There are two types of Neisseria: pathogenic and non-pathogenic. Neisseria gonorrhoeae is a pathogenic Gram-negative bacterium that causes gonorrhea.

Albert Ludwig Sigesmund Neisser discovered the bacterium in 1879. Gonorrhea is a sexually transmitted infection (STI) and the causative agent of it is Neisseria gonorrhoeae, which is an obligatory human pathogen. It particularly affects young adults. This bacterium mostly causes urethritis in men and cervicitis in women and affects only humans.
Taxonomy and Classification of Neisseria gonorrhoeae
Table 1: Classification of Neisseria gonorrhoeae
| Domain | Bacteria |
| Phylum | Proteobacteria |
| Class | Betaproteobacteria |
| Order | Neisseriales |
| Family | Neisseriaceae |
| Genus | Neisseria |
| Species | gonorrhoeae |
Habitat of Neisseria gonorrhoeae
- Human is only the natural host.
- Found in human urogenital tract.
- Rectal carriage in healthy individuals.
- Typically seen in pus cells (intracellular)
- Found intracellularly in polymorphonuclear leukocytes, or a specific category of white blood cells with varying shapes of nuclei.
Morphology and Microscopy of Neisseria gonorrhoeae
- N. gonorrhoeae are oval shaped cocci which are 0.6-1 µm in diameter.
- They appear in pairs or flattened.
- It has pili on their surface.
- The organism observed in smears from purulent materials are intracellular within polymorphs and remaining are extracellular within the exudate.
- Non-sporing
- Non-capsulated
- Gram-negative diplococci flattened along the adjoining side
- Fastidious, capnophilic and susceptible to cool temperatures, drying and fatty acids
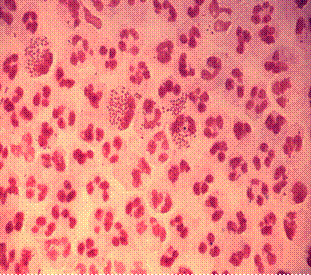
https://en.wikipedia.org/wiki/Neisseria_gonorrhoeae#/media/File:Gonococcal_urethritis_PHIL_4085_lores.jpg
Genome of Neisseria gonorrhoeae
- Circular DNA genome
- 2069 Genes
- 67 Structural RNA’s
- Genome Length: 2,153,922 nt
- Protein encoding genes: 2002
- G+C Content: 52.4%
- Have surface protein called Opa protein.
Cultural and Growth Characteristics of Neisseria gonorrhoeae
- It is a fastidious organism and requires complex media to grow like chocolate agar, thayer-martin medium etc.
- PH required is 7.2-7.6
- Requires complex media pre-warmed to 35- 37 °C
- Soluble starch added to neutralize fatty acid toxicity
- Grow best in moist atmosphere supplemented with CO2
- Produce acid from glucose, but not from other sugars
- Enriched media with antibiotics like vancomycin, colistin, nystatin etc and lysed blood are used as a selective medium.
- Small grey and glistening colonies are observed after 24hrs of incubation in selective media.
- It produces five types of colonies i.e. T1, T2, T3, T4, and T5.
- Type 1 and Type 2 produce small brown colonies and possess pili.
- Types 3 and 4 produce large granular, nonpigmented and non-piliated colonies.
Biochemical and Identification Tests of Neisseria gonorrhoeae
N. gonorrhoeae is oxidase positive, catalase positive, ferment only glucose with acid production, and do not ferment any other carbohydrates.
Virulence Factors and Pathogenesis of Neisseria gonorrhoeae
- The determinants of pathogenicity are capsule, pili, outer membrane proteins such as Por protein, Opa protein, Rmp proteins, cell wall LOS (endotoxin) and the peptidoglycan.
- Antiphagocytic, capsule-like negative surface charge
- Only fimbriated (piliated) cells (formerly known as colony types T1 & T2) are virulent
Outer membrane proteins (formerly Proteins I, II, & III):
Por (porin protein) prevents phagolysosome fusion following phagocytosis, thereby promoting intracellular survival
Opa (opacity protein) mediates firm attachment to epithelial cells and subsequent invasion into cells
Rmp (reduction-modifiable protein) protects other surface antigens from bactericidal antibodies (Por protein, LOS)
Acquisition of iron is mediated through Tbp 1 and Tbp 2 (transferrin-binding proteins), Lbp (lactoferrin binding protein) & Hbp (hemoglobin-binding protein)
Lipooligosaccharide (LOS) (Lipid A plus core polysaccharide but no O-somatic antigen
polysaccharide side chain) has endotoxin activity
IgA protease – destroys IgA
Acquisition of antibiotic resistance: Plasmid-encoded beta-lactamase production Chromosomally mediated changes in cellular permeability inhibit entry of penicillin, tetracycline, erythromycin, aminoglycosides
Pathogenesis
N. gonorrhoeae is responsible for causing Gonorrhea, which is a sexually transmitted disease. At first, N. gonorrhoeae attaches to mucosal cells or mucosal surfaces of urethra via pili and other surface proteins.
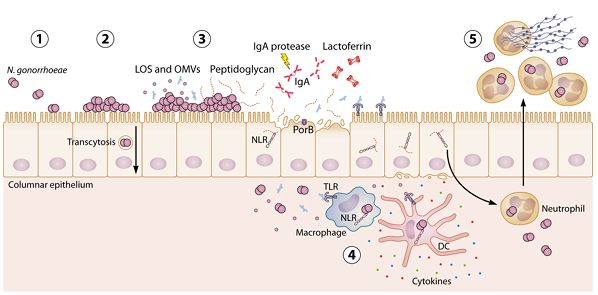
Induces production of inflammatory cytokines by epithelial cells.
Evades host immune system by changing surface proteins
Often asymptomatic infection
Pili, outer membrane proteins, lipopolysaccharides
Binding to epithelial surfaces
Passage through epithelium
Interaction with phagocytes
Permeability penetration of antibiotics is controlled by outer membrane Porin- P1 and Por
Requires
- Carbon dioxide
- Sulfur in form of cysteine
- Iron
The incubation period ranges from 2 to 8 days.
Epidemiology and Transmission of Neisseria gonorrhoeae
Almost 3 million new cases of Gonococcal disease are reported each year, mostly asymptomatic (90% in women and 40% in men). Most of them are undiagnosed, which is the main reason for the spread of the disease. Unmarried, 20-24 age groups of people are often infected. N. gonorrhea is usually transmitted through sexual contact, mother to infants during birth, and rarely from inanimate objects such as soiled towels etc. Asymptomatic carriage is major reservoir.
Clinical Manifestations of Neisseria gonorrhoeae
Most infections among men are acute and symptomatic with purulent discharge and dysuria, known for painful urination, after 2-5 days incubation period. Male host seeks treatment early preventing serious sequelae, but not soon enough to prevent transmission to other sex partners. The two bacterial agents primarily responsible for urethritis among men are N. gonorrhoeae and Chlamydia trachomatis.
As for women, they often have asymptomatic or have atypical indications (subtle, unrecognized S/S); often untreated until PID complications develop. Pelvic inflammatory disease (PID) may also be asymptomatic, but difficult diagnosis accounts for many false negatives. It can cause scarring of fallopian tubes leading to infertility or ectopic pregnancy. Gonococcal vulvovaginitis is a rare form of gonorrhea which occurs in young girls (mostly prepubertal girls).
Anorectal gonorrhea is found in homosexual men and women.
Laboratory Diagnosis of Neisseria gonorrhoeae
Specimens: Urethral and cervical discharge of acute stage, mid-stream urine
Microscopy
Gram-negative diplococci, but in women, due to the presence of normal flora, it’s difficult to isolate gram-negative bacteria.
For the rapid diagnosis of the N. gonorrhoeae, direct immunofluorescence using anti- N. gonorrhea monoclonal antibody and hybridization techniques are used.
Culture
N. gonorrhoeae is a fastidious organism. It cannot tolerate temperature changes and is intolerant of drying. Chocolate agar and modified Thayer-Martin medium are used as a selective medium for its growth. It requires high amount of CO2 for growth. Colonies appear after 24-48 hrs. of incubation. In cases of suspected sexual abuse, culture is the only accepted test for legal purposes.
Biochemical test
It is an oxidase- positive and ferments glucose with acid only.
Serology
Serological tests are mostly done for identifying asymptomatic infections in females and in complicated gonorrheal infections, mostly, when the bacteria can’t be cultured. Crude Antigen tests and Purified Antigen Tests are commonly used rapid tests. The most common test is the Gonococcal Complement Fixation Test (GCFT). It uses crude extracts of bacterium. Purified Antigen tests are the newer methods which use modern techniques: RIA (Radioimmunoassay) and ELISA (Enzyme-Linked Immunosorbent Assay).
Treatments of Neisseria gonorrhoeae
Antibiotics are mainly used for the treatment of gonorrhea in adults. The Centers for
Disease Control and Prevention recommend the antibiotic ceftriaxone for the emerging strains of drug-resistant N. gonorrhoeae. Even after the uptake of antibiotic, it can still be transmitted for upto seven days. Therefore, CDC recommends getting tested for gonorrhoeae three months after treatment. As for the Patients with PID, combination of antibiotics (ceftriaxone and tetracycline) is used.
Prevention and Control of Neisseria gonorrhoeae
Vaccination plays no role in prophylaxis because of antigenic variation in pilin proteins and phase variation. Tracing of contacts, health education and other general measures can be used to control gonorrhoeae. Using condoms as a barrier also can greatly reduce the rate of transmission.
References
- Chakraborty P et al 1976 Gonococcal and Nongonococcal urethritis. Antiseptic 73: 549.
- Knapp JS 1988 Historical perspective and identification of Nesseria and related species. Clin Microbiol Rev 1: 415-431.
- Ng, L. K., & Martin, I. E. (2005). The laboratory diagnosis of Neisseria gonorrhoeae. The Canadian journal of infectious diseases & medical microbiology = Journal canadien des maladies infectieuses et de la microbiologie medicale, 16(1), 15–25. https://doi.org/10.1155/2005/323082
- Hill, S. A., Masters, T. L., & Wachter, J. (2016). Gonorrhea – an evolving disease of the new millennium. Microbial cell (Graz, Austria), 3(9), 371–389. https://doi.org/10.15698/mic2016.09.524
- Ghanem KG. Clinical manifestations and diagnosis of Neisseria gonorrhoeae infection in adults and adolescents. https://www.uptodate.com/contents/search. Accessed Sept. 21, 2023.
- Casper W. A. (1937). The Serological Classification of Gonococci by Comparative Agglutination. Journal of bacteriology, 34(4), 353–379. https://doi.org/10.1128/jb.34.4.353-379.1937
