Shigella dysenteriae is a species of gram-negative, facultatively anaerobic, rod-shaped bacteria that is extremely pathogenic and causes severe dysentery.
Infection with this organism often leads to ulceration of the intestinal epithelium.
It is known to produce an exotoxin (Shiga toxin) which disrupts protein synthesis and produces endothelial damage.
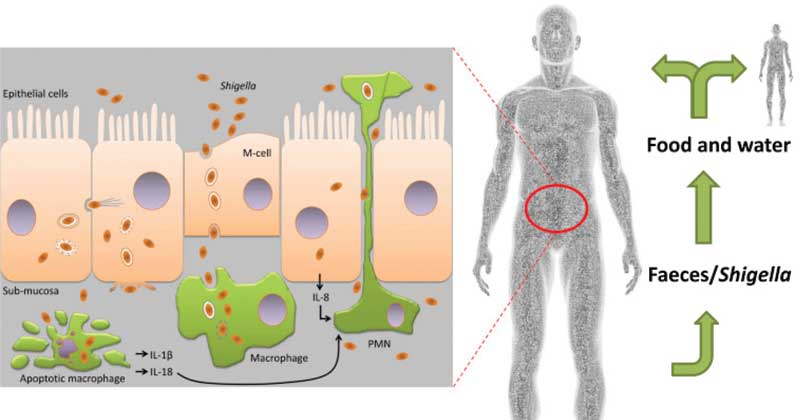
Figure: Shigella spread via fecal-oral and person-to-person transmission.
Image Source: https://doi.org/10.1016/j.micres.2015.08.006
Pathogenicity of Shigella dysenteriae
- Shigella cause disease by invading and replicating in cells lining the colon.
- Structural gene proteins mediate the adherence of the organisms to the cells, as well as their invasion, intracellular replication, and cell-to-cell spread.
- These genes are carried on a large virulence plasmid but are regulated by chromosomal genes. Thus the presence of the plasmid does not ensure functional gene activity.
- Rather than attaching to differentiated mucosal cells; they first attach to and invade the M cells located in Peyer patches.
- The type III secretion system mediates secretion of four proteins (IpaA, IpaB, IpaC, IpaD) into epithelial cells and macrophages.
- These proteins induce membrane ruffling on the target cell, leading to engulfment of the bacteria.
- Shigella lyse the phagocytic vacuole and replicate in the host cell cytoplasm (unlike Salmonella, which replicates in the vacuole).
- With the rearrangement of actin filaments in the host cells, the bacteria are propelled through the cytoplasm to adjacent cells, where cell-to-cell passage occurs. In this way, Shigella organisms are protected from immune-mediated clearance.
- Shigella survive phagocytosis by inducing programmed cell death (apoptosis). This process also leads to the release of IL-1β, resulting in the attraction of polymorphonuclear leukocytes into the infected tissues.
- This, in turn, destabilizes the integrity of the intestinal wall and allows the bacteria to reach the deeper epithelial cells.
- S. dysenteriae strains produce an exotoxin, Shiga toxin.
- Similar to Shiga toxin produced by STEC, this toxin has one A subunit and five B subunits.
- The B subunits bind to a host cell glycolipid (Gb3) and facilitate the transfer of the A subunit into the cell.
- The A subunit cleaves the 28S rRNA in the 60S ribosomal subunit, thereby preventing the binding of aminoacyl-transfer RNA and disrupting protein synthesis.
- The primary manifestation of toxin activity is damage to the intestinal epithelium; however, in a small subset of patients, the Shiga toxin can mediate damage to the glomerular endothelial cells, resulting in renal failure (HUS).
Clinical Manifestation of Shigella dysenteriae
A. Shigellosis
Shigellosis is characterized by:
- Abdominal cramps
- Diarrhea
- Fever
- Bloody stools
- The clinical signs and symptoms of the disease appear 1 to 3 days after the bacteria are ingested.
- Shigella initially colonize the small intestine and begin to multiply within the first 12 hours.
- The first sign of infection (profuse watery diarrhea without histologic evidence of mucosal invasion) is mediated by an enterotoxin.
- However, the cardinal feature of shigellosis is lower abdominal cramps and tenesmus (straining to defecate), with abundant pus and blood in the stool. It results from the invasion of the colonic mucosa by the bacteria.
- Abundant neutrophils, erythrocytes, and mucus are found in the stool.
- Infection is generally self-limited, although antibiotic treatment is recommended to reduce the risk of secondary spread to family members and other contacts.
- Asymptomatic colonization of the organism in the colon develops in a small number of patients and represents a persistent reservoir for infection.
B. Hemolytic Uremic Syndrome (HUS)
- Hemolytic-uremic syndrome (HUS) is a group of blood disorders characterized by low red blood cells, acute kidney failure, and low platelets.
- HUS can occur after S. dysenteriae type 1 infection.
- Convulsions may occur in children; the mechanism may be related to a rapid rate of temperature elevation or metabolic alterations and is associated with the production of the Shiga toxin.
- It is usually complicated by severe dysentery, intravascular volume depletion, and cardiovascular collapse, and has a higher morbidity and mortality rate than HUS associated with E. coli.
References
- Murray, P. R., Rosenthal, K. S., & Pfaller, M. A. (2013). Medical microbiology.Philadelphia: Elsevier/Saunders.
- https://www.ncbi.nlm.nih.gov/mesh?Db=mesh&term=Shigella+dysenteriae
- https://healthywa.wa.gov.au/Articles/S_T/Shigella-infection-and-dysentery
- https://www.sciencedirect.com/topics/medicine-and-dentistry/shigella-dysenteriae
- https://www.who.int/maternal_child_adolescent/documents/9241592330/en/
- http://textbookofbacteriology.net/Shigella.html

Thank you
The presentation is very nice and well explained