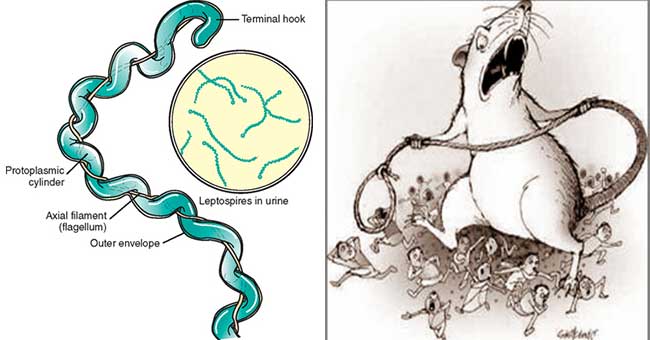
Pathogenesis of Leptospira interrogans
- Leptospires usually enter the body through the mucous membranes of the upper respiratory tract or the conjunctivae, or through abraded skin, following exposure to contaminated water, infected urine or animal tissues.
- Ingestion is considered to be less important.
- The severity of the leptospirosis depends on (a) host immunity, (b) virulence of infecting strain, and (c) the number of infecting leptospires.
- After entering through the mucosa (conjunctiva or oral) or abraded skin, L. interrogans spill over to the bloodstream and it multiplies in blood and tissues, resulting in leptospiraemia.
- After an incubation period of 1–2 weeks, there is a variable febrile onset during which spirochetes are present in the bloodstream.
- The infection presents with an influenza-like illness characterized by the sudden onset of headache, muscular pain, especially in the muscles of the lower back and calf, fever and occasionally rigors.
- Conjunctival suffusion and a skin rash may be seen in some cases.
- Many infections are mild or subclinical
- L. interrogans then disseminate hematogenously to various organs including brain, liver, lung, heart and kidney.
- They then establish themselves in the parenchymatous organs (particularly liver and kidneys), producing hemorrhage and necrosis of tissue and resulting in dysfunction of those organs (jaundice, hemorrhage, nitrogen retention).
- Leptospirosis is actually a generalized vasculitis.
- The pathogens damage mainly the endothelial cells of the capillaries, leading to greater permeability and hemorrhage and interrupting the oxygen supply to the tissues.
- Jaundice is caused by a non necrotic hepatocellular dysfunction.
- It manifests itself often as “aseptic meningitis” with an intense headache, stiff neck, and pleocytosis of the CSF.
- Disturbances of renal function result from hypoxic tubular damage. Kidney involvement in many animal species is chronic and results in the shedding of large numbers of leptospirae in the urine. Human urine also may contain spirochetes in the second and third weeks of disease.
- The illness is often biphasic which means bacteraemic phase is followed by an ‘immune’ phase, with the appearance of antibody and the disappearance of recoverable leptospires from the blood.
- After initial improvement, the second phase develops when the IgM antibody titer rises.
- Antigen antibody complexes are deposited in various organs.
- Agglutinating, complement-fixing, and lytic antibodies develop during the infection.
- Humoral immunity plays an important role in clearance of leptospires from the circulation.
- Furthermore, immune reactions of the host to leptospira appears to be responsible for many complications, such as meningitis and other clinical manifestations seen during the later stage of the disease.
Clinical manifestations of Leptospira interrogans
A. Anicteric leptospirosis
- Approximately, 90% of infections with L. interrogans manifest as a mild anicteric (absence of jaundice) form of the disease.
- It is biphasic; a septicemic phase occurs first, followed by immune phase.
- It is characterized by fever with chills, headache, and myalgias that set in after an incubation period of 7 to 12 days.
B. Icteric leptospirosis
- Approximately 10% of the patients develop icteric manifestations of the disease, otherwise known as Weil’s disease.
- The disease is characterized by the development of jaundice.
- The disease shows two distinct phases: septicemic and immune (leptospuric) phase.
- These two phases of illness are continuous and indistinguishable.
- First stage is the septicemia or leptospiremia stage.
- This stage is so called because during this phase, Leptospira organisms are usually isolated from the blood, CSF, and most tissues by culture.
- This stage is characterized by a nonspecific influenza-like illness with fever and myalgias.
- This phase lasts for 4–7 days.
- The first stage is followed by 1–3 days period of improvement during which the temperature falls down and the patient becomes afebrile and relatively asymptomatic.
- Immune or leptospuric stage: The second stage starts with the recurrence of fever. This stage is called immune or leptospuric stage, because circulating antibodies may be detected in serum or leptospira may be isolated from the urine, but not from blood or CSF. This stage occurs as a result of body’s immune response to infection.
- This stage is characterized by the diseases affecting specific organs, such as meninges, liver, kidney, and eye.
- Aseptic meningitis is the most important clinical manifestation.
- Profound jaundice, renal dysfunction, pulmonary dysfunction, hepatic necrosis, and hemorrhagic diastases are other severe manifestations.
- Mortality is very high with Weil’s syndrome.
- It may be as high as in cases of Weil’s syndrome associated with hepatorenal involvement and jaundice, and in older patients.