Cryptococcus spp
- Cryptococcus spp is a fungal group that belongs to the Phylum Basidiomycota (Basidiomycetes).
- They undergo sexual reproduction forming dikaryotic hyphae and basidiospores supported by a club-shaped basidium with hyphae that has a complex septate.
- There are four known species of Cryptococcus:
- Cryptococcus neorformans
- Cryptococcus gattii
- Cryptococcus albidus
- Cryptococcus laurentii
- Cryptococcus inuguttulatus
- C. albidus and C.laurentii are the most common species and C.neorformans is the most pathogenic of these species, for both humans and animals, while C. laurentii and C.gittii are mildly pathogenic.
- Cryptococcus neorformans distinguishes from other fungal yeasts by the presence of a polysaccharide capsule, the formation of melanin, and urease activity, which all function as virulence determinants.
- Its human pathogenicity is via inhalation of desiccated yeast cells or small basidiospores. The yeast then migrates to the central nervous system causing meningoencephalitis.
- This infection is otherwise known as cryptococcosis, which is a systemic infection primarily involving the lungs and central nervous system.
- Cryptococcus neoformans affect immunocompetent persons but more often in patients with HIV/AIDS, tuberculosis, hematogenous malignancies, and hospitalized patients majorly those with invasive devices.
Habitat of Cryptococcus neoformans
- Cryptococcus neoformans are commonly found in the environment growing as unicellular yeast and they reproduce by budding.
- In the natural environment, it exists as a saprophytic forming a large budding yeast morphology.
- It is an encapsulated yeast-like fungus that is isolated from dried avian (particularly pigeon) and bat excreta, and in dust contaminated with such droppings.
Morphology of Cryptococcus neoformans
- Cryptococcus neoformans is a yeast fungus, producing yeast cells during reproduction.
- The yeast cells are dry, mildly encapsulated, and light, making them easy to aerosolize.
- In culture, they produce whitish mucoid colonies which are spherically budding cells 5–10 μm in diameter and are surrounded by a thick nonstaining capsule.
Cultural characteristics of Cryptococcus neoformans
- In culture, they produce whitish mucoid colonies within 2-3 days.
- They have spherically budded yeast cells of 5–10 μm in diameter with a thick nonstaining capsule surrounding it.
- They lack hyphae.
- It has the ability to grow at 37°C, producing laccase, which is a phenol oxidase that catalyzes the formation of melanin from phenolic substrates such as catecholamine, which can be detected by biochemical characterization.
Life Cycle of Cryptococcus neoformans
- Cryptococcus neoformans is a facultative intracellular pathogen, which uses human phagocytes to spread within the body.
- The fungus has the ability to colonize phagocytic cells and undergoes vomocytosis, hence it escapes phagocytosis without processing.
- The yeast-like fungus gains entry into the human host via inhalation of aerosolized basidiospores.
- They then disseminate into the Central nervous system where it causes meningoencephalitis.
- When it gains entry into the lungs, they get phagocytosed by the alveolar macrophages. the macrophages produce oxidative and nitrosative agents which normally kill microorganisms but Cryptococcus neoformans have the ability to escape killing by Oxidative reaction, by upregulation of expressing genes of oxidative stress.
- They then remain latent in the macrophages which have been associated with disease dissemination and resistance to antifungal drugs.
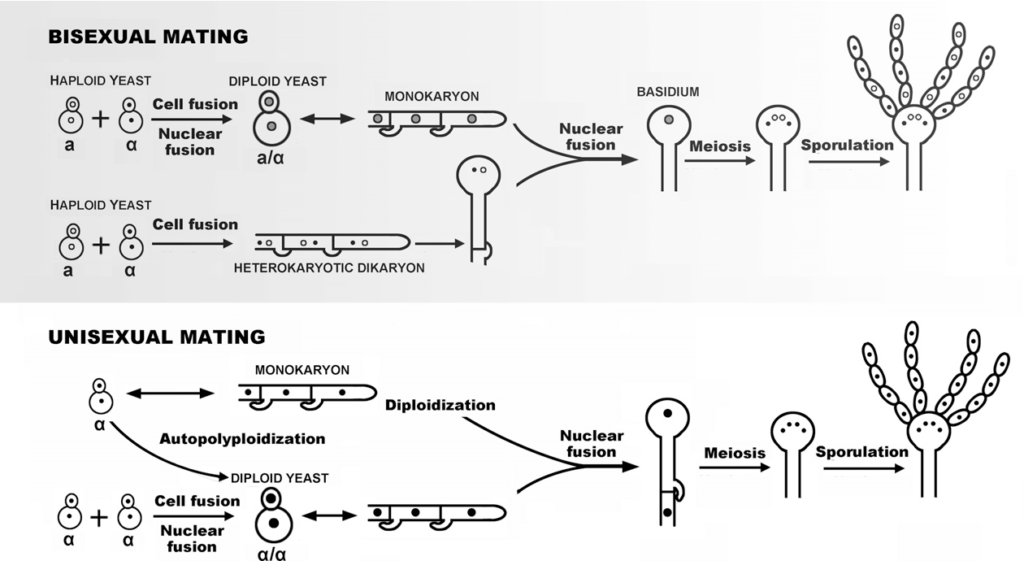
Figure: The life cycle of Cryptococcus neoformans. The upper panel depicts the traditional bisexual mating involving partners of opposite mating types a and α, and the lower panel depicts unisexual mating that occurs between partners of the same mating-type or with itself. Image Source: Elsevier Inc.
They can also undergo sexual reproduction of meiosis by the alpha types of the fungi.
- The filaments of the mating types alpha have a haploid nucleus, which undergoes diploidization forming diploid cells called blastospores. Blastospores have the ability to undergo meiosis to form haploid basidiospores that are easily dispersed. This mechanism is known as monokaryotic fruiting.
- During this process of meiotic reproduction, they can also promote DNA repair from damages of oxidative and nitrosative stress. This produces the monokaryotic fruit which contributes to the fungal virulence.
Pathogenesis and Clinical Features of Cryptococcus neoformans Infection
Virulence Factors
- Their virulence is enhanced by the production of laccase and capsule, and the presence of the capsular polysaccharide.
- The capsular polysaccharides are long, unbranched polymers consisting of an α-1,3-linked polymannose backbone with β-linked monomeric branches of xylose and glucuronic acid.
- On infection, the capsular polysaccharide solubilizes in spinal fluid, serum, or urine, increasing the yeast’s virulence of infection and disease spread.
Infection
- The infection of Cryptococcus neoformans is initiated by the inhalation of yeast cells, which are dry and lightweight making them easy to aerosolize.
- The fungus gains entry into the body through the respiratory tract system, causing a minimal pulmonary infection that is transitory.
- The primary pulmonary infection can be asymptomatic, mimicking influenza infection and it resolves spontaneously.
- For immunocompromised patients, the yeast replicates and spreads to other parts of the body and majorly to the Central Nervous system.
- Affecting about 15% of HIV/AIDS patients, it starts by causing mild infections of the pulmonary system, which spreads to the skin, bones, viscera, and the central nervous system.
- When the CNS is affected, it eventually causes cryptococcal meningitis.
- Other common sites of dissemination include the skin, adrenals, bone, eye, and prostate gland.
- There is a minimal inflammation-causing granulomatous reaction.
- Patients who get cryptococcal meningitis and are under Highly Active Antiretroviral Therapy (HAART) are likely to develop immune reconstitution inflammatory syndrome (IRIS), which greatly exacerbates the illness. This is also common in AIDS patients with Tuberculosis.
Clinical features of Cryptococcus neoformans infection
- C. neoformans causes a fungal infection commonly known as cryptococcosis.
- This is an infection that majorly affects persons with an immune-deficient system and majorly AIDS patients are associated with symptoms such as:
-
- Flu-like symptoms
- Chronic meningitis resembling brain tumor, brain abscess, degenerative central nervous system
- Mycobacterial mimicked disease
- Fungal meningitis
- Patients with meningitis symptoms have complications of severe headaches, neck stiffness, and disorientation
- They may also have lesions in skin, lungs, bone weakness with muscle dystrophy and inability to move.
- Untreated cases may end in fatality.
Laboratory Diagnosis of Cryptococcus neoformans
Specimen and specimen preparation
- Cerebrospinal fluid, tissue, exudates, sputum, blood, cutaneous scrapings, and urine.
- Spinal fluid is centrifuged before microscopic examination and culture.
Staining and Microscopic examination:
Gram staining
- The cells of Cryptococcus neoformans may appear round with Gram-positive granular inclusion on a pale lavender cytoplasmic background or as Gram-negative lipoid bodies.
Negative staining
- Using India Ink for visualizing the cerebral spinal fluid, indicating that particles of ink pigments can not enter the cell capsule surrounding the yeast cells. This forms a zone of clearance known as a halo, around the cells. This is a quick method for the identification of Cryptococcus neoformans.
Mucicarmine stain
- This stain is specific for the identification of polysaccharide cell walls of Cryptococcus neoformans in tissue samples.
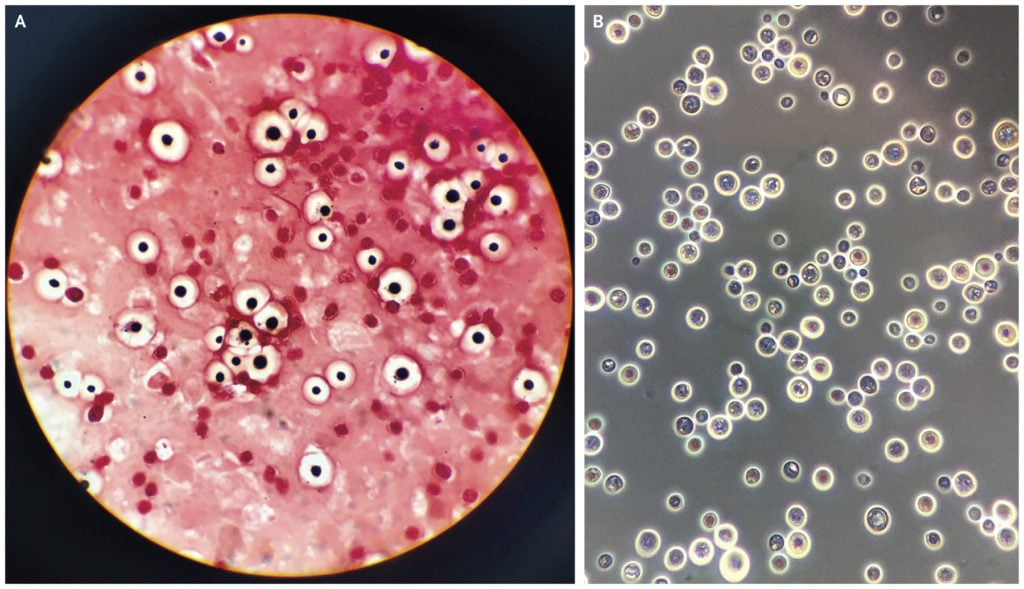
Figure: Gram’s stain (Panel A) and India ink stain (Panel B) revealed abundant encapsulated, round yeasts, with some budding forms. Image Source: Massachusetts Medical Society (NEJM).
Cultural examination
- Culture examination uses Sabouraud Dextrose Agar (SDA).
- The yeast develops colonies within a few days on most cultural media at room temperature or 37°C.
- Media with cycloheximide inhibit Cryptococcus and should be avoided.
- Detection of urease production in the culture media.
- Alternatively, on an appropriate diphenolic substrate, the phenoloxidase (or laccase) of C. neoformans produces melanin in the cell walls, and colonies develop a brown pigmentation.
Biochemical characterization
- Demonstrating the production of urease and laccase or a specific pattern of carbohydrate assimilations immediately after the cultural examination
Serological Examination
Antigen detection
- Detection of the capsular polysaccharide antigen of Cryptococcus is the idlest diagnostic test by using spinal fluid or serum or urine by the application of enzyme immunoassays or agglutination of latex particles coated with antibodies to the polysaccharide antigen.
- This test is sensitive and specific for antigen detection in cases of cryptococcal meningitis.
Antibody Quantification
- Antibodies produced against the polysaccharide capsule antigen can be quantified
Treatment of Cryptococcosis
- Infection that does not spread to the CNS can be treated with fluconazole.
- Cryptococcal meningitis is treated by combination therapy which is the standard treatment. Administration of intravenous administration of amphotericin B and oral fluconazole for two weeks. This is then followed with oral fluconazole for 10 weeks and a lower dose a year to improve the patients’ CD4 count.
- For patients who develop side effects to amphoterin B, intravenous ambisome can be used.
Prevention and Control
- Immunosuppressed people should avoid contact with birds and avoid digging and dusty activities in areas heavily contaminated with bird droppings.
- Avoiding areas with dried pigeon feces.
- Wearing masks may help to prevent the inhalation of Cryptococcus neoformans.
Reference
- Medical Microbiology by Jawertz, Melnick, and Adelberg, 26th Edition
- Microbiology by Prescott, 5the Edition
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4066639/
- https://www.cdc.gov/fungal/diseases/cryptococcosis-neoformans/index.html
- https://www.sciencedirect.com/topics/neuroscience/cryptococcus-neoformans
- https://www.frontiersin.org/articles/10.3389/fimmu.2018.00855/full
Sources
- 1% – https://www.researchgate.net/publication/232248316_Answer_to_November_2012_Photo_Quiz
- 1% – https://www.researchgate.net/publication/12460907_Cryptococcus_neoformans_Is_a_Facultative_Intracellular_Pathogen_in_Murine_Pulmonary_Infection
- 1% – https://www.ncbi.nlm.nih.gov/pubmed/24985132
- 1% – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4456224/
- 1% – https://www.cdc.gov/fungal/diseases/candidiasis/invasive/index.html
- 1% – https://onlinelibrary.wiley.com/doi/epdf/10.1111/jvim.15599
- 1% – https://jcm.asm.org/content/43/9/4766
- 1% – https://emedicine.medscape.com/article/1952165-overview
- 1% – https://academic.oup.com/mmy/article-abstract/48/1/90/1250507
- <1% – https://www.sciencedirect.com/topics/medicine-and-dentistry/nigrosin
- <1% – https://www.medicinenet.com/cryptococcosis/article.htm
- <1% – https://quizlet.com/136175210/microbiology-pathology-flash-cards/
- <1% – https://aidsinfo.nih.gov/drugs/6/amphotericin-b/117/professional

very good
I always to your websites, very informative and useful. Thank you so much! I am from Mycology Lab in Ministry of Health, Malaysia. We have many collection of clinical important fungi. I hope I can do similar with your web and help others.