- Embryo refers to the early developmental stage of an animal while it is in the egg or within the uterus of the mother.
- In humans the term is applied to the unborn child until the end of the seventh week following conception; from the eighth week, the unborn child is called a fetus.
- Embryo transfer refers to a step in the process of assisted reproduction in which embryos are placed into the uterus of a female with the intent to establish a pregnancy.
- This technique may be used in humans or in animals, in which situations the goals may vary.
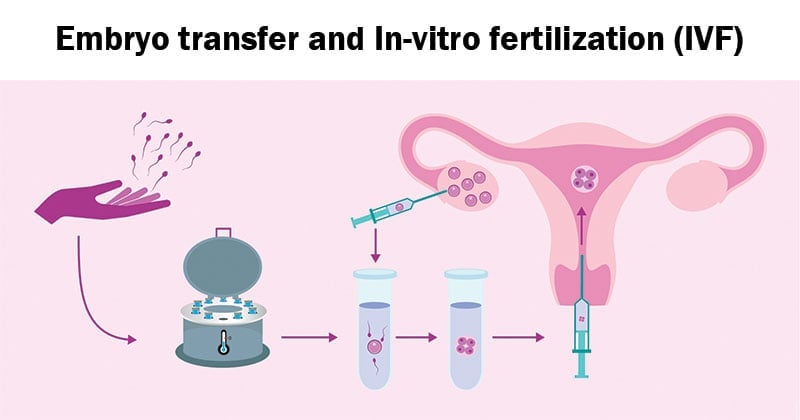
Original Image Source: https://www.invitra.com/en/ivf-with-donor-sperm/ivf-sperm-donor/
Original Article: https://www.invitra.com/en/ivf-with-donor-sperm/ By Andrea Rodrigo BSc, MSc (embryologist), Mark P. Trolice MD, FACOG, FACS, FACE (reproductive endocrinologist) and Sandra Fernández BA, MA (fertility counselor).
Embryo transfer and In-vitro fertilization (IVF)
- An embryo transfer is the last part of the in vitro fertilization (IVF) process.
- During IVF, fertility medications are used to stimulate the ovaries into releasing healthy eggs.
- These eggs are then removed from a woman’s ovaries and fertilized in a lab. Once the fertilized eggs have multiplied, the embryos are transferred to the woman’s uterus.
- For a pregnancy to begin, the embryo must then attach itself to the wall of her womb or uterus.
- The objective of embryo transfer is to facilitate conception following fertilization from the in vitro fertilization procedure.
- Embryos are generally transferred to the woman’s uterus at the 2-8 cell stage.
- Embryos may be transferred anytime between day 1 through day 6 after the retrieval of the egg, although it is usually between days 2-4.
- Some clinics are now allowing the embryo to reach blastocysts stage before transferring, which occurs around day 5.
The Embryo Transfer Technique
Choice of Embryos:
- Around 2 or 3 days before the embryo transfer, the doctor will choose the best eggs to transfer to the womb.
- There are many processes available to aid selection, though non-invasive methods such as metabolomic profiling are being tested.
- Metabolomic profiling is the process of selecting the most beneficial eggs based on a number of different factors.
Fertilization and Culture:
- These eggs will then be fertilized in a lab and left to culture for 1-2 days.
- If many good quality embryos develop, the ones that are not going to be transferred can be frozen.
The Transfer:
Embryo transfer is a 15-minute procedure accomplished by inserting a catheter (preloaded with embryos) into the uterine cavity.
- The embryo transfer process is similar to the process for a pap smear.
- The doctor will insert a speculum into the woman’s vagina to keep the vaginal walls open.
- Using ultrasound for accuracy, the doctor will then pass a catheter through the cervix and into the womb.
- From there, the embryos are passed through the tube and into the womb.
- The process is usually pain-free and rarely requires any sedatives.
Types of Embryo Transfer
Once fertilization has occurred, there are a few different options available for embryo transfer:
- Fresh embryo transfer: Once eggs have been fertilized, they are cultured for 1-2 days. The best embryos are chosen to transfer directly to the woman’s uterus.
- Frozen embryo transfer: Any healthy embryos that were not used in the first transfer can be frozen and stored for future use. These can be thawed and transferred to the uterus.
- Blastocyst embryo transfer: If many healthy embryos develop after the fertilization, it is common to wait to see if the embryos develop into blastocysts. Blastocyst embryo transfer has a higher success rate than the standard embryo transfer on day 3. However, recent studies suggest that it may pose risks later in pregnancy and should not always be recommended.
- Assisted hatching (AH): A study in the Reproductive Biomedicine Online found that the process of assisted hatching – weakening the outer layer of the embryo before it is transferred to the uterus – does not improve pregnancy and implantation rates in women who are having fresh embryos transferred. The researchers noted, however, that women having frozen 1embryos implanted do benefit from having their embryos treated in this way.
Conditions for Embryo Transfer
Embryo transfer is needed in cases where natural fertilization is not an option or has difficulty occurring. There are many reasons for embryo transfer, including:
- Ovulation disorders: If ovulation is infrequent, fewer eggs are available for successful fertilization.
- Damage to Fallopian tubes: The Fallopian tubes are the passageway through which the embryos travel to reach the uterus. If the tubes become damaged or scarred, it is difficult for fertilized eggs to safely reach the womb.
- Endometriosis: When tissue from the uterus implants and grows outside of the uterus. This can affect how the female reproductive system works.
- Premature ovarian failure: If the ovaries fail, they do not produce normal amounts of estrogen or release eggs regularly.
- Uterine fibroids: Fibroids are small, benign tumors on the walls of the uterus. They can interfere with an egg’s ability to plant itself in the uterus, preventing pregnancy.
- Genetic disorders: Some genetic disorders are known to prevent pregnancy from occurring.
- Impaired sperm production: In men, low sperm production, poor movement of the sperm, damage to the testes, or semen abnormalities are all reasons natural fertilization may fail.
Risks and Precautions of embryo transfers
- The risks of embryo transfers themselves are very low.
- These risks are mostly related to increased hormonal stimulation, causing an increased risk such as a blood clot blocking a blood vessel.
- The woman can also experience bleeding, changes in her vaginal discharge, infections, and complications of anesthesia if it is used. The risk of a miscarriage is about the same as in natural conception.
- The greatest risk of embryo transfer is the chance of multiple pregnancies. This occurs when multiple separate embryos attach to the uterus.
- This may increase the risk of stillbirth and children born with disabilities and is more common in pregnancies due to IVF than natural conception.
References
- https://www.britannica.com/science/embryo-human-and-animal
- http://americanpregnancy.org/infertility/embryo-transfer/
- https://www.verywellhealth.com/what-to-expect-during-an-embryo-transfer-2616453
- https://www.medicalnewstoday.com/articles/314571.php
- https://www.pacificfertilitycenter.com/treatment-care/in-vitro-fertilization/ivf-tour/embryo-transfer
- https://www.ivf1.com/embryo-transfer/
- https://www.invitra.com/en/ivf-with-donor-sperm/
