- Enterotoxigenic E. coli (ETEC) is defined as containing the E. coli strains that elaborate at least one member of two defined groups of enterotoxins: heat-stable toxin (ST) and heat-stable toxin (LT).
- Enterotoxigenic Escherichia coli, or ETEC, is thus the name given to a group of E. coli that produces special toxins that stimulate the lining of the intestines causing them to secrete excessive fluid, producing diarrhea.
- ETEC strains were first recognized as causes of diarrheal disease in piglets, where the disease continues to cause lethal infection in newborn animals.
- Common serotypes associated are-06, 08, 0 15, 025, 0 27, 0 153, 0 159, etc.
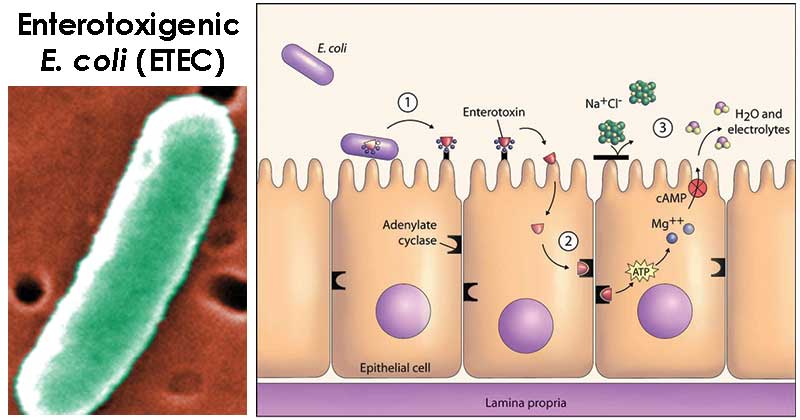
Image Source: CDC and Johns Hopkins Bloomberg School of Public Health
Disease Caused
- Enterotoxigenic E. coli (ETEC) is one of the most common causes of bacterial diarrheal disease in developing countries and in an estimated 30% of travelers to these countries with diarrheal disease.
- The disease caused is named Traveler’s diarrhea and Weanling diarrhea (infant diarrhea) in developing countries.
Mode of Transmission
The infections are primarily acquired through consumption of fecally contaminated food or water. Person-to-person spread does not occur.
Toxins and Pathogenesis
Plasmid-mediated, heat-stable (ST) and heat-labile (LT) enterotoxins that stimulate hypersecretion of fluids and electrolytes/
- The organisms colonize the surface of the small bowel mucosa and elaborate their plasmid-encoded enterotoxins, giving rise to a net secretory state.
- ETEC strains cause diarrhea through the action of the enterotoxins LT and ST. These strains may express an LT only, an ST only, or both an LT and an ST.
- Disease requires bacterial attachment to the small bowel epithelium by bacterial surface proteins (colonization factors [CF]) and elaboration of heat-stable and heat-labile enterotoxins.
- The genes for the colonization factors and enterotoxins are encoded on a transmissible plasmid.
- The colonization factors are subdivided into families (CFA/I, CFA/II, CFA/IV are the most common) and further subdivided by their antigenic properties (coli surface antigens [CS]). More than 20 CS colonization factors have been described, and host specificity is defined by their affinity for receptors on host cells.
- ETEC produces two classes of enterotoxins: heat-stable toxins (STa and STb) and heat-labile toxins (LT-I, LT-II).
- Heat-stable toxin STa is only associated with human disease, is found in 75% to 80% of ETEC either alone or associated with LT, and is responsible more commonly for severe disease than LT-only ETEC strains.
- STa is a small monomeric peptide that binds to the transmembrane guanylate cyclase C receptor on the intestinal epithelium, leading to an increase in cyclic guanosine monophosphate (cGMP) and subsequent hypersecretion of fluids well as inhibition of fluid absorption.
- Of the heat-labile toxins, LT-I is more commonly associated with human disease. LT-I is functionally and structurally similar to cholera toxin (80% homology) and consists of one A subunit and five identical B subunits.
- The B subunits bind to the same receptor as cholera toxin (GM1 gangliosides), as well as other surface glycoproteins on epithelial cells in the small intestine. After endocytosis, the A subunit moves across the membrane of the vacuole and interacts with a membrane protein (Gs) that regulates adenylate cyclase. The net effect of this interaction is an increase in cyclic adenosine monophosphate (cAMP) levels, resulting in enhanced secretion of chloride and decreased absorption of sodium and chloride. These changes are manifested in watery diarrhea.
- Exposure to the toxin also stimulates prostaglandin secretion and production of inflammatory cytokines, resulting in further fluid loss.
Signs, Symptoms, and Complications
Illness develops 1-3 days after exposure and symptoms rarely last more than 3 weeks.
The characteristic symptoms include:
- Watery, non-bloody diarrhea
- Abdominal cramps
- Less commonly nausea and vomiting
Symptoms are similar to those of cholera but are usually milder, although mortality is high in malnourished individuals and in those with underlying diseases, particularly children and the elderly.
Diagnosis
Detection of ETEC has long relied on the detection of the enterotoxins LT and/or ST.
- Commercial immunoassays are available for detecting ST in clinical specimens and cultures.
- PCR assays used with clinical specimens.
Treatment
The illness usually lasts 3-4 days. Some infections may take a week or longer to resolve. Most patients recover with supportive measures alone and do not require hospitalization or antibiotics.
Prevention
Infection can be prevented by avoiding or safely preparing foods and beverages that could be contaminated with the bacteria, as well as washing hands with soap frequently.
For travelers in developing countries, ETEC infection can be prevented by avoiding foods and beverages that could be contaminated with bacteria.
References
- Murray, P. R., Rosenthal, K. S., & Pfaller, M. A. (2013). Medical microbiology. Philadelphia: Elsevier/Saunders
- Parija S.C. (2012). Textbook of Microbiology & Immunology.(2 ed.). India: Elsevier India.
- Sastry A.S. & Bhat S.K. (2016). Essentials of Medical Microbiology. New Delhi : Jaypee Brothers Medical Publishers.
- https://cmr.asm.org/content/11/1/142
- https://www.cdc.gov/ecoli/etec.html

Thank you so much