Habitat of Bacillus cereus
- Bacillus cereus is isolated from soil, vegetables, milk, cereals, spices, fried rice, cooked poultry and meats, soups, and desserts.
- It is also found in mashed potatoes, beef stew, apples, hot chocolates sold in vending machines, and other improper food handling areas.
- In 1887, B. cereus was isolated from air in a cowshed by Frankland and Frankland.
- It is a saprophytic species of Bacillus.
- Vegetative cells and spores are widely distributed in nature.
- It is opportunistic pathogens to immunocompromised patients and sometimes pathogens of man.
- It is not considered as normal flora of humans but maybe transiently colonize skin or the gastrointestinal or respiratory tracts.
- Endospores show much greater resistance to physical and chemical agents such as heat, cold, desiccation, radiation, disinfection, antibiotics, and other toxins.
- It is able to grow either in the presence or in the absence of oxygen.
- It interacts with other microorganisms in the rhizosphere, the region surrounding plant roots.
- It is also found in the gut of microflora of invertebrates and is an intestinal symbiont of arthropods where it exhibits filamentous growth in sowbugs, roaches, and termites.
- Bacillus cereus are not easily killed by alcohol; in fact, they have been known to colonize distilled liquors and alcohol-soaked swabs and pads in numbers sufficient to cause infection.
- The presence of B. cereus in a patient’s stool is not sufficient to make a diagnosis of B. cereus because the bacteria may be present in normal stool specimens, a concentration of 105 bacteria or more per gram of food is considered diagnostic.
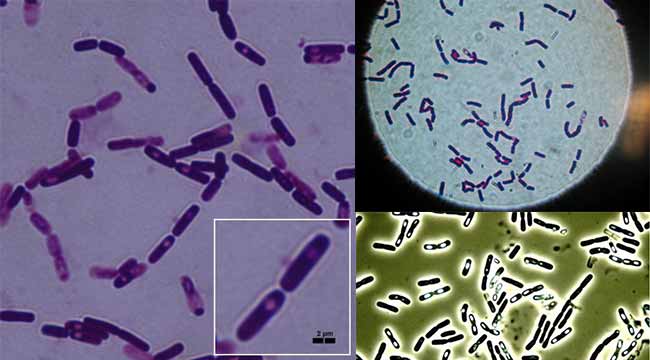
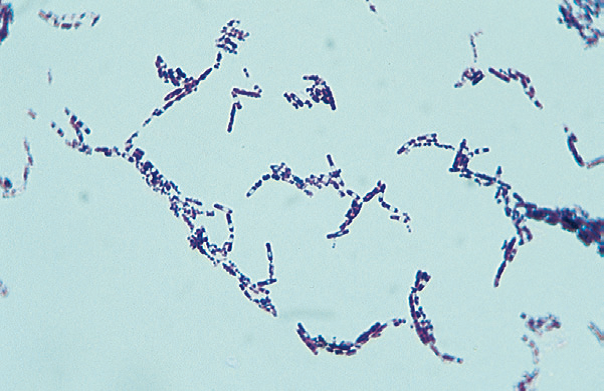
Morphology of Bacillus cereus
- Bacillus cereus is gram-positive rod-shaped bacilli with square ends.
- Occasionally may appear gram variable or even gram-negative with age.
- They are single rod-shaped or appear in short chains.
- Clear cut junctions between the members of chains are easily visible.
- Tissue section staining may appear long and filamentous.
- They are straight or slightly curved.
- They are non-capsulated.
- It contains spores with central spores.
- Spores are oval (ellipsoidal) and not swelling the mother cell, and not formed in the animal’s blood and tissues or in aerobic culture.
- It is 1×3-4 µm in size.
- It is motile and flagellated with peritrichous flagella.
- It is motile by two types of motility, swimming and swarming.
- Endospores are able to survive long periods of exposure to air and other adverse environmental conditions.
- It is a beta-hemolytic bacterium that causes foodborne disease.
- Its virulence factors include cerolysin and phospholipase.
Genome Structure
- The circular chromosome with 5,411,809 nt in length.
- It contains 5481 genes, 5234 proteins coding, 147 structural RNA, and 5366 RNA operons.
- The plasmid is 5 to 500 kb in size.
Cultural Characteristics of Bacillus cereus
- Most Bacillus spp grow readily on nutrient agar or peptone media.
- The optimum temperature for growth varies from 20°C to 40°C, mostly 37°C.
- B. cereus is mesophilic and is capable of adapting to a wide range of environmental conditions.
- On Nutrient Agar at 37°C, it forms large (2-5 mm) grey-white, granular colonies with a less wavy edge and less membranous consistency.
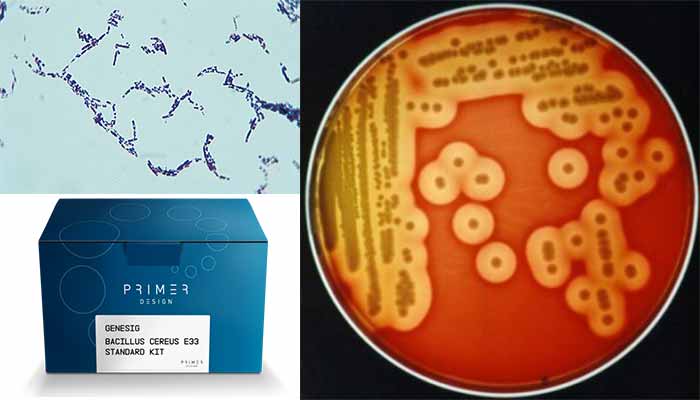
- On 5% sheep blood agar at 37°C, B. cereus colonies are large, feathery, dull, gray, granular, spreading colonies, and opaque with a rough matted surface and irregular perimeters.
- On blood agar, it is beta-hemolytic.
- Colony perimeters are irregular and represent the configuration of swarming from the site of initial inoculation, perhaps due to B. cereus swarming motility.
- In some instances, smooth colonies develop either alone or in the midst of rough colonies.
- When grown apart from the initial inoculum, smooth colonies are surrounded by a uniform zone of beta-hemolysis framing the centrally situated colony.
- The MYP agar has been the standard media for plating B. cereus, but it has little selectivity so background flora is not inhibited and can mask the presence of B. cereus. B. cereus colonies are usually lecithinase-positive and mannitol-negative on MYP agar.
- Bacara is a chromogenic selective and differential agar that promotes the growth and identification of B. cereus but inhibits the growth of background flora. Bacillus cereus colonies turn pink-orange with an opaque halo.
- The chromogenic agar has been suggested for the enumeration of the B. cereus group as a substitute for MYP. Typical colonies will grow as pink-orange uniform colonies surrounded by a zone of precipitation.
Biochemical Characteristics of Bacillus cereus
Pathogenicity and Virulence factors of Bacillus cereus
- B. cereus is most commonly associated with food poisoning, but the organism can also cause post-traumatic ophthalmitis, which requires rapid, aggressive management locally.
- The organism is widespread in the environment and is found in most raw foods, especially cereals such as rice.
- Gastroenteritis caused by B. cereus is mediated by one of two enterotoxins.
- The heat-stable, proteolysis-resistant enterotoxin causes the emetic form of the disease. The mechanism of action of the heat-stable enterotoxin is unknown.
- The emetic form is manifested by nausea, vomiting, abdominal cramps, and occasionally diarrhea and is self-limiting, with recovery occurring within 24 hours.
- The heat-labile enterotoxin causes the diarrheal form of the disease; each stimulates the adenylate cyclase–cyclic adenosine monophosphate system in intestinal epithelial cells, leading to profuse watery diarrhea.
- The diarrheal form has an incubation period of 1–24 hours and is manifested by profuse diarrhea with abdominal pain and cramps; fever and vomiting are uncommon.
B. cereus is the most commonly encountered species of Bacillus in opportunistic infections including posttraumatic eye infections, endocarditis, and bacteremia. The pathogenesis of B. cereus ocular infections is also incompletely defined.
- At least three toxins have been implicated; they are necrotic toxin (a heat-labile enterotoxin), cereolysin, and phospholipase C (a potent lecithinase).
- It is likely that the rapid destruction of the eye that is characteristic of B. cereus infections results from the interaction of these toxins and other unidentified factors. Bacillus species can colonize skin transiently and can be recovered as insignificant contaminants in blood cultures.
- In the presence of an intravascular foreign body, however, these organisms can be responsible for persistent bacteremia and signs of sepsis (i.e., fever, chills, hypotension, shock).
- Infections of other sites are rare and usually involve intravenous drug abusers or immunocompromised patients.
Clinical manifestation of Bacillus cereus
A. Food poisoning
Two forms of food poisoning: vomiting disease (emetic form) and diarrheal disease (diarrheal form).
- Emetic form
The emetic form of the disease results from the consumption of contaminated rice. Most bacteria are killed during the initial cooking of the rice, but the heat-resistant spores survive. If the cooked rice is not refrigerated, the spores germinate, and the bacteria can multiply rapidly. The heat-stable enterotoxin that is released is not destroyed when the rice is reheated. The emetic form of the disease is an intoxication, caused by the ingestion of the enterotoxin and not the bacteria. Thus the incubation period after eating the contaminated rice is short (1 to 6 hours), and the duration of illness is also short (less than 24 hours). Symptoms consist of vomiting, nausea, and abdominal cramps. Fever and diarrhea are generally absent.
- Diarrheal form
The diarrheal form of B. cereus food poisoning is a true infection, resulting from the ingestion of the bacteria in contaminated meat, vegetables, or sauces. There is a long incubation period, during which the organism multiplies in the patient’s intestinal tract, and the release of the heat-labile enterotoxin follows. This enterotoxin is responsible for the profuse watery diarrhea, nausea, and abdominal cramps.
B. Eye infections
- B. cereus ocular infections usually occur after traumatic, penetrating injuries of the eye with a soil contaminated object.
- These include severe keratitis and endophthalmitis.
C. Other infections
- B. cereus has also been associated with localized infections, such as wound infections, and with systemic infections, including endocarditis, catheter-associated bacteremia, central nervous system infections, osteomyelitis, and pneumonia.
- The presence of a medical device or intravenous drug use predisposes to these infections.
Laboratory Diagnosis of Bacillus cereus
SPECIMENS: Faeces, vomitus, remaining food (if any), eye specimen (corneal swab)
DIRECT DETECTION METHODS
- Microscopically the organisms appear as large gram-positive rods in singles, pairs, or serpentine with square ends after Gram staining.
- Endospores formation are seen as an unstained oval or round region within the center of the cell. Spores are oval (ellipsoidal) and not swelling of the mother cell.
Figure: Gram stain of Bacillus cereus.
CULTURE
- Growth on 5% sheep blood agar, chocolate agar, routine blood culture media, and nutrient broths.
- Detectable growth within 24 hours following incubation on media incubated at 35° C, in ambient air, or in 5% carbon dioxide (CO2).
- Colony character on blood agar: Large, feathery, spreading, dull, gray, granular, spreading colonies and opaque with a rough matted surface and irregular perimeters, beta-hemolytic.
- Bacillus cereus can be isolated from feces by using selective media such as MYPA (mannitol, egg yolk, polymyxin, phenol red, and agar), PEMBA (polymyxin, egg yolk, mannitol, bromothymol, blue agar).
- These media take advantage of the phospholipase C positive reaction on egg yolk agar, no production of acid from mannitol, and incorporation of pyruvate or polymyxin as the selective agents.
BIOCHEMICAL ANALYSIS
- Catalase: positive
- Oxidase: negative
- OF test: fermentative
- Indole: negative
- Methyl red: positive
- Vogues proskauer: positive
- Glucose: fermentative, production of acid
- Sucrose: fermentative, production of acid
- Lactose: no fermentation
- Starch hydrolysis: positive
- Nitrate reduction: positive
- Gelatin hydrolysis: positive
- Spore staining: endospore-forming bacteria
- Motility: motile
SERODIAGNOSIS
- Serologic methods are available for the detection of B. cereus toxin in food and feces.
- Microslide gel diffusion test is generally used as a toxin detection system.
MOLECULAR METHOD
- The toxigenic potential of B. cereus isolates, genes encoding emetic-toxin cereulide (ces), and enterotoxins (nhe, hbl and cytK) can be analyzed by multiplex PCR.
Treatment of Bacillus cereus
- Persons with B. cereus food poisoning require only supportive treatment.
- Oral rehydration or, occasionally, intravenous fluid and electrolyte replacement for patients with severe dehydration is indicated. Antibiotics are not indicated.
- Patients with the invasive disease require antibiotic therapy. Bacillus cereus is susceptible to clindamycin, erythromycin, vancomycin, aminoglycosides, and tetracycline. It is resistant to penicillin and trimethoprim.
Prevention and Control of Bacillus cereus
- Diarrheal and vomiting intoxications by this organism are readily preventable by appropriate food-handling procedures.
- Meat and vegetables should not be held at temperatures between 10 and 45 °C for long periods, and rice held overnight after cooking should be refrigerated and not held at room temperature.
- Prevention of infection in patients following surgery or in those who are immunocompromised or who are otherwise predisposed to infection depends on good practice.
References and Sources
- Bacillus cereus HiCynth™ Agar Base. HiMedia Laboratories Pvt. Ltd.
- Bacillus cereus. Mehrdad Tajkarimi. Materials from Maha Hajmeer.
- Bailey and Scott’s Diagnostic Microbiology. Part 3. Section 4. Chapter 18. Bacillus and Similar Organisms, 281.
- Choma C et al. Effect of temperature on growth characteristics of Bacillus cereus International Journal of Food Microbiology 55 (2000) 73–77.
- Edward J. Bottone. Bacillus cereus, a Volatile Human Pathogen. Clin Microbiol Rev. 2010 Apr; 23(2): 382–398.
- Floristean V., Carmen CreŃu, M. Carp-Cărare. Bacteriological Characteristics of Bacillus cereus isolates from poultry. Bulletin USAMV-CN, 64/2007 (1-2).
- LM Wijnands, JB Dufrenne, FM van Leusden. Bacillus cereus: characteristics, behaviour in the gastro-intestinal tract, and interaction with Caco-2 cells. RIVM report 250912003/2005.
- Mackie and McCartney Practical Medical Microbiology. Section B. Bacteria and Related Organisms. Chapter 17. Bacillus, 317.
- Ralph A. Slepecky and H. Ernest Hemphill. The Genus Bacillus—Nonmedical. Prokaryotes (2006) 4:530–562.
- S Fazlani, M Abubakar, S Shah, M ul Hassan, M Arshed. Bio-Morphological Characteristics of Bacterial Species Identified from Mastitic Milk Samples of Camel. The Internet Journal of Veterinary Medicine. 2008 Volume 6 Number 1.
- Topley and Wilson’s Microbiology and Microbial Infection. Bacteriology Volume 2. Part IV. Organisms and their biology. Chapter 36. Bacillus cereus, 922.
- http://academic.pgcc.edu/~kroberts/web/colony/colony.htm
- http://textbookofbacteriology.net/Bacillus_4.html
- http://www.antimicrobe.org/b82.asp
- http://www.antimicrobe.org/b82.asp
- http://www.biomerieux-industry.com/food/bacillus-cereus-culture-media
- http://www.fda.gov/Food/FoodScienceResearch/LaboratoryMethods/ucm070875.htm
- http://www.foodsafety.gov/poisoning/causes/bacteriaviruses/bcereus/
- http://www.microbiologyinfo.com/different-size-shape-and-arrangement-of-bacterial-cells/
- http://www.microbiologyinpictures.com/bacteria-micrographs/gram-stain/gram-positive/bacillus-cereus.html
- http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2863360/
- http://www.ncbi.nlm.nih.gov/pubmed/25528535
- http://www.phac-aspc.gc.ca/lab-bio/res/psds-ftss/bacillus-cereus-eng.php
- http://www.ppdictionary.com/bacteria/gpbac/cereus.htm
- http://www.tgw1916.net/Bacillus/cereus.html
- http://www.uptodate.com/contents/bacillus-cereus-and-other-non-anthracis-bacillus-species
- https://bioweb.uwlax.edu/bio203/s2013/salaba_jaco/habitat.htm
- https://catalog.hardydiagnostics.com/cp_prod/Content/hugo/Bacillus.htm
- https://efoodalert.wordpress.com/2011/10/30/profiling-bacillus-cereus/
- https://en.wikipedia.org/wiki/Bacillus_cereus
- https://microbewiki.kenyon.edu/index.php/Bacillus_cereus
- https://modmedmicrobes.wikispaces.com/B.Cereus
- https://sites.google.com/site/allmicrobiologysite/medical-microbiology-ii/summary-of-bacterial-pathogens/bacillus-cereus