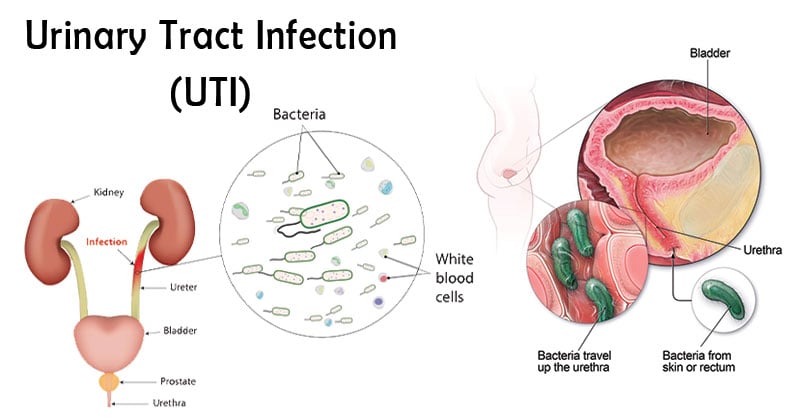
- A urinary tract infection (UTI) is an infection that affects part of the urinary tract. The urinary system is made up of the kidneys, ureters, the urinary bladder, and the urethra.
- Most UTIs are restricted to infection of the bladder (cystitis), though infection may occur in any area of the urinary tract, from the kidney to urethra.
- The presence of bacteria in urine is called bacteriuria. It is usually regarded as significant when the urine contains 105 organisms or more per ml (108/1) in pure culture.
- Infection of the bladder is called cystitis. It causes frequency, dysuria (pain on passing urine), suprapubic pain, sometimes haematuria and usually pyuria (increased number of pus cells in urine).
- The term acute urethral syndrome, (dysuria-pyuria) is used to describe acute cystitis accompanied by pyuria but in which no bacteria are detected by routine culture.
- Infection of the kidney is called pyelonephritis. It causes loin pain, pyuria, rigors, fever, and often bacteraemia.
- Most UTIs are caused by uropathogenic organisms from the gastrointestinal or vaginal florae that colonize the periurethral mucosa.
- Organisms are able to ascend through the urethra to the bladder by various mechanisms.
- Urinary tract infections (UTIs) are some of the most common bacterial infections, affecting 150 million people each year worldwide.
- They are thus a severe public health problem and are caused by a range of pathogens, but most commonly by Escherichia coli, Klebsiella pneumoniae, Proteus mirabilis, Enterococcus faecalis and Staphylococcus saprophyticus.
Types of UTI
Clinically, UTIs are categorized as uncomplicated or complicated.
Uncomplicated UTIs
They typically affect individuals who are otherwise healthy and have no structural or neurological urinary tract abnormalities; these infections are differentiated into lower UTIs (cystitis) and upper UTIs (pyelonephritis).
Uncomplicated cystitis rarely progresses to severe infection.
Complicated UTIs
Complicated UTIs are defined as UTIs associated with factors that compromise the urinary tract or host defence, including urinary obstruction, urinary retention caused by neurological disease, immune-suppression, renal failure, renal transplantation, pregnancy and the presence of foreign bodies such as calculi, indwelling catheters or other drainage devices.
Causative Agents of UTI
- UTIs are caused by both Gram-negative and Gram-positive bacteria, as well as by certain fungi.
- The most common causative agent for both uncomplicated and complicated UTIs is uropathogenic Escherichia coli (UPEC).
- For the agents involved in uncomplicated UTIs, UPEC is followed in prevalence by Klebsiella pneumoniae, Staphylococcus saprophyticus, Enterococcus faecalis, group B Streptococcus (GBS), Proteus mirabilis, Pseudomonas aeruginosa, Staphylococcus aureus and Candida spp.
- For complicated UTIs, the order of prevalence for causative agents, following UPEC as most common, is Enterococcus, K. pneumoniae, Candida spp., S. aureus, P. mirabilis, P. aeruginosa and GBS.
- UTI is typically caused by a single organism that is present in a high concentration, usually ≥ 105 CFU/ml.
- Polymicrobial infections may occur in patients with anatomical abnormalities or foreign bodies, but suspect colonization or culture contamination for cultures that yield growth of more than two different species.
General Pathogenesis
- The bacteria that cause urinary tract infections typically enter the bladder via the urethra. However, infection may also occur via the blood or lymph.
- It is believed that the bacteria are usually transmitted to the urethra from the bowel, with females at greater risk due to their anatomy.
- After gaining entry to the bladder, most agents are able to attach to the bladder wall and form a biofilm that resists the body’s immune response consequently resulting into an infection.
Symptoms of UTI
- Polyuria
- Hesitancy
- Incontinence
- Suprapubic pain
- Loin-to-groin pain e.g. flank and back
- Fever or chills
- Rigors
- Tachycardia
- Sepsis
Complications of UTI
- Persistent or recurrent urinary tract infection (UTI) can lead to renal failure.
- Permanent kidney damage from an acute or chronic kidney infection (pyelonephritis) due to an untreated UTI.
- Increased risk in pregnant women of delivering low birth weight or premature infants.
- Urethral narrowing (stricture) in men from recurrent urethritis, previously seen with gonococcal urethritis.
- Sepsis, a potentially life-threatening complication of an infection, especially if the infection works its way up the urinary tract to the kidneys.
Risk Factors
- Several risk factors are associated with cystitis, including female gender, a prior UTI, sexual activity, vaginal infection, obesity and genetic susceptibility.
- Pregnancy
- Urinary tract abnormality, including anatomical obstruction, indwelling foreign body, recent surgery, or instrumentation.
- Medical conditions, including diabetes, underlying renal disease, immunosuppression,
- History of complicated UTI, or recent hospitalization.
- Urinary tract infections occur more frequently in women than men due to the shortness of the female urethra. Moreover, Symptomatic and asymptomatic UTI is common in pregnancy.
- Risk of infection is increased when there is urine retention due to the bladder not emptying completely, or when urinary flow is obstructed due to renal stones, urinary schistosomiasis, enlarged prostate (commonest cause of recurring UTI in men), or tumour.
Diagnostic and Laboratory Findings
- Uncomplicated UTI can be reliably diagnosed on the basis of typical symptoms.
- Urinalysis and urine culture are not routinely needed; patients may be treated empirically.
- Uninalysis and urine culture should be performed for patients if complicated UTI is suspected, and for patients with symptoms of pyelonephritis.
Diagnostic Tests
- Urinalysis (dipstick or microscopic)
- Dipstick urinalysis performs best when urine culture yields growth >105 cfu/mL and dipstick shows positive leukocyte esterase and nitrite reactions (sensitivity 84%; specificity 98%).
- Most patients with UTI have pyuria (WBCs by microscopy or dipstick leukocyte esterase); WBC casts suggest pyelonephritis.
- Proteinuria and hematuria are also frequent findings.
- A positive dipstick nitrite reaction is typical for UTI caused by E. coli and other Enterobacteriaceae, but may be negative for other uropathogens, like Enterococcus.
- Gram stain
- Gram stain of an unconcentrated urine may be useful for detecting urine specimens that yield growth >105 cfu/mL, but are not reliable for detecting specimens that yield lower level, but significant growth.
- Because of the limited sensitivity for detecting significant cultures, and because of the labor intensity to perform, Gram staining is not recommended for urine specimens.
- Routine culture
- Quantitative culture is performed by inoculation of 1 microliter of urine onto SBA and selective (e.g. MacConkey or CNA) agar.
- The lower level of detection, therefore, is 103 cfu/mL.
- The extent of workup (identification and susceptibility testing) depends on several factors, including: type of specimen (clean catch versus invasively collected), number of species isolated (pure culture versus mixed), pathogenic potential of isolate (typical uropathogen versus common contaminant) and quantity of growth.
Culture for possible complicated UTI
- For symptomatic patients at risk for complicated UTI, bacteriuria at quantities <103-4 cfu/mL may predict significant UTI.
- For such patients, culture methods using a 10-microliter inoculum allow detection of growth at a lower detection limit of 102 cfu/mL.
- The extent of workup follows similar guidelines used for routine cultures, except that full ID and appropriate susceptibility testing is performed when one or two uropathogens are isolated in quantities >103 cfu/mL (versus the 104 cfu/mL cutoff used for routine cultures).
Note:
Urine culture may be normal in patients with renal or perinephric abscess if the infected tissue does not communicate with the collecting system. Drainage of such localized infections is performed for therapeutic reasons, as well as to collect material for culture, Gram stain and any other laboratory evaluation.
- Other Laboratory Testing
- Pregnancy testing may be appropriate for women presenting with otherwise uncomplicated UTI.
- In patients with complicated UTI, blood cultures are recommended for patients with fever, hypotension, or other signs of sepsis.
- Other laboratory testing appropriate for the clinical presentation is recommended.
Treatment of UTI
- The mainstay of treatment is antibiotics.
- However, antibiotics do not work for urethral syndrome because the antibiotics do not stay in the urethra long enough to be effective.
- Treatment is to increase fluid intake to flush bacteria out of the urethra.
UTI (Uncomplicated and Complicated)
- 1st line: PO Trimethoprim
- 2nd line (if 1st line contradicted) : PO Nitrofurantoin
- Pregnancy: PO Cephalexin
Pyelonephritis
- 1st line: IV Co-amoxidav + IV Gentamicin
- 2nd line (if 1st line contradicted) : PO or IV Ciprofloxacin + IV Gentamicin
- Pregnancy: IV Cefuroxime
- Complicated UTIs are more difficult to treat and usually requires more aggressive evaluation, treatment and follow-up.
- It may require identifying and addressing the underlying complication.
- Increasing antibiotic resistance is causing concern about the future of treating those with complicated and recurrent UTI.
Prophylaxis and Prevention
- Prophylactic antibiotics are used in children who experience recurrent UTIs in order to try and preserve renal function.
- Drinking plenty of fluids especially water.
References
- Cheesbrough M. (2006). District Laboratory Practice Tropical Countries,2nd Edition. Cambridge University Press.
- Williamson MA and Snyder LM. (2015). Wallach’s Interpretation of Diagnostic Tests Pathways to Arriving at a Clinical Diagnosis. TENTH EDITION. LWW: Philadelphia
- Flores-Mireles AL, Walker JN, Caparon M, Hultgren SJ. Urinary tract infections: epidemiology, mechanisms of infection and treatment options. Nat Rev Microbiol. 2015;13(5):269-84.
- http://www.microbiologynutsandbolts.co.uk/urinary-infections.html
- Hay AD, Birnie K, Busby J, et al.; on behalf of the DUTY team. The Diagnosis of Urinary Tract infection in Young children (DUTY): a diagnostic prospective observational study to derive and validate a clinical algorithm for the diagnosis of urinary tract infection in children presenting to primary care with an acute illness. Southampton (UK): NIHR Journals Library; 2016 Jul. (Health Technology Assessment, No. 20.51.) Chapter 4, Microbiological diagnosis of urinary tract infection by NHS and research laboratories. Available from: https://www.ncbi.nlm.nih.gov/books/NBK373515/
- http://www.helenacollege.edu/library/docs/ResearchPapers/LibraryResearchWinner_Sturdevant_Spring2016.pdf
- https://www.mayoclinic.org/diseases-conditions/urinary-tract-infection/symptoms-causes/syc-20353447
- http://www.columbia.edu/itc/hs/medical/pathophys/id/2008/utiBW.pdf

I agree with you
Please edit the notes with addition of significant bacteriuria counting methods.