What is Blood Agar?
Blood Agar is an enriched medium provided with multiple nutrients that generally comes as a basal media for the preparation of blood agar by supplementation with blood.
- Blood Agar comes as a basal medium that can be used as it is as a general growth medium. The basal medium can be either Columbia Agar or Tryptic Soy Agar.
- Blood agar is an excellent medium for the cultivation of fastidious bacteria that require particular nutrients and don’t profusely grow on general media like Nutrient Agar.
- About 5% of defibrinated mammalian blood (human, sheep, or horse) is added to the autoclaved basal media to prepare blood agar medium.
- It is an enriched medium that supports the growth of fastidious bacteria and inhibits the growth of some bacteria like Neisseria and Haemophilus.
- For the growth of these bacteria, the inhibitors in the blood must be deactivated by heated blood agar. The heated blood agar becomes Chocolate Agar which supports Neisseria and Haemophilus.
- One of the essential uses of blood agar is to observe the hemolysis caused by the growing bacteria, which can then be used for the identification of the organism.
- Blood agar is mostly used for the cultivation of pathogenic organisms that are capable of producing extracellular enzymes that cause hemolysis of the blood.
Composition of Blood Agar
Blood agar, like most other nutritional media, has one or more protein sources, salt, and beef extract for vitamins and minerals. Besides these components, 5% defibrinated mammalian blood is also added to the medium. The blood agar base is commercially sold by various vendors, or it can also be prepared in the laboratory if the necessary ingredients are available. The exact composition of the blood agar base is given below:
| S.N | Ingredients | Gram/liter |
| 1. | Peptone | 10.0 |
| 2. | Tryptose | 10.0 |
| 3. | Sodium chloride | 5.0 |
| 4. | Agar | 15.0 |
| Final pH at 25°C: 7.3 ±0.2 | ||
- To the base medium, 5% sterile mammalian blood is added after autoclaving and before pouring onto the plates.
Principle of Blood Agar
- Blood agar is an enriched nutritious medium that supports the growth of fastidious organisms by supplementing it with blood or as a general medium without the blood.
- The blood added to the base provides more nutrition to the medium by providing additional growth factors required for these fastidious organisms.
- The blood also aids in visualizing hemolytic reactions of different bacteria. The hemolytic reactions, however, depend on the type of animal blood used.
- Sheep blood is mostly used for Group A Streptococci as it provides the best results, but it fails to support the growth of Haemophilus haemolyticus. It is because sheep blood is deficient in pyridine nucleotides.
- The growth and hemolysis of H. haemolyticus are best with horse blood, and the pattern of hemolysis might even mimic Streptococcus pyogenes on sheep blood.
- Besides the blood used in the medium, peptone and tryptose provide carbon, nitrogen, amino acids, vitamins, and minerals required for the bacteria. Peptone and tryptose are water-soluble, which makes it easier for the organism to absorb the nutrients.
- Sodium chloride is added to the medium in order to maintain the osmotic equilibrium of the medium and prevent the change in pH of the medium during growth.
- The distilled water provides a medium to dissolve the nutrients so that it is easier for the bacteria to absorb them.
- Agar is the solidifying agent that provides a stable surface for the organism to grow on, which allows for the observation of colony morphology and enumeration of the organism.
- In some case, phenolphthalein phosphate is added to the medium for the detection of phosphate producing Staphylococci, with added salt and agar for assessment of surface contamination.
Blood Agar and Hemolysis
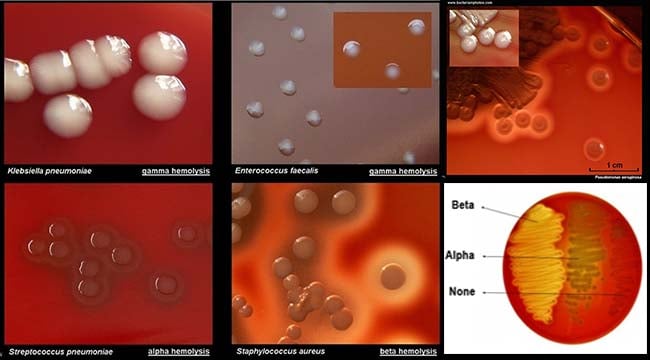
Hemolysis is the lysis of red blood cells in the blood due to the extracellular enzymes produced by certain bacterial species. The extracellular enzymes produced by these bacteria are called hemolysins which radially diffuse outwards from the colonies, causing complete or partial lysis of the red blood cells. Four different types of hemolysis are observed on blood agar which can each be identified by a zone of hemolysis present around the growing colonies.
1. Alpha hemolysis
- Alpha hemolysis is defined by a greenish-grey or brownish discoloration around the colony as a result of the partial lysis of the red blood cells.
- During α-hemolysis, H2O2 produced by the bacteria causes hemoglobin present in the RBC of the medium is converted into methemoglobin.
- Some of the α-hemolytic species are a part of the human normal flora, but some species like Streptococcus pneumonia cause pneumonia and other such severe infections.
2. Beta hemolysis
- Beta hemolysis is defined by a clear zone of hemolysis under and around the colonies when grown on blood agar.
- The clear zone appears as a result of the complete lysis of the red blood cells present in the medium, causing denaturation of hemoglobin to form colorless products.
- β-hemolytic bacteria include group A streptococci like S. pyogenes and group B streptococcus like S. agalactiae, both of which are associated with severe infections in humans.
3. Gamma hemolysis
- Gamma hemolysis is also called non-hemolysis as no lysis of red blood cells occurs.
- As a result, no change of coloration or no zone of hemolysis is observed under or around the colonies.
- Species like Neisseria meningiditis are non-hemolytic or gamma-hemolytic.
4. Alpha prime or wide zone alpha hemolysis
- Alpha prime hemolysis is defined by a small zone of intact erythrocytes adjacent to the bacterial colony, with a zone of complete lysis of RBCs surrounding the zone of intact erythrocytes.
- This might be confused with β-hemolysis due to the appearance of a clear zone around the colonies.
Preparation of Blood Agar
- About 40 grams of the prepared medium is added to 1000 ml distilled or deionized water.
- The suspension is heated up to boiling to dissolve the medium completely.
- It is then sterilized by autoclaving it at 15 lbs pressure and 121°C for about 15 minutes.
- The medium is then taken out of the autoclaved and cooled to about 40-45°C.
- To this, 5% v/v sterile defibrinated blood is added aseptically and mixed well.
- The media is then poured into sterile Petri plates under sterile conditions.
- Once the media solidifies, the plates can be placed in the hot air oven at a lower heat setting for a few minutes to remove any moisture present on the plates before use.
Storage of Blood Agar
- The media in the powder form should be stored between 10 to 30°C in a tightly closed container, and the prepared medium should be stored at 20-30°C.
- After opening, the product should be appropriately stored when dry, after tightly capping the bottle in order to prevent lump formation as the medium is hygroscopic in nature and thus, absorbs moisture relatively quickly.
- The container with the medium should be stored in a dry ventilated area protected from extremes of temperature and sources of ignition.
- The product should be used before the expiry date on the label.
Result Interpretation on Blood Agar
Image Source: https://www.microbiologyinpictures.com/index.php
The basal medium appears light amber colored which might look clear to slightly opalescent gel. After the addition of 5%, v/v sterile defibrinated blood; however, the cherry red-colored opaque gel is formed on the Petri plates. The following table demonstrates the growth of important medical bacteria with their colony morphologies on Blood Agar Medium:
S.N |
Organism |
Growth |
Colony Morphology |
Hemolysis |
| 1. | Neisseria meningiditis | Good-luxuriant | Grey and unpigmented colonies that appear round, smooth, moist, glistening, and convex, with a clearly defined edge. | Non-hemolytic or γ-hemolytic. |
| 2. | Salmonella Typhi | Good-luxuriant | Smooth colorless colonies that are smooth, moist, and flat with a diameter range of 2-4 mm. | Non-hemolytic or γ-hemolytic. |
| 3. | Staphylococcus aureus | Luxuriant | Golden yellow colored circular, convex and smooth colonies of the diameter range of 2-4 mm; opaque colonies with a zone of hemolysis. | β-hemolytic. |
| 4. | Staphylococcus epidermidis | Luxuriant | Circular, colonies of the size 1-4 mm in diameter; grey to white-colored with low convex elevation; moist, glistening colonies. | Non-hemolytic or γ-hemolytic. |
| 5. | Streptococcus pyogenes | Luxuriant | White-greyish-colored colonies with a diameter of > 0.5 mm; the colonies are surrounded by a zone of β-hemolysis that is often two to four times as large as the colony diameter. | β-hemolytic. |
| 6. | Streptococcus pneumonia | Luxuriant | small, grey, moist (sometimes mucoidal in encapsulated virulent strains), colonies with the characteristic zone of alpha-hemolysis (green); due to autolysis, often produces a dimple-like zone of hemolysis than the typical crater-like appearance. | α-hemolytic. |
| 7. | Pseudomonas aeruginosa
|
Good-luxuriant | Large colonies of the size 2-5mm in diameter; flat colonies that are grey to white-colored with an undulate margin with a zone of β-hemolysis. | β-hemolytic. |
Uses of Blood Agar
- The primary purpose of Blood agar is for the cultivation and isolation of fastidious organisms like Neisseria and Streptococcus.
- It can also be used for the differentiation of the bacteria-based type of hemolysis (α-, β- or γ-hemolytic) they produce on the agar.
- Blood agar can be used for the detection of phosphate-producing Staphylococci by adding phenolphthalein phosphate to the medium.
- Blood agar is often used for the preparation of Salmonella Typhi antigens.
- The blood agar base is considered a standard method for the analysis of food samples.
Limitations of Blood Agar
- The growth of Haemophilus hemolyticus is inhibited on Blood agar due to the presence of different inhibitors which can be deactivated only by heating the medium after the addition of the blood.
- The pattern of hemolysis might differ with the type of blood used.
- The addition of rabbit or horse blood to the basal medium supports the growth of H. hemolyticus, but the growth resembles that of Streptococcus species and thus should be confirmed.
References and Sources
- Blood Agar Base (Infusion Agar). M073. HiMedia Laboratories.
- Spellerberg B, Brandt C. Laboratory Diagnosis of Streptococcus pyogenes (group A streptococci) 2016 Feb 10. In: Ferretti JJ, Stevens DL, Fischetti VA, editors. Streptococcus pyogenes: Basic Biology to Clinical Manifestations [Internet]. Oklahoma City (OK): University of Oklahoma Health Sciences Center; 2016-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK343617/
- Li-li Zhu, Feng-cai Zou, Yu-lin Yan, Qi-hui Wang, Yong-qiang Shi, Wei-jie Qu, “The Characteristics of Staphylococcus aureus Small Colony Variant Isolated from Chronic Mastitis at a Dairy Farm in Yunnan Province, China”, The Scientific World Journal, vol. 2016, Article ID 9157605, 8 pages, 2016. https://doi.org/10.1155/2016/9157605
- https://www.cdc.gov/meningitis/lab-manual/chpt08-id-characterization-streppneumo.pdf
- https://www.cdc.gov/meningitis/lab-manual/chpt07-id-characterization-nm.html

thank you so much I really appreciate sir
Sir, Sagar, you are a great and sophisticate blog mentor to me, note only me but to everyone around the globe. Indeed, Your blog site have given me an incentive to improve academically.
Are there organisms that demonstrate Alpha prime or wide zone alpha hemolysis on blood agar which are different from those that demonstrate Alpha hemolysis?
Alpha-prime (α′) or wide-zone alpha hemolysis is generally considered a variant of alpha hemolysis rather than an entirely separate category. It is most commonly observed in certain strains of alpha-hemolytic streptococci (particularly some viridans group streptococci), rather than in a completely different set of organisms.
Hello guzs please explain the entercoccus like including spps
Bouis differentiate from other how
please what are the procedures for blood agar?
Good notes
Very good post, really appreciate your efforts keep it up
S.agalactiae is not a group A strep.
….it’s a group B STREP.
Both GAS & GBS exhibit B haemolysis
Hello, actually we mean to say Group A streptococci like S. pyogenes and S. agalactiae separately. We will make it more clear so that there will be no confusion. Thank you so much for the suggestions.
What indicator is used for blood agar?
No indicator separately used
We are adding Blood, itself act as indicator ,The microorganism utilizes the RBCs
based on Haemolysis
Thanks helpful presentation
How would you need to add to an agar-based medium to determine whether a microbe produced a hemolytic compound(s)?
Good job
That notes are simply understandable. Thanks to reminding for me..????????????
Plz give me makonky agar pripration
Dear Sagar, your posts are so appreciated. They are very relevant to the training we provide our Medical Technologists in South Africa. We find them so helpful and informative. Thank you. Keep it up!
Thank you so much for inspiring comments 🙂