What is Sporothrix schenckii?
Sporothrix schenckii is a dimorphic fungus that is widely distributed in soil and in and on living and dead decaying environments.
- It is a pathogenic fungus that causes an infection known as sporotrichosis, in both animals and humans.
- Sporotrichosis is a chronic mycotic infection that affects the cutaneous and subcutaneous tissues.
- The fungal infection is associated with the formation of small, ulcerative, and suppurative lesions on and in the skin tissues.
- It can also affect the lymphatic system by forming nodular lesions which can be ulcerative and suppurative.
- The fungus gains entry into the host through skin abrasions and sometimes through inhalation into the lungs.
- Evidence of secondary spread to the muscles and bones is rare, with occasional infection of the central nervous system, lungs, and the genitourinary tract have been reported.
- Sporothrix schenckii was first isolated in 1896 by Benjamin Schenck, a medical student at the Johns Hopkins Hospital in Baltimore, MD, from a 36-year-old male patient presenting lesions on the right hand and arm.
Habitat of Sporothrix schenckii
- This fungus is commonly found in soil.
- It can also be found on living plants such as barberry shrubs and roses or in plant debris such as sphagnum moss and pine bark mulch.
- Sporothrix schenckii grows as a mold in the environment and at temperatures below 35°C.
- It transforms into a yeast form in vivo and at temperatures above 35°C.
- Sporotrichosis, an infection caused by Sporotrix schenckii is an occupational disease to florists, gardeners, and foresty workers.
- It is commonly prevalent in Tropical and subtropical regions.
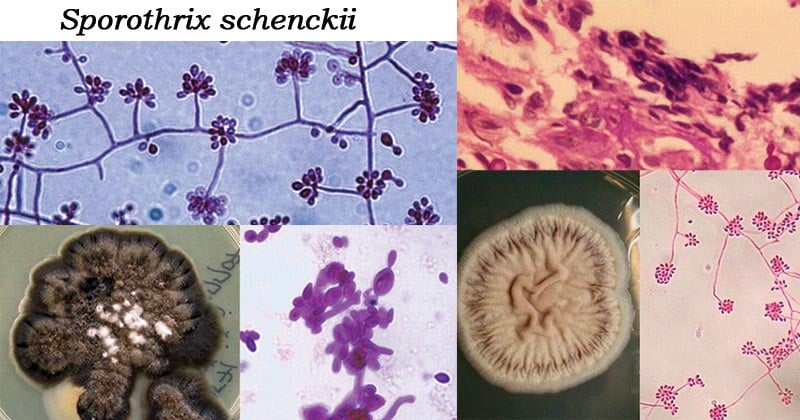
Morphology of Sporothrix schenckii
- Sporothrix schenckii is a dimorphic fungus.
- In the basic mycological culture at 25°C, it has a filamentous form that is composed of hyaline, septate hyphae 1 to 2 μm wide.
- The fungal growth in the colonies is characterized by branched septate hyphae which produce small distinct asexual spores known as conidia of 3–5 μm, which are brown in color.
- The conidia are produced by conidiophores, which arise at right angles from the septate hyphae.
- The conidiophore, are tapered at the ends.
- The formed conidia are clustered on tiny denticles at the apex of the conidiophore forming a flower-like appearance.
- The conidia are ovoid or elongated, 3-6 x 2-3 µm, hyaline, single-celled, and smooth-walled.
- Large singly occurring conidia may also be formed as the fungal culture ages.
- The large conidia are dark, thick-walled obovate to angular.
- In rich media budding yeast cells which are fusiform of about 1–3 × 3–10 μm are formed which are spherical, or oval-shaped.
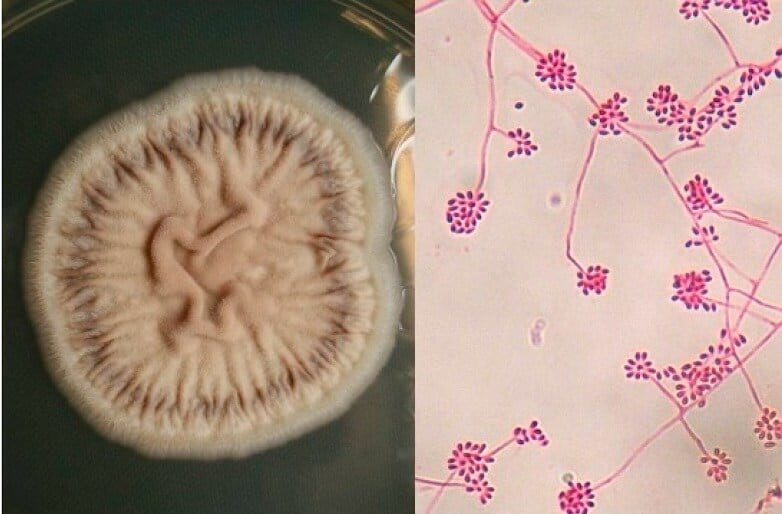
Figure: Culture of Sporothrix schenckii (Sabouraud media, 28 °C) Filamentous state with thin hyphae and denticle microconidia like “daisy flowers” (Erythrosine, 40×). Image Source: MDPI.
Cultural Characteristics of Sporothrix schenckii
- In routine mycological agar media such as malt extract agar and potato dextrose agar, at room temperature 25°C, they grow slowly, forming blackish/greyish and shiny colonies that mature to moist, glabrous, wrinkled, and fuzzy colonies, colored in black.
- In a rich medium such as brain heart infusion media (BHI) at 35-37°C, Sporotrix schenckii is thermally dimorphic whose growth is characterized by multiple budding yeast cells.
- In the BHI medium, they produce colonies that are glabrous, white-greyish to yellowish color, yeast cells.
Transmission of Sporothrix schenckii
- The fungus inoculation into the host is via traumatic implantation of the fungus from contaminated soil, plants, and organic matter with the fungus.
- It is common in florists, gardeners, miners, and forest workers.
- Zoonotic transmission from cats has also been reported in a few cases in Brazil.
- It has a 1-12 week incubation period.
Pathogenesis of Sporothrix schenckii
Virulence Factors of Sporothrix schenckii
Thermotolerance
- Sporothrix schenckii has the ability to grow in temperatures of 35-37°C.
- At 35°C, it can cause lymphatic sporotrichosis and at 37°C, it can cause disseminated and extracutaneous lesions of sporotrichosis.
Melanin synthesis
- Sporothrix schenckii has the ability to synthesize melanin, an insoluble compound that has been linked to the virulence of many fungal groups.
- The melanin is found on the dematiaceous conidia of the fungus
- Conidial melanization enhances the resistance of Sporotrix schenckii to macrophage phagocytosis initiating the first stage of infection by the conidia spores, the infective particle of the fungus.
- The melanin pigmentation plays a major role in causing cutaneous sporotrichosis by enhancing the invasiveness of the fungus into the host.
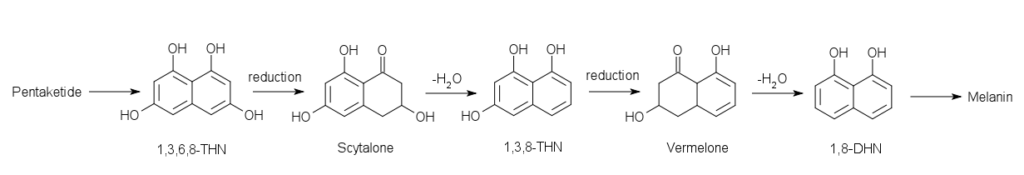
Figure: Structures of some intermediates in the pentaketide pathway of melanin biosynthesis in S. schenckii. Image Source: Wikipedia.
Adherence
- Sporotrix schenckii has adhesins such as integrins and adhesin lectin-like molecules that are able to recognize the glycoproteins on the extracellular matrix of the cutaneous tissues i.e fibronectin, laminin and type II collagen.
- The fibronectin adhesins are located on the surface of yeast cells and they attribute to the fungal adherence factors to the host.
- Laminin receptors are located on the fungus hyphae and yeasts which have the ability to bind to the extracellular matrix.
- The presence of these adhesins favors the fungus adherence to the host tissues and enhance disease dissemination.
Clinical Manifestations of Sporotrichosis
Lymphocutaneous infection
- It is the most common manifestation of Sporotrix schenckii
- Lesions occur on the hands and arms, lower extremities, trunk, and face.
- Primary lesions occur within the first few weeks of fungal inoculation.
- The lesions are small nodules that progress to ulceration
- The lesions are a bit painful and nonpruritic.
- New nodules spread on the lymphatics and become ulcerated.
- Lymphangitis may develop, making the lymph nodes swollen and painful.
Cutaneous Infection
- Sporothrix schenckii is a common causative agent of suppurative and granulomatous inflammatory reaction in the dermis and subcutaneous tissue.
- It is characterized by microabscess and fibrosis, hyperkeratosis, parakeratosis, and pseudoepitheliomatous hyperplasia.
Fixed Cutaneous Infection
- This is the development of a single lesion normally on the face.
- The lesion may be ulcerated or verrucous
- The lesion only disappears on antifungal therapy.
Osteoarticular sporotrichosis
- It is a rare condition of sporotrichosis, commonly affecting alcoholics
- It is characterized by septic arthritis which occurs due to traumatic inoculation which spreads to the joints.
- Bursitis and tenosynovitis can occur presented with carpal tunnel syndrome.
Pulmonary sporotrichosis
- It is a subacute to chronic infections
- It is common in persons with Chronic Obstructive Pulmonary Disease (COPD).
- It occurs after the inhalation of conidia.
- It is characterized by fever, fatigue, weight loss, coughing, sputum productions, and hemoptysis
- Infected individuals often have chronic cavitary pulmonary histoplasmosis, tuberculosis, or atypical mycobacterial infection.
Diagnosis of Sporotrichosis
Specimen: Tissue biopsy, pus from lesions, sputum, urine, blood, and cerebrospinal and synovial fluids.
Direct Examination
- 10% potassium hydroxide (KOH) wet mount to observe for budding yeast cells
- Gram staining stains the yeast cells gran positive.
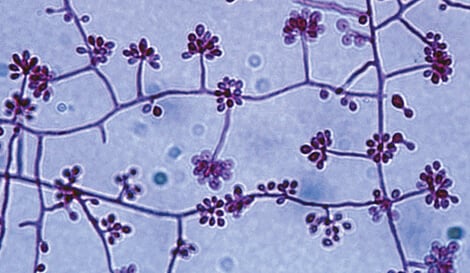
Figure: Sporothrix schenckii conidiophores and conidia at 25°C. Image Source: The University of Adelaide.
Histological Examination
- Hematoxylin and eosin (H&E) stain,
- Gomori methenamine silver (GMS)
- Periodic acid-Schiff (PAS) stain
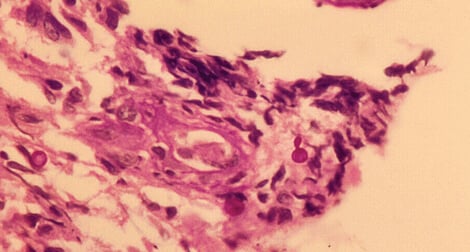
Figure: Sporothrix schenckii PAS stained tissue section showing budding yeast-like cells. Image Source: The University of Adelaide.
Cultural Examination
- Sabouraud agar with chloramphenicol and on media with cycloheximide, such as mycobiotic agar, growth occurs in 5-7 days at 25°C, forming filamentous hyaline colonies which become dark at the center as the culture ages. Dematiaceous conidia are also observed.
- Potato Dextrose Agar and Cornmeal agar are used to show conidiogenesis.
- Brain Heart Infusion Agar, Chocolate agar and blood agar are used to show dimorphism at 35 to 37°C. Growth of colonies develops within 5-7 days to form yeast cell colonies which are creamy and yellow, to tan color.
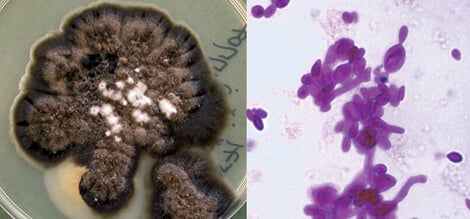
Figure: Sporothrix schenckii culture at 25C and budding yeast cells in BHI at 37°C. Image Source: The University of Adelaide.
Molecular Detection
- Detection of PCR amplicons
- Oligonucleotide primers for differentiation of Sporortrix schenckii from other fungal species.
Serological Test
- Tube agglutination test to detect for agglutinin antibodies (high titers)
- Latex Agglutination – Antigen-coated latex particle to detect for sporotrichin antigen in the sera of infected patients
Sporotrichin Skin Test
- This test is meant to detect delayed hypersensitivity (cellular immune response).
- It can detect and confirm the present and previous infection by Sporothrix schenckii.
- The sporotrichin skin test has been used to confirm the diagnosis of bulbar conjunctival sporotrichosis.
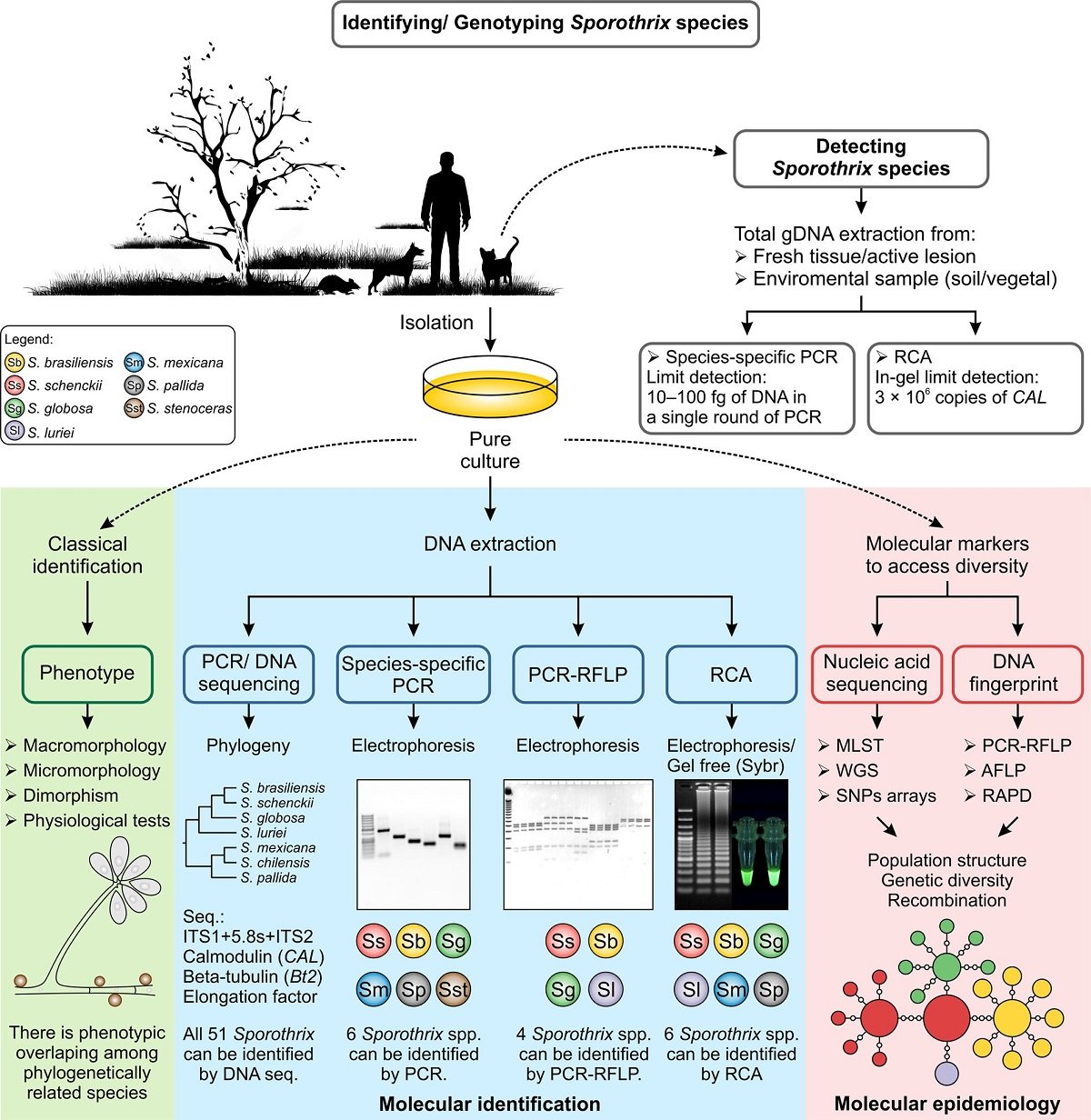
Figure: Recognition of Sporothrix species using classical and molecular approaches. Image Source: https://doi.org/10.1093/mmy/myx103
Treatment of Sporotrichosis
- Oral administration of a saturated solution of potassium iodide
- Itraconazole is currently the first-choice treatment
- Systemic infection can be treated with amphotericin B
Prevention and Control of Sporotrichosis
- Putting on protective clothing such as gloves and long sleeves during high-risk activities, for example, handling sphagnum moss, wires, rose bushes, hay bales, conifer (pine) seedlings, or other materials that may facilitate the exposure to the fungus
- Cats with sporotrichosis should be correctly treated and kept isolated in a proper place to prevent zoonotic transmission.
References and Sources
- 3% – http://europepmc.org/articles/PMC3194828
- 2% – https://mycology.adelaide.edu.au/descriptions/hyphomycetes/sporothrix/
- 1% – https://www.sciencedirect.com/science/article/pii/S003130251730082X
- 1% – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4659463/
- 1% – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4169245/
- 1% – https://www.medicinenet.com/sporotrichosis/article.htm
- 1% – https://cmr.asm.org/content/24/4/633?cited-by=yes&legid=cmr;24/4/633
- <1% – https://www.thermofisher.com/order/catalog/product/R01630
- <1% – https://www.spandidos-publications.com/10.3892/ol.2019.10071
- <1% – https://www.researchgate.net/publication/51069537_Sporotrichosis_Clinical_and_Histopathological_Manifestations
- <1% – https://www.researchgate.net/profile/Salam_MA/publication/244942184_Potassium_Hydroxide_KOH_Wet_Preparation_for_the_Laboratory_Diagnosis_of_Suppurative_Corneal_Ulcer/links/0deec52ebb6cd52641000000.pdf
- <1% – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5245785/
- <1% – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4845149/
- <1% – https://www.medicalnewstoday.com/articles/307076
- <1% – https://mycology.adelaide.edu.au/mycoses/subcutaneous/
- <1% – https://en.wikipedia.org/wiki/Dimorphic_fungus
- <1% – https://cmr.asm.org/content/cmr/24/4/633.full-text.pdf

Excellent Research, thank you do much. This is a breakthrough revelation for many physicians who cannot accept the fact that, due to unscrupulous modifications of the environment, pharmaceutical abominations, etc., patients suffering from the mysterious and taboo Morgellons Disease, can be justified and cured.