What is Shigella infection?
Shigella species are responsible for causing acute gastrointestinal tract infections that damage the ileal and colonic epithelium and cause bacillary dysentery. Shigella infection is mainly reported in poor underdeveloped and developing countries where there is a lack of hygiene, sanitation, and health care facilities.
- The mortality rate of Shigellosis is high especially in children under 5 years with malnutrition.
- The person suffering from Shigella infection undergoes impaired nutrition due to the heavy loss of electrolytes and blood during diarrhea which may lead to the death of a person.
- Shigella species are classified into four serogroups namely S. dysenteriae (serogroup A), S. flexneri (serogroup B), S. boydii (serogroup C) and S. sonnei (serogroup D).
- Among these, S. dysenteriae Type 1 is responsible for causing deadly epidemic outbreaks whereas other serotype causes minimum and rare disease.
Biological characteristics of Shigella
- Gram-negative
- Facultative anaerobes
- Non-sporulating
- Non-motile
- Non-encapsulated
- Prokaryotic rods
- Optimum temperature – 7 to 46°C
- Can resist 5% NaCl and pH
- Can survive the harsh physical and chemical condition
- Sensitive to pasteurization temperature
Sources and transmission of Shigella infection
- The main reservoir of Shigella species is in the intestinal tract of the human host.
- In animals, the infection by Shigella is rarely present.
- The route of transmission is via the fecal-oral route or through person-to-person contact.
- Ingestion of water and food contaminated with human feces are the primary sources.
- Contaminated water used by the farmers during irrigation contaminates vegetables and fruits.
- Children and infants are more prone to shigellosis mainly in poor and developing countries due to lack of sanitary facilities and good hygienic practices.
Epidemiology of Shigella infection
- Shigella dysenteriae is named after the Japanese microbiologist Kiyoshi Shiga while investigating a large epidemic of dysentery that occurred in Japan in 1896.
- A small amount of bacterial cells (10 to 100) is capable of causing shigellosis while other pathogens require 1000 to 100000 bacterial cells.
- According to World Health Organization (WHO), it is estimated that 165 cases of shigellosis occur all over the world each year having 55,000 death rates counted in children under five years.
- In Kolkata, a sporadic outbreak occurred which was caused by S. dysenteriae and S. flexneri isolated from the stool sample of an infected person.
- In the last decades, endemic and epidemic mostly occurred in South Asia and East Africa.
Diseases and symptoms of Shigella infection
- Symptoms usually begin after 1 to 3 days of ingestion of bacterial cells but depend on the amount of dose ingested ranges from 12 hours to 7 days.
- Typical symptoms include fever, loss of appetite, abdominal pain, bloody or watery diarrhea, inflammation of the colon, fatigue, malaise, fever.
- Due to the excretion of excess watery fluid, dehydration may occur but is usually rare and not a big concern.
- Anorexia and malnutrition require active management which is the main cause of death in children under 5 years of age.
- Neurological disorders may develop in some patients such as lethargy, irregular movement of the body and headache.
- The disease resolves itself within 5 to 7 days but an infected person may shed the bacteria in their feces for a long time being asymptomatic and may cause a threat of spreading the infection.
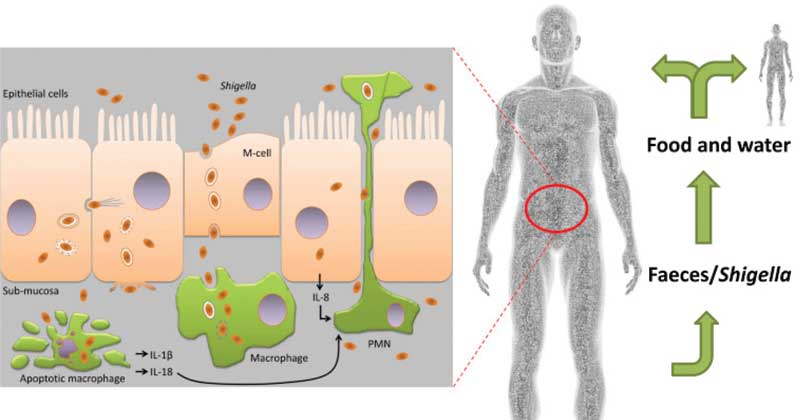
Mechanism of toxicity of Shigella infection
- The infection starts as the organism enters the body orally and reaches the large intestine.
- Shigella can resist the stomach pH and does not adhere to the small intestine as there is an increased movement of epithelial cells and fast liquid flux.
- Pathogens enter into the intestinal epithelium layer where M cells bind the organism in the vacuoles.
- The pathogen then escapes and travels to the macrophages which get phagocytized and induce apoptosis.
- In the large intestine, Shigella reproduce rapidly and moves through the epithelial layer spreading to neighbor cells causing tissue destruction and inflammation.
- S. flexneri is known to destroy mitochondria due to the release of proinflammatory cytokine IL-12 which results in necrosis in the host body.
- During inter and intracellular (cell-to-cell) movement, the pathogens are enveloped by a plasma membrane and start intracellular replication and cell-to-cell bacterial spread.
- It has been reported that the inflammation and ulceration of the mucosal layer are caused by the host’s immune system and are not associated with the intracellular multiplication of the pathogen.
- S. dysenteriae is known to produce Shiga toxin, a potent toxin that causes bloody diarrhea.
- This toxin enters into the host cell by endocytosis and terminates the protein synthesis mechanism resulting in the death of the host cells.
- The lipopolysaccharide (LPS) layer of the gram-negative bacteria also acts as an endotoxin which only activates once the cell gets destroyed and damages the epithelial tissues.
Laboratory diagnosis of Shigella
1. Bacterial culture methods
- A stool sample of the patient with clinical signs of dysentery should be taken and tested immediately as the organism remains viable outside the host body only for a limited time.
- The sample to be tested should be collected at the initial stage of infection to isolate the bacteria.
- MacConkey agar, Salmonella-Shigella agar and Xylose-Lysine Deoxycholate agar are the selective media used for the growth of Shigella.

2. Bioassays
- Various animals such as guinea pigs, rodents, rabbits and monkeys are administered orally to detect the effect of the pathogens.
- Some showed visible inflammatory reactions in the eye followed by tissue damage in the large intestine.
- However, the use of animals is restricted due to ethical issues.
3. Immunological assays
- Kits for enzyme immunoassay (EIA) are available for the detection of pathogens which is also known as dot blot assay.
- EIA kit has 94% efficiency and is usually cheap and easy to use.
- Other immunoassays are latex agglutination test, dipstick immunoassays and Wellcolex Color Shigella test (WCT-Shigella).
4. Molecular techniques
- Matrix-assisted laser desorption/ionization-time of flight mass spectrometry (MALDI-TOF MS) is the most reliable technique to detect the gene of Shigella in a short time.
- Conventional PCR increased the diagnosis by 50% by detecting the various species of Shigella.
- They can detect the target genes such as ipaH, virA, iral, LPS and plasmid DNA.
Treatment of Shigellosis
- A person with shigellosis symptoms must receive antibiotic treatment however in some cases Shigella develops resistance to antibiotics.
- Ciprofloxacin, ampicillin, sulfamethoxazole and nalidixic acid were used to show effectiveness against Shigella and are still in a clinical trial.
- For now, fluoroquinolones and azithromycin are the choice of antibiotics for shigellosis.
- Treatment depends on the severity of the infection and should start early in the course of illness.
- Oral rehydration and intravenous fluid therapy is a common treatment used for an infected person to replace the loss of electrolytes.
Prevention and Control of Shigellosis
- The most effective way of preventing shigellosis is appropriate sanitation, good personal hygiene and a proper way of disposing of feces.
- Food-borne shigellosis is transmitted through the fecal-oral route, therefore forbidding a person to prepare food showing symptoms of digestive disorder should be done.
- Washing fruits and vegetables with chlorinated water before consuming.
- Proper refrigeration of food products to avoid bacterial proliferation.
- Shigellosis usually occurs in under-developed and developing countries, therefore to minimize the cases educating people about the good practices of hygiene and sanitation, avoiding food and water that are fecally contaminated and encouraging them to take nutrition-rich foods during illness.
Shigellosis Frequently Asked Questions (FAQs)
Q. What is Shigellosis?
A. Shigellosis is a disease caused by Shigella species, responsible for causing acute gastrointestinal tract infections that damage the ileal and colonic epithelium and cause bacillary dysentery.
Q. Which bacteria causes Shigellosis?
A. Shigella flexneri, Shigella boydii, Shigella dysenteriae and Shigella sonnei causes Shigellosis in humans.
Q. What are the symptoms of Shigellosis?
A. Typical symptoms include fever, loss of appetite, abdominal pain, bloody or watery diarrhea, inflammation of the colon, fatigue, malaise, fever.
Q. Is Shigellosis contagious?
A. Yes, shigellosis is very contagious.
Q. Is Shigellosis a zoonotic disease?
A. Yes, shigellosis is a zoonotic disease.
Q. What is the treatment for Shigellosis?
A. Ciprofloxacin, ampicillin, sulfamethoxazole, and nalidixic acid were used to show effectiveness against Shigella and are still in a clinical trial. For now, fluoroquinolones and azithromycin are the choice of antibiotics for shigellosis. Oral rehydration and intravenous fluid therapy is common treatment used for an infected person to replace the loss of electrolytes.
Q. How is Shigella prevented?
A. The most effective way of preventing shigellosis is appropriate sanitation, good personal hygiene, and a proper way of disposing of feces, washing fruits and vegetables with chlorinated water before consuming, and proper refrigeration of food products to avoid bacterial proliferation.
Q. How is Shigellosis diagnosed?
A. Bacterial culture methods, Bioassays, Immunological assays, and Molecular techniques like MALDI-TOF MS and PCR helps in the diagnosis of Shigellosis.
References
- Mumy, K. L. (2014). Shigella. Encyclopedia of Toxicology, 254–255.
- Ashkenazi, S. (2018). Shigella Species. Principles and Practice of Pediatric Infectious Diseases, 842–846.e2.
- https://www.researchgate.net/publication/324720426_Shigellosis_A_Conformity_Review_of_the_Microbiology_Pathogenesis_and_Epidemiology_with_Consequence_for_Prevention_and_Management_issues
- https://www.ncbi.nlm.nih.gov/books/NBK7627/
