Laboratory diagnosis of Syphilis caused by Treponema pallidum
Specimen
- Samples collected from ulcers and lesions should not be contaminated with blood, microorganisms, or tissue debris.
- Polymerase chain reaction (PCR) samples should be collected on a sterile Dacron or cotton swab and placed in a cryotube containing nucleic acid transport medium or universal transport medium.
- Tissue or needle aspirates of lymph nodes should be placed in 10% buffered formalin at room temperature.
- For congenital syphilis, a small section of the umbilical cord is collected and fixed in formalin or refrigerated until processed.
- Serum is the specimen of choice for serology.
- Cerebrospinal fluid (CSF)
Microscopy
- T. pallidum is too thin to be seen by light microscopy, hence darkfield microscopy or special fluorescent stains must be used.
- Examination of the exudate from skin lesions by darkfield microscopy for diagnosis of primary, secondary, or congenital syphilis is done.
- Direct fluorescent antibody test is a more useful test for detecting T. pallidum.
- In DFA-TP, Fluorescein-labeled antitreponemal monoclonal antibodies are used to stain the bacteria.
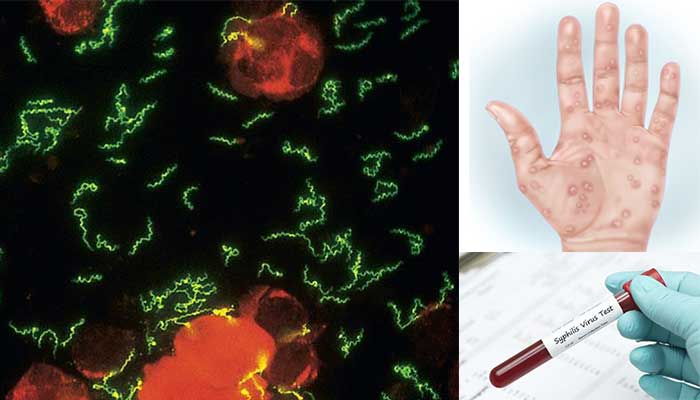
- DFA-TP visualizes specimens on slides with fluorescein isothiocyanate (FITC) labeled antibodies where T. pallidurn appears as distinct, sharply outlined, apple green fluorescent color bacilli.
Figure: Treponema pallidum in the direct fluorescent antibody testCulture
- Efforts to culture T. pallidum in vitro should not be attempted because the organism does not grow in artificial cultures.
Nucleic Acid–Based Tests
- Nucleic acid amplification tests (i.e., polymerase chain reaction [PCR]) have been developed for detecting T. pallidum in genital lesions, infant blood, and cerebrospinal fluid (CSF) but are only available in research or reference laboratories.
- Direct detection of spirochaetal deoxyribonucleic acid (DNA) in clinical material by molecular methods, may have a future role in confirming a diagnosis of syphilis in difficult or atypical cases.
Serology
- Serologic tests for treponematosis measure the presence of two types of antibodies: treponemal and non-treponemal.
- Treponemal antibodies are produced against antigens of the organisms themselves, whereas non-treponemal antibodies, often referred to as reagin antibodies, are produced in infected patients against components of mammalian cells.
Non-specific antibody detection / Non-treponemal antibody detection
- Nontreponemal tests measure immunoglobulin (IgG) and IgM antibodies (also called reaginic antibodies) developed against lipids released from damaged cells during the early stage of disease and that appear on the cell surface of treponemes.
- The antigen used for the non-treponemal tests is cardiolipin, which is derived from beef heart.
- The non treponemal tests are universally used as screening tests for syphilis and to check the efficacy of treatment.
a) VDRL (Venereal Disease Research Laboratory) test
- Measured amount of cardiolipin antigen is taken in a tube or slide
- Serum is heated to inactivate complement
- Anti-cardiolipin antibodies (IgG, IgM or IgA) called reagin, react with the cardioplipin antigen which is visualized through flocculation of the fluid in test tube or on slide.
b) RPR (Rapid Plasma Reagin) Test
- Serum is not heated to inactivate complement.
- In RPR, Choline chloride is added to prevent complement.
- Observation of flocculation on slide.
c) Toluidine Red Unheated Serum Test (TRUST)
- The TRUST antigen suspension is identical to VDRL antigen but contains a toluidine red pigment.
- When a specimen contains antibody, the TRUST antigen agglutinates and the reaction appears as red clumps against the white background of the test cards.
- If antibody is not present, the test mixture remains a faint red color and no agglutination occurs.
d) Unheated serum regain test (USR)
- USR is similar to VDRL except for EDTA is used as antigen stabilizer.
- Choline chloride is used to inhibit the non specific inhibitors in serum.
Specific antibody test / Treponemal antibody test
A. Microhemagglutination Treponema pallidum (MHA-TP) test
- In the MHA- TP, heated serum is mixed with a sonicated non pathogenic Reiter strain and incubated with sheep erythrocytes coated with sonicated Treponema pallidum Nichols strain in a microtiter plate.
- If antibodies to Treponema pallidum are present, they react with the sensitized erythrocytes to produce a uniformly thin mat of agglutinated cells that covers the entire bottom of the well.
B. Treponema pallidum hemagglutination assay (TPHA)
- TPHA is an indirect hemagglutination assay that uses sensitized red blood cells that aggregate when exposed to positive patient serum.
- In this test, T. pallidum antigen is coated on to the surface of red blood cells, and specific antibody in test sera causes haemagglutination.
C. Treponema pallidum–particle agglutination (TPPA)
- The pallidum particle agglutination (TPPA) test works on the same principle as the TPHA, but treponemal antigen is coated onto coloured gelatin particles rather than red blood cells.
D. Fluorescent treponemal antibody absorbed (FTA -ABS)
- Patient serum is mixed with a sorbent/absorbent (the “ABS” part of the test).
- The sorbent/absorbent contain an extract of a non-pathogenic treponeme, Treponema phagedenisbiotype Rieter.
- The purpose of the absorbent is to remove anti-treponemal antibodies that are not specific for the syphilis bacteria.
- Patient’s serum is layered on a slide previously coated with killed T
- Fluorescein-conjugated antihuman antibody reagent is then applied as a marker for specific anti-treponemal antibodies in the patient’s serum and then slide is examined under fluorescent microscope.
E. Enzyme lmmunoassays
- ELISA specific to IgG and IgM have been developed for the diagnosis of syphilis.
- They have excellent sensitivity and specificity.
- IgM ELISA is more sensitive than IgM FTA-ABS for diagnosis of congenital syphilis.
F. Western Blot
- Western blot is available for detecting lgG and IgM antibodies separately.
- It is highly sensitive and specific.
G. Group-specific test
- Reiter’s protein complement fixation test (RP-CFT):
- It works on the principle of CFT.
- Detects group or genus specific treponemal antibodies against the protein antigen prepared from cultivable Reiter strain.
- Its sensitivity is low and is obsolete now-a-days.
Treatment of Syphilis
- The treponemes cannot be cultivated, hence susceptibility testing is not performed.
- Penicillin is the drug of choice for treating T. pallidum infections.
- Long-acting benzathine penicillin is used for the early stages of syphilis, and penicillin G is recommended for congenital and late syphilis.
- Ceftriaxone is also highly active in most cases of syphilis other than early syphilis.
- Doxycycline or Tetracycline or Erythromycin or Chloramphenicol can be used as alternative antibiotics for patients allergic to penicillin.
- However , treatment varies depending on the stage of disease and the host (e.g., children or adults, HIV-infected or infected with congenital syphilis).
- Only penicillin can be used for the treatment of neurosyphilis. Thus penicillin allergic patients must undergo desensitization.
- This is also true for pregnant women, who should not be treated with the tetracyclines.
Prevention and control of Syphilis
Protective vaccines are not available and hence prevention and control can be done by
- Treatment of cases and contacts (sexual partners)
- Education about safe sex practices
- Prophylactic use of barrier contraceptive methods

worthy learning