Specimens: stool, mucus flecks, and rectal swabs for culture. Large numbers of fecal leukocytes and some red blood cells often are seen microscopically.
Microscopic examination
- Microscopic examination of stool smears reveals higher number of PMN cells.
- They are Gram negative small rod shaped, non-motile, non-capsulated.
Culture and biochemical analysis
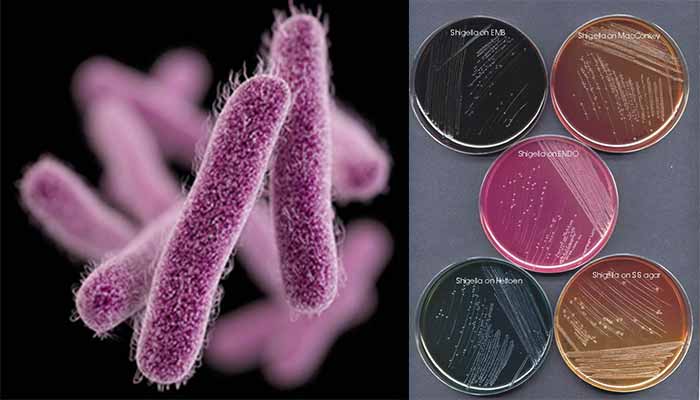
- The materials are streaked on differential media (eg, MacConkey or EMB agar or SS agar) and on selective media (Hektoen enteric agar or xylose-lysine-deoxycholate agar), which suppress other Enterobacteriaceae and gram-positive organisms.
- After overnight incubation, pale non-lactose-fermenting colonies are tested by standard biochemical and sugar utilization tests to differentiate them from other enterobacteria.
- On MacConkey, Hektoen, BCP and SS agar, typical colonies have a small diameter of 0.5–1 mm; they are convex and translucent with a smooth surface. Colorless (lactose-negative) colonies are inoculated into TSI agar.
- On Hektoen agar blue green, convex colonies are observed.
- Organisms that fail to produce H2S, that produce acid but not gas in the butt and an alkaline slant in TSI agar medium, and that are nonmotile, should be subjected to slide agglutination by specific Shigella
- Strains of S. dysenteriae are characteristically negative for mannitol fermentation and production of catalase, and they are occasionally o-nitrophenyl-b-D-galactopyranoside (ONPG) positive.
Serology
- Expression of Shiga toxin can be detected by Vero and HeLa cell tests and immunoassays designed for the Verocytotoxin produced by certain E. coli strains.
- Patients infected with S. dysenteriae 1 produce serum and salivary antibodies to the lipopolysaccharide antigens, but tests for the antibodies are not available routinely.
Molecular methods
- Strains of Shigella can be detected with polymerase chain reaction (PCR) tests targeting the genes encoding the invasion plasmid antigen H (ipaH).
- The genes for Shigella enterotoxin 2 can be detected with the ShET-2 PCR and strains with the genes encoding an aerobactin-mediated iron uptake system can be identified with a PCR using primers targeting the iuc gene complex.
- There are several commercial NAATs that directly detect shigellae in fecal samples along with some of the other major enteric pathogens.
Treatment of Shigella dysenteriae
- Treatment with a suitable antibiotic is necessary in the very young, the aged or the debilitated, and in those with severe infections.
- The World Health Organization recommends the use of ciprofloxacin, ceftriaxone and pivmecillinam for the treatment of dysentery in children.
- There is no evidence that antibiotics reduce the period of excretion of the organisms, and they should not be used in the asymptomatic person, either prophylactically or in attempts to hasten clearance after recovery.
- Ciprofloxacin, ampicillin, doxycycline, and trimethoprim– sulfamethoxazole are most commonly inhibitory for Shigella isolates and can suppress acute clinical attacks of dysentery and shorten the duration of symptoms.
- Azithromycin is often used to treat children with shigellosis.
- Some antibiotics may fail to eradicate the organisms from the intestinal tract.
- Multiple drug resistance can be transmitted by plasmids, and resistant infections are widespread.
- Many cases are self-limiting.
- Opioids should be avoided in Shigella.
Prevention and Control of Shigella dysenteriae
- Control efforts must be directed at eliminating the organisms from this reservoir by
- sanitary control of water, food, and milk; sewage disposal and fly control.
- Isolation of patients and disinfection of excreta.
- detection of subclinical cases and carriers, particularly food handlers.
- antibiotic treatment of infected individuals.
- Protection of the water and food supply and personal hygiene are crucial for preventing Shigella infections.
- Candidate vaccines in advanced development stages include a conjugate vaccine composed of O-antigen polysaccharides from Shigellae and a live attenuated vaccine.

The information is quite impressive
I need this pdf
dear sagar sir please add pathogenesis of bacteria in ur upcoming post and update the old post too ,that will b more beneficial for the students ..thank you
Hola cómo están?? Yo quiero o necesito pedirles si por favor me podrán mandar material sobre chagas… Soy Patricia de Buenos Aires Argentina…
that was great , may be can you post something about campylobacter jejuni ? THANK 🙂
Sure we will post soon. We will update all the bacteria very soon !!!