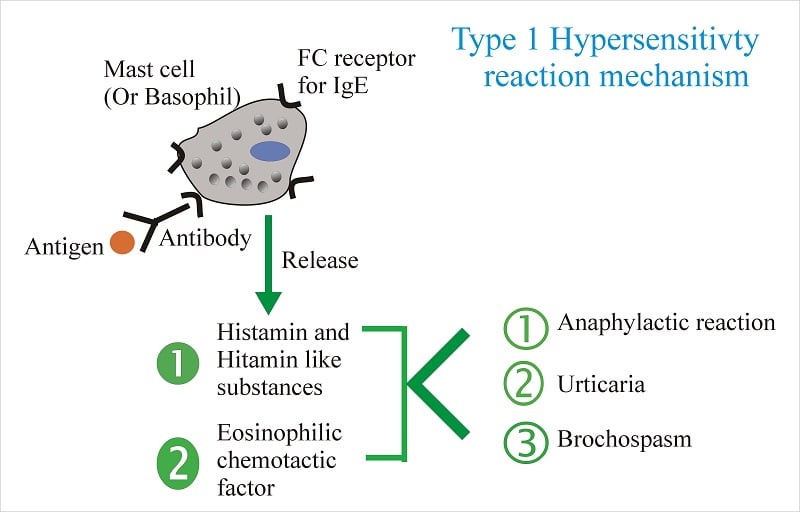
- Hypersensitivity is increased reactivity or increased sensitivity by the animal body to an antigen to which it has been previously exposed.
- The most widely adopted current classification is that of Coombs and Gellthat designates immunoglobulin-mediated (immediate) hypersensitivity reactions as types I, II, and III, and lymphoid cell-mediated (delayed-type) hypersensitivity/cell-mediated immunity as a type IV reaction.
- A hypersensitive response (HR) is an anti-pathogen response in plants produced by avr-R system activation that leads to alterations in Ca+ flux, MAPK activation, and NO and ROI formation.
- Type I hypersensitivity reaction is commonly called allergic or immediate hypersensitivity reaction.
- This reaction is always rapid, occurring within minutes of exposure to an antigen, and always
involves IgE-mediated degranulation of basophils or mast cells. - Type I reactions are also known as IgE-mediated hypersensitivity reactions.
- IgE is responsible for sensitizing mast cells and providing recognition of antigen for immediate hypersensitivity reactions.
- The short time lag between exposure to antigen and onset of clinical symptoms is due to the presence of preformed mediators in the mast cells.
- Thus, the time taken for these reactions to initiate is minimal, so the onset of symptoms seems to be immediate.
- Type I reaction can occur in two forms: anaphylaxis and atopy.
Clinical Manifestations of Type 1 Hypersensitivity
- A wide variety of hypersensitivity states can be classified as immediate hypersensitivity reactions.
- Some have a predominantly cutaneous expression (hives or urticaria), others affects the airways (hay fever, asthma), while still others are of a systemic nature.
- The latter are often designated as anaphylactic reactions, of which anaphylactic shock is the most severe form.
- The expression of anaphylaxis is species-specific.
- The guinea pig usually has bronchoconstriction and bronchial edema as predominant expression, leading to death in acute asphyxiation.
- In the rabbit, on the contrary, the most affected organ is the heart, and the animals die of right heart failure.
- In man, allergic bronchial asthma in its most severe forms closely resembles the reaction in the guinea pig.
- Most frequently, human type I hypersensitivity has a localized expression, such as the bronchoconstriction and bronchial edema that characterizes bronchial asthma, the mucosal edema in hay fever, and the skin rash and subcutaneous edema that defines urticaria (hives).
- The factor(s) involved in determining the target organs that will be affected in different types of immediate hypersensitivity reactions are not well defined, but the route of exposure to the challenging antigen seems an important factor.
- For example, allergic (extrinsic) asthma and hay fever are usually associated with inhaled antigens while urticaria is seen as a frequent manifestation of food allergy.
- However, the manifestations of food allergy are very diverse, and, in addition to hives, can include a variety of symptoms affecting different organs and systems.
-
Systemic Anaphylaxis
- Systemic anaphylaxis is usually associated with antigens that are directly introduced into the systemic circulation, such as in the case of hypersensitivity to insect venom or to systemically-administered drugs, such as penicillin.
- However, seafood and peanuts can also elicit anaphylactic reactions.
- Systemic anaphylactic reactions in humans can present in diverse forms, affecting different organs and systems.
- Cardiovascular involvement is associated with the highest mortality rates.
-
Atopy
- Some individuals have an obvious tendency to develop hypersensitivity reactions.
- The term atopy is used to designate this tendency of some individuals to become sensitized to a variety of allergens (antigens involved in allergic reactions) including pollens, spores, animal danders, house dust, and foods.
- These individuals, when skin tested, are positive to several allergens and successful therapy must take this multiple reactivity into account.
- A genetic background for atopy is suggested by the fact that this condition shows familial prevalence.
Pathogenesis of Type 1 Hypersensitivity
- Immediate hypersensitivity reactions are a consequence of the predominant synthesis of specific IgE antibodies by the allergic individual; these IgE antibodies bind with high affinity to the membranes of basophils and mast cells.
- When exposed to the sensitizing antigen, the reaction with cell-bound IgE triggers the release of histamine through degranulation, and the synthesis of leukotrienes C4, D4, and E4 [this mixture constitutes what was formerly known as slow-reacting substance of anaphylaxis-A].
- These substances are potent constrictors of smooth muscle and vasodilators and are responsible for the clinical symptoms associated with immediate hypersensitivity.
- In recent years, it has been shown, mainly through animal studies, that IL-13, released by Th2 cells, can induce clinical manifestations of asthma, independently of IgE and eosinophils.
- Thus, cell-mediated, IgE-independent mechanisms may also play a pathogenic role in type I hypersensitivity reactions.