- Neisseria meningitidis has a thin peptidoglycan layer in its cell wall and an outer membrane, causing it to stain pink or red in a Gram stain.
- It is a coccus. However, it is most often observed as a diplococcus, meaning it occurs in pairs. The two cocci in a pair have flattened or concave sides adjacent to each other, giving them a characteristic “kidney bean” or “coffee bean” shape.
- This arrangement can also be found intracellularly, within white blood cells (polymorphonuclear leukocytes) in cerebrospinal fluid (CSF) samples from infected patients.
- A crucial morphological feature and virulence factor of N. meningitidis is its polysaccharide capsule.
- This capsule surrounds the bacterium and plays a vital role in its ability to evade the host’s immune system, particularly by inhibiting phagocytosis.
- The serogroups of N. meningitidis (e.g., A, B, C, W-135, Y) are classified based on the chemical composition of this capsule.
- N. meningitidis does not have flagella and is non-motile. It is non-spore-forming
Cultural characteristics of Neisseria meningitidis
- Neisseria meningitidis is a fastidious bacterium; it has complex nutritional and environmental requirements for growth.
- It grows best in an environment with increased carbon dioxide (CO2), typically 5% to 10% CO2. This is often achieved in a laboratory setting using a CO2 incubator or a candle jar.
- Since it is a nasopharyngeal commensal, Meningitis requires a narrow temperature range for optimal growth, flourishing at 35–37°C, which is the human body temperature.
- Since it is fastidious, it won’t grow on standard, unenriched media. It requires enriched media that contain essential nutrients.
- Media such as Chocolate agar, Blood agar, and Modified Thayer-Martin medium can be used to culture these microorganisms
- Biochemical properties that N. meningitidis possesses include catalase positive, oxidase positive, and ferments sugar such as glucose and maltose, but not lactose or sucrose
Virulence Factors of Neisseria meningitidis
- Virulence is a microorganism’s capacity to cause disease and the severity of the harm it inflicts on a host.
- This ability is determined by virulence factors, which are specific traits or molecules that help the pathogen invade the host, evade the immune system, and cause damage.
- Neisseria meningitidis possesses several key virulence factors that allow it to colonize, invade, and cause severe disease in its human host
- The polysaccharide capsule is the most important virulence factor of N. meningitidis. It is a slimy, protective outer layer that prevents phagocytosis by host immune cells.
- N. meningitidis uses thin, hair-like structures called pili to attach to the epithelial cells lining the nasopharynx, its natural habitat.
- This initial adherence facilitates the formation of small bacterial clusters known as microcolonies.
- A crucial survival strategy is the ability of the pili to undergo antigenic and phase variation, which allows the bacterium to change its surface proteins and effectively evade the host’s immune response.
- Lipooligosaccharide (LOS) is an endotoxin on the outer membrane of N. meningitidis. When the bacteria die, they release LOS into the bloodstream, which triggers a powerful inflammatory response. This reaction leads to the severe symptoms of meningococcaemia, such as fever, shock, and tissue damage.
- Outer Membrane Proteins (OMPs) such as Opa and Opc help N. meningitidis attach to and invade host cells. They are critical for the bacteria to cross the endothelial cells of the blood-brain barrier. This allows the bacteria to enter the central nervous system, leading to meningitis.
Pathogenesis of Neisseria meningitidis
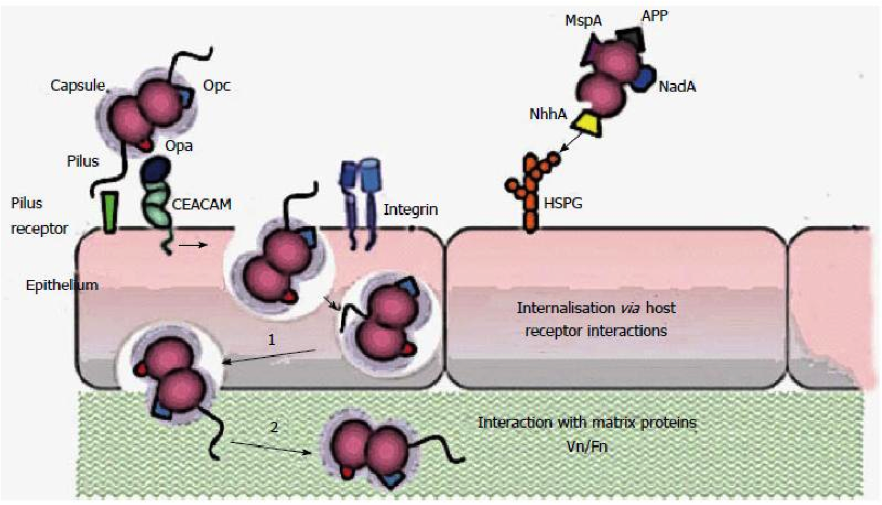
Jose Uberos, et al. (2015), World Journal of Clinical Infectious Diseases 5(2): 37-43.
- The bacteria are spread through droplets of saliva or mucus from an infected person’s cough, sneeze, or talk. Transmission requires close and prolonged contact with the individual.
- The initial and most common stage is Asymptomatic Colonization, where the bacterium resides in the nasopharynx without causing disease.
- Using hair-like structures called pili, particularly Type IV, found on the surface of many Gram-negative and some Gram-positive bacteria. They are complex protein structures that play a crucial role in bacterial pathogenesis and survival.
- Type IV pili are long, helical filaments made of thousands of protein subunits called pilins. A key feature is their dynamic ability to rapidly extend and retract, using a grappling-hook-like mechanism powered by ATPases (PilB and PilT) to perform essential bacterial functions.
- The bacteria attach to cells in the nasopharynx to establish a carrier state. These pili also allow the bacteria to move and form clusters known as microcolonies.
- Using pili and OMPs, the bacteria penetrate the nasopharyngeal barrier either through or between cells. Once in the bloodstream, they use a polysaccharide capsule to protect themselves from the host’s immune system. This invasion is often triggered by a weakened immune state, such as from a prior viral infection.
- After invading the bloodstream, N. meningitidis can lead to two main clinical syndromes: meningitis or meningococcaemia (sepsis), which may occur at the same time. These conditions arise from the bacteria multiplying uncontrollably and engaging with the host’s systemic immune defences.
- After invading the bloodstream, rapid multiplication of N. meningitidis causes meningococcaemia (sepsis) due to the release of Lip oligosaccharide (LOS). This potent endotoxin is shed from the bacterial outer membrane, particularly as the bacteria multiply and die.
- The bacteria cross the blood-brain barrier using OMPs and pili to enter the cerebrospinal fluid (CSF). Once in the CSF, they multiply rapidly due to its poor immune defences. This triggers an intense inflammatory response of the meninges, causing the classic symptoms of meningitis, including a stiff neck and headache.
Symptoms of Meningococcal meningitis
- Meningococcal meningitis is a serious bacterial infection that requires immediate medical attention. The symptoms can develop rapidly and may differ between age groups.
- The very common symptom that a patient may experience is High Fever, a sudden rise in body temperature, and intense headaches
- Nuchal rigidity, which is the medical term for neck stiffness, specifically a resistance to passive neck flexion (bending the head forward)
- A characteristic rash that may start as small, reddish or purple pinpoint spots (petechiae) and progress to larger, bruise-like areas (purpura)
- Increased sensitivity to light, causing eye discomfort or pain.
- disorientation, difficulty concentrating, or feeling sluggish.
- Nausea, vomiting, joint aches
Lab diagnosis of Meningococcal meningitis
- The symptoms of meningococcal disease can rapidly get worse and often resemble the flu. A combination of physical exams, a patient’s health history, and specific tests is carried out to confirm the diagnosis.
- A blood sample is taken and sent to a lab to see if the bacteria, Neisseria meningitidis, will grow. This is a crucial step in confirming a bloodstream infection (meningococcaemia) or meningitis.
- The bacteria use the glucose for energy, so the sugar levels in the CSF are often low.
- Inflammation and infection cause an increase in protein in the CSF.
- A CT or MRI scan of the brain may be performed to check for swelling, fluid accumulation, or other complications.
- Lumbar puncture, or spinal tap, is a medical procedure for getting a sample of the cerebrospinal fluid (CSF), which is the fluid that cushions the brain and spinal cord.
Reference
- Rausch-Phung, E. A., Hall, W. A., & Ashong, D. (2025). Meningococcal Disease (Neisseria meningitidis Infection). In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK549849/
- Pizza, M., & Rappuoli, R. (2015). Neisseria meningitidis: pathogenesis and immunity. Current Opinion in Microbiology, 23, 68–72. https://doi.org/10.1016/j.mib.2014.11.006
- Rouphael, N. G., & Stephens, D. S. (2012). Neisseria meningitidis: Biology, Microbiology, and Epidemiology. In S. K. A. K. D. M. T. O’Toole G. A. (Ed.), Methods in Molecular Biology (Vol. 799, pp. 1–20). Humana Press. https://pmc.ncbi.nlm.nih.gov/articles/PMC4349422/
- https://www.cdc.gov/meningococcal/about/index.html
- Riedel, S., Morse, S. A., Mietzner, T. A., & Miller, S. (2019). Jawetz, Melnick & Adelberg’s medical microbiology (28th ed.). McGraw-Hill Education.
- https://www.sciencedirect.com/topics/medicine-and-dentistry/neisseria-meningitidis
- Surface adhesion and host response as pathogenicity factors of Neisseria meningitidis” by Jose Uberos, et al. (2015), World Journal of Clinical Infectious Diseases 5(2): 37-43.
