Clostridioides difficile, formerly known as Clostridium difficile, is a bacterium most commonly found in soil and hospital environments and is responsible for causing diarrheal illness.
The bacterium infects individuals taking antibiotics. It produces toxins that damage the intestinal mucosa, leading to conditions ranging from mild diarrhea to life-threatening colitis.
Taxonomy and Classification of Clostridioides difficile
Domain: Bacteria
Kingdom: Bacillati
Phylum: Bacillota
Class: Clostridia
Order: Peptostreptococcales
Family: Peptostreptococcaceae
Genus: Clostridioides
Species: C. difficile
Morphology and Microscopy of Clostridioides difficile
- Gram-positive rod-shaped bacillus
- Approximately 0.6 µm wide and 3 to 7 µm long, occurring singly or in chains.
- Spore-forming
- Motile
- Capsulated
Under the microscope, they appear as pink-colored, rod-shaped bacilli.
Cultural and Growth Characteristics of Clostridioides difficile
- Obligate anaerobes but can grow under microaerophilic conditions.
- Optimum temperature: 37˚C
- Optimum pH: 7.2
- On Nutrient Agar: large, flat, filamentous, and translucent colonies with irregular edges.
- On Blood Agar: Shows a double zone of β-hemolysis.
- On MacConkey Agar: Forms green fluorescent colonies.
- On Marshal’s Medium: produce black colonies
- On Robertson’s Cooked Meat Broth: Proteolytic species turn meat black with a foul smell, while saccharolytic species turn meat pink. Production of gas.
- On Litmus Milk: acid clot and stormy fermentation.
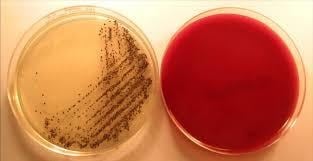
Source: https://www.researchgate.net/figure/Culture-of-C-difficile-from-a-stool-sample-after-24-h-of-incubation-on-IDCd-medium_fig1_45951767
Biochemical and Identification Tests of Clostridioides difficile
| Tests | Results |
| Gram Staining | Positive |
| Catalase | Negative |
| Oxidase | Negative |
| Indole | Negative |
| OF (Oxidative-Fermentative) | Anaerobic |
| VP (Voges Proskauer) | Negative |
| H2S | Usually Negative and sometime Positive |
| Urease | Negative |
| Gelatin Hydrolysis | Positive |
| Nitrate Reduction | Negative |
| Fermentation of | |
| Glucose | Positive |
| Maltose | Negative |
| Ribose | Negative |
| Lactose | Negative |
| Mannitol | Positive |
| Fructose | Positive |
| Arabinose | Negative |
| Cellobiose | Positive |
| Xylose | Negative |
| Sucrose | Negative |
| Mannose | Positive |
| Galactose | Negative |
| Starch | Negative |
| Glycerol | Negative |
| Trehalose | Negative |
| Glycogen | Negative |
| Enzymatic Reactions | |
| Esculin Hydrolysis | Positive |
| Lecithinase | Negative |
| Casein Hydrolysis | Negative |
| Lipase | Negative |
| Tryptophan Deaminase | Negative |
Pathogenesis and Virulence Factors of Clostridioides difficile
- The normal flora of the intestine is disturbed by broad-spectrum antibiotics.
- C. difficile then enters the gut after the loss of protective bacteria.
- After that, the infection begins with the ingestion of C. difficile spores.
- These spores then resist gastric acid and reach the intestine.
- After arriving in the colon, the spores sprout into vegetative cells, which are aided by bile salts.
- After that, the bacteria adhere to the intestinal mucosa, where they multiply rapidly.
- Toxin A known as entertoxin and Toxin B known as cytotoxin are produced which obstruct the cytoskeleton of epithelial cells.
- This results in mucosal injury, increased intestinal permeability, apoptosis of epithelial cells, and necrosis.
There are various virulence factors that contribute in pathogenicity of C. difficile, which are explained below:
Toxin A (Enterotoxin)
- It is 308 kDa in size, proteinaceous, and encoded by tcdA.
- It disturbs the compact linkage among epithelial cells.
- It is responsible for secreting fluid, which causes diarrhea.
- Causes inflammation marked by neutrophil presence.
Toxin B (Cytotoxin)
- Is 269 kDa in size and encoded by tcdB.
- Is more potent than toxin A.
- Causes disruption of the cytoskeleton by inactivating Rho GTPases.
- It is responsible for cell rounding, apoptosis, and mucosal damage.
Cytolethal Distending Toxin (CDT)/Binary Toxin
- Found in hypervirulent strains such as ribotype 027 and 078.
- Helps with the attachment of bacteria to intestinal epithelial cells.
- Causes changes in the cytoskeleton.
Surface Layer Proteins (SLPs)
- Responsible for the increased attachment to the mucosal surface of the gut.
- Helps in evasion of the immune system.
Cell Wall Protein 84
- Assist in the release and distribution of bacteria in the host.
- Helps in the attachment and colonization of bacteria to the epithelial cells of the gut.
Biofilm Formation
- Protects bacteria from host immune response and antibiotics.
- It contributes to infection recurrence and duration of infection.
Flagella
- Helps motility and aids bacterial colonization and biofilm formation.
Spore Formation
- Helps protect against environmental stresses such as heat and desiccation.
- Assists in the transmission and presence of bacteria in hospital environments.
Epidemiology and Transmission of Clostridioides difficile
C. difficile is an important causative agent associated with hospital-based post-antibiotic colitis, which occupies up to 3-5% of the intestines of healthy people without manifesting any symptoms. Early 2000s data show a remarkable rise in the incidence of C. difficile infections.
Between 2003 and 2006, infection by C. difficile was found to be more severe and frequent, with a higher likelihood of relapse, compared to those described previously, which was found predominantly in North America and Europe, and was attributed to the emergence of the strain known as BI, NAP1, or ribotype 027. These strains are more virulent than others due to increased toxin production compared with previous strains.
In 2005 in the Netherlands, an infection caused by C. difficile ribotype 078 emerged, with severity similar to that of ribotype 027. Similarly, in 2007, infection with C. difficile was a leading cause of gastroenteritis, with a 5-fold rise in mortality. Likewise, an article published in 2011 by the Centers for Disease Control and Prevention reported an increase in the incidence of C. difficile infection across 10 geographic areas of the United States compared with the previous decade, with higher rates among females and older adults. Half a million people from America are annually infected with C. difficile.
The common reservoir of C. difficile is humans; however, it is also present in various animals. C. difficile is transmitted mainly via the fecal-oral route. Spore transmission frequently occurs in hospitals and long-term care facilities where individuals touch shared objects. It is commonly transmitted through the following methods:
- Contaminated Surfaces: Objects like door handles, bed sheets, and bathroom fixtures contaminated with stool can spread the bacteria.
- Unwashed Hands: If people do not wash their hands after using the bathroom or before eating, C. difficile can spread.
- Shared Items: Medical equipment, especially in healthcare settings, can cause the spread of C. difficile.
Clinical Manifestations of Clostridioides difficile
Symptoms generally start within 5-10 days after medications, which can begin as soon as the first day or up to 3 months later. It causes various types of infection, explained as follows:
- Asymptomatic Colonization
- Carriers carry bacteria without manifesting any symptoms
- Mild to Moderate Infection
- Watery Diarrhea
- Cramp and tenderness in the abdomen
- Low-grade fever
- Severe Infection
- Watery Diarrhea for more than 10 times a day
- Severe pain and cramps in the belly
- Increase in heart rate
- Dehydration
- Nausea
- Fever
- Increase in WBC count
- Loss of appetite
- Loss in body mass
- Swelling in the belly
- Nausea
- Presence of pus or blood in stool
- Complications
- Toxic megacolon: massive dilation in colon, possibility of perforation.
- Sepsis: systemic infection caused by the distribution of toxins or bacteria.
- Pseudomembranous colitis: formation of yellowish plaques on the mucosa of the colon.
- Dehydration and Electrolyte Imbalance: Caused by severe diarrhea.
- Reactive arthritis: causes inflammation, pain, and swelling in the joints and other parts of the body.
- Fluid Leakage: fluid leaks into the abdominal cavity, causing protein loss from the colon and resulting in low albumin levels.
- Recurrent Infection: Found in 20-30% of patients.
- Rare Manifestations
- Perforation in the Bowel
- If untreated, multi-organ failure
Risk Factors
The following are the risk factors for infection with C. difficile:
- People taking antibiotics such as Cephalosporins, Penicillins, Clindamycin, and Fluoroquinolones are at risk.
- People staying in health care settings or who have been in health care settings are at higher risk, as this bacterium spreads through hands, bedside tables, telephones, toilets, and sinks.
- Those having a serious illness or medical procedure can increase the risk of infection with C. difficile, such as those with chronic kidney disease, inflammatory bowel disease, those on chemotherapy, those undergoing digestive tract procedures, and those undergoing stomach surgery.
- People aged 65 and older are at a higher risk of C. difficile infection.
Laboratory Diagnosis of Clostridioides difficile
- Sample Collection and Transportation
- Fresh feces are collected as the sample.
- Specimens that are collected for the detection of toxins should be kept at 4˚C.
Culture
- Cycloserine Cefoxitine Fructose Agar (CCFA), commercially available Chromogenic Media, and Clostridium difficile Selective Agar are used for the culture.
- Fresh diarrheal stool from patients is used for culture.
- Culture alone cannot be used to diagnose Clostridium difficile infection, as it cannot identify toxin-producing strains.
Examination of the Colon
- The inner part of the colon is examined using either colonoscopy or flexible sigmoidoscopy.
- A flexible tube with a small camera at one end is inserted into the colon to observe the infected areas.
- Enzyme Immunoassay for the detection of toxin
- Used for the detection of toxin A and toxin B in fecal samples.
- Is most commonly used because it is low-cost and provides results within hours.
- However, it is less sensitive, having values less than 50-90%.
Glutamate Dehydrogenase (GDH) detection using Immunoassay
- Detection of GDH, a C. difficile antigen, is used as a surrogate marker for the presence of C. difficile strains.
- It is used as a screening test.
- Have high sensitivity but low specificity.
Molecular tests
- Nucleic Acid Amplification Test (NAATs) is used to detect RNA or DNA sequences.
- Uses either PCR or Loop-mediated isothermal amplification to target CD toxin genes.
- Have high sensitivity and specificity.
Imaging Tests
- X-ray or a CT scan is used to observe the following:
- Enlarged bowel
- Perforation in the lining of the colon
- Thickened wall of the colon
Testing with biomarkers
- Inflammation caused by C. difficile toxin can be tested in feces using Cytokines, Myeloperoxidase, Lactoferrin, and Calprotectin.
- Calprotectin and Lactoferrin are found in both intestinal inflammatory processes and inflammatory bowel disease.
- These biomarkers are not specific but could be used as indicators of disease severity.
Treatments of Clostridioides difficile Infections
- Antibiotics
- Vancomycin
- Fidaxomicin
- Metronidazole
- Surgery
Surgery is required if there is:
- Severe pain
- Organ failure
- Toxic megacolon
- Inflammation around the stomach area
For recurrent infection, there are options that are explained as:
- Repeat antibiotic therapy
- Use of different antibiotics.
- Longer prescription of the same antibiotics.
- Fecal Microbiota Transplant
- If antibiotic treatment fails to cure the disease, fecal transplant is used.
- In this transplant, feces from a healthy donor are transmitted to the colon of a diseased person.
- Antibody-based therapy
- Bezlotoxumab is a human antibody against C. difficile toxin B.
- It is used to reduce the risk of recurrent C. difficile infection.
- Probiotics
- These are foods or supplements that contain microorganisms to increase good bacteria in the body.
- However, the exact role of these probiotics are still unknown.
Prevention and Control of Clostridioides difficile Infections
A number of control measures are implemented to prevent the transmission of the bacteria, which are explained below:
Isolation
- There should be contact precautions for both suspected and confirmed cases until the diarrhea resolves or is determined to be non-infectious.
Hand Hygiene
- Regular hand washing with soap and water every time you shake hands with someone.
- No use of sanitizer as it has no effect on C. difficile.
- Environmental Cleaning and Disinfection
- Cleaning by using chlorine-containing disinfectant or other sporicidal agents.
Visitor Management
- It includes restrictions on the number of visitors and education on precautionary measures.
Antibiotic Resistance of Clostridioides difficile
C. difficile is found to be resistant to multiple antibiotics like lincomycin, erythromycin, tetracyclines, penicillins, cephalosporins, and aminoglycosides. Recent studies published between 2012 and 2015 showed resistance patterns of 8.3-100% against Clindamycin, 51%, 47%, and 13-100% against Cephalosporins, Fluoroquinolones, and Erythromycin, respectively. Resistance to second-generation Cephalosporins and Fluoroquinolones is very common.
However, certain strains of C. difficile show resistance towards third-generation Cephalosporins and broad-spectrum Fluoroquinolones. Metronidazole and Vancomycin are the first-line drugs used to treat C. difficile infection.
Conclusion
C. difficile is the main cause of hospital-acquired infection, which has the ability to produce spores to resist environmental stresses like heat and desiccation. It is responsible for producing toxins that can lead to a range of clinical manifestations, from mild diarrhea to severe intestinal conditions.
References
- Henrich, T. J., Krakower, D., Bitton, A., & Yokoe, D. S. (2009). Clinical risk factors for severe Clostridium difficile–associated disease. Emerging Infectious Diseases, 15(3), 415–422. https://doi.org/10.3201/eid1503.080312
- Fernández-García, L., Blasco, L., López, M., & Tomás, M. (2017). Clostridium difficile infection: Pathogenesis, diagnosis and treatment. In Clostridium difficile – A comprehensive overview (Chapter). InTech. https://doi.org/10.5772/67754
- Quality Insights Staff. (2024, November 7). How is C. diff spread? Understanding transmission and preventing contagion of C. difficile infections. Quality Insights. https://www.qualityinsights.org/quality-quest/how-is-c.-diff-spread-understanding-transmission-and-preventing-contagion-of-c.-difficile-infections
- Schwartz, O., Rohana, H., Azrad, M., Shor, A., Rainy, N., Maor, Y., Nesher, L., Sagi, O., & Peretz, A. (2024). Virulence factors, antibiotic susceptibility and sequence type distribution of hospital-associated Clostridioides difficile isolates in Israel, 2020–2022. Scientific Reports, 14(1), 20607. https://doi.org/10.1038/s41598-024-71492-2
- Tijerina-Rodríguez, L., Villarreal-Treviño, L., Morfín-Otero, R., Camacho-Ortíz, A., & Garza-González, E. (2019). Virulence factors of Clostridioides (Clostridium) difficile linked to recurrent infections. Canadian Journal of Infectious Diseases and Medical Microbiology, 2019, Article 7127850. https://doi.org/10.1155/2019/7127850
- Buddle, J. E., & Fagan, R. P. (2023). Pathogenicity and virulence of Clostridioides difficile. Virulence, 14(1), 2150452. https://doi.org/10.1080/21505594.2022.2150452
- Vaishnavi, C. (2021). Virulence factors associated with Clostridiodes difficile: An overview. Journal of Gastrointestinal Infections, 11(1), 24–29. https://doi.org/10.5005/jp-journals-10068-3047
- Mada, P. K., & Alam, M. U. (2024). Clostridioides difficile infection. In StatPearls [Internet]. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK431054/
- Lamont, J. T., Bakken, J. S., & Kelly, C. P. (2025). Clostridioides difficile infection in adults: Epidemiology, microbiology, and pathophysiology. In UpToDate. UpToDate, Inc. Retrieved [date you accessed it], from https://www.uptodate.com/contents/clostridioides-difficile-infection-in-adults-epidemiology-microbiology-and-pathophysiology
- Mayo Clinic Staff. (2023, September 1). C. difficile infection – Symptoms and causes. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/c-difficile/symptoms-causes/syc-20351691
- Chung, H.-S., et al. (2024). Laboratory diagnosis of Clostridioides difficile infection: Guidelines and status of practice in Korea. Annals of Clinical Microbiology, 27(1), 3–10.
- Mayo Clinic. (2023, September 1). C. difficile infection – Diagnosis and treatment. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/c-difficile/diagnosis-treatment/drc-20351697
- College of American Pathologists. (2023). Clostridioides (Clostridium) difficile testing (Version 2.0). https://documents.cap.org/documents/ClostridiffTesting.FullModule2.0.13APR23.pdf
