Through normal everyday activities, the human body is exposed to microorganisms in the environment. Hundreds of species and countless individual microbial cells, collectively called the normal microflora, grow on or in the human body. This is the human microbiome, the sum total of all microorganisms that live on or in the human body.
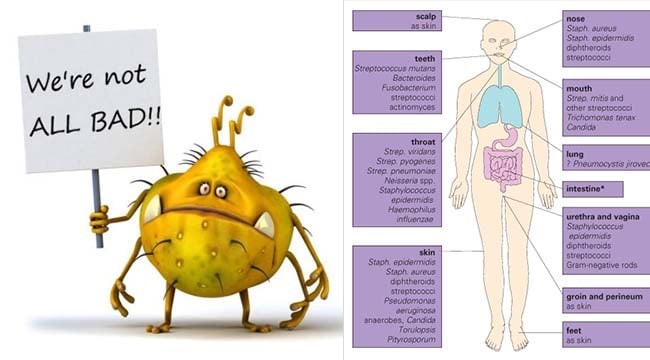
- The normal microflora have developed a symbiotic relationship with the mammalian host.
- They contribute to the health and wellbeing of the host by producing beneficial microbial products and inhibiting growth of dangerous microorganisms.
- In turn, the host contributes various micro-environments that support microbial growth.
- The normal microflora are first introduced at birth.
Normal Microbiota of the Skin
- The skin is the human body’s largest organ, colonized by a diverse array of microorganisms, most of which are harmless or even beneficial to the host.
- Because of its constant exposure to and contact with the environment, the skin is particularly
apt to contain transient microorganisms. - Nevertheless, there is a constant and well-defined resident flora, modified in different anatomic areas by secretions, habitual wearing of clothing, or proximity to mucous membranes (mouth, nose,
and perineal areas). - The predominant resident microorganisms of the skin are:
- Staphylococcus epidermidis
- Staphylococcus aureus (in small numbers)
- Micrococcus species
- α-Hemolytic and nonhemolytic streptococci (eg, Streptococcus mitis)
- Corynebacterium species
- Propionibacterium species
- Peptostreptococcus species
- Acinetobacter species
- Small numbers of other organisms (Candida species, Pseudomonas aeruginosa, etc)
Normal Microbiota of Mouth and Upper Respiratory Tract
- The flora of the nose consists of prominent corynebacteria, staphylococci (S epidermidis, S aureus), and streptococci.
- In direct contrast to the highly differentiated communities of their mothers, neonates harbored bacterial communities that were undifferentiated across multiple body habitats, regardless of delivery mode.
- Thus, at its earliest stage of community development (<5 minutes postdelivery), the human
microbiota is homogeneously distributed across the body. - Vaginally delivered infants harbor bacterial communities (in all body habitats) that are most similar in composition to the vaginal communities of the mothers; C-section babies lack bacteria from the vaginal community (eg, Lactobacillus, Prevotella, Atopobium, and Sneathia spp.).
- Infants delivered via C-section harbor bacterial communities (across all body habitats) that are most similar to the skin communities of the mothers (eg, Staphylococcus, Corynebacterium, or Propionibacterium spp.).
- Early in life, aerobic and anaerobic staphylococci, gram-negative diplococci (Neisseriae, Moraxella catarrhalis), diphtheroids, and occasional lactobacilli are added.
- When teeth begin to erupt, the anaerobic spirochetes, Prevotella species (especially Prevotella melaninogenica), Fusobacterium species, Rothia species, and Capnocytophaga species establish themselves along with some anaerobic vibrios and lactobacilli.
- Actinomyces species are normally present in tonsillar tissue and on the gingivae in adults, and
various protozoa may also be present. - Yeasts (Candida species) occur in the mouth.
- The predominant organisms in the upper respiratory tract, particularly the pharynx, are non-hemolytic and α-hemolytic streptococci and Neisseriae. Staphylococci, diphtheroids, haemophili, pneumococci, mycoplasmas, and prevotellae are also encountered.
Normal Microbiota of the Intestinal Tract
- The human gastrointestinal tract is divided into sections, allowing digestion and nutrient absorption in the proximal region to be separate from the vast microbial populations in the large intestine.
- At birth, the intestine is sterile, but organisms are soon introduced with food.
- The environment (eg, maternal vaginal, fecal, or skin microbiota) is a major factor in determining the early microbial profile.
- Many early studies reported that the intestinal microbiota of breastfed children is dominated by Bifidobacteria.
- However, recent studies employing microarrays and quantitative PCR suggested that in most babies, Bifidobacteria did not appear until several months after birth and thereafter persisted as
a minority population. - In bottle-fed children, a more mixed flora exists in the bowel, and lactobacilli are less prominent.
- As food habits develop toward the adult pattern, the bowel flora changes.
- Diet has a marked influence on the relative composition of the intestinal and fecal flora.
- For example, individuals on an animal-based diet have been shown to have an increased abundance of bile-tolerant microorganisms (Alistipes, Bilophilia, and Bacteroides) and decreased levels of Firmicutes that metabolize dietary plant polysaccharides (Roseburia, Eubacterium rectale, and Ruminococcus bromii).
- Bowels of newborns in intensive care nurseries tend to be colonized by Enterobacteriaceae, such as Klebsiella, Citrobacter, and Enterobacter.
- From the hundreds of phylotypes detected in the human stomach, only Helicobacter pylori persists in this environment.
- In the upper intestine, the bacterial population associated with the mucosa include the phylum Bacteroidetes and members of the Clostridiales, and those of the lumen can include members of the Enterobacteriales and enterococci.
- In a normal adult colon, 96–99% of the resident bacterial flora consists of anaerobes.
- Six major phyla predominate; these are Bacteroidetes, Firmicutes, Actinobacteria, Verrucomicrobiota, Fusobacteria, and Proteobacteria.
Normal Microbiota of the Urethra
- The anterior urethras of both sexes contain small numbers of the same types of organisms found on the skin and perineum.
- In the anterior urethra of humans, S. epidermidis, enterococci, and diphtheroids are found frequently; E. coli, Proteus, and Neisseria (nonpathogenic species) are reported occasionally (10 to 30 percent).
- Because of the normal flora residing in the urethra, care must be taken in clinically interpreting urine cultures; urine samples may contain these organisms at a level of 104/ml if a midstream (clean-catch) specimen is not obtained.
Normal Microbiota of the Vagina
- Soon after birth, aerobic lactobacilli appear in the vagina and persist as long as the pH remains acidic (several weeks).
- When the pH becomes neutral (remaining so until puberty), a mixed flora of cocci and bacilli is present.
- At puberty, aerobic and anaerobic lactobacilli reappear in large numbers.
- After menopause, lactobacilli again diminish in number, and a mixed flora returns.
- The normal vaginal flora includes group B streptococci in as many as 25% of women of childbearing age.
- The normal vaginal flora often also includes α-hemolytic streptococci, anaerobic streptococci
(peptostreptococci), Prevotella species, clostridia, Gardnerella vaginalis, Ureaplasma urealyticum, and sometimes Listeria or Mobiluncus species. - The cervical mucus has antibacterial activity and contains lysozyme.
- In some women, the vaginal introitus contains a heavy flora resembling that of the perineum and perianal area.
- This may be a predisposing factor in recurrent urinary tract infections.
- Vaginal organisms present at time of delivery may infect the newborn (eg, group B streptococci).
Normal Microbiota of the Conjunctiva
- The predominant organisms of the conjunctiva are diphtheroids, S epidermidis, and nonhemolytic streptococci.
- Neisseriae and gram-negative bacilli resembling haemophili (Moraxella species) are also frequently present.
- The conjunctival flora is normally held in check by the flow of tears, which contain antibacterial lysozyme.

thanks alot …this helps alot 😊
Very detailed and insightful. Thank you
EXCELLENT STUDY MATERIALS FOR STUDENTS AND FACULTY ALSO FOR REMEMBRING AND PREPARING ALSO ACHEVING ACADEMIC SUCCESS.