Lipids may be regarded as organic substances relatively insoluble in water, soluble in organic solvents (alcohol, ether, etc.), actually or potentially related to fatty acids, and utilized by living cells.
They have chemical compositions of mainly hydrogen, oxygen, and carbon.
Lipids are the esters of fatty acids and alcohol.
- Lipids have three main biological functions in the body: as constituents of structural components of cell membranes, as a source of energy, and as key signaling molecules.
- There are three main types of lipids: triglycerides, phospholipids, and sterols.
What are Triglycerides?
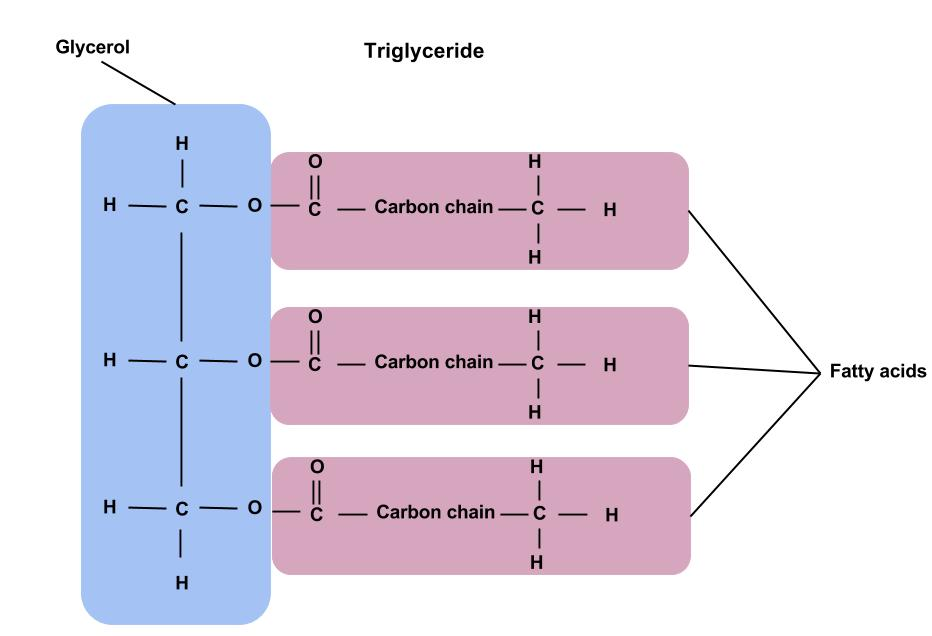
- Triglycerides are a type of lipid that is an ester of three fatty acids with glycerol.
- Triglycerides are the main constituents of body fat in humans, other vertebrates, and vegetable fats.
- They account for over 95% of dietary lipids, appearing either as visible fats and oils or as hidden fat within foods.
- Fatty acids vary in chain length and saturation (saturated vs unsaturated), influencing physical properties like melting point.
- Triglycerides primarily function as the body’s main energy storage form, providing insulation, organ protection, and aiding fat-soluble vitamin absorption while releasing energy on hormonal demand.
What are Phospholipids?
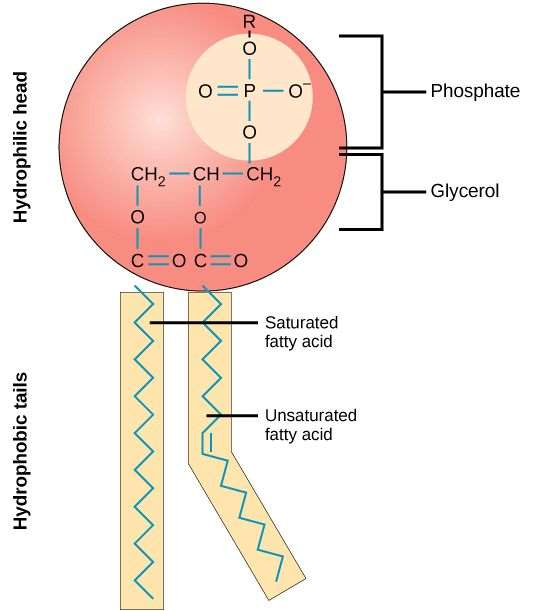
- Phospholipids are similar in structure to triglycerides, with the only difference being a phosphate group and a nitrogen-containing compound in place of a fatty acid.
- Phospholipids possess a unique amphiphilic structure, being both fat- and water-soluble, with hydrophobic fatty acid tails that repel water and hydrophilic phosphate groups plus glycerol that attract it.
What is Cholesterol?
- Cholesterol, exclusively found in animals, is the most abundant animal sterol.
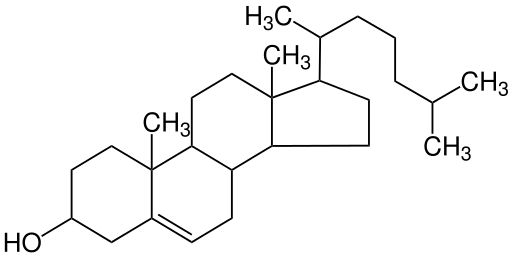
- Cholesterol is formed of four linked hydrocarbon rings forming the bulk of the steroid structure. One end of cholesterol consists of a hydrocarbon tail, whereas the other end is linked to an alcohol group.
- It is widely distributed in all cells and is a major component of cell membranes and lipoproteins.
- Cholesterol is not an essential dietary nutrient because the body synthesizes it in the liver.
- Essential components of cell membranes and precursors for steroid hormones, bile acids, and vitamin D.
The Initial Phase: Mechanical Digestion and Lingual Lipase
- The first step in the digestion of lipids begins in the mouth as it encounters saliva.
- As food is chewed in the mouth, mechanical breakdown occurs, increasing the surface area of the food particles.
- Saliva contains an enzyme called lingual lipase, secreted by the Ebner’s glands on the dorsal surface of the tongue. Its action continues in the stomach.
- This enzyme begins some enzymatic digestion of triglycerides, cleaving individual fatty acids from the glycerol backbone.
- Its activity in the mouth is relatively minor due to neutral pH.
- It becomes active in the acidic stomach environment.
- These actions cause the fats to become more accessible to digestive enzymes.
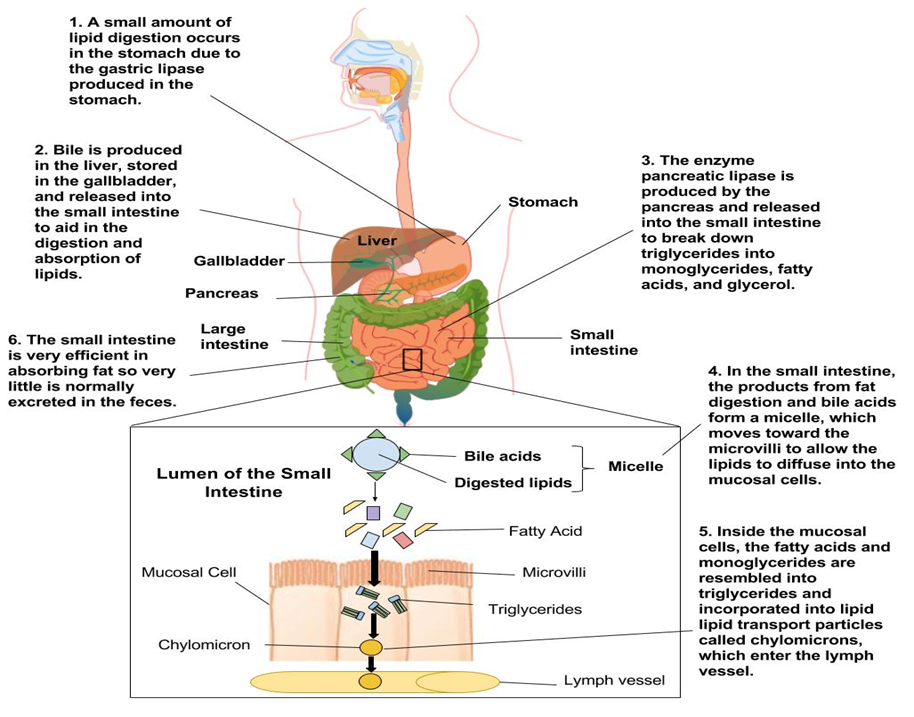
Gastric Digestion: The Role of Gastric Lipase in the Stomach
- Once swallowed, food enters the stomach, where mechanical churning continues to mix and further emulsify fats.
- Gastric lipase is an enzyme produced by chief cells of the stomach and is secreted into gastric juice under the stimulation of gastrin, which continues the breakdown of triglycerides into diglycerides and fatty acids.
- Lingual lipase, swallowed with food, remains active in the stomach.
- Together, these lipases contribute 10–30% of total fat digestion in adults.
- These two lipases play only a minor role in adults but are crucial in infants, whose pancreatic lipase activity is limited.
Emulsification: How Bile Salts Prepare Fats for Hydrolysis
- As the stomach contents enter the small intestine, most of the dietary lipids are undigested and clustered in large droplets.
- When chyme enters the duodenum, fatty acids stimulate intestinal I-cells to release the hormone cholecystokinin (CCK) into the bloodstream.
- CCK signals the gallbladder to contract and release bile into the duodenum via the common bile duct.
- Bile is produced in the liver and stored in the gallbladder.
- Bile contains bile salts, lecithin, and substances derived from cholesterol, so it acts as an emulsifier.
- Bile salts have both a hydrophobic and a hydrophilic side, so they are attracted to both fats and water.
- This makes them effective emulsifiers, meaning that they break large fat globules into smaller droplets.
- Emulsification makes lipids more accessible to digestive enzymes by increasing the surface area for them to act.
Pancreatic Enzymes: The Function of Pancreatic Lipase and Colipase
- In reaction to the CCK hormone, the pancreas releases pancreatic juice that contains active pancreatic lipase, cholesterol esterase, lecithinase (phospholipase A2), and procolipase(inactive precursor) into the duodenum.
- The trypsin enzyme changes procolipase into colipase.
- Bile salts emulsify fats but also inhibit lipase by coating fat droplets.
- Colipase acts as a molecular “anchor” or “bridge.” It has a high affinity for both the bile salts and the lipase.
- Colipase attaches to the surface of fat droplets, displacing part of the bile salt coating, creating an attachment site for pancreatic lipase.
- Binding to the colipase-lipid complex shifts pancreatic lipase’s molecular “lid,” exposing its active site for fat hydrolysis.
- Lipase chemically hydrolyzes triglycerides at the 1st and 3rd positions into two free fatty acids and one 2-monoglyceride molecule.
- Cholesterol esterase hydrolyzes cholesteryl esters into free cholesterol and fatty acids.
- Phospholipase A2 (lecithinase) hydrolyzes phospholipids into lysolecithin and free fatty acids.
- These products are small enough to form micelles, ready for intestinal absorption.
Formation of Mixed Micelles: Solubilizing Fats for Transport
- Small lipid fragments do not form micelles; they are absorbed directly into the bloodstream.
- Even after digestion, larger lipid molecules face a problem because the intestinal lining is covered by a watery mucus layer, which fats cannot cross on their own.
- Bile solves this problem by releasing bile salt into the small intestine.
- Bile salts surround free fatty acids and monoglycerides, forming small transport structures called micelles.
- Micelles have a fatty (lipid) core and a water-soluble outer surface, which allows them to move easily through the watery intestinal environment.
- Mixed micelles transport digested lipid products to the intestinal microvilli, enabling their diffusion into enterocytes.
- Bile salts are recycled back to do more work, emulsifying fat and forming micelles.
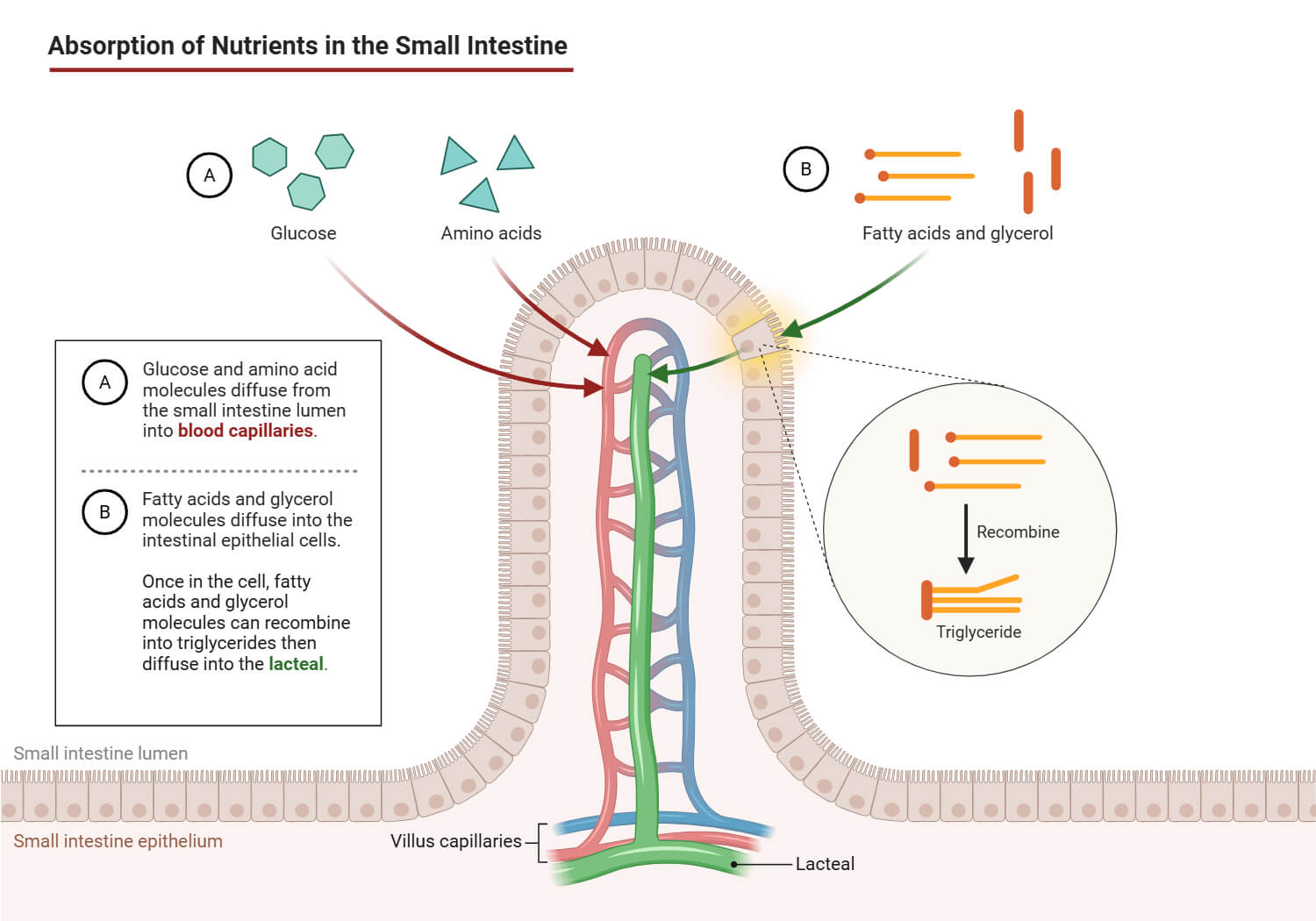
Mechanism of Absorption: Passive Diffusion and Membrane Transporters (CD36)
- Absorption of FA in the small intestine is likely mediated by both diffusion and protein-mediated transfer.
- Fatty acids from micelles enter enterocytes mainly by passive diffusion due to their high luminal concentration, without the need for energy or carriers.
- CD36, a transmembrane fatty acid transporter expressed on the apical membrane of enterocytes, mediates high-affinity uptake of fatty acids, particularly when free fatty acid concentrations are low, complementing passive diffusion.
- Though its overall quantitative role in total fat absorption is relatively small in the intestine.
- Functionally, CD36 facilitates early fatty acid uptake and helps regulate processes like chylomicron formation and enteroendocrine signaling.
Intracellular Processing: Re-synthesis of Triglycerides and Chylomicron Assembly
- Inside enterocytes, long-chain fatty acids and monoglycerides are re-esterified into triglycerides, and cholesterol forms cholesteryl esters.
- These lipids, in combination with phospholipids and apolipoproteins (Apo A, Apo B-48), are combined into nascent chylomicron.
- Chylomicron contains a triglyceride and cholesterol core and the phospholipid-protein outer layer and is therefore soluble in water.
- Chylomicrons facilitate the safe flow of fats in the bloodstream, just like lipids require special processing to facilitate their movement in the intestinal lumen.
- They enter the lymphatic system and finally end up in the blood, where they carry dietary fats to the liver and other tissues.
Lipid Transport: The Lymphatic System vs. Portal Vein
- Fatty acids of medium and short chains, and glycerol are hydrophilic, become albumin-bound, and directly diffuse into capillaries of the portal vein, and directly to the liver, where they are metabolized rapidly.
- The long-chain fatty acids re-esterify triglycerides, which are mixed with cholesterol, phospholipids, and apolipoproteins to create chylomicrons.
- The chylomicron is too big to get into the blood capillaries and drains into the lymphatic system, and then is drained into the bloodstream through the thoracic duct. Bypassing the liver initially.
- The transport depends on the chain length, i.e., short/medium-sized chains run by the portal vein, and long chains use lymph for systemic distribution.
Special Case: Digestion and Absorption of Medium-Chain Triglycerides (MCTs)
- MCTs consist of 6-12 carbon fatty acids coupled to a glycerol backbone and are smaller and more water-soluble compared to long-chain triglycerides (LCTs).
- They do not need bile or pancreatic enzymes to be emulsified or digested.
- The MCTs are digested to free fatty acids and monoglycerides in the stomach and small intestine by enzymatic action.
- These products are absorbed directly into the portal vein, by-passing the lymphatic system, and are directed directly to the liver.
- Fatty acids produced by MCT are immediately converted to ketones in the liver, which gives fast and easily accessible energy, particularly when glucose in the blood is low.
Clinical Significance
Fat Malabsorption Disorders
- Fat malabsorption disorders are conditions that arise because the small intestine is unable to absorb the dietary fats in the normal manner, resulting in the unabsorbed fats being released in the colon.
- This causes loss of nutrients (fat-soluble vitamins A, D, E, and K) and may lead to weight loss, bloating, gas, and diarrhea.
- The prolonged malabsorption interferes with energy equilibrium and causes deficits affecting vision, bone, immunity, and coagulation.
- The causes behind this may be loss of pancreatic enzymes, a shortage of bile salts, or damage to the mucosa due to diseases such as celiac disease or Crohn’s disease.
Steatorrhea
- Steatorrhea refers to the excessive amount of fat excretion in the stools, and it usually causes pale, bulky, malodorous, loose stools due to unabsorbed fat.
- Etiology: It develops as a result of conditions that hinder the digestion or intake of fat, which include:
- Exocrine pancreatic insufficiency (e.g., chronic pancreatitis, cystic fibrosis).
- Bile acid deficiency (e.g., primary biliary cholangitis, ileal disease).
- Small intestinal mucosal disorders (e.g., tropical sprue, celiac disease).
- Pathophysiology: The normal digestion of fats depends on the presence of bile acids, pancreatic enzymes, and well-functioning intestinal villi.
- Failure in any aspect of bile secretion, lipase activity, or villous absorption interferes with the formation of the micelle and uptake of lipids, resulting in the retention of fat in the lumen and stools.
- Consequences & Clinical Significance: Chronic steatorrhea is a sign of underlying disease and leads to malnutrition, weight loss, and defects of fat-soluble vitamins (A, D, E, K). Diagnosis and treatment of the contributing disorder must be recognised early.
Conclusion
- The dietary fats, which are mainly cholesterol, phospholipids, and triglycerides, play a vital role in signaling, energy, and structure.
- The breakdown of fat starts in the mouth and stomach and is finished in the small intestine with the help of bile through emulsification and the enzymes produced by the pancreas.
- Lipid absorption throughout the intestinal mucosa requires bile salts and the formation of micelles.
- Depending on the length of the fatty acid chains, absorbed lipids are rearranged into chylomicrons and carried either through lymph or portal circulation.
- Disturbance of any stage results in malabsorption of fats and clinical manifestations like steatorrhea.
References
- Azer, S. A., & Sankararaman, S. (2025). Steatorrhea. In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK541055/
- BioExplorer. (n.d.). Phospholipid bilayer. https://www.bioexplorer.net/phospholipid-bilayer.html/
- Cifarelli, V., & Abumrad, N. A. (2018). Intestinal CD36 and Other Key Proteins of Lipid Utilization: Role in Absorption and Gut Homeostasis. Comprehensive Physiology, 8(2), 493–507. https://doi.org/10.1002/cphy.c170026
- Dixon, J. B. (2010). Lymphatic lipid transport: Sewer or subway? Trends in Endocrinology & Metabolism, 21(11), 716–723. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC2914116/
- Lumen Learning (n.d.). 4.7 Lipid uptake, absorption & transport. In Nutrition Flexbook. Retrieved from https://courses.lumenlearning.com/suny-nutrition/chapter/4-7-lipid-uptake-absorption-transport/ courses.lumenlearning.com
- Open Oregon State University. (2020). 5b: Lipid types and structures. In Nutrition: Science and everyday application, v. 1.0. https://openoregon.pressbooks.pub/nutritionscience/chapter/5b-lipid-types-structures/reference
- Parrish, C. R. (Ed.). (2017, February). The use of medium-chain triglycerides in gastrointestinal disorders. Practical Gastroenterology. Stanford University. https://med.virginia.edu/ginutrition/wp-content/uploads/sites/199/2014/06/Parrish-February-17.pd
- Weininger, J., & Britannica Editors. (n.d.). Lipids. Encyclopaedia Britannica. https://www.britannica.com/science/human-nutrition/Lipids
