Image created with biorender.com
General Characteristics of Aspergillus spp
- It is commonly found in soil, with a saprophytic mode of nutrition, obtaining its nutrients from dead and decaying matter.
- The saprophytic nature of Aspergillus spp means they fully depend on environmental materials, which allows them to produce enzymes such as amylase that breaks down compounds into simple products that can be absorbed by the vegetative hyphae.
- High production of the amylase enzymes enables the consistent decaying of all organic materials within their subsequent environment and availability of more food materials for utilization during reproduction and growth.
- It is a spore-forming mold fungus reproduces asexually by producing spores in the form of conidia (conidium: singular).
- The conidia are densely found in the air.
- In the availability of moisture, warmth, and nutrients, the conidia can germinate forming hyphae that later develop the fungal mycelium.
- The hyphal filament allows the fungus to grown and reproduce.
- The conidial spores are densely produced into the air during sporulation and are consistently inhaled by humans and animals in hundreds per day.
- It can be pathogenic in humans causing severe allergic reactions and respiratory opportunistic fungal infection known as Aspergillosis, especially in immune-compromised individuals.
- Some of the common Aspergillus spp include:
- Aspergillus fumigatus
- Aspergillus niger
- Aspergillus flavus
- Aspergillus nidulans
- Aspergillus clavans
Habitat of Aspergillus fumigatus
- Aspergillus fumigatus is a fungus belonging to the Aspergillus group of fungi,
- Their ecological niche is in soil, surviving and growing on organic debris.
- It is one of the most common ubiquitous airborne saprophytic fungi
- It is predominantly found in the air hence it is constantly inhaled in the form of conidia by humans and animals.
Morphology of Aspergillus fumigatus
- The morphology of Aspergillus fumigatus is defined by the hyphal conidia and conidiophores.
- They have a green spiked conidia i.e the surface has small spikes covering its surface.
- The conidia are 2.5-3um in diameter.
- The conidia have a smooth surface or spiked (spinose).
- Conidia are produced in column chains that are basipetal (facing downwards) from green phialides of 6-8 by 2-3um in size.
- Some A. fumigatus strains produce white conidia because they lack pigment.
- Conidia chains are produced directly on broadly clavate vesicles (20-30um in diameter) in the absence of metulae (one of the outermost branches of a conidiophore from which flask-shaped phialides radiate).
Cultural Characteristics of Aspergillus fumigatus
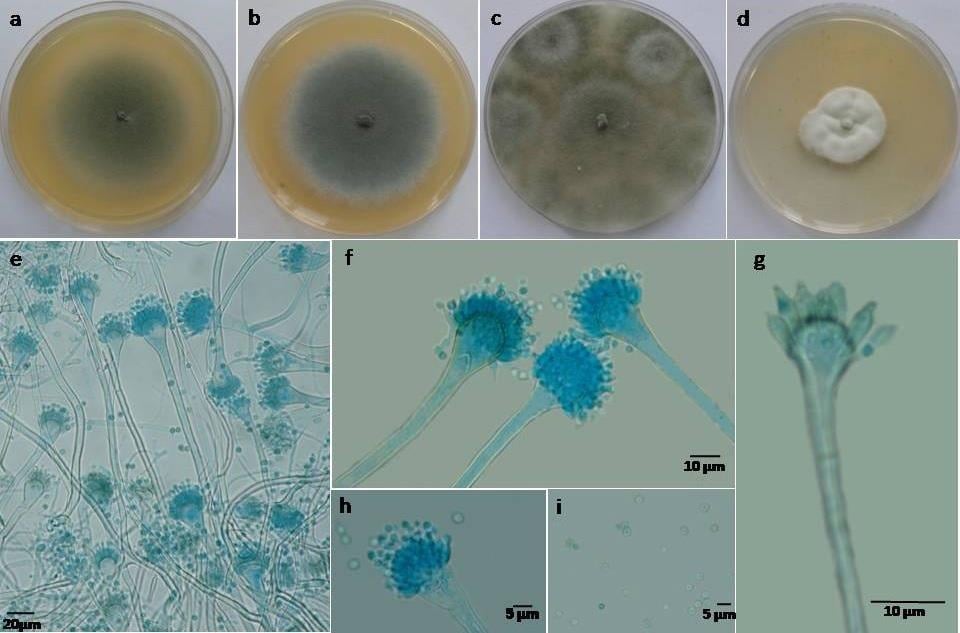
Figure: Aspergillus fumigatus. a, b. Seven days colonies of autumn (A.PZ1) and spring (A.BZ1) isolates on MEA; c, d. Seven days colonies of autumn (A.PZ1) and spring (A.BZ1) isolates on CYA; e, f. conidiophores; g. vesicle and phialides; h, i. conidiophores with conidia. Image Source: Mycologia Iranica
- Aspergillus fumigatus is thermophilic hence it in temperatures as high as 55°C and can survive in temperatures of up to 70°C.
- It is a fast-growing fungus in fungal culture.
- It grows well in the basic fungal medium, Sabouraud Dextrose Agar (SDA).
- It produces white, yellow, yellow-brown, brown to black or green colored colonies.
- On Czapek-Dox agar at 25°C, it produces colonies of 4 ± 1 cm within a week.
Life Cycle of Aspergillus fumigatus
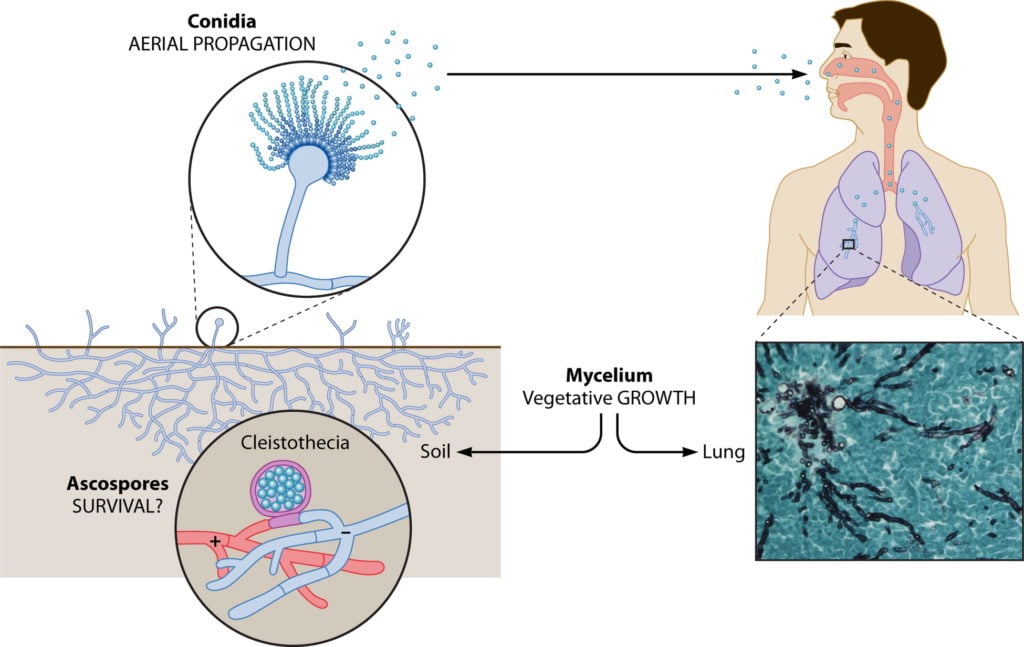
Figure: Life Cycle of Aspergillus fumigatus. Image Source: American Society for Microbiology
They have asexual sporulation type of reproduction.
- When the released spores, called conidia, land on a surface with suitable growth and nutrition factors, the conidia germinate to form hyphae.
- The hyphae grow and produce aerial hyphae and subsurface hyphae.
- These aerial hyphae grow the conidiophore, which produces the phialides.
- Column phialides produce spores in the form of conidia, in chains.
Pathogenesis of Aspergillus fumigatus
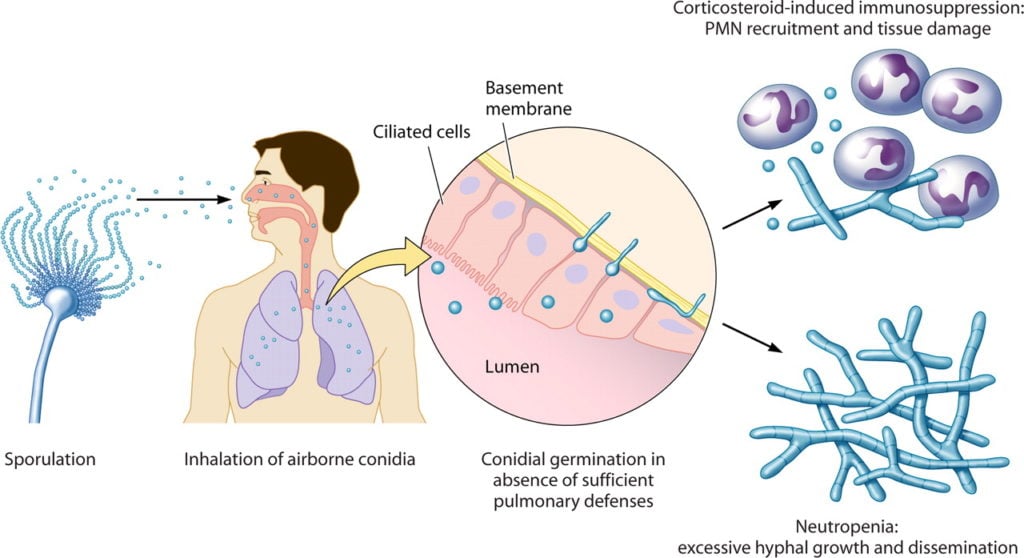
Aspergillus fumigatus is a highly ubiquitous fungus, known to spread its spores in dense numbers that can be inhaled by both humans and animals in over 100spores in a day.
Image Source: American Society for Microbiology
Transmission
- They are transmitted by the inhalation of fungal spores (conidia).
- They are found ubiquitously in the environment and they are continuously inhaled by humans.
- When inhaled by persons with a weakened immunity of the respiratory tract, they can cause opportunistic infections.
Host colonization
- After inhalation by immune defected individuals, the fungal spores attach to the epithelial cells that are damaged by immune therapies such as drugs such as corticosteroids, radiations, that allow the spores to colonize the damaged surface.
- A unique characteristic of the Aspergillus fumigatus conidia is there ability to evade the innate immune defenses by cilia and the mucosal lining of the respiratory tract. Conidia spores have gliotoxin, helvolic acid, and fumagillin which assist in evading the mucociliary layer of the respiratory tract.
- The conidia then bind to the defected epithelial cells of the respiratory tract and membranes within the tract by the help of sialic acid. Sialic acid helps in the asexual reproduction in pathogenic Aspergilli.
- The conidia are then engulfed by macrophages forming a phagosome where they germinate preventing apoptotic cell death of epithelial cells.
- The fungi also produce protease enzymes that assist in the colonization of lung tissues, elastase enzyme which degrades the host tissues in the lungs.
Evading of macrophage mechanisms
- Acute inflammation causes a reduction in the effector mechanism of alveolar macrophages. This causes the Aspergillus fumigatus to invade and kill the macrophages, leading to inflammations immediately the fungal conidia starts to germinate.
- Conidial spores are recognized by macrophages by a carbohydrate complex known as beta (1,3) glucal found of the surface of the spores.
- This complex binds to the dectin on the alveolar macrophages, activating macrophage phagocytosis and inflammation in the alveolar and the lung tissues.
- Additionally, conidia in the resting phase also have the ability to evade the macrophage mechanisms because of the presence of superoxide dismutases that acts as a reactive oxygen species (ROS) scavenger.
Dissemination
- During hyphal growth, the aerial hyphae start to invade the endothelial cells of the blood vessels in the lungs.
- They first start to invade the outer blood vessels, moving through the endothelial cells into the inner part of the blood vessels.
- When the hyphae reach the blood, they fragment and start to circulate in the bloodstream and attach to the luminal of the endothelial cells.
- They then grow into the abluminal parts and continues to spread within the bloodstream and the rest of the body.
- The body reacts by producing neutrophils that act by adhering and killing the hyphae but because of the defragmentation and spread, sometimes the number of neutrophils may be overwhelmed by the hyphal colonization.
- This may lead to an invasion of the pulmonary tissues and the vascular system causing thrombosis and tissue necrosis, This causes a hematogenous spread to other body organs and even to the brain and its tissues.
Clinical manifestation of Aspergillus fumigatus infection
- Asthma-like allergic bronchopulmonary aspergillosis-This occurs when IgE antibody production is triggered by the Aspergillus conidia causing an immediate asthmatic reaction. In others, the conidia germinate and hyphae colonize the bronchial tree without invading the lung parenchyma, a major characteristic of allergic bronchopulmonary aspergillosis associated with asthma, recurrent chest infiltrates, eosinophilia and type I (immediate) and type III (Arthus) skin test hypersensitivity to Aspergillus antigen. Many patients produce sputum with Aspergillus and serum precipitins. They have difficulty breathing and may develop permanent lung scarring. Normal hosts exposed to massive doses of conidia can develop extrinsic allergic alveolitis and allergic sinusitis.
- Invasive pulmonary aspergillosis- This infection is most common among patients with HIV with a low CD4 count, lymphocytic or myelogenous leukemia and lymphoma, stem cell transplant recipients, and especially individuals taking corticosteroids. It occurs after the inhalation and germination of conidia leading to the development of the pneumonic disease that may or may not disseminate. Its symptoms include fever, cough, dyspnea, and hemoptysis. The hyphae invade the lumen and the walls of blood vessels that cause thrombosis, infarction, and necrosis in the lungs. It can then spread to the gastrointestinal tract, kidney, liver, brain, or other organs, producing abscesses and A lack of rapid treatment, the patients can deteriorate fast.
- Endocarditis- It occurs when invasive aspergillosis infects the heart muscles which may result in heart failure, shocks, and cardiomyopathies.
- Cutaneous aspergillosis- it affects patients with surgical wounds and skin burns which my cause septicemic infections and wound sepsis.
Laboratory diagnosis of Aspergillus fumigatus
Specimen: Sputum, bronchial wash, tracheal aspirates collected from patients with pulmonary disease. Tissue biopsies from patients with disseminated disease.
Direct Microscopy
- Using KOH Wet mount or calcofluor white, sputum samples, bronchoalveolar lavage, bronchial biopsies show non-pigmented septate hyphae with repeated dichotomous branching.
Cultural isolation
- Using basic fungal media Saboraud Dextrose Agar (SDA), Aspergillus fumigatus produces fast-growing colonies that are white, yellow, yellow-brown, brown to black, or green in color. Microscopically, cultures show colonies with characteristic radiating chains of conidia.
Antigen detection
- There are several antigen tests for the detection of Aspergillus from blood, urine, and CFS. In a person with invasive aspergillosis, there may be high levels of galactomannan antigen in serum. Galactomannan is rapidly eliminated from the blood, therefore serial screening twice weekly is recommended for optimal diagnosis.
Serology
- Immunodiffusion tests for the detection of antibodies to Aspergillus species in the diagnosis of allergic, aspergilloma, and invasive aspergillosis. Patients with Allergic Bronchopulmonary Asthma have high levels of IgE specific for Aspergillus antigens and some IgG precipitins.
Treatment
- Invasive Aspergillosis is effectively treated with voriconazole. However, the species seems to have developed resistance to azoles and therefore a combination of voriconazole with Amphotericin-B or any antifungal drugs can be used.
- In rare cases, surgery is used to remove the infected tissue, although this is risky since patients with IA are already very ill. As a preventative measure, patients at high risk of developing IA can be given anti-fungal drugs like aerosolized liposomal amphotericin B. The key to the treatment of invasive aspergillosis (IA) is early detection.
- Treat allergic forms of aspergillosis with corticosteroids or disodium cromoglycate.
Prevention and Control
- Persons at risk of allergic infection and invasive aspergillosis should avoid exposure to conidial spores od Aspergillus spp.
- Bone-marrow transplant units should have filtered air-conditioning systems, monitored airborne contamination of patients, reduced visits to patients and application of measures that isolate patients and minimize the risks of exposure to Aspergillus conidia and molds,
- Preventive measures like prophylactic low dosage of amphotericin B or Itraconazole for persons at risk.
References
- Medical Microbiology, by Jawertz: 2013
- Microbiology by Prescott L., 5th Edition
- https://cmr.asm.org/content/12/2/310
- https://www.microscopemaster.com/aspergillus.html
- https://mycology.adelaide.edu.au
- Latgé J. P. (1999). Aspergillus fumigatus and aspergillosis. Clinical microbiology reviews, 12(2), 310–350.
Sources
- 2% – https://microbeonline.com/aspergillus-fumigatus-characteristics-pathogenesis-diagnosis/
- 1% – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC88920/
- 1% – https://quizlet.com/53655848/opportunistic-fungal-infections-flash-cards/
- 1% – https://quizlet.com/283138309/quiz-3-mycology-flash-cards/
- <1% – https://www.researchgate.net/publication/277682686_Efficacy_of_aerosolized_amphotericin_B_desoxycholate_and_liposomal_amphotericin_B_in_the_treatment_of_invasive_pulmonary_aspergillosis_in_severely_immunocompromised_rats
- <1% – https://www.poz.com/basics/hiv-basics/aspergillosis
- <1% – https://www.ncbi.nlm.nih.gov/pubmed/1338541
- <1% – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3488923/
- <1% – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3407891/
- <1% – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3326383/
- <1% – https://www.ncbi.nlm.nih.gov/books/NBK26848/
- <1% – https://www.medindia.net/patientinfo/fungal-infections.htm
- <1% – https://universityofglasgowlibrary.wordpress.com/2011/08/22/ubiquitous-fungus/
- <1% – https://thorax.bmj.com/content/70/3/270
- <1% – https://old.aspergillus.org.uk/secure/speciesdatabase/fumigatus/fumicult.php
- <1% – https://old.aspergillus.org.uk/secure/sequence_info/Aterreus.pdf
- <1% – https://courses.lumenlearning.com/microbiology/chapter/respiratory-mycoses/
- <1% – http://www.microbiologybook.org/mhunt/rna-ho.htm
- <1% – http://onlinelibrary.wiley.com/doi/10.1111/j.1398-9995.2006.01116.x/full

Good job
I am writing a research paper on Aspergillosis infection. However I seem stuck on the methodology as I want to do in vitro analysis and document results.Which is the easiest method to obtain results for herbal medicine/extracts?
Hello Gabriel,
even if the answer comes quite late and you have probably already finished your research, here is my view on the best methods.
You can work with perforated plates. To do this, take a 1.5% agar plate with a defined minimal medium. A certain quantity of spores (1000000 spores/conidia in total) is mixed in 5ml of softer agar (0.7%) at a maximum temperature of 56°C and poured onto the plate. This agar is distributed on the plate by means of uniform swirling. After hardening, a hole can be punched in the centre of the agar plate using the back of a 1 ml pipette tip. Various plant extracts, e.g. in dilutions, can now be pipetted into this hole. Incubate at appropirate temperature. A halo can be observed after 24h/48h/72h if the extracts have an effect on fungal growth.
An alternative in vitro method is the so-called liquid minimal medium (MIC) test. In 96-well plates (flat bottom), the extracts to be tested can be perfectly diluted in a row in liquid minimal nutrient medium. A corresponding quantity of spores (e.g., 1000) is then added and allowed to germinate at the appropriate temperature (dependent on the fungal strain). The plates are then incubated for 24, 48, or 72 hours, and the results are compared to those obtained from the medium without extracts.