Coccidioidomycosis is a systemic infection caused by inhalation of Coccidioides immitis or Coccidioides posadasii spores.
- It affects both humans and animals.
- It is also known as Valley fever or cocci or California fever, or desert rheumatism, or San Joaquin Valley fever.
- The spores of the causative agents are commonly found in soil in endemic areas, where they get distributed into the air.
- It commonly occurs in gardening areas, construction, farming, wind areas.
- Endemic areas affected are the arid areas of the United States in Arizona, California, Nevada, New Mexico, Texas, Utah, and Northern Mexico.
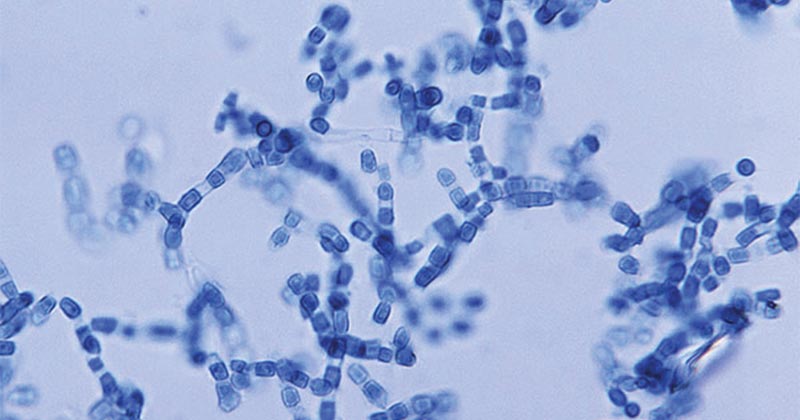
Causative agents of coccidioidomycosis
- Coccidioidomycosis is caused by dimorphic fungi of the Coccidioides.
- Coccidioides are a genus of dimorphic fungi existing as mycelia or as spherules of asexual forms and they lack the sexual form of reproduction and structures.
- The two species within the genus coccidioides are C. immitis and Coccidioides posadasii.
- They are known to cause Coccidioidomycosis in different regions in the endemic areas.
- The two species of coccidioides are phenotypically identical and can only be identified and differentiated by molecular methods and not clinically.
- The coccidioides produce infective spores known as arthroconidia. The arthroconidia get deposited into the lungs during inhalation. They then germinate and grow into spherules within the lungs and tissues.
- Spherules are filled with tiny endospores of about 2um-5um, which burst into the tissues releasing the endospores which cause severe disease.
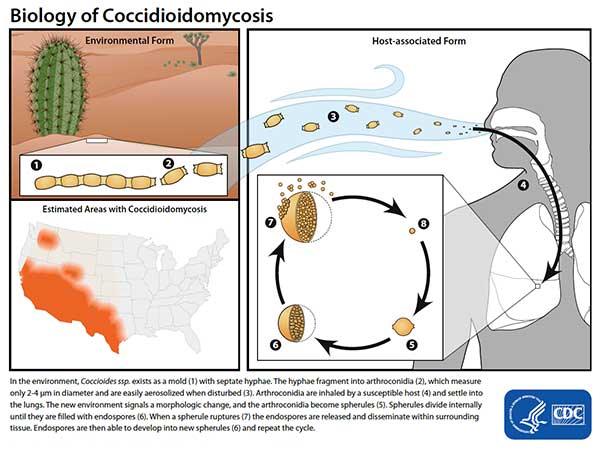
Pathogenesis of Coccidioidomycosis
Risk factors of Coccidioidomycosis infection
- People that are living or traveling into endemic areas where the Coccidioides fungus occurs are at risk of infection.
- Dust storms carrying the fungal spores of contaminated soil such as farms or construction sites increases the risks of exposure and infection.
- People who have compromised immune systems are at increased risk of developing the severe or disseminated disease. These include:
- HIV/AIDS patients
- Autoimmune patients and rheumatoid disease patients taking immune-suppressing drugs
- Organ transplant recipients
- Diabetic patients
- Pregnant women
Virulence factors of the causative agents
- Adherence
- During mycelial growth and formation of the septae, processes of autolysis and thinning of the spores leaves some cells which are barred-shaped that have the ability to adhere to epithelial cells and tissues.
- The lightweight and loosely chained arthroconidia allow them to easily become airborne and attach to surfaces and be inhaled by hosts.
- Specialization and remodeling
- The arthroconidia undergo remodeling when in the host cells shedding off the outer layer of the spore, to form the spherules.
- The spherules which divide internally through the formation of an internal septae divide the spherules into compartments and each compartment contains several small endospores.
- A fully impregnated spherule with endospores raptures and releases the endospores into the epithelial cells, alveolar sacs, and alveolar macrophages.
- The alveolar macrophages pick the endospores which cause an acute inflammatory response due to the accumulation of neutrophils and eosinophils, as a host response to the endospores. The endospores can further multiply within the cells and tissues and spread by causing mycelial growth in the tissues.
- Antigenic Variation
- The coccidiodes produce two antigens known as coccidiodin and spherulin. Coccidiodin is extracted from mycelial cultures of the coccidiodes and spherulin antigen are produced from broth cultures.
- They contribute to the immune responses of the fungi.
Clinical features of coccidioidomycosis
- Clinically, over 60% of the infections are asymptomatic; with most of them resembling bacterial pneumonia infections.
- Symptoms appear at least 21 days after infection with symptoms of fever, cough, shortness of breath, and chest pains. Headaches, weight loss, and rashes are common with the rashes appearing faintly, maculopapular, transient and the commonly occur during early infection.
- A headache, weight loss, and rash are often seen. The rash is faint, maculopapular, transient, and occurs early during disease, but not often to detected.
- In women reddish, painful, tender lumps known as erythema nodosum or erythema multiforme occur on the legs just below the knees. most commonly located in the front of the legs below the knees, associated with migratory arthralgias, a form of pain the spreads from the joints to other parts of the body. These symptoms are collectively known as desert rheumatism
- Lung cavities are common in children but less common in adults. This is a pulmonary infection of nodules and cavities often in the early stage of infection
- Cavities are solitary, and peripheral with a thin wall, often solitary, and with time develop a distinctive thin wall.
Some of the major clinical manifestations of coccidioidomycosis include:
- Acute and chronic inflammation which is associated with the production of neutrophils and eosinophils in response to endospore exposure in the alveolar sacs and the lung tissues. Neutrophils and eosinophils get attracted to the site where the spherules rupture and release endospores.
- Chronic granulomatous infection occurs when mature spherules do not rupture, which is an indication of Coccidiodes’ control.
- progressive Pulmonary coccidioidomycosis which is normally chronic with multiplication and enlargement of nodules or/and cavities.
- Disseminated coccidioidomycosis which is debilitating and life-threatening; commonly affecting men than women except for pregnant women. Men most affected are those the elderly, those with underlying conditions, HIV/AIDS patients. Majorly caused by C. immitis which has estrogen-binding proteins, and elevated levels of estradiol and progesterone stimulate its growth.
- Coccidioides Meningitis which is a disseminated infection commonly affecting the Central Nervous system and brain of AIDS patients.
Diagnosis of Coccidioidomycosis
Clinical diagnosis of Coccidioidomycosis
- Physical examination and history of patients, through Chest X-rays which shows unilateral infiltration, lobar consolidation, nodular infiltrate, cavitation, and hilar and peritracheal adenopathy or mediastinal lymphadenopathy, for extrathoracic.
Laboratory Diagnosis of Coccidioidomycosis
Specimen: Sputum, pleural fluid, Cerebrospinal fluid, lesion exudates, biopsy
Microscopic examination
- Use of KOH Wet mount and calcofluor stains are used for observation of spherules which is usually 20 to 80 micrometers in diameter, thick-walled, and small endospores of 2 to 4 um for C. immitis.
Cultural Examination
- Culturing Coccidioides in mycological and/or bacterial media produces white to tan cottony colonies within 5-7 days.
- On Sabouraud’s agar, the colonies have hyphae with chains of arthroconidia which independently form hyphal cells.
- Bacterial media can be prepared with or without antibacterial antibiotics and cycloheximide to inhibit contaminating bacteria
or saprophytic molds, respectively. Because the arthroconidia are highly infectious, suspicious cultures are examined only
in a biosafety cabinet - A complex medium can be used to cultivate and produce spherules of these fungi.
Histological diagnosis
- Use sputum or tissue samples to diagnose for spherules of the fungi which are thick with a double refractile wall with a diameter of 80 μm.
Serological Testing
- Complete blood count and differentiation to show eosinophilia or inflammatory markers such as erythrocyte sedimentation rate (ESR) or CRPE.
- Testing for anti-coccidiodidal antibodies, IgG and IgM for confirmation
- Enzyme immunoassays for detection of antibodies against the disease or presence of coccidiododial antigens
- Immunodiffusion for detection of IgM and IgG antibodies against coccidioidomycosis
- Complement Fixation Testing for IgG for estimation of disease severity, with high titers indication severe disease and low titters, indication less severe disease or decline in severity. Complement Fixation also detects the presence of complement-fixing antibodies in the CSF which is an important diagnosis for coccidial meningitis.
- Urine Antigen Test is used in immunocompromised. patients with severe forms of the disease inclusive of pneumonia and disseminated disease.
- Delayed cutaneous hypersensitivity, is used for epidemiological studies in endemic areas, majorly to detect hypersensitivity to coccidioidin or spherulin that develops within 10 to 21 days after acute infections in immunocompetent patients. However, the spherulin is absent in progressive disease.
Skin Test
- The coccidiosis skin test reaches maximum induration (≥5 mm in diameter) between 24 and 48 hours after cutaneous
injection of 0.1 mL of a standardized dilution.
Molecular Diagnosis
- cDNA probing rapidly identifies fungal growth.
- Polymerase Chain Reaction (PCR) is used to test for fungal DNA from samples from the lower respiratory tract.
Treatment of Coccidioidomycosis
- Mild to moderate disease can be treated with fluconazole or itraconazole
- Severe disease is treated with Amphotericin B
- In Low endemic areas where the risks are low and less hematogenous seeding of the fungi, patients are treated with fluconazole which is less toxic
- Mild to moderate nonmeningeal extrapulmonary infections are treated with fluconazole or itraconazole is taken orally. Voriconazole can be administered orally or intravenously or treat with oral posaconazole.
- HIV/AIDS patients with coccidioidomycosis associated infections use maintained therapy of fluconazole or itraconazole while monitoring the CD4 cell count at about > 250/mcL.
- Meningeal coccidioidomycosis is treated with longterm administration of oral fluconazole.
- Surgical removal of involved bone to cure osteomyelitis
- Surgical removal of a lung or pulmonary cavities that cause hemoptysis may be necessary when the disease is diagnosed early to resection the cavity and close pulmonary leaks.
Prevention and Control of Coccidioidomycosis
- Close monitoring of risk groups from contracting opportunistic coccidioidomycosis
- Some measure of control can be achieved by reducing dust, paving roads and airfields, planting grass or crops, and using oil sprays.
References
- Medical Microbiology by Jawertz 25th Edition.
- https://www.msdmanuals.com/professional/infectious-diseases/fungi/coccidioidomycosis
- https://www.ncbi.nlm.nih.gov/books/NBK448161/
- https://my.clevelandclinic.org/health/diseases/17754-valley-fever-coccidioidomycosis
- https://dermnetnz.org/topics/coccidioidomycosis/
- https://www.scielo.br/scielo.php?pid=s1806-37132009000900014&script=sci_arttext&tlng=en
- https://www.bcmj.org/articles/textbook-case-coccidioidomycosis
- https://www.atsjournals.org/doi/full/10.1513/AnnalsATS.201308-286FR
