Habitat of Candida albicans
- Normal Habitat: mucosal membranes of human and other warm blooded animals.
- Also found in the gut, the vagina or also in the surface of the skin.
- Found in the digestive tract of birds also.
- Isolated from soil, animal, hospitals, in-animate objects and food.
- Worldwide distribution
Morphology of Candida albicans
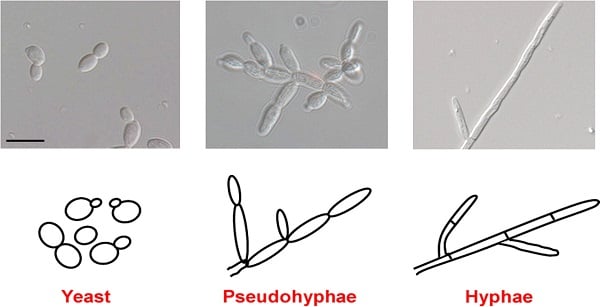
- Small, oval, measuring 2-4 µm in diameter.
- Yeast form, unicellular, reproduce by budding.
- Single budding of the cells may be seen.
- Both yeast and pseudo-hyphae are gram-positive.
- Encapsulated and diploid, also form true hyphae.
- Polymorphic fungus (yeast and pseudohyphal form)
- Can form biofilms
- Normal condition: Yeast
- Special condition (pH, Temperature): Pseudohyphae
- 80-90% of cell wall is carbohydrate
Cultural Characteristics of Candida albicans
SDA
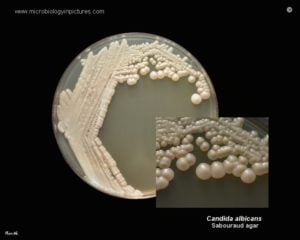
- Creamy, pasty colonies, smooth after 24-48 hours at 25-37°C
- Yeast smell (odour)
Blood Agar
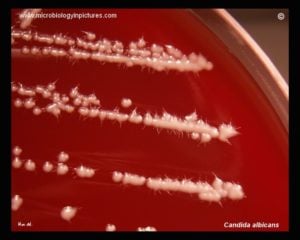
- White creamy colored
- Foot-like extensions from the margin.
PDA
- Smooth creamy colonies after 24-48 hours
CHROMAGAR
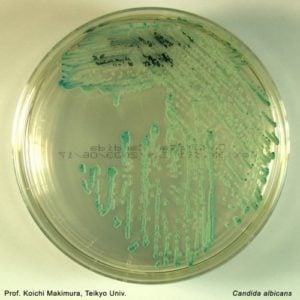
- Green colonies
Life Cycle of Candida albicans
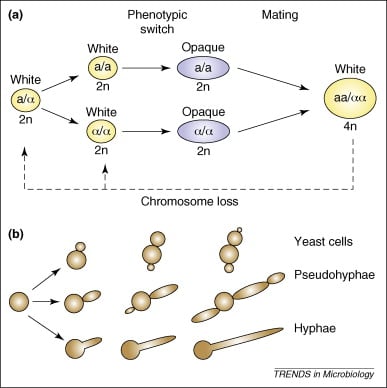
- Asexual and doesn’t perform meiosis
- Ability to grow with three distinct morphologies- yeast, pseudo-hyphae and true hyphae
- Para-sexual life cycle
- Switch between different phenotypes
- Efficient mating requires the diploid cells of opposite mating types first to switch from the more common “white” phase to the “opaque” phase and then undergo cell fusion.
- The resulting tetraploid strains can return to the diploid state via a non-meiotic parasexual program of concerted chromosome loss.
- White form: white and rounded cells forming dome-shaped colonies
- Opaque form: opaque, elongated cells forming a flatter colony.
- Opaque form is more efficient for mating than the white form
Pathogenesis of Candida albicans
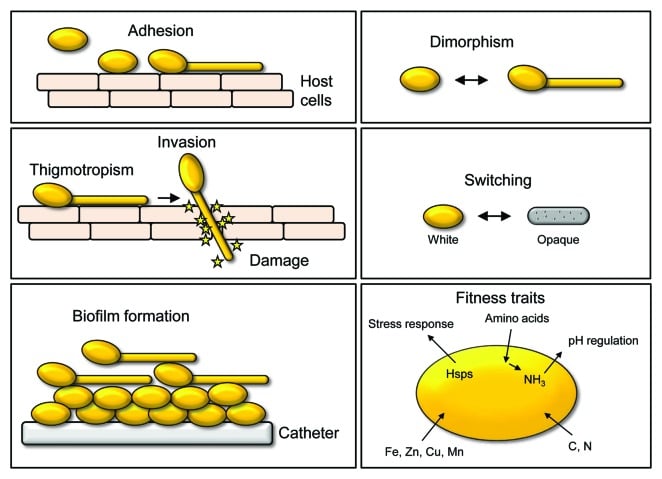
- Opportunistic fungal pathogen that causes candidiasis in human
- Occurs in immunocompromised peoples such as HIV infected, transplant recipients, chemotherapy patients, etc.
- Mode of transmission:
- Mother to infant through childbirth
- Rarely through sexual contact
- People to people transmission in hospital settings
Virulence Factors of Candida albicans
- Polymorphism
- Yeast, pseudohyphae and hyphae
- Hyphae is more important for infection
- Adhesins (Als 3 Protein)
- Sets of glycosylphatidylinositol (GPH)- linked cell surface glycoproteins that allow it to the surfaces of microorganisms
- Helps with biofilm formation also
- Invacins (Als 3 Protein)
- Helps with the invasion of C. albicans into host epithelial and endothelial cells.
- Ssa1 codes for heat shock protein
- Induces host cells to engulf the fungal pathogens
- Invasion by the active penetration of C. albicans into host cells by involving hyphae.
- Biofilm Formation
- Yeast cells à adherence à surface à development of hyphae cells à in the upper part of biofilm à leads to a more resistant mature biofilm à dispersion of yeast cell.
- Bcr1, Tec1 and Efg1 function as important transcriptional factors.
- Secreted hydrolases
- 3 main classes of hydrolases: proteases, phospholipases and lipases
- Helps in active penetration into host cells
- Helps in uptake of extracellular nutrients from the environment.
- 10 proteases (Sap 1-10), 4 major classes (A, B, C and D) of phospholipases and lipases consist of 10 members (LIP 1-10).
- Metabolic Adaption
- In the process of infection, it undergoes metabolic adoption such as their glycolysis, gluconeogenesis and starvation responses.
- Example: quickly switch from its glycolysis to starvation responses with the activation of glyoxylate cycle.
- Due to this, it can infect almost any organ through the blood stream.
Stages of Infection
- Colonization
- Epithelial adhesion
- Nutrient acquisition
- Superficial Infection
- Epithelial penetration
- Degradation of host protein
- Deep-Seated Infection
- Tissue penetration
- Vascular invasion
- Immune evasion or escape
- Disseminated Infection
- Endothelial adhesion
- Infection of other host tissues
- Activation of coagulation and blood clotting cascades.
Types of Candidiasis
Mucosal Candidiasis
- Oral candidiasis: mucous membrane of mouth
- Denture related stomatitis: mild inflammation and redness of oral mucous membrane beneath a denture.
- Angular cheilitis: inflammation of one or both corners of the mouth
- Median rhomboid glossitis: redness and loss of lingual papillae
- Vulvovaginitis: white lesions on the epithelial surfaces of vulva, vagina and cervix
- Balanitis: infection of glans penis
- Esophageal candidiasis: infection of esophagus painful swallowing.
Cutaneous Candidiasis
- Candida folliculitis: infection and inflammation of hair follicles, rash may appear as pimples.
- Candidal intertrigo: infection of skin located between intertriginous folds of adjacent skin.
- Candidal paronychia: inflammation of the nail fold.
- Perianal candidiasis: irritation of the skin at the exit of the rectum.
- Chronic mucocutaneous candidiasis: immune disorder of T cells, deficient of CMI.
- Congenital cutaneous candidiasis: skin condition in new borne babies caused by premature rupture of membranes together with a birth canal infected with C. albicans.
- Diaper candidiasis: infection of a child’s diaper area.
- Erosio interdigitalis blastomycetia: characterized by an oval shaped area of macerated white skin on the web between and extending onto the sides of the fingers.
- Candidal onychomycosis: nail infection
Systemic Candidiasis
- Candidemia: leads of sepsis
- Disseminated candidiasis (organs)
- Endocarditis
- Gastro intestinal tract infection
- Respiratory tract infection
- Genitourinary candidiasis
- Hepatosplenic candidiasis (Chronic Disseminated Candidiasis)
Lab Diagnosis of Candida albicans
Specimens: Exudates, Tissues, Scrapings
- Microscopy (Scraping)
- Examined in wet film in 10% KOH
- Visualization of pseudohyphae and budding yeast cells of candida
- Gram staining: Gram positive (+ve)
- Culture
- SDA: Creamy white, smooth colonies
- CHROMAGAR: Green colonies
- Identification of albicans
- Germ Tube Test: produce germ tube test within 2 hours when incubated in human serum at 37°C.
- Chlamydospores: produced by C. albicans on corn meal/rice agar at 25°C. They produces round thick walled chlamydospores borne terminally or laterally.
- Biochemical Tests: Glucose and maltose fermented with acid and gas production, sucrose and lactose not fermented, Pale pink coloration in Tetrazolium reduction medium
- Serology
- Limited specificity
- Serum antibodies and cell mediated immunity are demonstrable in most people because of life long exposure to C. albicans.
- C. albicans antigen is a delayed hypersensitivity skin test, which is used as an indicator of functions of the CMI.
- ELISA and RIA: detection of circulating Candidial antigen either cell wall mannan or cytoplasmic constituents.
- 1,3-beta-D-glucan assay
- Beta-D-glucan is a component of the cell wall of fungi.
- Detected by its ability to activate factor G of the horse-shoe crab coagulation cascade.
- Highly specific and sensitive test.
- DNA probe and PCR
Treatments of Candida albicans

- Oral candidiasis: Nystatin, miconazole, amphotericin B.
- Cutaneous candidiasis: Clotrimazole, econazole, ciclopirox, miconazole, ketoconazole, nystatin.
- Systemic and oral azoles: Fluconazole, itraconazole or posaconazole.
- Vulvovaginitis: single dose of oral fluconazole, topical antifungals (butoconazole, clotrimazole, miconazole, nystatin, ticonazole, terconazole).
- Blood infections: intravenous fluconazole or an echinocandin (caspofungin)
- Candidemia: Fluconazole and Anidulafungin
Prevention and Control of Candida albicans
- Keep healthy life style
- Good hygiene, proper nutrition, careful antibiotic use.
- Add probiotics, reduce sugar intake
- Wear cotton underwear and loose pants
- Change immediately wet clothes

Thank you very much. it is very useful information
Thanks it helps me alot to grasp the concept easily
‘Diploid Stage à form cells à homozygous à phenotypic switch from white to mating component ‘opaque’ cells à mating of opaque cells (cell fusion) à tetraploid cells à loss of chromosomes (splitting) à Diploid State’
This sentence is not clear
Thanks for the correction. The sentence has been made more clear now.
Thank you and may you please provide me with your reference in Havard style j don’t see any references
This information helped me but please help me to find references oh a havest form
So interested the pages and so rich in information concerning the PATHOLOGY
Much love bros indeed it’s really helpful.Thank you so much. Please need reference
I want your reference in Havard style j don’t see any references
Thanks very much. it helped
thank you so much.. it helped my degree program
Me too.Am persuing bachelors in nursing and you
Thank you very much, enjoyed and learnt a lot
Thank you much. This is very helpful.
nice,,i enjoyed the lesson
Nice bro .i am also completed my bsc mlt.u r giving good information to us.
Very good