Pancreatic cells are cells that form the pancreas. The pancreas is an organ located behind the stomach that plays two main roles in the body: it produces digestive enzymes to break down food, and it produces hormones such as insulin and glucagon to regulate blood sugar levels.
So, the pancreas performs both endocrine and exocrine functions. The majority of the pancreas consists of exocrine cells called pancreatic acinar cells that are responsible for producing digestive enzymes.
The endocrine component is made up of pancreatic islet cells that produce and release hormones that are necessary for regulating glucose metabolism.
Types of Pancreatic Cells
Two main types of pancreatic cells form the pancreas:
1. Acinar cells
Acinar cells are the pancreatic cells involved in the exocrine function of the pancreas. These are secretory cells that form the majority of the pancreas. They produce and release digestive enzymes into the pancreatic duct which is connected to the duodenum. The digestive enzymes produced by acinar cells are essential for breaking down food into simpler forms. The pancreas secretes different enzymes, including proteolytic enzymes, lipolytic enzymes, and amylase.
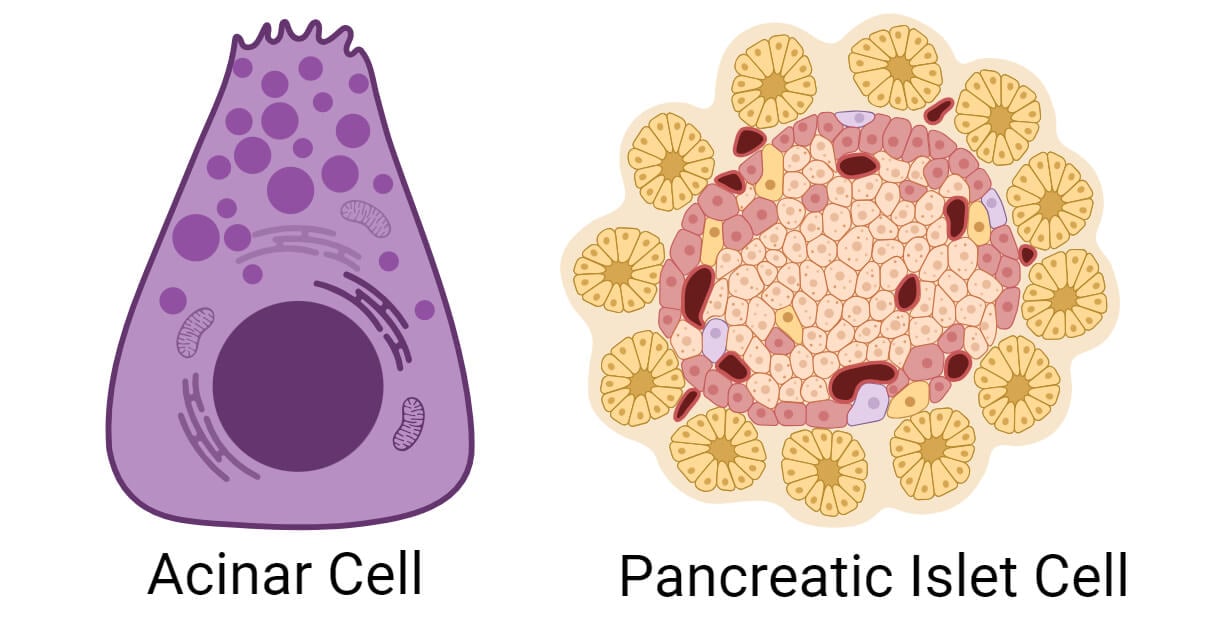
2. Pancreatic islet cells (Islets of Langerhans)
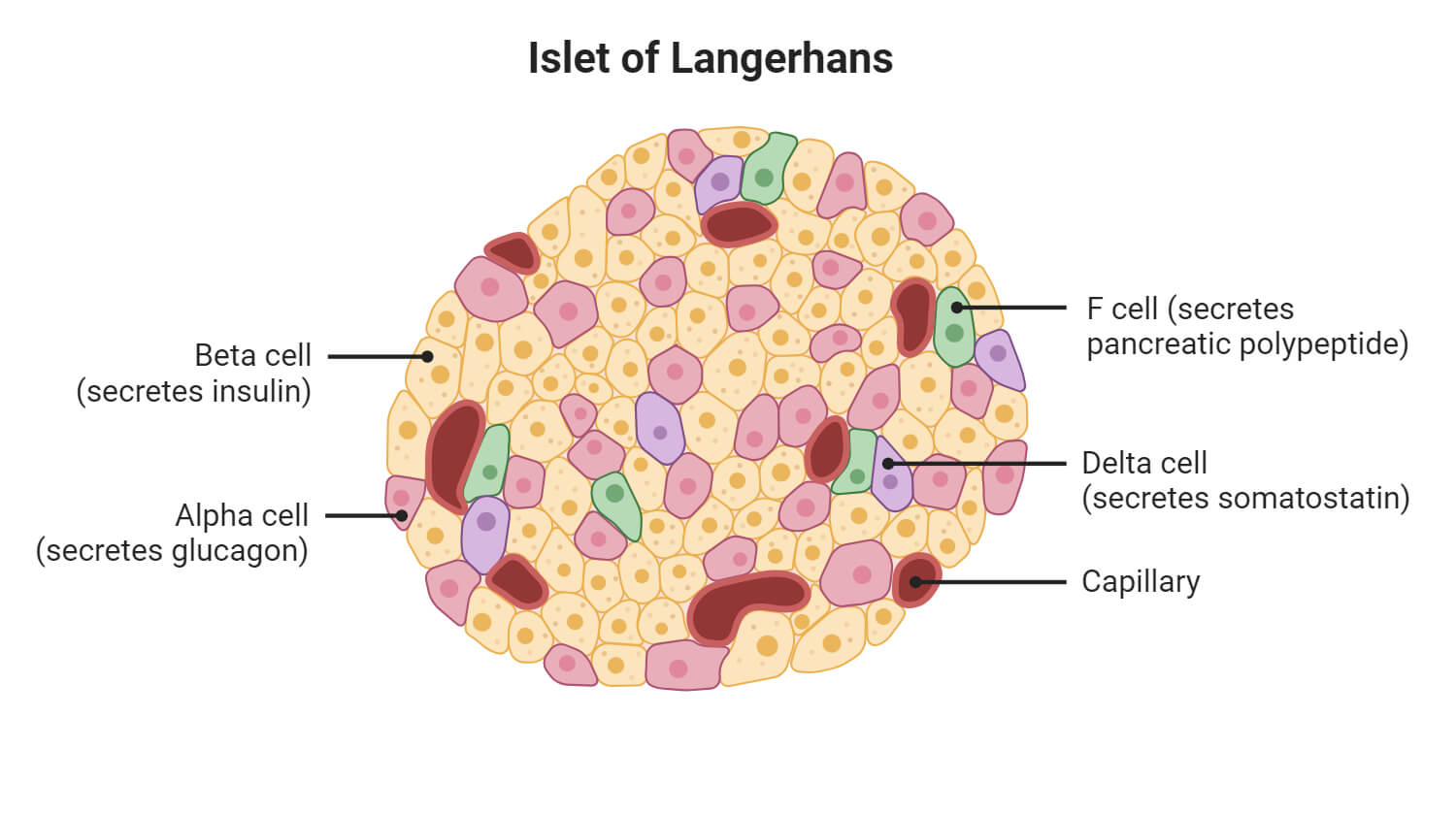
Pancreatic islet cells (Islets of Langerhans) are clusters of cells found scattered throughout the pancreas that perform endocrine functions. They are responsible for producing and releasing hormones that regulate glucose levels. These islets are made up of various types of endocrine cells, including beta (β), alpha (α), delta (δ), gamma (γ), and epsilon (ϵ) cells, each producing different hormones like insulin, glucagon, somatostatin, pancreatic polypeptide, and ghrelin, respectively.
- Beta cells are the most common type of islet cells. They produce insulin that helps regulate glucose levels. Beta cells make up about 70% of the total islet cells and are located centrally in the islet.
- Alpha cells produce glucagon that increases blood sugar levels by stimulating the liver to convert stored glycogen into glucose. This process occurs when blood glucose levels are low, such as during fasting.
- Delta cells produce somatostatin that regulates the secretion of both insulin and glucagon, helping to maintain stable blood sugar levels. Delta cells make up about 3–10% of the islet cells and are scattered throughout the islet.
- Gamma cells, also known as PP cells (Pancreatic polypeptide cells) are cells that produce pancreatic polypeptide, which helps regulate the release of digestive enzymes from the pancreas.
- Epsilon cells are the least common type of islet cells and represent less than 1% of the total islet cells. These cells produce the hormone ghrelin which stimulates hunger. Ghrelin levels increase before meals and decrease after eating, helping to regulate hunger.
Anatomy and Structure of Pancreatic Cells
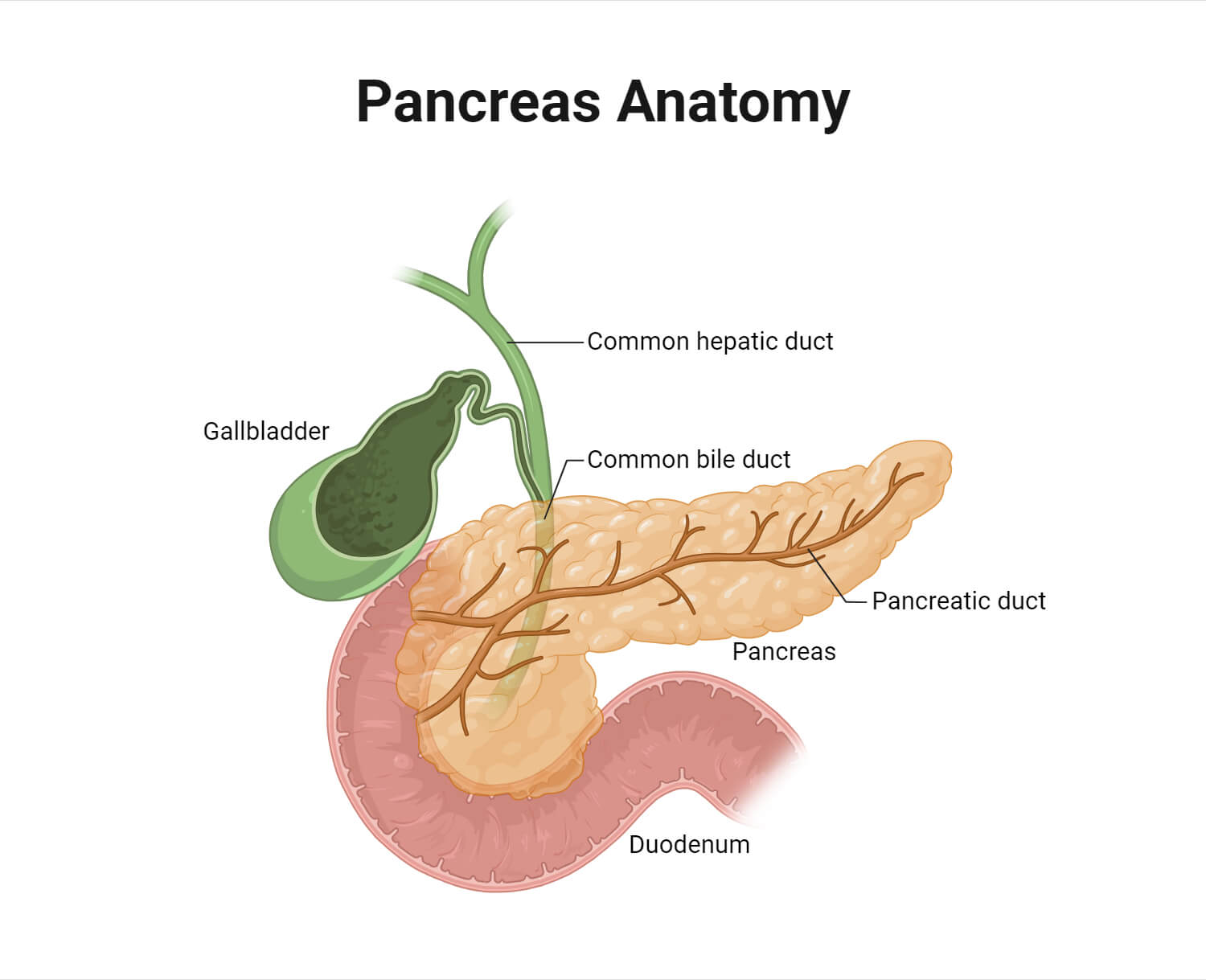
- The pancreas is located behind the stomach and situated between the duodenum on the right side and the spleen on the left. Anatomically, the pancreas is divided into the head, body, and tail regions.
- The pancreas is composed primarily of networks of tubes including the main pancreatic duct and other accessory ducts. The pancreatic duct releases substances into the duodenum.
- The pancreas consists of two main cell types: exocrine cells and endocrine cells. The majority of the pancreas is formed by the exocrine portion.
- The exocrine part of the pancreas forms about 98% of the pancreas. Acinar cells are the primary exocrine cells of the pancreas. These are pyramidal-shaped cells that produce digestive enzymes. They contain abundant rough endoplasmic reticulum and Golgi apparatus which indicates their active secretory function. These cells contain dense zymogen granules in the apical region, where digestive enzymes are stored and released. They have a broad base and a narrow apical surface that surrounds a small central lumen, which is connected to a system of ducts that lead to the pancreatic duct.
- The endocrine part forms about 2% of the pancreas. Within the exocrine tissue, there are small clusters of endocrine cells called pancreatic islets that are scattered throughout the pancreas. They contain different types of endocrine cells, including α, β, δ, ε, and PP cells. These islets appear as large, pale-staining clusters surrounded by exocrine tissue. They secrete hormones such as insulin, glucagon, somatostatin, and pancreatic polypeptide, which are essential for maintaining metabolic balance. These islets are surrounded by a sheath of reticular fibers.
Functions of Pancreatic Cells
The pancreatic cells perform two vital functions in the body: endocrine and exocrine. The endocrine function is performed by islet cells while the exocrine function is carried out by the acinar cells.
- Acinar cells are involved in the exocrine function of the pancreas. They produce and release digestive enzymes essential for breaking down complex food molecules into simpler forms.
- Beta cells produce and secrete insulin which regulates blood sugar levels by promoting the uptake of glucose. This lowers blood glucose levels after meals. These cells also inhibit the liver from releasing glucose, promote the uptake of amino acids for protein synthesis, and prevent the breakdown of fats.
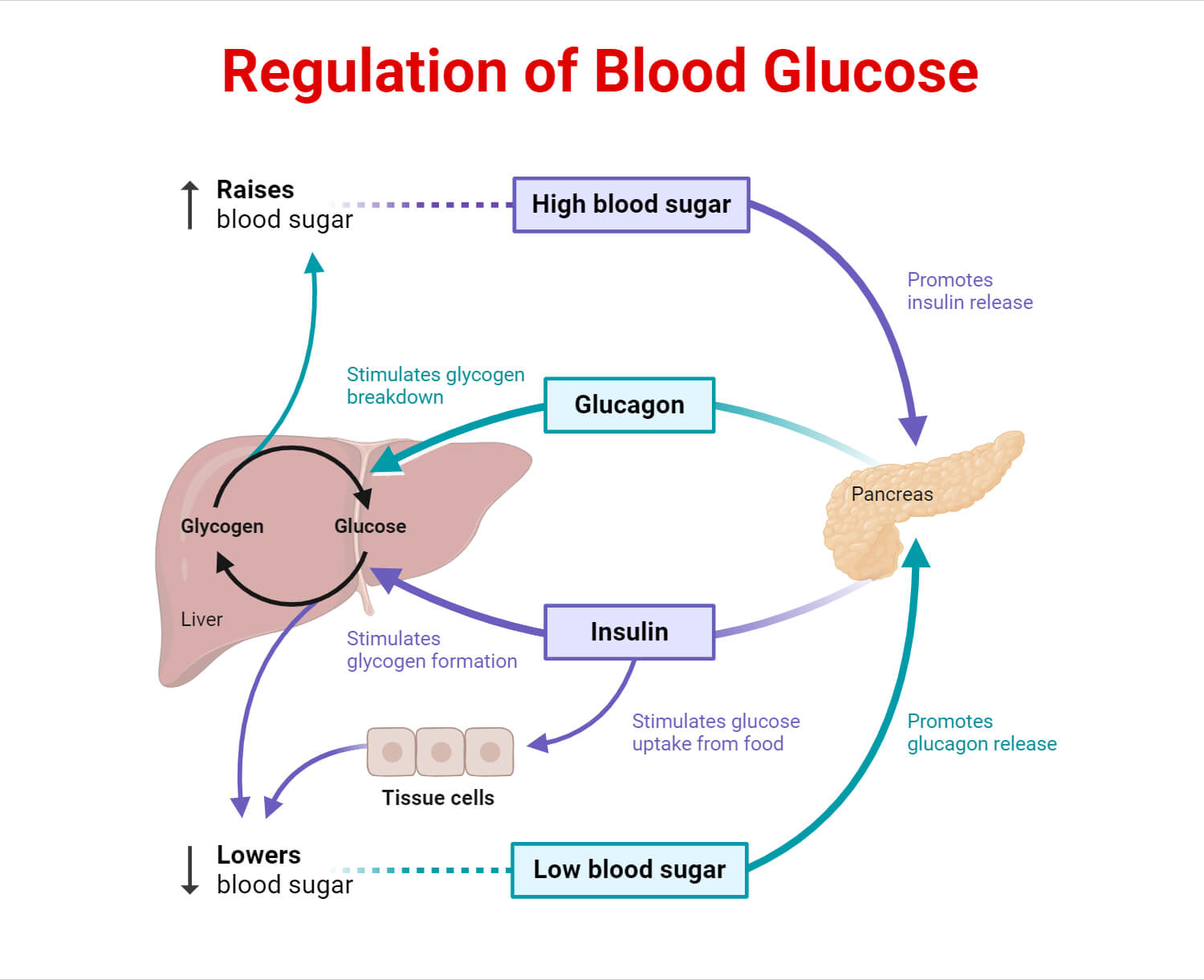
- Alpha cells produce the hormone glucagon that increases blood sugar levels by promoting the release of glucose from storage sites like the liver. Glucagon works opposite to insulin. It increases blood glucose levels during fasting or low blood sugar conditions.
- Delta cells produce and release somatostatin that acts as an inhibitor and regulates the secretion of insulin and glucagon. This helps maintain stable blood sugar levels by regulating the release of these hormones.
- Gamma cells produce pancreatic polypeptide that regulates the release of digestive enzymes from the pancreas.
- Epsilon cells produce and secrete the hormone ghrelin that stimulates hunger and regulates food intake.
Diseases and Disorders of Pancreatic Cells
- Chronic pancreatitis is the most common pancreatic disorder characterized by inflammation of the pancreas which is caused by different factors such as poor health habits, improper diet, alcohol abuse, smoking, genetic factors, autoimmune conditions, or certain medications. Repeated inflammation can lead to irreversible damage to pancreatic cells impacting digestive processes and insulin production. Severe cases may lead to other complications such as kidney failure and respiratory issues.
- Acute pancreatitis is a sudden inflammation of the pancreas caused by factors like gallstones, excessive alcohol intake, certain medications, or infections. Its symptoms may include severe abdominal pain, fever, and vomiting. Severe cases can result in pancreatic necrosis or abscess formation.
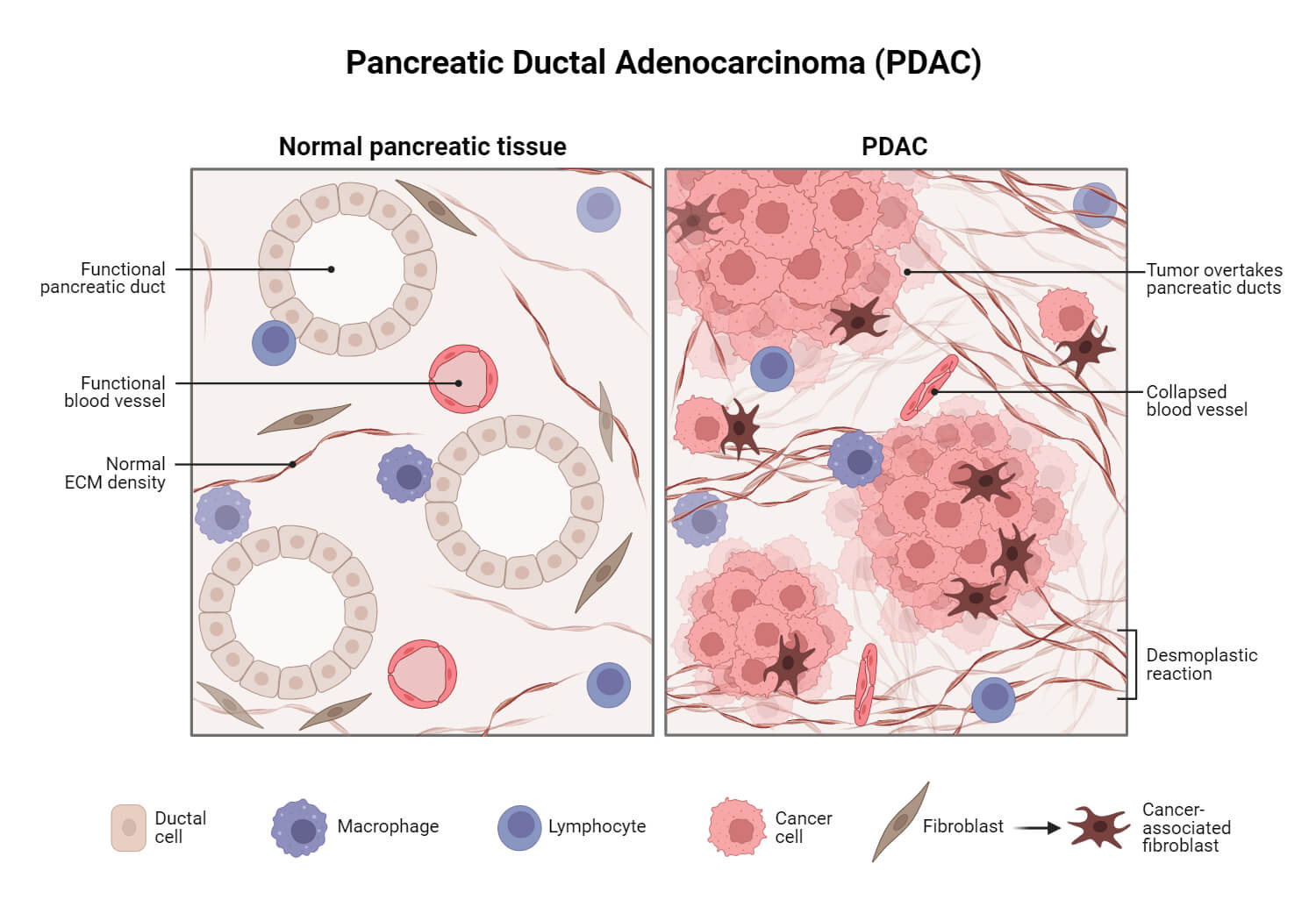
- Pancreatic cancer can occur in both exocrine and endocrine pancreas cells but it often arises from the exocrine cells. Risk factors include smoking, age, obesity, family history, and certain genetic mutations. Symptoms include jaundice, abdominal pain, weight loss, changes in stool color, and fatigue. Pancreatic cancer treatment includes various approaches based on the stage of the cancer and the condition of the patient. The primary treatment approaches are surgery, radiation therapy, chemotherapy, targeted therapy, and certain medications to relieve pain.
- Pancreatic cysts are fluid-filled sacs in the pancreas that are often detected incidentally during imaging tests like CT and MRI. Pancreatic cysts can be classified as neoplastic or nonneoplastic. Factors such as age, pancreatitis history, family history of pancreatic cancer, or specific hereditary syndromes like Von Hippel-Lindau disease or cystic fibrosis can increase the risk of developing these cysts.
- Exocrine Pancreatic Insufficiency (EPI) is a disorder that occurs when the pancreas cannot produce enough digestive enzymes. It can occur due to chronic pancreatitis, cystic fibrosis, pancreatic cancer, or other pancreatic disorders. Symptoms include weight loss, diarrhea, bloating, and nutrient deficiencies. Treatment options for EPI include pancreatic enzyme replacement therapy, a high-calorie and high-fat diet, and taking prescription vitamins.
- Diabetes is a metabolic disorder characterized by high blood sugar levels caused by inadequate insulin production or insulin resistance. In Type 1 diabetes, the immune system attacks and destroys the insulin-producing pancreatic beta cells resulting in insufficient insulin production and high blood sugar. Type 2 diabetes involves insulin resistance causing cells to become less responsive to insulin and thus leading to high blood sugar levels. Both type 1 and type 2 diabetes result from damaged pancreatic cells.
- Zollinger-Ellison syndrome is a rare disease caused by gastrin-secreting tumors in the pancreas or duodenum. This leads to excessive production of the hormone gastrin which in turn produces excessive gastric acid. Symptoms include severe peptic ulcers, abdominal pain, diarrhea, and heartburn.
- Shwachman-Diamond Syndrome (SDS) is another rare disease that affects different organs, including the pancreas. Patients with SDS may develop exocrine pancreatic insufficiency that causes difficulties in digesting food and absorbing nutrients. It also involves bone marrow dysfunction and skeletal abnormalities.
References
- 15.11B: Types of Cells in the Pancreas – Medicine LibreTexts
- Benjamin O, Lappin SL. Chronic Pancreatitis. [Updated 2022 Jun 21]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK482325/
- Britannica, T. Editors of Encyclopaedia (2022, August 13). islets of Langerhans. Encyclopedia Britannica. https://www.britannica.com/science/islets-of-Langerhans
- Capurso, G., Traini, M., Piciucchi, M., Signoretti, M., & Arcidiacono, P. G. (2019). Exocrine pancreatic insufficiency: prevalence, diagnosis, and management. Clinical and experimental gastroenterology, 12, 129–139. https://doi.org/10.2147/CEG.S168266
- Da Silva Xavier G. (2018). The Cells of the Islets of Langerhans. Journal of clinical medicine, 7(3), 54. https://doi.org/10.3390/jcm7030054
- El Sayed SA, Mukherjee S. Physiology, Pancreas. [Updated 2023 May 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459261/
- Gapp J, Tariq A, Chandra S. Acute Pancreatitis. [Updated 2023 Feb 9]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK482468/
- Karpińska, M., Czauderna, M. (2022). Pancreas—Its Functions, Disorders, and Physiological Impact on the Mammals’ Organism, 13. https://www.frontiersin.org/journals/physiology/articles/10.3389/fphys.2022.807632
- Longnecker, Daniel S. 2021. Anatomy and Histology of the Pancreas.
- Pancreapedia: Exocrine Pancreas Knowledge Base, DOI: 10.3998/panc.2021.01
- Pancreatic Cancer Treatment – NCI
- Pancreatic Cyst: Symptoms, Causes, Types & Treatment (clevelandclinic.org)
- Shahid Z, Singh G. Physiology, Islets of Langerhans. [Updated 2022 Oct 3]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK542302/
- Talathi SS, Zimmerman R, Young M. Anatomy, Abdomen and Pelvis, Pancreas. [Updated 2023 Apr 5]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK532912/
