What is Streptococcus bovis?
Streptococcus bovis is a Gram-positive bacterium that belongs to the bovis/equinus complex of the viridans Streptococci.
- It is present in the gastrointestinal tract of humans as a normal inhabitant, along with other Streptococcus species. However, it is present in much fewer numbers than other such species.
- Previously S. equinus and S. bovis were considered as two separate species, but recent studies involving DNA–DNA hybridization have led to the recognition that the names Streptococcus equinus and Streptococcus bovis are subjective synonyms with the specific epithet Streptococcus equinus having priority.
- However, so far, this has not been adopted in clinical microbiology and the name ‘S. bovis‘ remains widely used.
- Despite being a commensal of the gastrointestinal tract in humans and other animals, S. bovis has been associated with numerous diseases, the most important being colorectal cancer.
- The species is one of the older members of the bovis group which has now been changed to bovis/ equinus complex because of the genetic similarity of the two species.
- The species ‘bovis‘ is taken from the Latin word ‘bovis’ which means cow, bull, or ox, indicating the primary host of the species.
- S. bovis was first isolated from the gastrointestinal tract of cattle or ruminants by Andrewes and Horder in 1906.
- It belongs to the Group D of the Lancefield antigen grouping and is considered one of the crucial etiologic agent in different Group D Streptococcus infections.
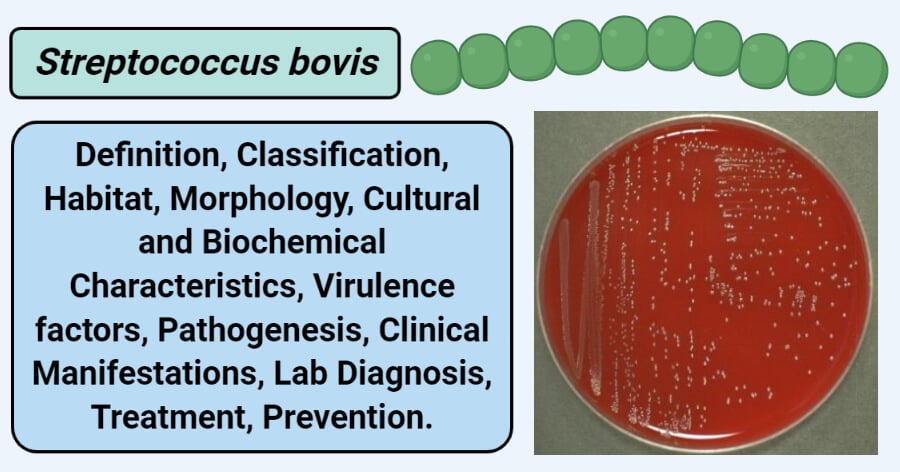
Image Source: Faculty of Health and Medical Sciences – University of Copenhagen – Denmark.
Classification of Streptococcus bovis
- The genus Streptococcus consists of more than 60 species and 12 subspecies that are closely related to other lactic acid bacteria that produce lactic acid as the sole or major end product during carbon metabolism.
- The family Streptococcaceae is present in the branch of Eubacteria within the low (< 50 mol%) G+C content based on their 16S rRNA gene sequence analysis.
- The primarily morphological characteristic of this genus is Gram-positive cocci arranged in the form of chains as a result of division on successive planes that are parallel to each other.
- S. bovis is one of the first species placed in the bovis group which was later renamed as bovis/equinus group because of the similarity between their gene sequences.
- It has been argued that S. bovis and S. equinus can be used as synonyms, and the use of S. equinus is more acceptable due to taxonomical priority.
- S. bovis is also a part of the viridans group Streptococci because of the production of the characteristic green colored zone by α-hemolysis on blood agar. It belongs to the Group D of the Lancefield antigen grouping.
The following is the taxonomical classification of S. bovis:
| Domain: | Bacteria |
| Phylum: | Firmicutes |
| Class: | Bacilli |
| Order: | Bacillales |
| Family: | Streptoococcaceae |
| Genus: | Streptococcus |
| Species: | S. bovis |
Habitat of Streptococcus bovis
- Streptococcus bovis is one of the regular inhabitants of the gastrointestinal tract of humans, but its number is relatively low when compared to other Streptococcus species.
- Besides, it has also been isolated from the alimentary tract of cows, horses, sheep, and other ruminants.
- The members of the bovis/ equinus complex are described as the colonizers of the rumen, crop, and cloaca of animals and colon of humans, with a fecal carriage rate of the members in humans ranging from 5% to over 60%.
- It is highly prevalent among most domesticated and wild animals, including bears, piglets, rodents, dogs, sea otters, and even some birds.
- The exact source of the organism not yet known, but these reach the gastrointestinal tract via the mouth. In some cases, S. bovis has also been isolated from the feces, but the transmission of bacteria via feces hasn’t been observed yet.
- Infections associated with S. bovis often result when the organism makes its way into the sterile parts of the body.
- The optimum temperature for the organism is the average body temperature of the host.
Morphology of Streptococcus bovis
- The cells of S. bovis are spherical or ovoid in shape with the diameter of the cells being about 0.8 to 1 µm.
- The cells are arranged in chains, mostly occurring in pairs to moderately long chains. Longer chains are seen with organisms cultured on liquid broth.
- The arrangement of the cells is due to the division of cells along successive planes that are parallel to each other like in rod-shaped cells.
- The organism is catalase-negative, facultative anaerobe, not capsulated, and usually carries sparsely distributed, long fibrils on the surface.
- The cell wall is made up of peptidoglycan and teichoic acid, along with different types of carbohydrates. The peptidoglycan type is Lys–Thr–Ala.
- The peptidoglycan consists of multiple glycan chains that are cross-linked through short peptides, and the individual glycan is made of alternating β-1,4-linked units of N-acetylglucosamine and N-acetylmuramic acid.
- The cell wall contains ribitol teichoic acid and lacks significant amounts of rhamnose, which is the primary sugar in some Streptococcus species. It contains phosphorylcholine residues in the teichoic acids of its cellular envelope.
Cultural characteristics of Streptococcus bovis
- Most Streptococcus species do not grow profusely on traditional media like Nutrient Agar and thus require media supplied with specific carbohydrates and nutrients.
- Media like Blood agar and Chocolate agar are commonly used in the identification of S. bovis by observing the pattern of hemolysis.
- For more selective isolation, media like Brain Heart Infusion Agar and Trypticase soy agar/broth with defibrinated sheep blood can be used.
- It is a facultative anaerobe, so abundant growth is observed in the air with 5% carbon dioxide at 37°C.
- No growth is seen at 10°C, but growth is positive at 45°C. The organism can tolerate 40% bile but cannot tolerate 6.5% NaCl and pH 9.6.
1. Nutrient Agar (NA)
- White to grey colored colonies of an average size of 1 mm in diameter. The colonies were round with raised elevation and an entire margin.
- Growth is mostly poor and requires air with supplied carbon dioxide.
2. Blood agar (BA)
- Typical smooth, non-pigmented, convex colonies with entire margin are observed on blood agar.
- Growth occurs readily on blood agar and exhibits various types of hemolysis, but mostly α-hemolysis. About 1-2 mm of a green-colored zone of hemolysis is observed on blood agar.
- Pronounced greening is observed on chocolate agar.
Biochemical characteristics of Streptococcus bovis
The biochemical characteristics of S. bovis can be tabulated as follows:
| S.N | Biochemical Characteristics | Streptococcus bovis |
| 1. | Capsule | No capsule |
| 2. | Shape | Cocci |
| 3. | Catalase | Negative (-) |
| 4. | Oxidase | Negative (-) |
| 5. | Citrate | Negative (-) |
| 6. | Methyl Red (MR) | Negative (-) |
| 7. | Voges Proskauer (VR) | Positive (+) |
| 8. | OF (Oxidative-Fermentative) | Facultative anaerobes |
| 9. | Coagulase | Negative (-) |
| 10. | DNase | Negative (-) |
| 11. | Clumping factor | Negative (-) |
| 12. | Gas | Negative (-) |
| 11. | H2O2 | Not determined |
| 12. | Hemolysis | α-hemolytic |
| 13. | Motility | Non-motile |
| 14. | Nitrate Reduction | Negative (-) |
| 15. | Gelatin Hydrolysis | Negative (-) |
| 16. | Pigment Production | Variable |
| 17. | Bile esculin test | Positive (+) |
| 18. | Ig A1 protease | Negative (-) |
| 19. | Urease | Negative (-) |
| 19. | Lancefield group | Group D |
Fermentation
| S.N | Substrate | S. bovis |
| 1. | Glucose | Positive (+) |
| 2. | Fructose | Positive (+) |
| 3. | Galactose | Positive (+) |
| 4. | Lactose | Positive (+) |
| 5. | Maltose | Positive (+) |
| 6. | Mannitol | Negative (-) |
| 7. | Mannose | Positive (+) |
| 8. | Raffinose | Variable |
| 9. | Ribose | Negative (-) |
| 10. | Sucrose | Positive (+) |
| 11. | Starch | Negative (-) |
| 12. | Trehalose | Variable |
| 13. | Xylose | Negative (-) |
| 14. | Salicin | Positive (+) |
| 15. | Glycerol | Negative (-) |
| 16. | Dulcitol | Negative (-) |
| 17. | Cellobiose | Positive (+) |
| 18. | Rhamnose | Negative (-) |
| 19. | Arabinose | Negative (-) |
| 20. | Inulin | Negative (-) |
| 21. | Sorbitol | Negative (-) |
| 22. | Pyruvate | Negative (-) |
| 23. | Glycogen | Negative (-) |
Enzymatic Reactions
| S.N | Enzymes | S. bovis |
| 1. | Acetoin | Positive (+) |
| 2. | Acid Phosphatase | Variable |
| 3. | Alkaline Phosphatase | Negative (-) |
| 4. | Ornithine Decarboxylase | Not determined |
| 5. | Hyaluronidase | Negative (-) |
| 6. | β-D-glucosidase | Positive (+) |
| 7. | Leucine aminopeptidase | Positive (+) |
| 8. | Neuraminidase | Not determined |
Virulence factors of Streptococcus bovis
- S. bovis is mostly a benign species that remain in the gut of animals as a commensal and helps prevent the colonization of different pathogenic microorganisms.
- However, it has various structures and proteins that support the colonization and invasion of host tissue surface in immune-compromised individuals.
- These structures not only help the organism make its way into the body and initiate invasion but also protect the organism from the host immune system.
- The exact mechanism of pathogenesis associated with S. bovis not yet known, which is why the virulence factors associated with such infections are also not entirely understood.
- The following are some of the factors that support the survival and growth of the organism inside the host’s body:
1. Adhesins/ Surface proteins
- Streptococcus bovis carries a number of genes coding for “microbial surface component recognizing adhesive matrix molecules” (MSCRAMM) and other adhesive proteins that can bind to components of the extracellular matrix (ECM) of host cells.
- These molecules remain on the cell wall of the organism and are specific to particular cells on the host’s body.
- Genomic sequences of S. bovis further support the existence of three pilus gene clusters assigned as pil1, pil2, and pil3, out of which Pil1 first virulence factor experimentally identified.
- Pil1 is responsible for binding to collagen, affected biofilm formation, and plays an essential role in the initial attachment and colonization stage of infective endocarditis.
- Furthermore, intestinal colonization by S. bovis is found to be dependent on Pil3 pilus, which assists bacterial attachment by binding to colonic mucus and fibrinogen in humans.
2. Biofilm
- Some strains of S. bovis are capable of forming biofilms around medical devices like catheters that might result in nosocomial or hospital-acquired infections.
- Biofilm formation provides protection to the bacteria as it works as a barrier against the immune cells as well as antimicrobial agents.
- The process of biofilm formation is assisted by the presence of fibrinogen-binding adhesions and several other enzymes.
3. Soluble cell-wall antigen
- In the case of colorectal cancer induced by S. bovis, soluble cell-wall antigens are found to play important roles in inducing inflammation and carcinogenic processes.
- These proteins or antigens induce interleukin-8 activity in different cells throughout the body. IL-8 is known to induce the over-expression of cyclooxygenase 2 (Cox-2) which in turn leads to increased levels of prostaglandin in Caro-2 cells.
- The increased formation of oxygen radicals and nitric oxide produces mutagenesis in the cells of the intestinal mucosa, which further promotes the induction of cancer.
Pathogenesis of Streptococcus bovis
Streptococcus bovis remains on the gastrointestinal tract of animals as a commensal but can cause different forms of infections. The exact mechanism of infection and pathogenesis of the disease is not yet clearly understood. Still, it has been assumed that biofilm formation is the major event that allows the growth and survival of the organism. Different virulence factors expressed by the organism aid in the process of pathogenesis.
1. Colonization
- The entry of the organism into the host body occurs through the mouth via different food materials.
- The bacteria then reaches the gastrointestinal area where it adheres to the epithelial cells of the mucosal layer of the tract.
- The attachment is initiated by the “microbial surface component recognizing adhesive matrix molecules” (MSCRAMM) and other adhesive proteins that can bind to components of the extracellular matrix of the epithelial cells.
- The initial attachment is then followed by the binding of the pil1 protein that binds to the collagen of the cells and helps in further colonization of the tract.
- Attachment and colonization are the initial steps in the pathogenesis of the infections as it ensures that the organism can grow, reproduce, and maintain the invasion.
2. Invasion
- Colonization of the intestinal tract is then followed by invasion where the bacteria invades the deeper tissue, ultimately reaching the bloodstream and causing infections in different parts of the body.
- Mucosal disruption allows the bacteria to enter the deeper tissues and the bloodstream, from where they reach the heart valves and cause infective endocarditis.
- The bacteria can uniquely colonize the thrombin present on the platelets and fibrin, and the bacterial colonies develop with protection from new layers of platelets and fibrin that are formed by stimulation from thromboplastin.
- The interaction of Pil1 and Pil3 with components of the intrinsic coagulation pathway induces the coagulation of blood which is an essential event during endocarditis.
- Besides, detection of bacteria by the immune system initiates an inflammatory response which further affects the heart valves and surrounding areas.
- Meanwhile, soluble cell-wall proteins produced by S. bovis induce the release of IL-8, which causes the over-expression of cyclooxygenase 2 (Cox-2).
- This, together with the inflammatory response induces the increased formation of oxygen radicals and nitric oxide in the body. The increased levels of these chemicals result in mutagenesis that ultimately leads to cancer.
- Thus, S. bovis bacteria are engaged in inducing severe inflammatory reactions in colorectal mucosa, causing the release of inflammatory and angiogenic cytokines leading to the formation of free radicals that are involved in the development of all types of human cancers.
Clinical manifestations of Streptococcus bovis
S. bovis was previously considered as a lower grade pathogen frequently involved in bacteremia and endocarditis. Besides infective endocarditis, the possibility of infections by S. bovis in various sites outside the colorectum such as osteomyelitis, discitis, and neck abscess has also been suggested. Depending on the geographic location of the patients, other forms of infections like colorectal adenoma, cholecystitis, cholangitis, and biliary tract diseases have also been associated with S. bovis.
1. Infective endocarditis
- Infective endocarditis is one of the infections associated with S. bovis where the organism induces coagulation of blood by binding to fibrinogen-binding proteins and collagen present in the blood.
- The organism moves through the blood and can bind to a pre-existing injury to the endothelium that might expose extracellular matrix components such as fibronectin, laminin, and collagen.
- Patients with endocarditis experience flu-like symptoms, including chills and fever.
- Chest pain and changed heart murmur are also typical.
- Endocarditis and bacteremia are found to be closely associated with colon cancer.
2. Malignancies
- S. bovis bacteremia is associated with malignancy irrespective of the site with about 29% of patients with positive S. bovis bacteremia harboring tumor lesions in the colon, duodenum, gallbladder, pancreas, ovary, uterus, lung, or hematopoietic system.
- As a result of the chronic inflammation and production of carcinogenic metabolites, lesions are formed in the colorectal area, which induces the malignancy of such organs.
Lab diagnosis of Streptococcus bovis
Lab diagnosis of infections caused by S. bovis begins with the collection of samples, which in this case, is blood. The first observation is a direct examination of these samples under the microscope. The diagnosis is mostly related to the identification of the organism; thus, it is mostly centered on the isolation and detection of the organism.
1. Cultural characteristics and Biochemical characteristics
- Culturing the organism on different selective media and observing the colony morphology on these media provides a basis for the identification of the organism.
- This also narrows the scope of diagnosis and makes the process more feasible.
- Isolation of the organism from primary clinical specimens is achieved on selective culture media like blood agar supplemented with 5 percent sheep blood, following an incubation period of 18–24 h in the air at 35–37°C.
- The isolated colonies are then subjected to different biochemical tests which help in the species determination.
- Depending on the microscopic observation, colony morphology, and biochemical tests, S. bovis can be detected.
2. Rapid identification kits
- Many clinical laboratories have started to employ different commercial identification kits or automated instruments that allow rapid determination of bacterial species.
- Microbial cellular fatty acid compositions are used for the identification of Streptococcal species.
- Some of the common automated systems for Streptococcal species identification include MicroScan Conventional Pos ID, Rapid Pos ID and BBL Crystal Gram-Pos ID.
3. Molecular diagnosis
- Molecular methods of diagnosis of bacteria usually include tests that help in the identification of the organism at a molecular level.
- This method utilizes the unique set of nucleic acid sequences present in each organism which provides a more detailed and accurate identification.
- One of the most important molecular methods is Polymerase Chain Reaction (PCR) which helps in the amplification and detection of bacterial DNA.
- Besides, DNA sequencing is performed to determine the DNA sequence of the bacteria that can then be used for its identification.
- Ribotyping is yet another molecular method that involves rRNA restriction fragment polymorphism methods.
Treatment of Streptococcus bovis
- Most S. bovis isolates are susceptible to penicillin (MIC ≤ 0.1 mg/L) and should be treated with intravenous penicillin G or ceftriaxone for four weeks.
- An alternative for only uncomplicated cases of native-valve endocarditis is a 2-week course of therapy with a combination of penicillin G or ceftriaxone and gentamicin.
- The treatment is comparatively easy as the infections are mostly mild, and most members of S. bovis are susceptible to most antibiotics.
- However, in the case of infective endocarditis, removal of implant valves or surgery might be required.
- If left untreated or in the case of late diagnosis, the lesions in the mucosal layer might become malignant and require extensive treatments.
References
- Topley WWC (2007). Topley and Wison’s Microbiology and Microbial Interactions; Bacteriology, 2 Vol. Tenth Edition. John Wiley and Sons Ltd.
- Bergey, D. H., Whitman, W. B., De, V. P., Garrity, G. M., & Jones, D. (2009). Bergey’s manual of systematic bacteriology: Vol. 3. New York: Springer.
- Abdulamir, A. S., Hafidh, R. R., & Abu Bakar, F. (2011). The association of Streptococcus bovis/gallolyticus with colorectal tumors: the nature and the underlying mechanisms of its etiological role. Journal of experimental & clinical cancer research : CR, 30(1), 11. https://doi.org/10.1186/1756-9966-30-11
- Papadimitriou K. (2018). Novel insight into the pathogenicity of Streptococcus gallolyticus subsp. gallolyticus belonging to the Streptococcus bovis/Streptococcus equinus complex. Virulence, 9(1), 662–665. https://doi.org/10.1080/21505594.2018.1432932
- Herrera, P., Kwon, Y. M., & Ricke, S. C. (2009). Ecology and pathogenicity of gastrointestinal Streptococcus bovis. Anaerobe, 15(1-2), 44–54. doi:10.1016/j.anaerobe.2008.11.003
- Abdul Azeez Ahamed Riyaaz, Randula Samarasinghe, Kolitha Sellahewa, Sabaratnam Sivakumaran, Manjula Sri Tampoe, “Native Valve Streptococcus bovis Endocarditis and Refractory Transfusion Dependent Iron Deficiency Anaemia Associated with Concomitant Carcinoma of the Colon: A Case Report and Review of the Literature”, Case Reports in Infectious Diseases, vol. 2016, Article ID 2670307, 4 pages, 2016. https://doi.org/10.1155/2016/2670307
- Pompilio, A., Di Bonaventura, G., & Gherardi, G. (2019). An Overview on Streptococcus bovis/Streptococcus equinus Complex Isolates: Identification to the Species/Subspecies Level and Antibiotic Resistance. International journal of molecular sciences, 20(3), 480. https://doi.org/10.3390/ijms20030480
- Salah Shanan, Samia A. Gumaa, Gunnar Sandström, Hadi Abd, “Significant Association of Streptococcus bovis with Malignant Gastrointestinal Diseases”, International Journal of Microbiology, vol. 2011, Article ID 792019, 5 pages, 2011. https://doi.org/10.1155/2011/792019
- Jans, C., de Wouters, T., Bonfoh, B., Lacroix, C., Kaindi, D. W., Anderegg, J., Böck, D., Vitali, S., Schmid, T., Isenring, J., Kurt, F., Kogi-Makau, W., & Meile, L. (2016). Phylogenetic, epidemiological and functional analyses of the Streptococcus bovis/Streptococcus equinus complex through an overarching MLST scheme. BMC microbiology, 16(1), 117. https://doi.org/10.1186/s12866-016-0735-2.

Thank you very much ????????
Strep bovis is oxidase negative.
Thanks for the correction, It has been updated 🙂