Microsporum spp are dermatophyte fungi that cause cutaneous infections of the nails, hair, and skin, known as dermatophytosis.
- They are ascomycetous molds producing macroconidial spores which are distinct for these group of dermatophyte, distinguishing them from other dermatophytes such as Trichophyton and Epidermophyton.
- Microsporum spp are keratolytic i.e they synthesis keratinase enzyme which digests fragments of the skin, hair, and nails causing cutaneous diseases.
- As a dermatophyte, it is restricted to the nonviable skin tissues because of its inability to grow in temperatures above 37°C.
- It is a highly transmissible fungus from animals to humans therefore it is a zoonotic fungus.
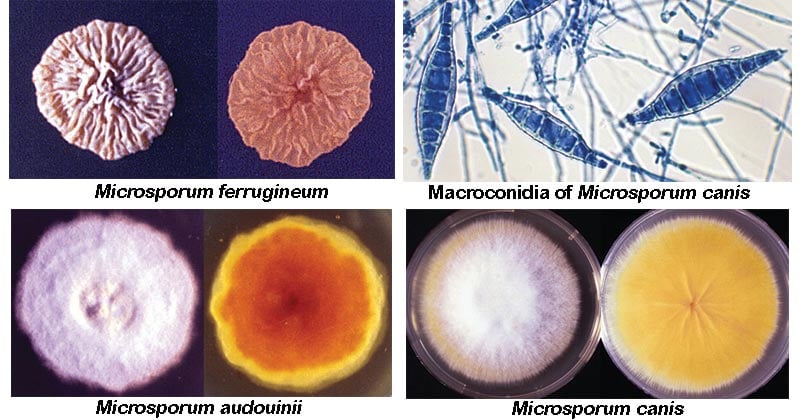
Image Source: The University of Adelaide.
Habitat of Microsporum spp
- They occur worldwide; naturally living in the soil.
- They thrive at room temperature of 25-27˚C, on keratin surfaces where temperatures are low.
- They are keratotic hence they live in areas with high keratin content such as akin, hair, and nails.
Morphological Characteristics of Microsporum spp
- Microsporum reproduces asexually forming Macroconidia and microconidia.
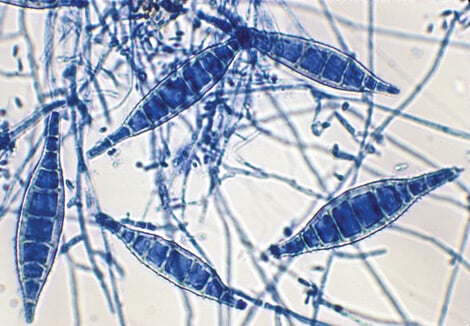
- Macroconidia are large asexual spores. They are hyaline, multiseptate with variants in its forms, spindle-like shape to obovate.
- The macroconidia are 7–20 μm by 30–160 μm in size, with a thin or thick echinulate to the verrucose cell wall.
- Because of they highly distinguished structure of the Macroconidia which is thick and rough, these fungi can be differentiated from other dermatophytes using these features,
- The microconidia are smaller than the macroconidia, and they are also asexual spores of Microsporum.
- Microconidia are hyaline and single-celled.
- Microconidia are pyriform to clavate shaped, having a smooth cell wall.
- The microconidia are 2.5–3.5 μm by 4–7 μm in size.
Figure: Macroconidia of Microsporum canis are typically spindle-shaped with 5-15 cells, verrucose, thick-walled, and often have a terminal knob. A few pyriform to clavate microconidia are also present. Image Source: The University of Adelaide.
Cultural Characterization of Microsporum spp
- They grow efficiently on Sabouraud dextrose agar, at 25˚C. Microsporum spp. producing a perfect form i.e a form of the fungus that accomplishes meiosis.
- They produce good growth in rice grain medium with pigmented peripheries.
- Trichophyton agar is the basic media used for the growth and identification of Microsporum species.
Selected Species of Microsporum
Microsporum audouinii
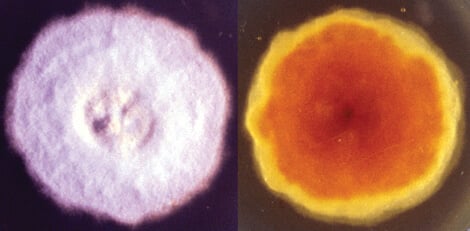
Figure: Culture of Microsporum audouinii. Image Source: The University of Adelaide.
- They are anthropophilic fungus.
- they cause non-inflammatory infections of the scalp and the skin in children.
- It is a major cause of tinea capitis, invading the hair shafts with an ectothrix infection on the site of the invasion,
- The ectothrix fluoresces a bright-yellow under Wood’s ultra-violet light.
- On basic media, they form spread flat colonies that are whitish-grey to tanned white in color.
- They have a furry texture.
- They form Macroconidia and rarely do they form microconidia.
- The macroconidia are long and smooth with irregular spindle shape
- If microconidia are formed, they are pyriform to clavate shaped
- They also form hyphal forms of pectinate (comb-like) and racquet hyphae (segmented series of hyphae with swollen tips)
Microsporum canis
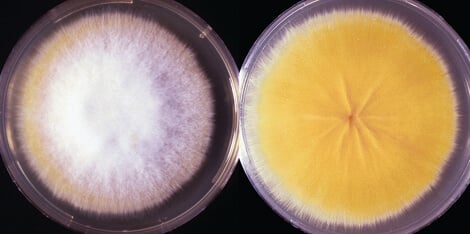
Figure: Culture of Microsporum canis. Image Source: The University of Adelaide.
- This is a zoophilic dermatophyte that is transmitted from dogs and cats to humans and it is distributed worldwide.
- It is a common cause of ringworms, especially in children.
- It invades the hair and skin showing an ectothrix infection which can be detected with the Wood’s ultra-violet light, fluorescing as bright greenish-yellow light.
- They produce good growth in rice grain agar with white aerial mycelium with the production of yellow pigment.
- In basic media, they form spread flat colonies that are white to cream-colored, with a cottony surface.
- The colonies also have an edged pigmented surface which is brownish-yellow.
- They produce macroconidia which are spindle-shaped with 5-15 cells, with a verrucose thock wall and a terminal end.
- They may also produce microconidia which are fewer in number, and they are pyriform to clavate.
- There are other strains of Microsporum canis dysgonic strains such as Microsporum canis var. distortum which commonly causes infection in cats and dogs and Microsporum canis var. equinum which causes ringworms in horses.
Microsporum ferrugineum
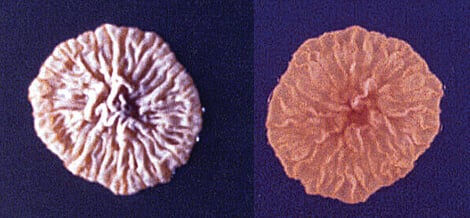
Figure: Culture of Microsporum ferrugineum. Image Source: The University of Adelaide.
- It is an anthropophilic fungus that causes epidemic juvenile tinea capitis in humans
- Its infection is similar to the infection caused by Microsporum audouinii.
- It invades the hair shafts causing an ectothrix infection that can be detected by the Wood’s ultra-violet light appearing or fluorescing as greenish-yellow.
- It is common in Asia, Russia, Africa, and Eastern Europe.
- In basic mycological media (SDA, PDA), colonies are slow-forming which have a waxy glabrous, convoluted thallus with a creamy to buff-colored surface.
- They have surface pigmentation from yellow to creamy to deep red.
- The colonies are downy and pleomorphic.
- They also show irregular branching hyphae with a bamboo hyphal appearance that carries chlamydospores.
- The bamboo-branched hyphae is a specific and distinct characteristic of Microsporum ferrugineum.
Microsporum fulvum
- This is the most common cause of ringworms (tinea corporis) and Atheletes’foot (Tinea pedis)
- It is commonly found in soil and it thrives in keratinized materials such as hair, nails, and skin.
- It is classified as an opportunistic fungal agent that causes cutaneous mycoses in humans and animals.
- They grow within 4-5 days forming floccose, wooly colonies in basic mycological media.
- The colonies produce clustered cells which have a granular appearance with a sandy-brown tinge and white edges.
- They are perfect fungi, reproducing both asexually and sexually.
- Sexual reproduction produces ascospores while asexual reproduction produces macroconidia and microconidia.
- The ascospores are 5-7 microns large with up to 8 spores
- The asexual macroconidia are largely occurring in clusters of 8 microns in diameter with branched hyphae.
- Macroconidia are fusoid-shaped with tapered ends and the are thin-walled.
- Microconidia are drop-shaped which sparsely populated irregular hyphae; which may appear as horsehair, fruity-bodies called cleistothecia forms.
Other species of Microsporum include:
Microsporum amazonicum, Microsporum boullardii, Microsporum cookei, Microsporum distortum, Microsporum duboisii, Microsporum ferrugineum, Microsporum fulvum.
Pathogenesis of Microsporum spp
- The virulence of Microsporum spp is attributed to their ability to colonized keratin containing materials such as skin, hair, and nails, hence it is a fungal keratinase.
- The fungi produce keratinase enzyme which degrades and breaks down keratin materials.
- The immune response elicited by the host in an inflammatory response that is localized, since the defense mechanisms of the body do not allow the fungi to invade the circulatory system.
- If the fungi colonize the mucous membrane, the fungi release the elastase enzyme which triggers severe immune responses.
- Microsporum causes several cutaneous infections on hair, skin, and nails, along with other dermatophytes.
- Due to this, the fungi are known to be a causative agent of several cutaneous infections (dermatophytosis) including:
- Tinea capitis
- Tinea corporis
Tinea capitis
- This is a fungal infection of the scalp hairs that is also known as ringworms and herpes tonsurans infection.
- It is also caused by Epidermophyton and Trichophyton spp.
- The fungi penetrate the hair follicles’ outer root sheath, invading the hair shafts.
- It can result in an inflammatory type of infection of non-inflammatory infection.
- Inflammatory type of tinea capitis is characterized by painful nodules that contain pus and scarring alopecia whereby the affected area loses hair while leaving a scar.
- It may also affect the eyelashes and eyebrows.
- It is common in children 3-14 years but it can affect any age group, and especially in immunocompromised individuals such as diabetics, cancer.
- Specific for Microsporum spp, Tinea capitis is in the principle of ectothrix, where the fungi affect the outer sheath root.
- It is characterized by:
- Subacute and chronic dermatitis either with or without follicular inflammation and destruction. Suppurative folliculitis may be present.
- Hyperkeratosis
- Parakeratosis
- Spongiosis
- A perivascular inflammatory infiltrate
- Clinical manifestations are:
- Black dot tinea capitis, that infects the hair.
- Kerion involves inflammation progressing to scarring alopecia.
- Favus is a boggy inflammation presented with deep-seated oozing nodules, abscesses, crusting, or scutula.
Tinea corporis
- Also known as ringworms;
- It is a pink-reddish round-shaped patch with plaques and a raised scaly border that expands on its periphery and clears at the center.
- The periphery has raised small papules that have pus.
- It affects the arms and legs, characterized by itching, scaling, redness, rashes, and maybe dry and flaky.
Laboratory Diagnosis of Microsporum spp
Specimens: Skin scrapings, nail scrapings, hair scraping, pus, tissue biopsies.
Differential diagnosis
The lesions formed by Microsporum spp can be distinguished from other microbial lesions such as bacterial abscess, psoriasis, eczema, syphilis, lupus erythematosus.
Direct Examination
KOH Wet mount using the skin scrapings and pus.
Cultural examination
- Microsporum audouinii produce pinkish-brown or salmon-colored fluffy colonies
- Microsporum canis produces bright yellow colonies.
Trichophyton Agar
- Microsporum audouinii produces flat, white, suede-like to downy, with yellow-brown reverse colonies with a furry texture
- Microsporum canis forms flat, white, suede-like to downy, with a yellow to pale yellow-brown reverse colonies.
Rice Grain Agar
- Microsporum canis produces white aerial mycelium with the production of yellow pigment
Histological Identification
- The periodic acid-Schiff stain is a special stain that will help in identifying Dermatophytic fungi.
Treatment and management of Microsporum spp infections
- Topical or Oral antifungals including imidazole, ciclopirox, naftifine, or terbinafine in cream, lotion, or gel, for mild-moderate lesions arising due to tinea corporis and tinea capitis.
- Extensive infections can be treated with oral itraconazole for a prolonged period of time.
- Use of antifungal shampoos for treatment and also for the prevention of fungal infection spread.
- Anti-fungal creams can also prevent tinea capitis and tinea corporis.
Prevention and control of Microsporum spp
- Hygienic handwashing after handling and exposure to animals, soil, and plants.
- Avoiding touching lesions on the skin and scalp of infected people
- Wearing loose-fitting clothing on the affected areas.
- Practicing good hygiene when engaging in activities that involve close human contact with skin.
References
- Medical Microbiology by Jawerts, 23rd Edition
- Microbiology by Prescott, 5th Edition
- https://mycology.adelaide.edu.au/descriptions/dermatophytes/microsporum/
- https://www.scielo.br/scielo.php?script=sci_arttext&pid=S1413-86702014000200181
- https://en.wikipedia.org/wiki/Microsporum_fulvum
- https://en.wikipedia.org/wiki/Microsporum
- https://www.msdsonline.com/resources/sds-resources/free-safety-data-sheet-index/epidermophyton-floccosum/
- https://www.ncbi.nlm.nih.gov/books/NBK536909/
Sources
- 3% – https://mycology.adelaide.edu.au/descriptions/dermatophytes/microsporum/
- 2% – https://www.ncbi.nlm.nih.gov/books/NBK536909/
- 1% – https://www.researchgate.net/profile/Mohamed_Khalid4/publication/332819961_LABORATORY_DIAGNOSIS_OF_THE_CAUSATIVE_DERMATOPHYTES_OF_TINEA_CAPITIS/links/5ccc63a692851c4eab80f2fa/LABORATORY-DIAGNOSIS-OF-THE-CAUSATIVE-DERMATOPHYTES-OF-TINEA-CAPITIS.pdf
- 1% – https://www.msdmanuals.com/professional/dermatologic-disorders/fungal-skin-infections/tinea-corporis-body-ringworm
- 1% – https://lookformedical.com/de/search/microsporum
- 1% – https://en.wikipedia.org/wiki/Microsporum
- 1% – http://hd.ingham.org/About/ArticlesPublications/tabid/3378/ctl/ArticleView/mid/4286/articleId/2618/Follow-Good-Hygiene-Practices-at-Ingham-County-Fair.aspx
- <1% – https://www.newhealthadvisor.org/Rash-on-Arms-and-Legs.html
- <1% – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3885931/
- <1% – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2386534/
- <1% – https://www.medicalnewstoday.com/articles/320618
- <1% – https://www.medicalnewstoday.com/articles/317970
- <1% – https://www.aad.org/media/news-releases/do-i-have-ringworm
- <1% – https://quizlet.com/4318615/vpw_micro_mycology-flash-cards/
- <1% – https://quizlet.com/21420337/chapter-24-immunity-flash-cards/
- <1% – https://drfungus.org/knowledge-base/microsporum-species/
- <1% – http://misc.medscape.com/pi/android/medscapeapp/html/A1091351-business.html