken after surgical removal of the Bursa of Fabricius: the primary site of B cell development in birds. They originate and mature both in the bone marrow. B cells express diverse antigen-specific molecules on their outer surface that helps in antigen detection. Thus, when naive B cells encounter an antigen in the lymphatic system, these undergo clonal expansion and some clones differentiate into Memory B cells and Plasma B cells (Plasma cells / Plasmocytes / Effector B cells).
- Plasma B cells: These secrete antibodies also called immunoglobulins (Igs).
- Memory B cells: They provide the immune system with long-lasting memory.
Mechanism of antibody-mediated immune response
On exposure of B cells with its receptor to its matching antigen, it internalizes the antigen, digests it, and displays its fragments on its surface bound to unique MHC II molecules. This complex attracts mature matching helper T cells which secrete cytokines, interleukins, etc. Thus, produced secretions help in turn stimulate mitosis in B cells and their multiplication. Some B cells mature into plasma and memory cells. Antibodies secreted by plasma cells attach to antigens forming antigen-antibody complexes which are later cleared off by complement cascade, neutralization, agglutination, precipitation, etc.
Cell-mediated immune response
This immune response is driven by T lymphocytes, APCs such as macrophages, B cells, and dendritic cells, and various cytokines. It does not use antibodies. It mostly kills viruses and cancerous cells. There are 4 types of T lymphocytes: T-helper cells, T-killer cells, T-suppressor cells, and T-memory cells.
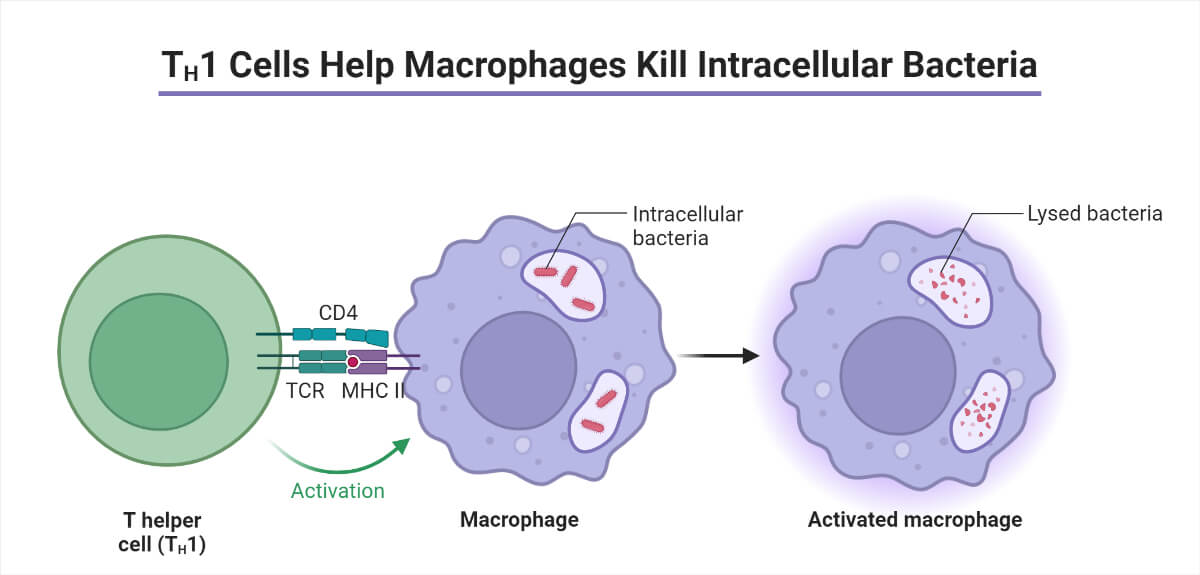
- TH /T helper cells (CD4+): These cells secrete cytokines which stimulate cell division of B cells and its maturation into plasma and memory cells, activation of macrophages to bring about phagocytosis, and clonal expansion of TH cells.
- Tc (T- killer/cytotoxic) cells (CD8+): These cells trigger the destruction of the pathogen’s DNA by secreting cytotoxin or creating holes in the pathogen’s cell membrane by perforin. This results in cell lysis or apoptosis.
- T-suppressor cells/Treg/Regulatory T cells: These form the part of the self-check built-in mechanism inside the body to prevent excessive immune reactions by shutting down T cell-mediated immunity once the pathogen has been defeated and also help to prevent autoimmune diseases.
- T-memory cells: The population of these cells increases only after their initial exposure to an antigen. If the same antigen presents itself again, they are triggered to convert themselves into cytotoxic T cells and kill the pathogen.
Mechanism of cell-mediated immune response
When APCs present antigenic fragments on its surface attached with MHC II protein, naïve T cells interact with MHC II- Ag complex with its T cell receptor (TCR) as well as several costimulatory interactions take place. They start a cross-talk with each other where APCs release interleukins while on the other hand, T cells secrete cytokines and interferons which induce their differentiation into subsets of effector T cells. T cell secretes IL-1 which signals activation of helper T cells and IL-2 which results in the proliferation of cytotoxic T cells and B cells. These are associated with not only promoting cellular immunity but also humoral immunity indirectly as TH cells stimulate B cells and their differentiation into plasma and memory cells. TC cells secrete cytotoxins and perforins that destroy pathogens or infected cells.
References
- Punt, J., Stranford, S. A., Jones, P. P., & Owen, J. A. (2019). Kuby Immunology. Macmillan Education.
- https://www.sciencelearn.org.nz/resources/178-the-body-s-second-line-of-defence
- https://bio.libretexts.org/Courses/Manchester_Community_College_(MCC)/Remix_of_Openstax%3AMicrobiology_by_Parker_Schneegurt_et_al/13%3A_Innate_Nonspecific_Host_Defenses/13.01%3A_1st_Line_defense-_Physical_and_Chemical_Defenses
- https://www.sciencelearn.org.nz/resources/177-the-body-s-first-line-of-defence
- https://ib.bioninja.com.au/standard-level/topic-6-human-physiology/63-defence-against-infectio/lines-of-defense.html
- https://universe-review.ca/R10-40-Immune.htm
- https://www.soinc.org/sites/default/files/uploaded_files/2018_IMMUNE_SYSTEM_HANDOUT.pdf
- https://www.austincc.edu/apreview/EmphasisItems/Inflammatoryresponse.html#ISF
- https://rsscience.com/white-blood-cells/
- https://www.immunology.org/public-information/bitesized-immunology/cells/
- https://www.khanacademy.org/science/high-school-biology/hs-human-body-systems/hs-the-immune-system/a/hs-the-immune-system-review
