- A microbe that is capable of causing disease is referred to as a pathogen.
- Pathogenicity is the ability of a microorganism to cause disease in another organism, namely the host.
- Pathogens vary in their ability to produce disease.
- The measurement of pathogenicity is called virulence, with highly virulent pathogens being more likely to cause disease in a host.
- “Virulence” is a quantitative measure of the pathogenicity of a micro-organism that may be expressed by the ratio of the number of individuals developing clinical illness to the number of individuals exposed to the micro-organism, or in a comparative manner, by the number of individuals that develop clinical illness if the same dose of different microorganisms is applied to each of them.
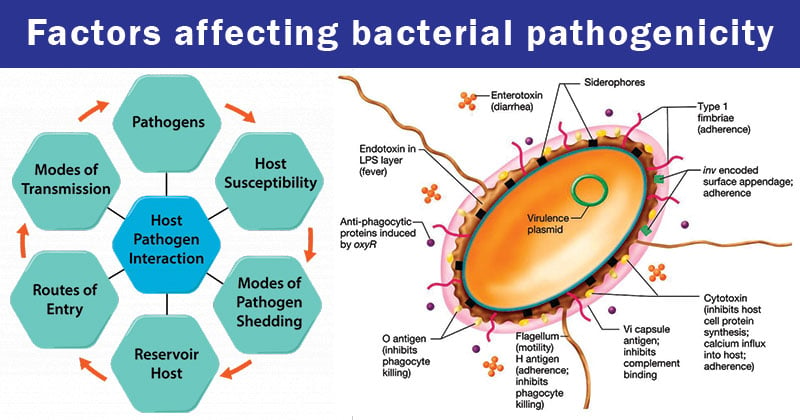
Factors determining Bacterial Pathogenicity
- Pathogenic bacteria have evolved a number of different mechanisms, which result in disease in the host.
- The virulence factors and determinants used by bacteria to interact with the host can be unique to specific pathogens or conserved across several different species or even genera.
- For instance, common mechanisms for adherence, invasion, evasion of host defenses and damage to host cells are shared by profoundly different microbial pathogens.
- However, a virulence factor can only contribute to the pathogenic potential of a bacterium in and as far as the micro-organism possesses the constellation of traits conducive to pathogenicity.
1. Host Susceptibility
- Susceptibility to bacterial infections depends on the physiologic and immunologic condition of the host and on the virulence of the bacteria.
- Before increased amounts of specific antibodies or T cells are formed in response to invading bacterial pathogens, the “nonspecific” mechanisms of host resistance (such as polymorphonuclear neutrophils and macrophage clearance) must defend the host against the microbes.
- Development of effective specific immunity (such as an antibody response to the bacterium) may require several weeks.
- The normal bacterial flora of the skin and mucosal surfaces also serves to protect the host against colonization by bacterial pathogens.
- Fortunately, most bacteria in the environment are relatively benign to individuals with normal immune systems.
- However, patients who are immunosuppressed, such as individuals receiving cancer chemotherapy or have AIDS, opportunistic microbial pathogens can establish life-threatening infections.
Example: In most healthy individuals, bacteria from the normal flora that occasionally penetrate the body (e.g., during tooth extraction or routine brushing of teeth) are cleared by the host’s cellular and humoral mechanisms. In contrast, individuals with defective immune responses are prone to frequent, recurrent infections with even the least virulent bacteria.
- A compromised physiologic and/or immunologic condition of the host thus aids the pathogenicity of pathogens.
2. Host Resistance
- Numerous physical and chemical attributes of the host protect against bacterial infection.
- These defenses include the antibacterial factors in secretions covering mucosal surfaces and the rapid rate of replacement of skin and mucosal epithelial cells.
- Once the surface of the body is penetrated, bacteria encounter an environment virtually devoid of free iron needed for growth, which requires many of them to scavenge for this essential element.
- Bacteria invading tissues encounter phagocytic cells that recognize them as foreign, and through a complex signaling mechanism involving interleukins, eicosanoids, and complement, mediate an inflammatory response in which many lymphoid cells participate.
3. Presence of Bacterial Virulence Factors
- In order for a bacterium to be virulent, it must have capabilities that allow it to infect a host.
- These capabilities arise from physical structures that the bacterium has or chemical substances that the bacterium can produce.
- Collectively the characteristics that contribute to virulence are called virulence factors.
- Bacterial pathogens have evolved specific virulence factors that allow them to multiply in their host or vector without being killed or expelled by the host’s defenses.
- Capsule: Bacterial capsules are protective coatings that surround the entire bacterial cell wall. They are composed of sugars except in the case of Bacillus anthracis whose capsule is composed of D-glutamine.
- Flagella: Flagella are long, whip-like proteinaceous filaments which are anchored within the bacterial cell wall and can extend several times the length of the bacteria itself. Rotation of bacterial flagella allows for bacterial movement, which is usually in the direction of nutrients.
- Pili: Pili are short, hair-like proteinaceous filaments, anchored to the bacterial cell wall, that extend only a short distance.
- Spores: Spores are small, metabolically inactive forms of bacteria that can survive for years. They contain little else beyond the bacterial genome, cell wall, and an extremely tough keratin-like outer coating.
- Toxins: These are proteins released by certain bacteria which can severely dysregulate critical cellular processes or improve the capacity of proteins to invade tissues.
- Siderophores: Siderophores are iron-binding factors that allow some bacteria to compete with the host for iron, which is bound to hemoglobin, transferrin, and lactoferrin.
- Other adherence, colonization factors, and invasion factors
4. Presence of Host-mediated Pathogenesis
- The pathogenesis of many bacterial infections cannot be separated from the host immune response, for much of the tissue damage is caused by the host response rather than by bacterial factors.
- Classic examples of host response-mediated pathogenesis are seen in diseases such as Gram-negative bacterial sepsis, tuberculosis, and tuberculoid leprosy.
- The tissue damage in these infections is caused by toxic factors released from the lymphocytes, macrophages, and polymorphonuclear neutrophils infiltrating the site of infection.
- Often the host response is so intense that host tissues are destroyed, allowing resistant bacteria to proliferate.
5. Ability for Intracellular Growth
- In general, bacteria that can enter and survive within eukaryotic cells are shielded from humoral antibodies and can be eliminated only by a cellular immune response.
- However, these bacteria must possess specialized mechanisms to protect them from the harsh effects of the lysosomal enzymes encountered within the cell.
References
- https://www.oecd-ilibrary.org/docserver/9789264253018 en.pdf?expires=1554285369&id=id&accname=guest&checksum=102B9FC7249C369C039F269E255730EF
- http://library.open.oregonstate.edu/microbiology/chapter/bacterial-pathogenicity/
- http://textbookofbacteriology.net/pathogenesis.html
- https://onlinelibrary.wiley.com/doi/pdf/10.1002/path.1700370204
- https://www.ncbi.nlm.nih.gov/books/NBK8526/
- http://www.pathwaymedicine.org/bacterial-virulence-factors

Help to shorten the sentences for easy understanding, help with WhatsApp number