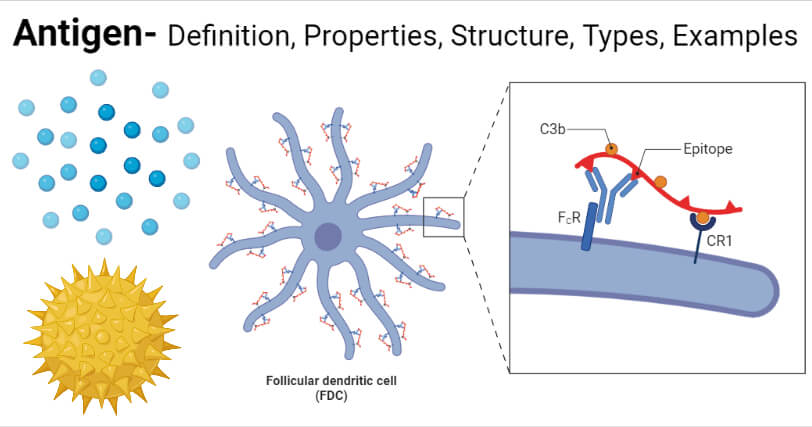
Antigens are molecules or molecular structures that are foreign to the body and generally induce an immune reaction in the form of the production of antibodies against them.
- In simple words, antigens can be anything that doesn’t belong to the body and are foreign.
- Even though antigens are usually defined by the induction of an immune response, all antigens might not induce an immune response. The antigens that induce a response are termed immunogens.
- The ability of antigens to elicit an immune response depends on the presence of specific regions on the antigens called antigenic determinants. The determinants bind to receptor molecules with the complementary structure on immune cells to elicit a response.
- Antigens are indicated by the term ‘Ag’, and these can occur in different forms like pollen, viruses, chemicals, or bacteria.
- The concept of antigen arose from the fact that our body can distinguish between the components of the body and foreign particles.
- In response to these antigens, the body induces the production of antibodies that act against the said antigens.
- Most antigens in humans are proteins, peptides, or polysaccharides; however, lipid and nucleic acids can also act as antigens when combined with proteins or polysaccharides.
- In addition, antigens might also be intentionally introduced into the body in the form of vaccines in order to induce the adaptive immune system of the body against the antigen.
Properties of Antigens
Antigens have different properties which determine the immunogenicity of the antigens and thus are essential in order to understand the immune reaction against them. Since these properties determine the immunogenicity, these are considered properties required to form a good antigen. The following are some of the properties of antigens;
1. Foreign Nature
- All antigens that induce an immune response in the host are foreign to the body of the recipient.
- The host body recognizes the antigen to be different from the normal body components.
- The immunogenicity of the antigen increases with the increase in the degree of foreignness. In the case of biological antigens, the foreignness increases with the increase in the phylogenetic gap between the two species.
- However, there are some exceptions in that some proteins occurring within the host might also induce an immune response, as in the case of autoantigens.
- Similarly, proteins and other molecules from other species might also not induce an immune response if they lack antigenic determinants or epitopes.
2. Chemical Nature
- The most potent and commonly encountered antigens are proteins followed by polysaccharides.
- However, other molecules like lipids and nucleic acids can also act as antigens when complex with proteins and polysaccharides.
- In the case of proteins, the antigen should contain immunogenic regions with at least 30% of amino acids like lysine, glutamine, arginine, glutamic acids, aspargine, and aspartic acid, along with a high number of hydrophilic or charged groups.
- The level of immunogenicity also increases with the heterogenicity of the molecules. Homopolymers are usually less immunogenic than heteropolymers.
3. Molecular Size
- The molecular size of the antigens is also crucial in the immunogenicity of the molecules.
- It has been established that antigens should have a minimum size of greater than 5000 Da before they can be considered immunogenic.
- However, low molecular weight substances can demonstrate immunogenicity when coupled with large-sized carriers.
- The low molecular weight substances are termed haptens that are considered ‘partial antigens’ with at least one antigenic determinant.
4. Molecular Rigidity and Complexity
- The rigidity and complexity of molecules are essential factors that determine immunogenicity.
- In general, rigid molecules are good antigens as they can raise antibodies to certain structures when compared to the less rigid ones.
- The complexity of the structure is also an essential factor as a peptide antigen with a repeating unit of a single amino acid is less immunogenic than a molecule with two or more repeating amino acids units.
5. Antigenic Determinants and Cross-reactivity
- Antigenic determinants are regions in an antigen molecule that is involved in the reaction with antibodies.
- Usually, antigens with two or more antigenic determinants can induce antibody production. Thus, a smaller antigen usually doesn’t induce antibody production as it is not possible for a small molecule to have more than one antigenic determinant.
- Cross-reactivity of antigens is also an essential factor where antibodies induced by a different antigen can interact with another antigen.
Antigen Structure
- The molecular structure of an antigen is characterized by its ability to bind to the antigen-binding site of an antibody.
- Antibodies differentiate between different antigens on the basis of the specific molecular structures present on the surface of the antigen.
- Most antigens are proteins or polysaccharides. These can include coats, capsules, flagella, toxins, and fimbriae of bacteria, viruses, or other microorganisms. Besides, secretions and other chemicals of the same nature can also act as antigens.
- Lipids and nucleic acids of these microorganisms are only antigenic when these are combined with proteins or polysaccharides.
- The structure of antigens might be different depending on the nature of the antigen, their size, and immunogenicity.
- All immunogenic antigens have a specific structural component called epitope or antigenic determinant.
- The number of epitopes differs in different antigens and determines the number of antibodies a single antigen can bound to.
- The structural components of interaction in antigens are different, which determines the classes of antibodies they bound to.
- The region on antibodies that interacts with antigens is called a paratope. It has been established that the structure of epitope and paratope can be defined with a lock and key metaphor as the structures are specific and fit with one another.
Types of Antigens
Antigens can be grouped into different types based on different factors. Some of the common classifications are based on the origin of the antigen and its immunogenicity.
1. Types of antigen-based on their origin
Antigens can be classified into two groups on the basis of their origin;
a. Exogenous Antigens
- Exogenous antigens are the antigens that are originated outside the body of the host and, thus, are foreign to the host.
- These antigens might enter the body through inhalation, ingestion, or injection and then circulate throughout the body via bodily fluids.
- The uptake of exogenous antigens is primarily mediated by phagocytosis via Antigen Processing Cells (APCs) like macrophages, dendritic cells, etc.
- Many antigens like intracellular viruses might begin as exogenous antigens and later become endogenous.
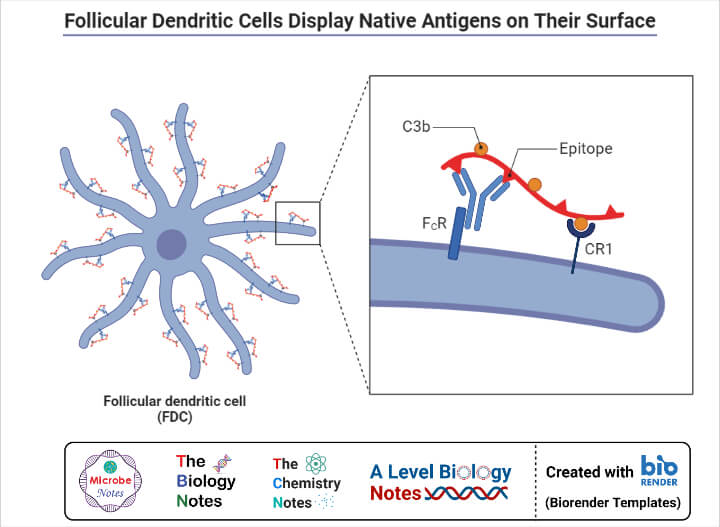
Figure: Follicular Dendritic Cells Display Native Antigens on Their Surface
b. Endogenous Antigens
- Endogenous antigens are antigens that originate within the body of the host during metabolism or as a result of intracellular viral or bacterial infection.
- Endogenous antigens are usually the cells of the body or fragments, compounds, or antigenic products of metabolism.
- These are usually processed in the macrophages and are later detected by cytotoxic T-cells of the immune system.
- Endogenous antigens include antigens that are xenogenic or heterologous, autologous, and idiotype or allogenic.
- Endogenous antigens might result in autoimmune diseases as the host immune system detects its own cells and particles as immunogenic.
Autoantigens
- Autoantigens are proteins or protein complexes of the host that are attacked by the host’s immune system, resulting in autoimmune disease.
- Autoantigens can be deadly to the host as the body’s own cells should not be targeted by the immune system.
- The immunological tolerance to such antigens is lost as a result of genetic and environmental factors.
Tumor Antigens (Neoantigens)
- Tumor antigens or neoantigens are presented by Major Histocompatibility Complex (MHC) I and II on the surface of tumor cells.
- The antigens are produced as a result of a tumor-specific mutation during the malignant transformation of normal cells.
- These antigens usually do not induce an immune response as the tumor cells develop ways to evade antigen presentation and immune defense.
Native Antigens
- Native antigens are antigens that are not processed by any antigen-presenting cells (APC), and thus immune cells like T-cells cannot bind to these antigens.
- However, B-cells can be activated such antigens even without any processing.
2. Types of antigens on the basis of immune response
- Antigens can be classified into two distinct groups on the basis of immune response;
a. Complete antigens/ Immunogens
- Complete antigens or Immunogens are antigens that elicit a specific immune response.
- These antigens can induce an immune response by themselves without any carrier particles.
- These are usually proteins, peptides, or polysaccharides with high molecular weight (greater than 10,000 Da).
b. Incomplete antigens/ Haptens
- Incomplete antigens or haptens are antigens that cannot generate an immune response by themselves.
- These are usually non-protein substances that require a carrier molecule to form a complete antigen.
- Haptens have a low molecular weight (usually less than 10,000 Da) and fewer antigenic determinant sites.
- The carrier molecule bonded to the hapten is considered a non-antigenic component and is a protein or a polysaccharide molecule.
Antigen Processing and Presentation
Antigen processing and presentation is the process of digestion of antigens into smaller peptide fragments by an antigen-presenting cell (APCs) that are then displayed on the surface of the cells via antigen-presenting molecules like MHC class I and II for recognition by lymphocytes.
Antigen processing and presentation can occur via three different pathways;
1. Endogenous Pathway or Classical MHC class I Presentation
- The endogenous pathway of antigen processing and presentation utilizes mechanisms similar to those involved in the normal turnover of intracellular proteins.
- The antigen-presenting cells degrade the protein antigen into short peptides by a specified cytosolic proteolytic system called the proteasome.
- The proteasome involved in the immune system is called the immunoproteasome, which has components induced by exposure to interferon-γ or TNF-α.
- The next step of the proteolytic mechanisms is the peptide trimming by aminopeptidases in the ER lumen.
- The peptides formed after proteolysis are transported to the ER lumen by the Transporter associated with Antigen Processing (TAP).
- In addition to TAP, tapasin and calnexin-calreticulin system mediates the trimming and loading of peptides on MHC class I molecules.
- Depending on the affinity of the loaded peptides, MHC class I molecules will either be transported to the cell membrane or recycled by a mechanism dependent on UDP-glucose glycoprotein transferase-1.
- In the case of high-affinity MHC class-1 complexes, the peptides are transported through the Golgi apparatus to the cell membrane in order to elicit antigen-specific CD8+ T cell responses.
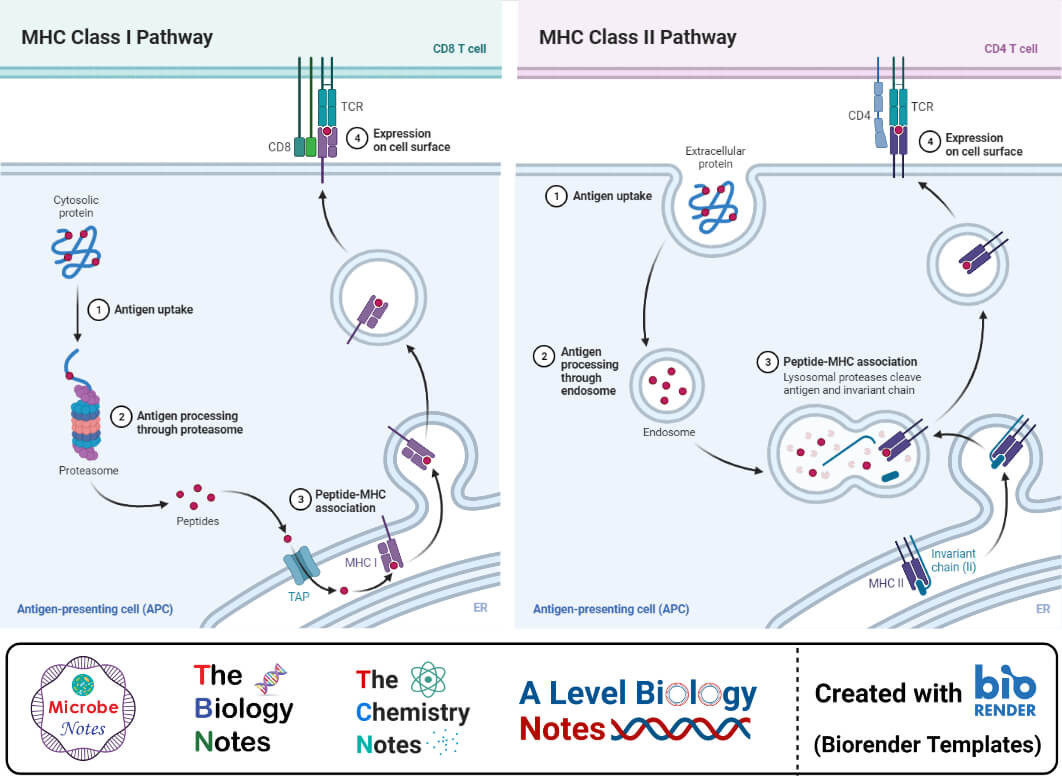
2. Exogenous Pathway/ Classical MHC class II Presentation
- In the case of the exogenous pathway, APCs internalize the antigen by simple phagocytosis, where the material first binds to specific surface receptors.
- The degradation of proteins into peptides occurs within the compartments of the cell by the endocytic processing pathway.
- The internalized antigen progresses through different acidic compartments encountering hydrolytic enzymes and low pH in each compartment.
- The APCs have a unique endosome in the MHC class II-containing compartment (MIIC), where the final protein degradation and peptide loading take place.
- Since APCs express both classes of MHC, there is a distinct mechanism to prevent the interaction of antigenic peptides for the class I molecules.
- When class II MHC molecules are synthesized, the class II αβ chains associate with a protein called the invariant chain. This protein interacts with the class II peptide-binding groove preventing the binding of endogenously derived peptides to the class II molecule.
- As the invariant chain moves through different compartments, it is degraded until it forms a short fragment termed CLIP (class II-associated invariant chain peptide).
- Later, a class II MHC molecule catalyzes the exchange of CLIP with antigenic peptide.
- The peptide binding is required to maintain the structure and stability of class II MHC molecules.
- After the binding of the peptide, the class II MHC –peptide complex is transported to the plasma membrane, where the neutral pH causes the complex to form a compact, stable form.
3. Cross-presentation
- Cross-presentation is the process where the APCs will divert antigen obtained by endocytosis (exogenous pathway) to a class I MHC loading and peptide presentation.
- The phenomenon of cross-presentation, however, requires the internalized antigens to be handled by the exogenous pathway leading to class II MHC presentation somehow are redirected to a class I loading pathway.
- Cross-presentation is primarily observed in the case of dendritic cells that accomplish cross-presentation by one of the two possible means.
- The first mechanism assumes that cross-presenting cells contain special antigen-processing machinery that enables the loading of exogenously derived peptides onto class I MHC molecules.
- The second mechanism hypothesizes that specialized endocytosis machinery is found in the cells that send internalized antigen directly to an organelle, where the peptides are then loaded onto class I MHC molecules.
- Cross-presentation of antigens has an advantage as APCs can capture viruses from extracellular environments, process them and activate cytotoxic T-cell lymphocytes that can attack virus-infected cells, which inhibit the further spread of the virus.
Antigen-Antibody Complex
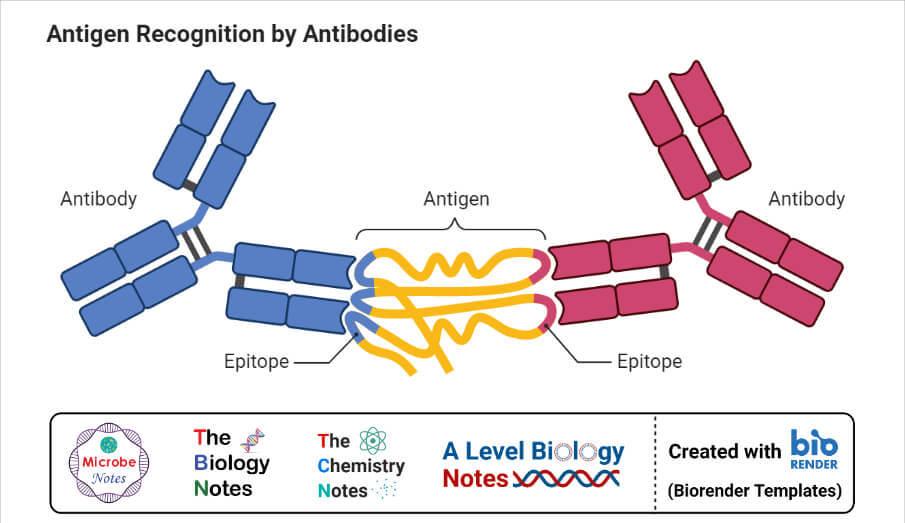
- An antigen-antibody complex or immunogenic complex is a molecule formed by binding multiple antigens to antibodies.
- The binding of antibody and antigen is determined by the epitope and paratope present in the antigen and antibody, respectively.
- The ability of antibodies to fight against multiple pathogens is due to their ability to distinguish between different antigens.
- The interaction between antigens and antibodies is highly specific, and it is determined by the amino acid sequence in the epitope and paratope of the species.
- The complex is formed by an antigen-antibody reaction which is then subject to a number of responses like complement deposition, opsonization, and phagocytosis.
- The shape and size of the immune complex are determined by the ratio of antigen to antibody. The size, in turn, determines the effect of the immune complex.
- Antigen-antibody complexes have become an important tool in understanding the antigen-antibody interaction and determining the basis of molecular recognition between an antibody and antigens.
- Immune complexes also play a role in regulating antibody production as the binding of antigen to cell receptors activates signaling cascade leading to the activation of antibodies.
- Even though immune complexes are essential for different immune functions, the deposition of the immune complex can lead to several autoimmune diseases like arthritis and scleroderma.
Antigen Examples
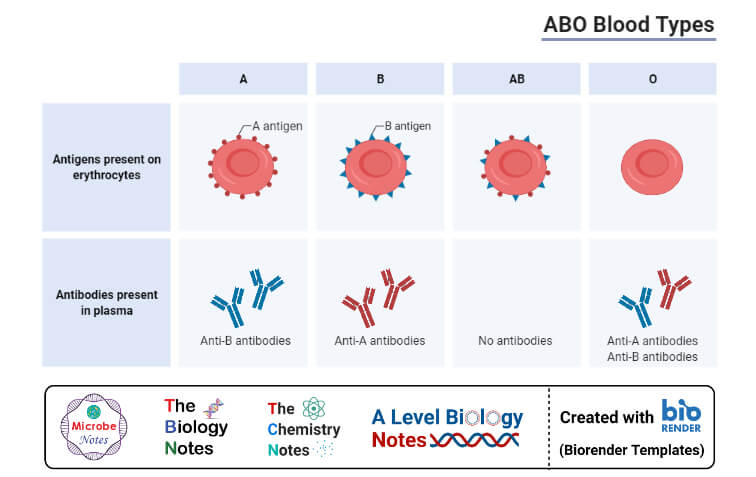
1. Blood group antigens
- Blood group antigens are proteins or sugars present on the surface of different components in the red blood cell membrane.
- The antigens in the ABO blood group are the sugar that is produced by a serried of reactions that catalyzes the transfer of sugar units.
- The type of sugar in the red blood cell is determined by the type of enzyme involved, which in turn is determined by the person’s DNA.
- The antigens of the Rh blood group are proteins that are also determined by the host’s DNA. The RhD gene encodes the D antigen, which occurs as a large protein on the red blood cell.
- These antigens can be distinguished by antigen-antibody reactions that help determine different blood groups in humans.
2. Bacterial Capsule
- A bacterial capsule is a polysaccharide layer occurring outside the cell envelope that induces an immunogenic reaction in the host.
- The capsule is a well-organized layer that cannot be removed easily and thus is considered a possible cause of bacterial pathogenicity.
- In some bacteria, the capsule can also be involved in evading phagocytosis as a capsule-specific antibody is required to cause phagocytosis.
- Bacterial capsules are also used as antigens used in vaccines where the polysaccharide component of the capsule is conjugated with protein carriers.
- The exact structure, function, and involvement of capsules in bacteria differ in different bacterial species.
Applications of Antigens
- The detection of different antigens in different species can be used to differentiate between bacteria species as antigens are usually very specific.
- Antigens can also be used for diagnostic purposes to detect the presence of antibodies in a sample.
- Antigens are an essential component of antigen-antibody complexes, which have forensic application in the identification of human blood and other samples.
- These are also used in immunoassays for the quantification of various chemical and biological substances.
- Autoantigens are responsible for autoimmune diseases, which in some cases can be lethal.
- Inactivated enzymes are used in vaccines as a form of passive immunity to prevent and cure different diseases.
References
- Peter J. Delves, Seamus J. Martin, Dennis R. Burton, and Ivan M. Roitt(2017). Roitt’s Essential Immunology, Thirteenth Edition. John Wiley & Sons, Ltd.
- Judith A. Owen, Jenni Punt, Sharon A. Stranford (2013). Kuby Immunology. Seventh Edition. W. H. Freeman and Company.
- Nossal, G J et al. “Antigens in immunity. XV. Ultrastructural features of antigen capture in primary and secondary lymphoid follicles.” The Journal of experimental medicine vol. 127,2 (1968): 277-90. doi:10.1084/jem.127.2.277
- Kotsias F, Cebrian I, Alloatti A. Antigen processing and presentation. Int Rev Cell Mol Biol. 2019;348:69-121. doi: 10.1016/bs.ircmb.2019.07.005. Epub 2019 Aug 1. PMID: 31810556.
- Kapingidza AB, Kowal K, Chruszcz M. Antigen-Antibody Complexes. Subcell Biochem. 2020;94:465-497. doi: 10.1007/978-3-030-41769-7_19. PMID: 32189312.
- Dean L. Blood Groups and Red Cell Antigens [Internet]. Bethesda (MD): National Center for Biotechnology Information (US); 2005. Chapter 2, Blood group antigens are surface markers on the red blood cell membrane. Available from: https://www.ncbi.nlm.nih.gov/books/NBK2264/
- Santambrogio Laura, Berendam Stella J., Engelhard Victor H. The Antigen Processing and Presentation Machinery in Lymphatic Endothelial Cells. Frontiers in Immunology. 2019. 10.3389/fimmu.2019.01033
- Saylor Kyle, Gillam Frank, Lohneis Taylor, Zhang Chenming. Designs of Antigen Structure and Composition for Improved Protein-Based Vaccine Efficacy. Frontiers in Immunology. 2020. 10.3389/fimmu.2020.00283
- Maurice Landy, Werner Braun. PROPERTIES OF ANTIGENS IN RELATION TO RESPONSIVENESS AND NON-RESPONSIVENESS. Immunological Tolerance. Academic Press. 1969, Pages 1-52. https://doi.org/10.1016/B978-1-4832-2727-6.50008-7.
- https://microbiologyinfo.com/antigen-properties-types-and-determinants-of-antigenicity/

I enjoyed reading
Oops! Amazing ????
I enjoyed reading and it’s easily understandable
nice