Mycoses (S., Mycosis, Greek mykes: Fungus) is a term used to describe the infection caused by fungi. More than 200,000 species of fungi have been scientifically documented, out of which only about 100-150 have been responsible for causing human disease, and 25 of the species are concurrently responsible to cause the most infections.
The field that specializes in the study of these disease-causing fungi is called medical mycology. It studies the epidemiology, characteristics of infection by particular species of fungi and identification by means of laboratory investigations that include histology, direct microscopy, culture and PCR.
Epidemiology of Mycoses
The major factor for mycoses is alteration of the host’s immune system by means of underlying disease or use of immunosuppressive agents. These alterations, when lead to an individual being immunocompromised trigger exogenous infections (by inhalation, ingestion or accidental physical injury or unintentional trauma during surgery) and endogenous infection (caused by the normal flora which becomes opportunistic pathogens).
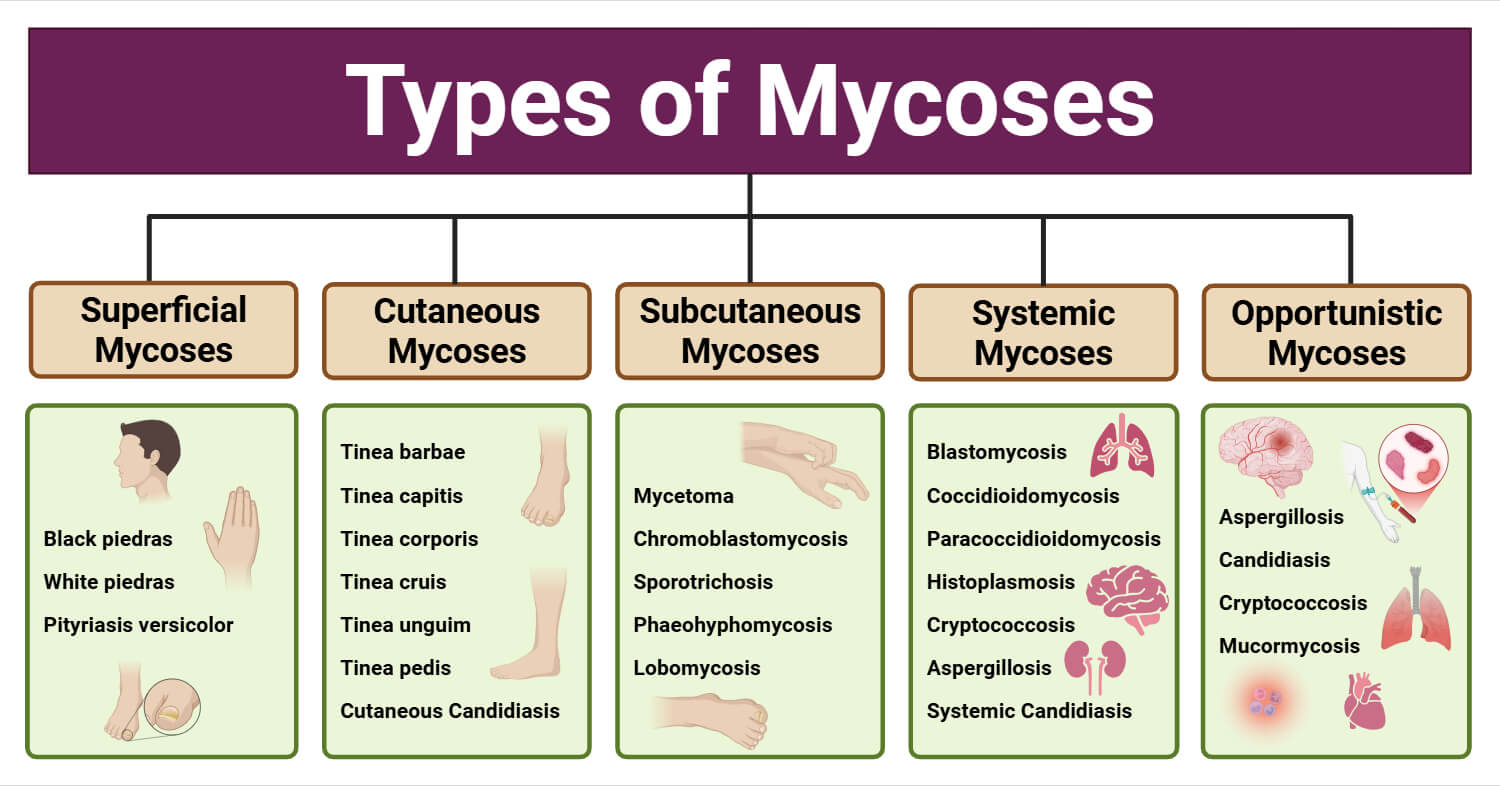
Types of Mycoses
- Superficial mycoses
- Cutaneous mycoses
- Subcutaneous mycoses
- Systemic mycoses
- Opportunistic mycoses
1. Superficial Mycoses
- The type of mycoses that infects the hair, nails and skin (stratum corneum) without disseminating into deeper tissues, hence being limited to the outer surface only.
- The infection of the hair shaft is called piedras. They are of two types: Black piedras is caused by Piedraia hortae, which forms black nodules on hair scalp, and White piedras, caused by Trichosporon beigelii, on the beard and mustache.
- The yeast Malassezia furfur causes skin infection i.e., pityriasis versicolor. Commensals like Candida (esp. C. albicans) cause yeast infection in the nails and the mucous membrane of the vagina and the mouth.
2. Cutaneous Mycoses
- This mycosis is primarily caused by dermatophytes that are mould fungi, also referred to as ringworm or Tinea, responsible for dermatomycoses. Dermatophytes break down and utilize keratin (a structural protein of skin, nail and hair) as a source of nitrogen. The predominate genera of dermatophytes include: Trichophyton, Epidermophyton and Microsporum.
- “Tinea barbae” refers to infection of beard hair caused by Trichophyton mentagrophytes.
- “Tinea capitis” is an infection of scalp hair caused by Trichophyton and Microsporum spp. It is characterized by loss of hair and scaling. In some cases, the dermatophytes lead to inflammation and suppurating lesions.
- “Tinea corporis” refers to infection of the skin i.e., characterized by itchy, red-circular, vesiculopustular lesions. It is mainly caused by Trichophyton rubrum or Microsporum canis.
- “Tinea cruis” is the infection of the groin caused by Trichophyton rubrum, Epidermophyton floccosum or Trichophyton mentagrophytes.
- “Tinea unguim” is the infection of the nail characterized by a thickened, discolored, crumbly appearance. Trichophyton rubrum or Trichophyton mentagrophytes are etiological agents.
- “Tinea pedis” or athlete’s foot, causative agent being T. rubrum and E. floccosum, is characterized by itchy vesiculopustular to scaly appearance.
3. Subcutaneous Mycoses
- In such mycoses, the subcutaneous tissues and the adjacent bones get infected via puncture, abrasion or cuts that introduce saprophytic fungus (present in soil, thorns or wood splinters) into the body.
- The disease develops slowly, and during this duration, they form subcutaneous nodules that ulcerate and spread via the lymph system, creating more nodules.
- The three main subcutaneous mycoses are: Mycetoma, Chromoblastomycosis and Sporotrichosis.
- Mycetoma: It causes chronic granulomatous infection characterized by tumor-like swelling of subcutaneous tissue, mainly the legs (due to walking barefoot). When not treated on time, the infection progresses to the fascia and bones, debilitating it, which then necessitate for an amputation.
- Mycetoma is caused by both fungi and bacteria. Actinomycotic (bacterial) mycetoma etiological agents are Nocardia, Streptomyces and Actinomadura spp.
- Eumycotic (fungal) mycetoma is characterized into two subcategories: White grain mycetomas caused by hyaline septate fungi like Pseudallescheria boydii, Acremonium and Fusarium spp.
- Black grain mycetomas caused by dematiaceous fungi like Madurella mycetomatis (maduromycosis), Exophiala jeanselmei and Curvularia spp.
- Chromoblastomycosis (Chromomycosis): The causative agents of this disease are: Cladophialophora carrionii, Phialophora verrucosa, Fonsecaea pedrosoi and F. compacta. The disease is characterized by a papule at the site of infection, which then slowly progresses into verrucous lesions (cauliflower-like warts).
- Sporotrichosis: The etiological agent of this disease is the dimorphic fungus Sporothrix schenckii. This dimorphic fungus is found in soil, in barberry shrubs and roses, sphagnum mosses and pine-bark mulch. Gardeners, florists are mainly susceptible to this disease.
- The disease is characterized by red papules (after 1-12 weeks of incubation) that begin to form sores. The primary lesions may remain localized, but in immunocompromised individuals, can disseminate into other part causing “extracutaneous sporotrichosis”, which can involve lungs, blood, lymph, bones and brain.
4. Systemic Mycoses
The infection occurs from inhalation of air-borne spores by the lungs, but unlike the aforementioned mycoses, this fungal infection gets disseminated into any other organ system and causes disease.
The etiological pathogens are divided into 2 types: i) True pathogens, ii) Opportunistic pathogens
a. True pathogens
These are dimorphic fungi that can infect immunocompromised as well as healthy hosts. These are: Blastomyces dermatitidis (causes blastomycosis), Coccidioides immitis (causes coccidioidomycosis), Paracoccidioides brasiliensis (causes paracoccidioidomycosis) and Histoplasma capsulatum (causes histoplasmosis). These dimorphic fungi exist as mould in the environment and as a yeast (except for C. immitis, because they form a spherule, which is not a true yeast) inside the body, which is their invasive/tissue form.
b. Opportunistic pathogens
These are fungi (yeast and moulds) that only infects mostly the immunocompromised patient. These are: Cryptococcus neoformans and C. gatti (causes Cryptococcosis), Aspergillus spp. (Causes Aspergillosis) and Candida spp. (Causes Candidiasis).
- Blastomycosis: Initially, it causes acute pulmonary blastomycosis, which can progress into chronic pulmonary disease depending upon the immune system of an individual. Disseminated infection may likely occur, the common site being skin characterized by suppurative and granulomatous infection with a demarcated edge. Chances of osteomyelitis, arthritis and meningitis (in rare cases) are possible.
- Coccidioidomycosis: The infection starts after inhaling the arthroconidia. Generally, coccidioidomycosis is asymptomatic or presents as an ordinary pulmonary infection. In a few cases, infection progresses into chronic pulmonary illness and disseminates. The disseminated cases are mostly observed in Asian and Black ethnicities and pregnant women.
- Paracoccidioidomycosis: It initiates as a primary pulmonary infection which is mostly asymptomatic. The progressive state of infection causes a chronic granuloma. In children and adolescents, disseminated forms lead to superficial or visceral lymph node enlargement. In adults, it disseminates to form lesions of the mucous membrane, commonly of the nasal and oral mucosa.
- Histoplasmosis: The primary infection begins in the lungs after inhaling the aerosolized microconidia. Most of the cases (about 95%) are asymptomatic and subside in an immunocompetent individual. But higher levels of exposure result in fever, cough and joint pain.
- Dissemination of histoplasmosis occurs via the reticuloendothelial system and the primary sites are mainly the liver, spleen and lymph nodes. In an immunocompromised individual, the chances of hepatic infection, adrenal deterioration are very likely. Regardless of a patient’s status being immunocompromised or immunocompetent, the infection causes ulcerative lesions in the lungs very reminiscent of tuberculosis.
- Cryptococcosis: C. neoformans infects the body via the respiratory tract and eventually causes transient pulmonary infection. Disseminated pulmonary infection may spread into the bones, skin and brain. When the disseminated site is the brain, cryptococcal meningitis occurs, its symptoms become very evident in an AIDS patient.
- C. gatti, on the other hand causes infection even in an immunocompetent host. It reduces the inflammatory response of the host’s immune system and completely overtakes it.
- Both C. neoformans and C. gatti are encapsulated yeasts, an attribute that ensures their survival in the gut of pigeons and also increases their pathogenicity.
5. Opportunistic Mycoses
The fungi exist as saprophytic fungi in the environment or as normal microbiota in the body. When a host has a debilitated immune system resulting from undergoing transplantation that requires treatment by immunosuppressive agents or has an underlying disease or through perpetuate use of antibiotics, they become defenseless against infection.
The two main frequent etiological agents of this type of mycoses are: Aspergillus spp. (causes Aspergillosis) and Candida spp (Candidiasis).
a. Aspergillosis
More than 200 species of Aspergillus are scientifically recorded, but at least 20 of them have been accountable with aspergillosis. The predominant species are: A. fumigatus, A. niger, A. flavus and A. nidulans.
The key entry portal inside the body is the respiratory system that can inhale the conidiophores. Both atopic and non-atopic individuals can suffer from allergic symptoms.
The subsequent infection after the exposure has been subcategorized into different types of aspergillosis based on clinical features: i. Invasive aspergillosis, ii. Aspergilloma, iii. Sinusitis, iv. Allergic bronchopulmonary aspergillosis.
i. Invasive aspergillosis
The main etiological agent is A. fumigatus. In an immunocompromised patient, the lungs are subjugated by the exponential growth of Aspergillus, including blood vessels, leading to septic emboli. Although fungemia is rare, neutropenic patients are susceptible to it.
ii. Aspergilloma
It is also called “fungus ball”, which colonizes the cavities in the lung and produces a thick ball of mycelium. Patients with aspergilloma are asymptomatic or produce sputum that can sometimes take the form of hemoptysis. The main etiological agent is A. fumigatus.
iii. Sinusitis
The main etiological agents are the A. flavus and A. fumigatus that infect the paranasal sinuses.
iv. Allergic bronchopulmonary aspergillosis
The main etiological agent is A. fumigatus, and is mostly observed in atopic patients. The fungus proliferates in the airways to produce mucus plugs.
External otomycosis, mycotic keratitis and onchomycosis are some other infection caused by Aspergillus spp.
b. Candidiasis
C. glabrata and C. albicans are the two main etiological agents of Candidiasis. Other species that have come to prominence are: C. tropicalis (especially in neutropenic patients), C. parapsilosis (nosocomial infection in neonatal intensive care unit) and C. krusei.
Based on the site of infection, the candidiasis is divided into: i) Superficial candidiasis, ii) Invasive candidiasis.
Superficial candidiasis
It infects nails, skin and mucous membrane of vagina and mouth (part of normal microbiota). In oropharyngeal candidiasis (also called oral thrush), white flecks form on the tongue and palate. In vaginal candidiasis, yellow-white curd-like discharge and white sores form on the vulva occurs accompanied by itching. Cutaneous candidiasis is a less common occurrence compared to dermatophytosis, but when present infects the moist sites like the groin.
Invasive candidiasis
This is a systemic infection that can either be confined to one organ or disseminated via blood (candidaemia) into deep organs or tissue, resulting in a wide spectrum of infections like meningitis, osteomyelitis and endocarditis. The primary sign of this candidiasis is Candida endophthalmitis very evident in neutropenic patients. Candida endophthalmitis forms white lesions in the eye leading to eye pain and poor vision.
References
- Denyer, S.P., Hodges, N.A. & Gorman, S.P. (2004). Hugo and Russell’s Pharmaceutical Microbiology (7th edition, pp. 47). Blackwell Science Willey, J.M., Sherwood, L.M. & Woolverton, C.J. (2008). Prescott, Harley and Klein’s microbiology (7th edition). McGraw-Hill.
- Greenwood, D., Barer, M., Slack, R. & Irving, W. (2012). Medical microbiology (18th edition). Churchill Livingstone Elsevier.
- Pelczar, M.J., Jr., Chan, E.C.S. & Krieg, N.R. (1993) Microbiology (5th edition, pp. 676-685). Tata McGraw Hill Education Private Limited.
- Tille, P.M. (2014). Bailey & Scott’s Diagnostic Microbiology (13th edition, pp. 705-757). Elsevier Mosby.
- Willey, J.M., Sherwood, L.M. & Woolverton, C.J. (2008). Prescott, Harley and Klein’s microbiology (7th edition, pp. 997-1018). McGraw-Hill.
