Hemostasis is the physiological process of stopping bleeding (hemorrhage). It protects the body from blood loss and exsanguination and restores blood circulation within the blood vessels.
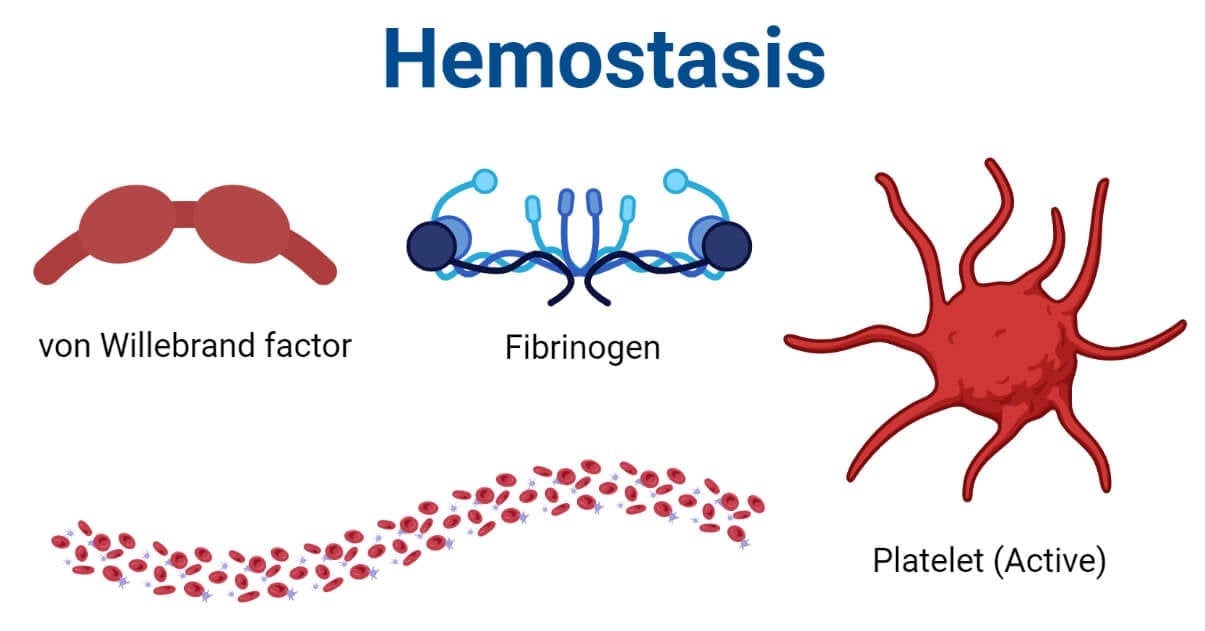
In general, it includes the conversion of liquid blood into solid (gel) form which plugs the ruptured blood vessel and prevents from blood loss. The body will then heal the ruptured vessel and repair the vessel for closed circulation.
Hemostasis Stages
Hemostasis can broadly be classified into two stages; (i) primary hemostasis, and (ii) secondary hemostasis.
- The primary hemostasis is the process of formation of the soft platelet plugs around the ruptured point. It is the first strategy adopted by the body to prevent blood loss. In this process, collagens are activated and accumulated in and around the area of the ruptured blood vessel. These accumulated collagens attract platelets and make them stick together to form a seal of the platelet. Besides, the platelets will induce vasoconstriction and release of factors which will attract more platelets in that ruptured site.
- The secondary hemostasis is the process of formation of fibrin fiber which will solidify the soft platelet plug into a hard and strong fibrin clot. It is induced after the primary hemostasis and involves a complex cascade which is described below in detail.
Clotting Factors
Clotting factors are the plasma proteins that help in the formation of blood clots.
These are the primary elements that form and maintain blood clots. These proteins are found freely floating in blood plasma mostly in the inactivated form. Once the body detects hemorrhage, these factors are activated and incorporated into the hemostasis cascade to form the blood clot.
- The major clotting factors are fibrinogen and prothrombin which forms fibrin and thrombin proteins respectively after activation and forms blood clots. However, there are more than 30 clotting factors that are involved in the complex process of hemostasis. The thirteen primary clotting factors are designated by the Roman numeral I to XIII while the other remaining factors and cofactors are named differently.
The primary clotting factors involved in hemostasis with their major functions are tabulated below.
| Clotting Factor (in numeral form) | Clotting Factor (name) | Functions |
| Factor I | Fibrinogen | Convert into fibrin fiber which forms a blood clot |
| Factor II | Prothrombin | Activates platelets and clotting factors I, V, VII, VIII, XI, XIII, etc. during the clotting process |
| Factor III | Thromboplastin (Tissue factor) | Initiation of thrombin formation |
| Factor IV | Calcium Ion | Initiates and regulates the binding of coagulation factors and phospholipids and acts as a cofactor of several other clotting factors |
| Factor V | Proaccelerin (Labile factor) | Co-factor of factor X |
| Factor VI | (Name unassigned) | Co-factor of serine protease factor XaForms prothrombinase complex |
| Factor VII | Proconvertin (Stable factor) | Promote the formation of prothrombin conversion into thrombinActivate factor IX and factor X |
| Factor VIII | Antihemophilic factor A | Combine with factor IXa and accelerate the activation of factor X by IXa |
| Factor IX | Antihemophilic factor B(Plasma thromboplastin)(Christmas factor) | Activate the factor X |
| Factor X | Stuart-Prower factor | Form prothrombinase complexActivate factor II |
| Factor XI | Antihemophilic factor C | Co-factor of factor IX and activate it |
| Factor XII | Hageman factor | Activate factor VII, factor XI, plasminogen |
| Factor XIII | Fibrin stabilizing factor | Promotes crosslinking of fibrin fibers |
Other factors like Fibronectin, von Willebrand factor, Antithrombin III, High molecular weight (HMW) kininogen, Heparin cofactor II, Plasminogen, etc. are also involved in hemostasis.
Mechanism of Hemostasis
As soon as the blood vessel rupture exposing the components inside the vessel wall into the blood and blood leaks outside the vessels, the hemostasis mechanism is triggered. It can be completed within seconds (around 15 seconds) or may take several hours based on the physiological and biochemical status of the person and the site and the degree of blood vessel rupture.
It is a complex process that can be described into three major steps viz. vascular spasm, platelet plug formation, coagulation, and the last step of fibrinolysis.
1. Vascular Spasm
Vascular spasm, also known as vasoconstriction, is the initial response that falls in primary hemostasis. As the endothelium cells are damaged during the vascular rupture, endothelin-1 (a vasoconstrictor) is released which mediates the vasoconstriction. The damaged endothelium of the vessel exposes other chemical components like sub-endothelial collagen, ATP (adenosine triphosphate), von Willebrand factor, and inflammatory mediators into the circulation. All of these promote vasoconstriction.
The sub-endothelial collagens and von Willebrand factors promote platelet accumulation and adhesion in that ruptured site. The attached platelets rupture and release serotonin, ADP (adenosine diphosphate), and thromboxane A2. All these components of the platelets further increase vasoconstriction. During the rupture of the blood vessel, local pain receptors initiate reflexes which further promote the vascular spasm.
The effect of vascular spasm is more promising in smaller vessels with minor rupture. The effect may last for 30 minutes to several hours.
2. Platelet Plug Formation
The freely floating platelets in the circulation begin to clump together forming spiked and sticky platelet clumps and attaching over the exposed vesicular lining and collagen. Under the influence of von Willebrand factors, the platelet plug stabilizes and further accumulates over the exposed endothelial tissue. These attached platelets release their contents, mainly the ADP, further attracting other platelets toward that site. These platelets bound with collagen and endothelial lining form a temporary seal called the platelet plug.
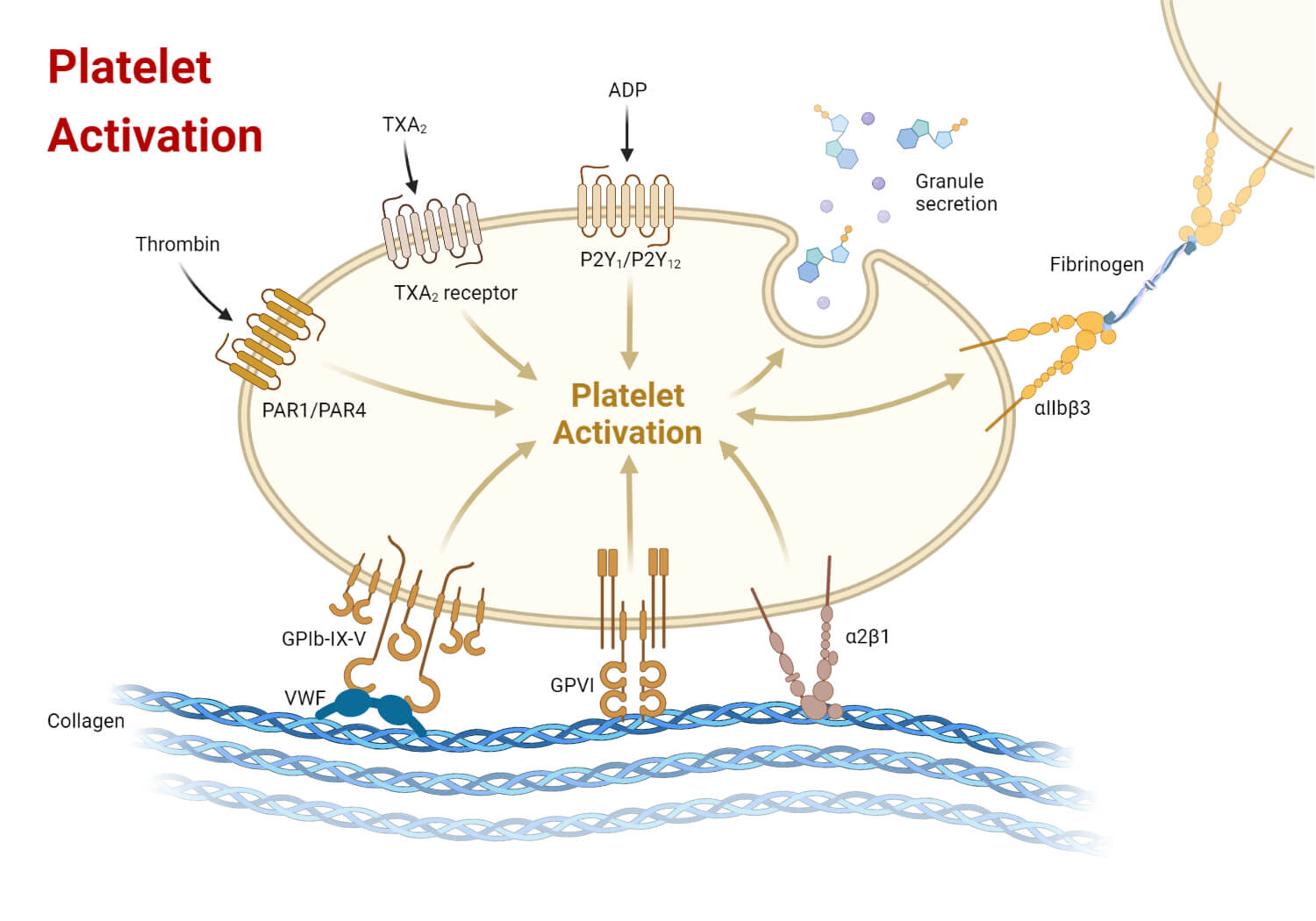
The platelet plug temporarily seals the vessel and prevents or slows down the rate of blood loss. This process results in primary hemostasis. Once the platelet plug is formed, the clotting factors are activated and the secondary hemostasis (blood coagulation process) begins.
3. Coagulation (Clotting)
Blood coagulation also called blood clotting, is the process of solidification of the blood due to the formation of fibrin fiber-associated blood clots. It is the secondary hemostasis stage and results in a stable solid blood clot. The overall process completes three major tasks; first, the activation of clotting factors, second the conversion of prothrombin into thrombin, and finally the conversion of fibrinogen into fibrin fiber.
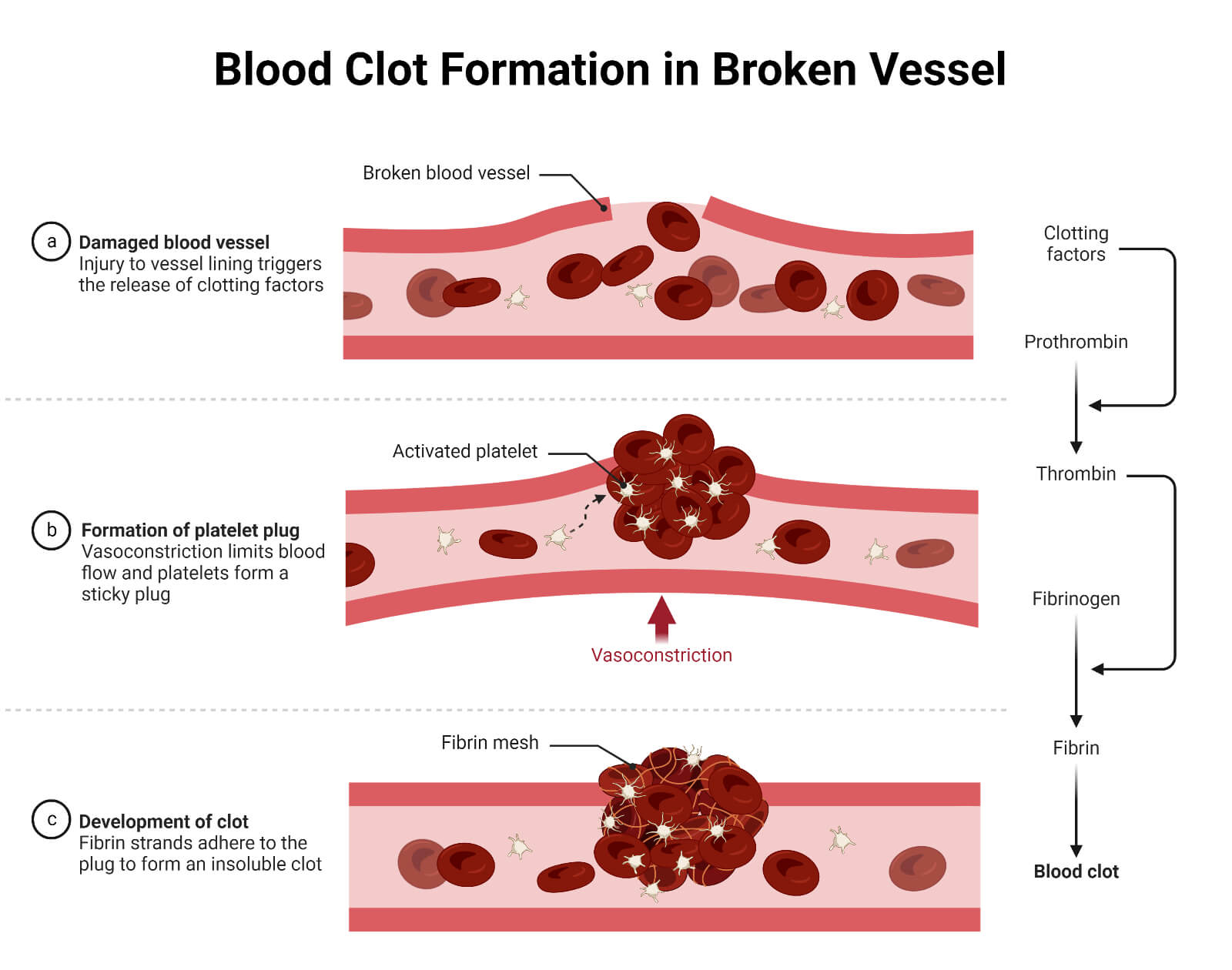
Coagulation Pathways
The coagulation process, also called coagulation cascade, is initiated through two different pathways; the extrinsic pathway and the intrinsic pathway, leading to a final common pathway of activating and stabilizing fibrin. The fibrin traps the platelets and blood cells forming a stable, gelatinous, and robust clot that ceases the hemorrhage.
The Extrinsic Pathway (Tissue Factor Pathway)
It is one of the initial cascades leading to the activation of factor X. It is a very fast and explosive pathway that begins immediately after the exposure of tissue factor (factor III) on circulation, and is completed within about 15 seconds of the exposure. It is induced by the tissue factor, hence the pathway is also known as the tissue factor pathway.
Factor III (TF) contacts factor VII (FVII) in circulation and forms the TF-FVIIa complex (activated FVII). The TF-FVIIa complex then leads to the activation of factor X (FX) triggering the common pathway.
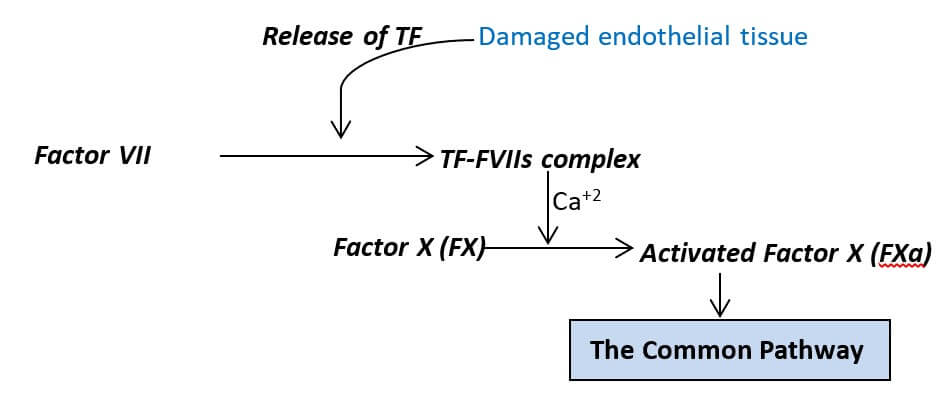
The Intrinsic Pathway (Contact Activation Pathway)
It is another cascade leading to the activation of factor X. It is comparatively complex and very slow than the extrinsic pathway, and usually takes about 1 to 6 minutes to form a blood clot. All the factors involved in this process are found within the circulation and the process begins when factor XII comes into contact with foreign materials (endothelial cells, or their contents, collagen, or other extravascular components), hence it is also called the contact activation pathway.
The cascade begins when a complex of factor XII (FXII), HMW kininogen (HMWK), and prekallikrein is formed over the collagen fibers. In the complex, the prekallikrein is activated into kallikrein which in turn activates the FXII and forms the activated FXII (FXIIa). The FXIIa, in the presence of Ca+2 ions, catalyzes the conversion of the clotting factor XI (FXI) into FXIa, its activated form. Sequentially, the FXIa, in the presence of Ca+2 ions, catalyze the conversion of the clotting factor IX (FIX) into its activated form, FIXa. The FIXa, in presence of the Ca+2 ions and platelet phospholipids (PL), combines with the activated factor VIII (FVIIIa) and forms the FIXa-FVIIIa complex. This protein complex then activates the factor X (FX) triggering the common pathway.
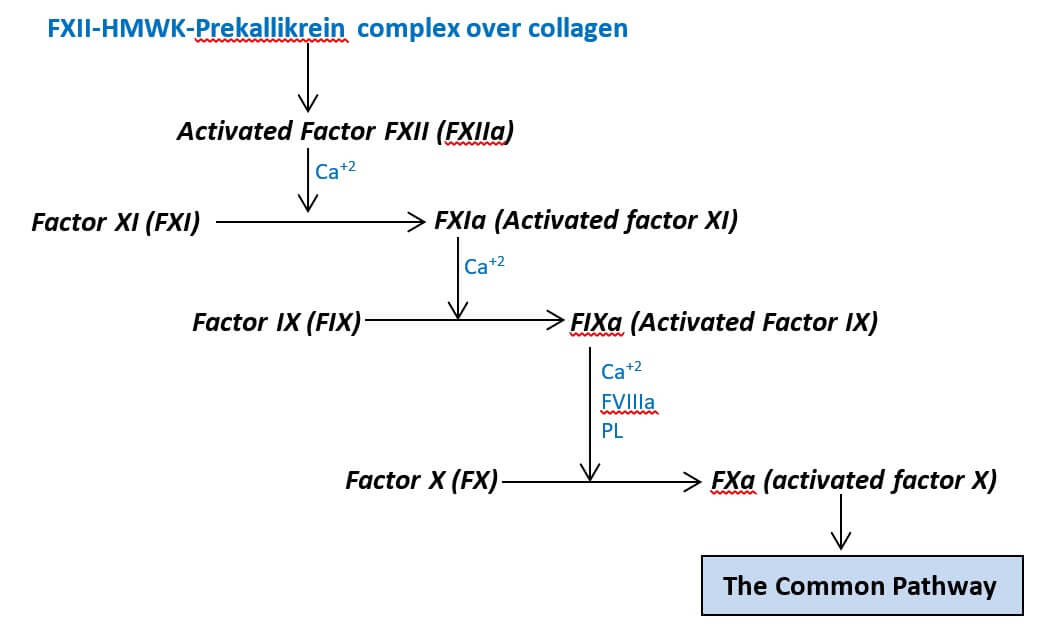
The Common Pathway
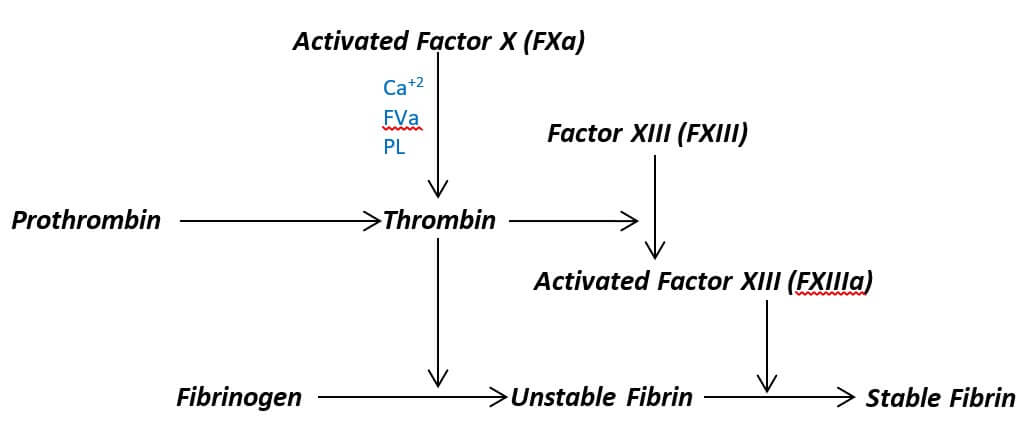
It is the final stage of the blood coagulation cascade which begins after the activation of factor X. The activated factor X (FXa) combines with activated factor V (FVa) and the Ca+2 ions on the phospholipid (PL) surface of the platelets and forms the prothrombinase complex. This complex activates the prothrombin (factor II) into thrombin (activated factor II (FIIa)).
Thus formed thrombin serves two primary functions; first, it activates fibrinogen (factor I) into fibrin (activated factor I (FIa)), and second, it activates fibrin stabilizing factor (Factor XIII (FXIII)) into activated form (activated factor XIII (FXIIIa)). The FXIIIa then stabilizes the fibrin fiber leading to the formation of a stable fibrin blood clot.
4. Fibrinolysis
It is the process of degradation of the fibrin fiber to remove the blood and restore normal blood flow. After the formation of a blood clot healing of the ruptured vessels begins. When the vessel is completely healed, then the fibrin is lysed in a complex process called fibrinolysis.
Factor XII, protein catabolizing enzymes, and other co-factors activate the plasminogen into plasmin. The activated plasmin then gradually breaks down the fibrin degrading the stable clot.
If the process is induced via chemicals or physical stress, then the process of degradation of the fibrin blood clot is called thrombolysis.
After fibrinolysis/thrombolysis, the blood clot is removed, and the blood circulation continues as usual.
Significance of Hemostasis
- Prevents excessive and uncontrolled blood loss and exsanguination.
- It helps to maintain homeostasis.
- Prevents from deposition of blood in internal organs during the bursting of blood vessels internally by quickly checking the bleeding process.
- It triggers the healing process of the ruptured vessels.
- Coagulation coincides with immune response and traps pathogenic microbes in the blood clot.
References
- Ross & Wilson Anatomy & Physiology in Health and Illness. 13th ed. Churchill Livingstone Elsevier. ISBN 978-0-7020-7276-5
- Betty Davis Jones. 3rd ed. Comprehensive medical terminology.
- Marieb, Elaine Nicpon; Hoehn, Katja (2010). Human Anatomy & Physiology (8th ed.). San Francisco: Benjamin Cummings. pp. 649–50.
- Johnson AB, Burns B. Hemorrhage. [Updated 2022 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK542273/
- LaPelusa A, Dave HD. Physiology, Hemostasis. [Updated 2022 May 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK545263/
- Barmore W, Bajwa T, Burns B. Biochemistry, Clotting Factors. [Updated 2022 May 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507850/
- Difference Between Intrinsic and Extrinsic Pathways in Blood Clotting | Compare the Difference Between Similar Terms
- Furie, Bruce. “bleeding and blood clotting”. Encyclopedia Britannica, 18 Feb. 2019, https://www.britannica.com/science/bleeding. Accessed 16 January 2023.
- What is hemostasis? – Siemens Healthineers (siemens-healthineers.com)
- Hemostasis: Causes & Treatment Options – Medicine.com
- List the clotting factors. (byjus.com)
- Clotting Factors | Lab Tests | 5MinuteConsult
- Hemostasis: Stages and How the Process Stops Blood Flow (clevelandclinic.org)
- Bleeding and blood clotting – The extrinsic pathway of blood coagulation | Britannica
- Hemostasis – Anatomy & Physiology (hawaii.edu)
- Coagulation. (2023, January 1). In Wikipedia. https://en.wikipedia.org/wiki/Coagulation
- Hemostasis – Hemostasis.com
- Embolism – NHS (www.nhs.uk)
- Hypocoagulability – an overview | ScienceDirect Topics
- Senst B, Tadi P, Basit H, Jan A. Hypercoagulability. 2022 Sep 26. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan–. PMID: 30855839.
- Sabih A, Babiker HM. Von Willebrand Disease. [Updated 2022 Aug 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459222/
- What is von Willebrand Disease? | CDC
