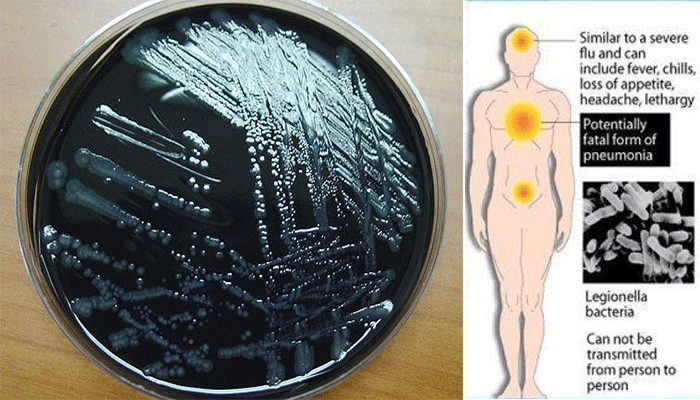
Laboratory diagnosis of Legionella pneumophila
Specimen: Respiratory secretions (sputum, bronchial aspirate or washings), as well as pleural fluid, lung biopsy or autopsy material.
Microscopy
- Legionellae in clinical specimens stain poorly with Gram stain and the small, intracellular bacteria are rarely recognized.
- The organism will stain with nonspecific methods, such as Dieterle silver stain, but this stain is used with tissue specimens and not sputum.
- The most sensitive way of detecting legionellae microscopically in clinical specimens is to use the direct fluorescent antibody (DFA) test, in which fluorescein-labeled monoclonal or polyclonal antibodies directed against Legionella species are used.
- Tests using monoclonal reagents are specific; however, false-positive reactions are common with the polyclonal reagents.
- Unfortunately, the sensitivity of the DFA test is low because (1) the antibody preparations are serotype- or species-specific and (2) many organisms must be present for detection.
- The latter problem is a result of the relatively small size and predominantly intracellular location of the bacteria.
- Because of the problems with the DFA test, microscopy has been replaced with antigen detection tests in most laboratories.
Culture
- Cultures are made on Buffered Charcoal Yeast Extract (BCYE) medium with and without antibiotics added to suppress other respiratory tract flora.
- Potentially contaminated material such as sputum or post-mortem material may also be heated at 50°C for 30 min in order to diminish growth by less heat-stable respiratory tract organisms that may inhibit growth of legionellae in culture.
- In heavy infections, growth on BCYE medium may appear after incubation for 48 h at 36°C in air, preferably enriched with 2.5% carbon dioxide.
- Colonies are 3 to 4 mm in diameter, gray-white to bluegreen, glistening, convex, and circular and may exhibit a cut-glass type of internal granular speckling colonies having a ‘cut glass’ appearance by plate microscopy, and those fluorescing blue–white under ultraviolet light, are Gram stained, and subcultured on to blood agar or cysteine-deficient medium to show that they will not grow on these media.
- Cultures are identified by use of specific antisera in an immunofluorescence test or by gene sequencing.
Antigen tests
- Rapid detection of Legionella antigen in urine and other body fluids has been accomplished by enzyme immunoassay (EIA) and immunochromatography.
- Antigen may be present in the prodromal period and by 3 days after the onset of symptoms.
- The examination of urine for legionella antigen by enzyme-linked immunosorbent assay (ELISA) is a rapid and specific method of identifying L. pneumophila as the likely cause of a pneumonia.
- Most legionella infections are now diagnosed by urine antigen tests, but failure to detect urinary antigen does not exclude infection with legionellae other than L. pneumophila serogroup 1.
Serology
- Although antibodies take at least 8 days to develop after the onset of infection, some patients may not reach hospital until this period has elapsed, so it is worthwhile examining serum for antibodies to L. pneumophila on admission to hospital.
- Further sera should be taken at intervals to show the development of antibodies or a rise in antibody titre.
- Antibodies usually develop after 8–10 days of illness and then increase in titre, but some patients may not produce antibody for some weeks or, rarely, for several months.
- A four-fold or greater rise in antibody titre in a typical clinical case indicates infection with
- A single titre of 256 or more is presumptive of infection.
- Most patients with legionellosis have been diagnosed retrospectively by detection of a fourfold rise in anti- Legionella antibody with an indirect fluorescent antibody (IFA) test.
- Serum specimens should be tested no closer than 2 weeks apart.
- Diagnostic efficacy associated with serologic testing increases with the collection and testing of acute and convalescent paired sera.
- Convalescent sera should be collected at 4, 6, and 12 weeks following the appearance of the disease.
- Disease is confirmed by a fourfold rise in titer to more than 128.
- A single serum with a titer of more than 256 and a characteristic clinical picture may be presumptive for legionellosis; however, because as many as 12% of healthy persons yield titers as high as 1:256, this practice is strongly discouraged.
Nucleic Acid Amplification
- Molecular methods are predominantly research based and are becoming increasingly available in reference andpublic health laboratories.
- The BD Probe Tec assay is only available for sputum specimens and detects serotype.
- The direct detection of Legionella nucleic acid by conventional and real-time polymerase chain reaction (PCR) has the potential to offer rapid results and increased sensitivity on respiratory and urine samples over current methods.
Treatment of Legionellosis
- An intravenous macrolide (often azithromycin) is the standard therapy in Legionella
- In severe cases a fluoroquinolone (usually ciprofloxacin) or rifampicin is usually added.
- Aminoglycoside and β-lactam antibiotics are not effective.
- Macrolides (erythromycin, azithromycin, telithromycin, and clarithromycin), quinolones (ciprofloxacin and levofloxacin), and tetracyclines (doxycycline) are effective.
- Prolonged therapy, upto 3 weeks, may be required depending on the clinical situation.
- Therapy should not be discontinued until the patient has been a febrile for 48–72 hours.
Prevention and control of Legionellosis
- Prevention of legionellosis requires identification of the environmental source of the organism and reduction of the microbial burden.
- Hyperchlorination of the water supply and the maintenance of elevated water temperatures have proved moderately successful.
- Because a single case of legionellosis may reflect a larger outbreak, clinical diagnosis is often the critical first step in prevention.