- Rapid Plasma Reagin (RPR) like the Venereal Disease Research Laboratory (VDRL) test is a screening test for syphilis which is a sexually transmitted infection caused by the spirochete bacterium Treponema pallidum.
- It is a rapid non-treponemal test that looks for non-specific antibodies in the blood of the patient that may indicate a syphilis infection.
- The test does not look for antibodies against the causative bacterium itself but rather for antibodies IgM and IgG against lipoprotein-like material released from damaged host cells caused by T. pallidum and possibly cardiolipin released from the treponemes. These antibodies are traditionally referred to as ‘reagins’.
- The tester antigen is prepared from a modified Venereal Disease Research Laboratory (VDRL) antigen suspension containing choline chloride to eliminate the need to heat inactivate serum, ethylenediaminetetraacetic acid (EDTA) to enhance the stability of the suspension, and finely divided charcoal particles as a visualizing agent.
Principle of RPR Test
The Rapid Plasma Reagin tests are macroscopic, non-treponemal flocculation card test that detect antibodies produced against antigens released by damaged host cells in patients suffering from syphilis. In the test, the RPR antigen is mixed with unheated or heated serum or with unheated plasma on a plastic-coated card. The antigen used for detection contains 0.03% cardiolipin, 0.21% lecithin, and 0.9% cholesterol in addition to choline chloride, EDTA and charcoal particles. If antibodies are present, they combine with the lipid particles of the antigen, causing them to agglutinate. The charcoal particles coagglutinate with the antibodies and show up as black clumps against the white card. If antibodies are not present, the test mixture is uniformly gray.
Requirements for RPR Test
Patient’s serum/plasma, RPR antigen suspension, Control serum samples, Plastic-coated RPR cards, mechanical rotator, pipettes.
Procedure of RPR Test
The test can be performed both qualitatively and quantitatively. Those tests that are reactive by qualitative test are subjected to quantitative test to determine the antibody titres.
Qualitative Method
- One drop (50 µl) of the test specimen, positive and negative controls is pipetted onto separate reaction circles of the card.
- Once spread smoothly, a drop of diluted antigen suspension is added to the measured volume of specimen, positive and negative controls. The antigen is not spread or moved.
- The card is gently placed on an automatic rotator and rotated continuously at 100 ± 2 rpm for 8 minutes.
- Following rotation, a brief hand rotation and tilting of the card (three or four to-and-fro motions) is performed to aid in differentiating nonreactive from minimally reactive results.
- Flocculation is checked macroscopically under high intensity light source.
Quantitative Method
- Dilute to an endpoint titer all serum specimens with rough nonreactive results in the qualitative test. Test each specimen undiluted (1:1), and in 1:2, 1:4, 1:8, and 1:16 dilutions.
- Place 50 µl of 0.9% saline in circles numbered 2 through 5. Do not spread the saline.
- Using a pipette, place 50 µl of serum in circle 1 and 50 µl of serum in circle 2.
- Mix the saline and the serum in circle 2 by drawing the mixture up and down in a pipette eight times avoiding bubble formation.
- Transfer 50 µl from circle 2 (1:2) to circle 3, and mix.
- Transfer 50 µl from circle 3 (1:4) to circle 4, and mix.
- Transfer 50 µl from circle 4 (1:8) to circle 5 (1:16), mix, and then discard the last 50 µl.
- Add exactly 1 free-falling drop (17 µl) of antigen suspension in each circle. DO NOT MIX.
- Place the card on the rotator under the humidifying cover and rotate the card for 8 minutes at 100 ± 2 rpm.
- Immediately remove the card from the rotator; briefly rotate and tilt the card by hand (three or four to-and-fro motions)
- If the highest dilution tested (1:16) is reactive, continue as follows:
- Prepare a 1:50 dilution of nonreactive serum in 0.9% saline to be used for making 1:32 and higher dilutions of the specimen to be tested.
- Prepare a 1:16 dilution of the test specimen by adding 0.1ml of serum to 1.5ml of 0.9% saline. Mix thoroughly.
- Place 50 µl of the 1:50 nonreactive serum diluent in circles 2 through 5 of an RPR card.
- Using a safety pipetting device with disposable tip, place 50 µl of the 1:16 dilution of the test specimen in circle 1 and 50 µl in circle 2.
- Using the same pipette and tip, make serial twofold dilutions. Complete test as described in steps above.
Result Interpretation of RPR Test
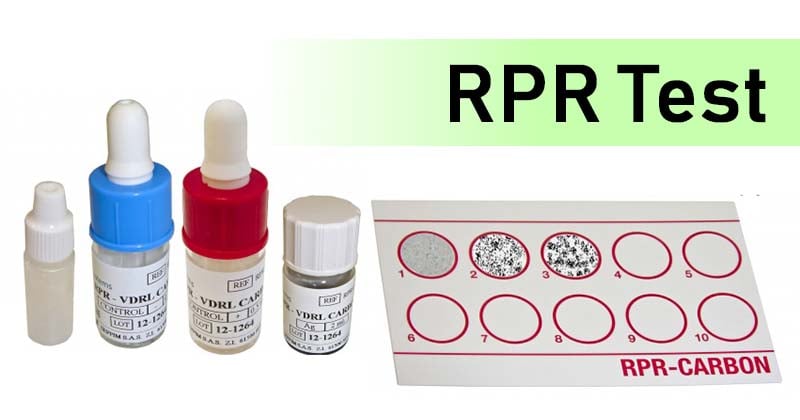
Positive test: Presence of characteristic antigen-antibody clumps (black) in the center or the periphery of the test circle indicate positive RPR test.
Negative test: Absence of antigen-antibody clumps. Indicated by slight roughness and no aggregates.
- All reactive serum requires serial dilution to estimate antibody titer. The titre is reported as the reciprocal of the highest dilution, which shows a positive test result.
- When the quantitative RPR card test is performed on patients with syphilis, a fourfold rise in titer in a repeat specimen may suggest an infection, a reinfection, or a treatment failure; a fourfold decrease in titer following treatment for early syphilis usually indicates that therapy was adequate.
Applications of RPR Test
- It is used mostly as the screening test for syphilitic infection. Combined with specific antibody testing, the RPR test allows confirming the diagnosis of active infection and starting treatment.
- Screening for syphilis is a routine part of pregnancy tests.
- The test for syphilis is also performed if being treated for another STI such as gonorrhea, infected with HIV, or if engaged in high-risk sexual activity.
Advantages of RPR Test
- The RPR test is an effective, easy to perform and a fast screening test.
- It is readily available in kit form for purchase.
- Results are observed without the use of a microscope.
- In addition to screening for syphilis, a titer can be used to track the progress of the disease over time and its response to therapy.
- Since, the organism Treponema pallidum cannot be cultured in artificial media, the screening of syphilis via serological testing such as RPR becomes important.
- Patient need not have the symptoms of syphilis for this test to be accurate. It can detect syphilis very effectively in patients without symptoms.
- Since it is a non-treponemal test (non-specific test) it is used to investigate syphilis along with other treponematose, Yaws and Pinta.
- More effective screening than VDRL test.
Limitations of RPR Test
- Without some other evidence for the diagnosis of syphilis, a reactive non-treponemal test such as RPR does not confirm pallidum infection. Any reactive RPR test must be confirmed with a specific or treponemal test such as TPHA, FTA-ABS test.
- The anti lipoidal antibodies detected are not only produced as a consequence of syphilis and other treponemal diseases, but also may be produced in response to nontreponemal diseases of an acute and chronic nature in which tissue damage occurs.
- The RPR test isn’t always accurate. For example, false-negative results may arise if an individual had syphilis for less than three months, as it could take long for the body to make antibodies. The test is also unreliable in late-stage syphilis.
- On the other hand, false-positive results can be seen in conditions like HIV, Lyme disease, malaria, pneumonia, systemic lupus erythematosus, IV drug use and tuberculosis.
- The antibodies produced as a result of a syphilis infection can stay in the body even after syphilis has been treated.
- A nonreactive RPR card test with clinical evidence of syphilis can be seen in early primary syphilis; in secondary syphilis, as a result of the prozone reaction; and in some cases of late syphilis.
- The RPR card test cannot be used to test spinal fluids.
- The RPR card test may be reactive in persons from areas where yaws, pinta or nonvenereal syphilis is endemic.
References
- Jameson JN, Kasper DL, Harrison TR, Braunwald E, Fauci AS, Hauser SL, Longo DL (2005). Harrison’s Principles of Internal Medicine (16th ed.). New York: McGraw-Hill Medical Publishing Division.
- https://www.cdc.gov/std/syphilis/manual-1998/chapt10.pdf
- Matthews HM, Yang TK, Jenkin HM. Unique lipid composition of Treponema pallidum (Nichols virulent strain). Infect Immun 1979; 24:713-9.
- https://www.urmc.rochester.edu/encyclopedia/content.aspx?contenttypeid=167&contentid=rapid_plasma_reagin_syphilis

Well simplified
Very informative
Thank you sir
Thanks
RPR