- Escherichia coli (commonly abbreviated E. coli) is a Gram-negative, facultative anaerobic, rod-shaped bacterium that is commonly found in the lower intestine of warm-blooded organisms (endotherms).
- Human Escherichia coli strains are classified as commensal microbiota E. coli, enterovirulent E. coli, and extraintestinal pathogenic E. coli (ExPEC) on the basis of their genetic features and clinical outcomes.
- Most infections (with the exception of neonatal meningitis and gastroenteritis) are endogenous; that is, the E. coli that are part of the patient’s normal microbial flora are able to establish infection when the patient’s defenses are compromised (e.g., through trauma or immune suppression).
Escherichia coli as Pathogens
The effectiveness of E. coli as a pathogen is illustrated by the fact that:
- the bacteria are the most common gram-negative rods isolated from patients with sepsis
- responsible for causing more than 80% of all community-acquired UTIs as well as many hospital-acquired infections,
- a prominent cause of gastroenteritis.
Pathotypes of E. coli
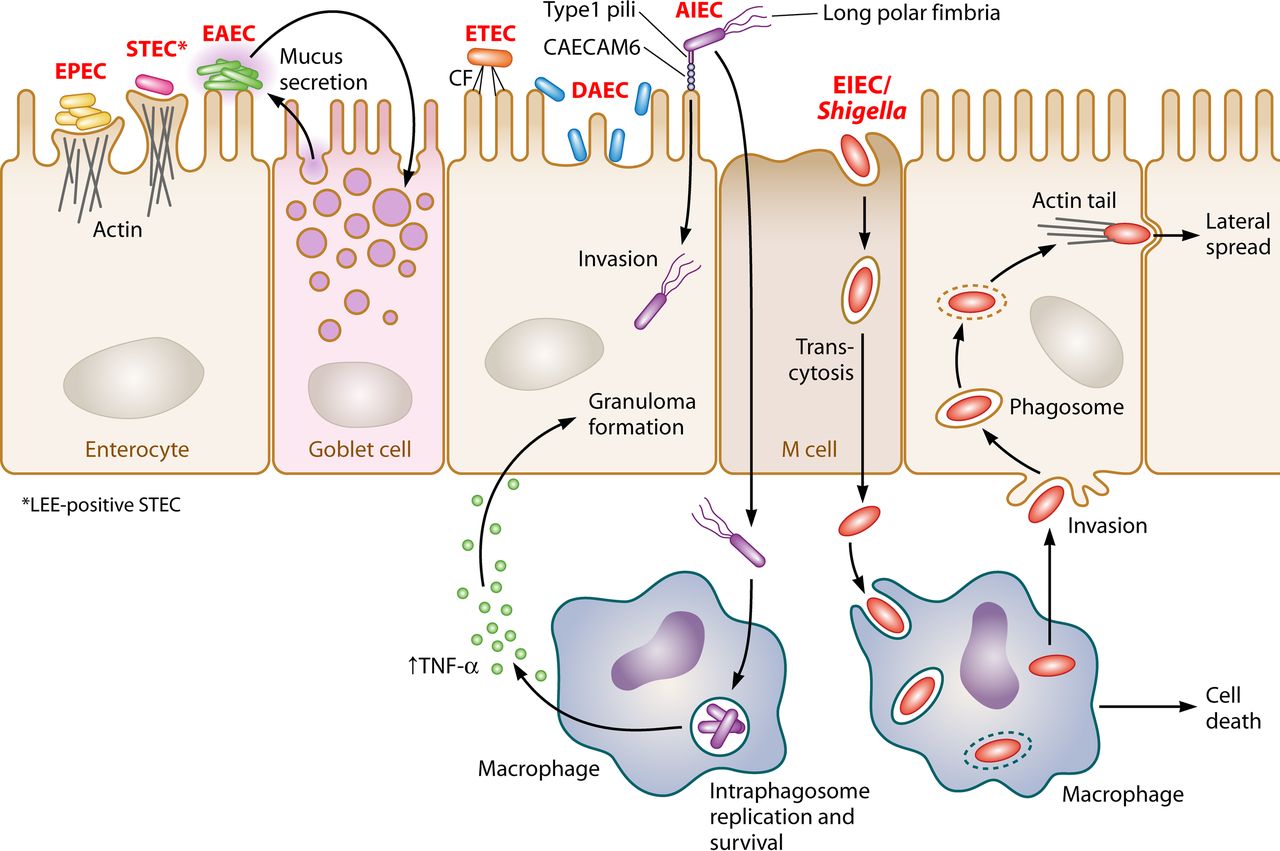
Source: DOI: 10.1128/CMR.00022-13
- The strains of E. coli that cause gastroenteritis are subdivided. For the pathogenic enteric E. coli strains, six pathotypes, i.e., enterotoxigenic E. coli (ETEC), enteropathogenic E. coli (EPEC), enterohemorrhagic E. coli (EHEC), enteroaggregative E. coli (EAEC), enteroinvasive E. coli (EIEC), and diffusely adhering E. coli (DAEC) are known.
- They are commonly referred to as the diarrheagenic E. coli .
- Diarrheagenic E. coli are antigenically distinct from the commensal E. coli which colonize the intestine. Only few serotypes of E. coli which express the enterotoxin or other virulence mechanisms can cause diarrhea.
- The different types are recognized on the basis of distinct epidemiological and clinical features, specific virulence determinants, and an association with certain serotypes.
A. Enterotoxigenic E. coli (ETEC)
- Enterotoxigenic E. coli (ETEC) is one of the most common causes of bacterial diarrheal disease in developing countries (estimated 840 million cases annually) and in an estimated 30% of travelers to these countries with diarrheal disease.
- It causes acute watery diarrhea in infants and adults.
- Because the inoculum for disease is high, infections are primarily acquired through consumption of fecally contaminated food or water. Person-to-person spread does not occur.
- Common serotypes associated are-06, 08, 0 15, 025, 0 27, 0 153, 0 159, etc.
- It is toxigenic, but not invasive.
- Pathogenesis of ETEC involves attachment to the intestinal mucosa mediated by fimbrial protein called CFA (colorlization factor antigen) and elaboration of heat-stable and heat-labile enterotoxins.
- ETEC produce two classes of enterotoxins: heat-stable toxins (STa and STb) and heat-labile toxins (LT-I, LT-II).
- Heat-stable toxin STa but not STb is associated with human disease, is found in 75% to 80% of ETEC either alone or associated with LT, and is responsible more commonly for severe disease than LT-only ETEC strains.
- Secretory diarrhea caused by ETEC develops after a 1- to 2-day incubation period and persists for an average of 3 to 5 days.
- The symptoms (watery, non-bloody diarrhea and abdominal cramps; less commonly nausea and vomiting) are similar to those of cholera but are usually milder, although mortality is high in malnourished individuals and in those with underlying diseases, particularly children and the elderly.
- Diagnosis is done by detection of toxins by in vitro and invivo methods.
B. Enteropathogenic E. coli (EPEC)
- Two groups of E. coli are responsible for enteric disease (Enteropathogenic E. coli [EPEC] and some Shiga toxin–producing E. coli [STEC]) possess a cluster of virulence genes located on a chromosomal pathogenicity island called the locus of enterocyte effacement (LEE).
- EPEC frequently causes infantile diarrhea (outbreaks) and occasionally cause sporadic diarrhea in adults.
- Disease is transmitted by fecal-oral exposure to contaminated surfaces or food products. Person-to-person spread is seen.
- However, it is non- toxigenic and non- invasive.
- Mechanism of diarrhea involves the adhesion to intestinal mucosa, mediated by plasmid coded bundle-forming pill, which form cup-like projections called pedestals.
- A/E lesions (attaching and effacing lesions) are produced on the intestinal epithelium (coded by chromosomal LEE gene, i.e. locus for enterocyte effacement); which leads to disruption of brush border epithelium causing increased secretion and watery diarrhea.
- The onset of disease may be as rapid as a few hours after ingestion of EPEC, and although most infections resolve after a few days, persistent diarrhea requiring hospitalization can occur.
C. Enteroaggregative E. coli (EAEC)
- Enteroaggregative E. coli (EAEC) are a heterogeneous collection of strains characterized by their autoagglutination in a “stacked-brick” arrangement over the epithelium of the small intestine and, in some cases, the colon. That is, it is so named because it adheres to HEP-2 cells in a distinct pattern, layering of the bacteria aggregated in a stacked-brick fashion.
- Most strains are “O” untypeable but “H “ typeable.
- The prevalence of disease caused by EAEC is unclear because a single molecular marker for these bacteria has not been discovered. Genes encoding adhesins, toxins including Shiga toxin, and other virulence proteins are highly variable among EAEC.
- The intestinal colonization is mediated by aggregative adhesion fimbriae I (regulated by aggR gene). It also produces EAST l toxin (entero-aggregative heat stable enterotoxin l).
- Manifestation of the disease include persistent and acute diarrhea are; especially in developing countries.
- These are one of the few bacteria associated with chronic diarrhea and growth retardation in children.
- E. coli 0104: H4 is an enteroaggregative strain that has caused major outbreaks in Germany in 2011. One peculiar feature of this strain is, it produces Shiga-like toxin and can cause HUS.
D. Shiga Toxin–Producing E. coli (STEC/VTEC/EHEC)
- Nomenclature for this group of E. coli is confusing, referring to them as Shiga toxin–producing E. coli (STEC), verocytotoxin-producing E. coli (VTEC), and enterohemorrhagic E. coli (EHEC).
- All members of this group are defined by the presence of Shiga toxin 1 (Stx1) or 2 (Stx2). Some but not all EHEC strains are LEE positive and form A/E cytopathology, resembling EPEC strains.
- Serotypes associated with EHEC are: 0157:H7 (most common serotype). Other serotypes are rarely associated such as 026:H11, 06, 055, 091, 0103, 0 111 and 0113.
- Diagnosis of STEC disease is now based on detection of the Shiga toxins rather than serotyping suspected isolates.
- STEC disease is most common in the warm months, and the highest incidence is in children younger than 5 years.
- Most infections are attributed to the consumption of undercooked ground beef or other meat products, water, unpasteurized milk or fruit juices (e.g., cider made from apples contaminated with feces from cattle), uncooked vegetables such as spinach, and fruits.
- Ingestion of fewer than 100 bacteria can produce disease, and person-to person spread occurs.
- Disease caused by STEC ranges from mild uncomplicated diarrhea to hemorrhagic colitis with severe abdominal pain and bloody diarrhea. Severe disease is more commonly associated with STEC O157:H7.
- Hemolytic uremic syndrome (HUS), a disorder characterized by acute renal failure, thrombocytopenia, and microangiopathic hemolytic anemia, is a complication in 5% to 10% of infected children younger than 10 years.
- Resolution of symptoms occurs in uncomplicated disease after 4 to 10 days in most untreated patients; however, death can occur in 3% to 5% of patients with HUS, and severe sequelae (e.g., renal impairment, hypertension, central nervous system [CNS] manifestations) can occur in as many as 30% of HUS patients.
E. Enteroinvasive E. coli (EIEC)
- Enteroinvasive E. coli (EIEC) strains are rare in both developed and developing countries.
- Pathogenic strains are primarily associated with a few restricted O serotypes: O124, O143, and O164.
- The strains are closely related by phenotypi and pathogenic properties to Shigella.
- The bacteria are able to invade and destroy the colonic epithelium, producing a disease characterized initially by watery diarrhea.
- A minority of patients progress to the dysenteric form of disease, consisting of fever, abdominal cramps, and blood and leukocytes in stool specimens.
- A series of genes on a plasmid mediate bacterial invasion (pInv genes) into the colonic epithelium.
- The bacteria then lyse the phagocytic vacuole and replicate in the cell cytoplasm.
- Movement within the cytoplasm and into adjacent epithelial cells is regulated by formation of actin tails (similar to that observed with Listeria).
- This process of epithelial cell destruction with inflammatory infiltration can progress to colonic ulceration.
F. Diffusely-adherent E. coli (DAEC)
- Recently, diffusely adherent E. coli (DAEC) strains have been recognized as the sixth class of diarrheagenic E. coli and appear as a heterogeneous group.
- It is characterized by the ability to adhere to HEp-2 cells in a diffuse pattern in which the bacteria uniformly cover the entire cell surface.
- It expresses diffuse adherence fimbriae which contribute to the pathogenesis.
- These strains are age dependently involved in diarrhea in children, are apparently not involved in diarrhea in adults, and can also be asymptomatic intestinal microbiota strains in children and adult.
- Hence, the pathogenesis and pathogenecity of the strains are still under question.
- DAEC is however thought to be capable of causing diarrheal disease, primarily in children aged 2-6 years.
References
- Murray, P. R., Rosenthal, K. S., & Pfaller, M. A. (2013). Medical microbiology. Philadelphia: Elsevier/Saunders
- Parija S.C. (2012). Textbook of Microbiology & Immunology.(2 ed.). India: Elsevier India.
- Sastry A.S. & Bhat S.K. (2016). Essentials of Medical Microbiology. New Delhi : Jaypee Brothers Medical Publishers.
- Scaletsky, I. C., Fabbricotti, S. H., Carvalho, R. L., Nunes, C. R., Maranhão, H. S., Morais, M. B., & Fagundes-Neto, U. (2002). Diffusely adherent Escherichia coli as a cause of acute diarrhea in young children in Northeast Brazil: a case-control study. Journal of clinical microbiology, 40(2), 645-8.
- https://cmr.asm.org/content/27/4/823
- https://bmcmicrobiol.biomedcentral.com/articles/10.1186/1471-2180-13-22
- https://cmr.asm.org/content/11/1/142
- https://nios.ac.in/media/documents/dmlt/Microbiology/Lesson-21.pdf
